© Springer Science+Business Media Dordrecht and People’s Medical Publishing House 2015
Hongjun Li (ed.)Radiology of Infectious Diseases: Volume 110.1007/978-94-017-9882-2_11. Radiology
(1)
CT Department, The Second Affiliated Hospital, Harbin Medical University, Harbin, Heilongjiang, China
(2)
Department of Radiology, Beijing Shijitan Hospital, Capital Medical University, Beijing, China
1.1 Radiography
1.1.1 Technology of Radiography
In recent years, radiography has been technologically digitalized, giving rise to a field of digital radiography (DR) which has replaced conventional radiography and computed radiography (CR).
Radiography can be categorized into three types, namely, routine radiography, special radiography, and contrast radiography.
1.1.1.1 Routine Radiography
The routine radiography includes fluoroscopy and X-ray. Fluoroscopy is applied for observation of dynamic pathological changes and is seldom applied for diagnosis. X-ray is commonly digital radiography which exhibits higher resolution, better image sharpness, clear visualization of details, and abundant image hierarchies. In addition, it has advantages of high temporal resolution within shorter period of time, wider exposure latitude, and possibility of processing and adjustment. It is powerful in post-processing and the images can be stored, transferred, and retrieved in computers. It also has direct access to PACS system to enable teleconsultation via the Internet.
1.1.1.2 Special Radiography
It is rarely applied. As for examination of some special organs such as mammary gland, the special radiography like molybdenum target X-ray is applied with the technology of soft radiation.
1.1.1.3 Contrast Radiography
It is an imaging technique by introducing contrast agents to create and/or enhance density contrast between tissues and organs in human bodies. Based on the routes of introducing contrast agents, contrast radiography falls into two types. One is direct introduction, including (1) oral intake of contrast agent such as barium meal examination for esophagus and gastrointestinal tract; (2) perfusion of contrast agent such as barium enema, bronchography, retrograde cholangiography, retrograde urethrography, fistula and abscess cavity radiography, and hysterosalpingography; and (3) puncture injection of contrast agent; contrast agents can be injected into organs or tissues or infused via catheters such as angiocardiography, arthrography, and myelography. The other is indirect introduction. The contrast agent is introduced initially into a specific tissue or organ before absorbed and accumulated at the target organ for imaging, including absorptive radiography such as lymphangiography and excretory radiography like intravenous cholangiography, intravenous pyelography, and oral cholecystography. The commonly applied contrast radiographies are described as the following:
Digital Subtraction Angiography (DSA)
It is an angiographic examination conducted by angiograph with functions of digital imaging and subtraction. Because the images are digital and subtracted, the harvested images demonstrate the target blood vessels with no distracting images of surrounding tissues and structures. Therefore, the images are subject to multiple post-processing to improve the quality of the images. In combination with various software functions, DSA can facilitate morphological and functional studies of the heart and blood vessels as well as movements of intraluminal structures and hemodynamics. Angiography is commonly applied for diagnosis of vascular diseases and for differential diagnosis of benign and malignant tumors.
Gastrointestinal Barium Radiography
Barium radiography is a preferred examination in radiology for the diagnosis of digestive disorders.
Upper Digestive Tract Barium Examination
During and after the oral intake of barium, the morphological changes, peristalsis, tension, and smoothness of the esophagus, stomach, small intestinal mucosa, and their contours can be observed from different perspectives under X-ray fluoroscope. In such a way, the lesions can be visible on a film for the diagnosis.
Lower Digestive Tract Barium Examination
Barium and air are instilled into the colon via anus to implement double contrast radiography. In such a way, ulcerations, polyps, and tumors on the colon mucosa can be detected.
Urography
Excretory Urography
Excretory urography, also known as intravenous pyelography, is the most commonly used imaging examination to evaluate the urinary system. It can visualize the urinary system by intravenous injection of organic iodine solution that is then excreted via the kidney. In such a way, the renal parenchyma and luminal morphology of the renal calyces, renal pelvis, ureter, and urinary bladder can be demonstrated. In addition, it also demonstrates the excretory function of both kidneys. The contraindications are iodine allergy; severe hepatic, renal, or cardiac insufficiency; and acute nephritis.
Retrograde Pyelography
This procedure requires cystoscopy before insertion of the ureteral catheters into the openings of the ureters. The top of the catheters should reach the ureteropelvic junction. Upon each catheter is injected slowly with 7–10 ml 12.5 % sodium iodide or 30 % meglumine diatrizoate, following immediate radiography. Retrograde pyelography can favorably demonstrate the morphologies of renal calyces and renal pelvis but fails to demonstrate the excretory function of the kidneys. Patients with poor excretory urogram or not indicated for excretory urography, with acute urinary tract infection or urethral stricture, are contraindicated to retrograde pyelography.
Cystography
A cystography necessitates cleansing of bowels and emptying bladder prior to the procedure. Then a catheter should be inserted into the bladder for infusion of 100–200 ml 3–6 % sodium iodide. Orthotropic and right and left oblique cystography should be performed prior to the discharge of the contrast agent. If necessary, moderate quantity of air can be injected for double contrast radiography.
Urethrography
The catheter is placed into the anterior urethra or the syringe is pressed directly against the urethral orifice to introduce 20–30 % meglumine diatrizoate, with simultaneous radiography. Otherwise, radiography can be performed when the patient is instructed to urinate after the catheter is pulled out upon completion of cystography. In the latter cases, the whole urethra is completely relaxed, which enables more favorable observation of urethral stricture and fistula.
1.1.2 Clinical Applications of X-Ray Radiography
1.1.2.1 Diagnosis by X-Ray Radiography
To define accurate diagnosis by X-ray radiography, the following principles and procedures should be observed for the analysis and diagnosis:
1.
Technical conditions of projection should be considered when X-ray films are being observed and analyzed, including position of radiography and parameter settings of radiography. These conditions guarantee the quality of X-ray films for the diagnosis.
2.
To avoid missing any important X-ray demonstrations, the observation should be in certain consequence for systemic analysis. For instances, in analysis of the chest X-ray films, attention should be paid on the thorax, lungs, mediastinum, diaphragm, and pleura, and one of them should be paid more focused attention in combination with clinical manifestations. The lung X-ray films should be observed from lung apex to base and from the hilum to peripheral area of the lungs. Analysis of bone joint films should be in the consequence from bones, joints, to soft tissues. Analysis of bone X-ray films entails consecutive observations of bone cortex, spongy bone, and marrow cavity. Otherwise, a physician may be distracted by conspicuous parts so as to omit or neglect other parts that happen to be the most important and indispensable.
3.
Normal and abnormal demonstrations should be differentiated during the observation and analysis. Therefore, a physician should fully understand the normal anatomy and anatomic variations as well as their X-ray demonstrations.
4.
Regarding the abnormal X-ray demonstrations, cautions should be given to their positions, distribution, quantity, shape, size, border, density, and homogeneity, as well as functional changes of the organ and changes of the organs and tissues adjacent to lesions.
5.
One or more significant X-ray demonstrations also need to be identified so that one or several diseases might be considered to explain such demonstrations. In this way, preliminary X-ray diagnosis can be made.
6.
The preliminary X-ray diagnosis should be verified by considering other clinical data and diagnostic imaging results. Clinical data such as age, gender, occupational history, contact history, life experience, signs and major examination findings, as well as prior therapies are essential to define the X-ray diagnosis. If the preliminary X-ray diagnosis is in consistency with other clinical data, the preliminary X-ray diagnosis is most likely to be correct. Otherwise, reviews should be conducted to figure out the correctness of the interpretation of the X-ray films, logicality of inferences, appropriateness of X-ray diagnosis, as well as the completeness and accuracy of clinical data.
X-ray diagnosis can be basically divided into three categories:
1.
Affirmative diagnosis that is defined by X-ray radiography.
2.
Exclusive diagnosis that excludes the possibility of a diagnosis. However, its limitations should be recognized since it takes some time for the lesions to be visualized by X-ray radiography from the onset of the diseases. Therefore, during this period of time, X-ray radiography may demonstrate negative. In addition, the natural contrast between the organs or tissues and their lesions also affect the demonstrations by X-ray radiography. Therefore, the accuracy of exclusive diagnosis should not be overestimated.
3.
Suspective diagnosis that indicates possibilities of several diseases by X-ray demonstrations but lacks sufficient evidence to define. In such cases, several possible diagnoses can be listed. Since the probability of each possible diagnosis varies tremendously, different words are necessary to accurately express the variance in probability.
1.1.2.2 Clinical Diagnosis by X-Ray Radiography
The clinical diagnosis by X-ray radiography has a history of over 100 years. Despite great superiorities of other advanced radiological techniques such as CT scanning and MR imaging in diagnosis of some diseases, X-ray radiography cannot be fully replaced, especially in examining body parts such as gastrointestinal tract, bones, and joints, as well as cardiovascular system. Moreover, X-ray radiography also has advantages of clear demonstration, low cost, and convenience to use. Therefore, X-ray radiography remains as the most widely used and fundamental examination in medical radiology.
1.2 Computed Tomography
Computed tomography is the most significant breakthrough ever achieved in diagnostic imaging since the discovery of X-rays by Röntgen in 1895 and is a product due to the joint of modern computer control technique and X-ray radiography.
1.2.1 CT Scanning
1.2.1.1 Plain Scanning
Plain scanning refers to the common scanning without contrast enhancement or radiography. It is often the first step of CT scanning.
1.2.1.2 Contrast Scanning
Contrast scanning involves intravenous injection of water-soluble organic iodinated contrast agents prior to scanning, which is commonly applied nowadays. When iodinated contrast agent is injected into blood vessels, the iodine concentrations in normal tissues and lesions are different to create density contrast. Therefore, the lesions that fail to be demonstrated or fail to be clearly demonstrated by plain scanning can be qualitatively diagnosed via such a way of lesions enhancement.
1.2.1.3 Images Post-processing
Spiral CT scanning and imaging requires shorter period of time, but with a wider scanning range. In addition, the slice thickness of scanning is thin and consecutive cross-sectional scanning data can be harvested. After computer processing, two-dimensional or three-dimensional images of any perspectives as well as CT angiogram can be reconstructed. The commonly applied techniques include:
Rendering Techniques
Rendering techniques comprise surface display, maximum intensity projection, and volume rendering technique. These techniques can generate CT three-dimensional images of the examined organ, which can, therefore, be observed from different directions via spinning. Such techniques are principally used for visualization of bones and CT angiography (CTA).
Virtual Endoscopy
Virtual endoscopy is developed by integrating virtual techniques, a computer technology, with CT or MRI. Incorporation of volume data with virtual techniques in computer science such as lumen navigation technique or roaming technique can imitate the process of endoscopic examination. Therefore, the inner lumen of luminal organs from one end to the other can be displayed gradually. The addition of pseudo-color coding technique renders the view of inner lumen more vivid. Currently available virtual endoscopes include virtual angioscope, virtual bronchoscope, virtual laryngoscope, virtual sinoscope, virtual choledochoscope, and virtual colonoscope, all of which show favorable values in clinical diagnosis.
CT Perfusion Imaging
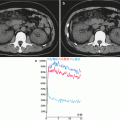
CT perfusion imaging requires continuous scanning of the organs of interest such as the brain, liver, kidney, and heart at a fixed plane after intravenous bolus injection of organic water-soluble iodinated contrast agents to produce multiple-frame images. Based on the changes of image density at different times, a time-density curve of each pixel is formulated to calculate such parameters as the time to peak, mean transition time, regional blood volume, and regional blood flow volume. After the parameters are processed by pseudo-color coding, four-parameter graphs can be harvested. Analysis of these parameters and parameter graphs provides knowledge about the hemodynamics of capillaries in the area of interest, namely, the blood flow perfusion condition. Therefore, CT perfusion imaging is a type of functional imaging.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree