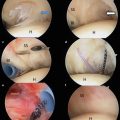
Group I—initial nonoperative treatment
• Tendonitis
• Partial-thickness tears (except maybe larger bursal-sided tears)
• Maybe small (<1 cm) full-thickness tears
Group II—consider early surgical repair
• All acute tears full-thickness (except maybe small [<1 cm] tears)
• All chronic full-thickness tears in a young (<65) age group (except maybe small [<1 cm] tears)
Group III—initial nonoperative treatment
• All chronic full-thickness tears in an older (>65 or 70) age group
• Irreparable tears (based on tear size, retraction, muscle quality, and migration)
The purpose of this chapter will utilize a case-based approach to highlight each group of patients. In groups I and III, nonoperative management was utilized initially in each of the cases. Cases were chosen in these groups that failed initial conservative treatment to review arthroscopic aspects of each case. Group II patients underwent initial early surgical repair. Cases were chosen not only to highlight the indications for surgical versus nonsurgical treatment but also to review specific aspects of surgical management that can be recognized on preoperative MRI and then translated to the arthroscopic repair. Topics reviewed will include tear pattern recognition (L-shaped tear, reverse L-shaped tear, U-shaped tear) requiring margin convergence, recognition of rotator cuff muscle and tendon quality, and improved identification of subscapularis tears.
Case 1: Group I—Partial Thickness Undersurface Subscapularis Rotator Cuff Tear
History and Exam
This is a 42-year-old right-hand-dominant miner with two years of anterior shoulder pain. He reports over a 20-year history of overhead work use as a miner. He has had prior intra-articular corticosteroid injections as well as multiple rounds of physical therapy. The injections temporarily improved his symptoms. He currently has difficulty with work relegating him to work out of the mine.
On physical examination, he has symmetric range of motion of the effected shoulder compared with the opposite shoulder. He has tenderness over his biceps tendon anteriorly and pain with Speeds maneuver and the active compression test. He has no tenderness over his acromioclavicular joint and no pain with cross shoulder adduction. He has pain with a bear-hug test, lift-off test, and abdominal compression testing although he has no weakness with these maneuvers. He has no pain and full strength with thumbs-down scapular plane elevation at 90° of elevation and external rotation at the side.
Imaging
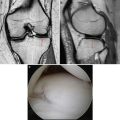
Axial T2 MRI images reveal partial undersurface detachment (red arrow) of the subscapularis tendon (Fig. 14.1). Waviness in the subscapularis tendon is a marker for probable tearing at the insertion. Sagittal T2 MRI images reveal the same partial undersurface tear of the upper third of the subscapularis tendon (red circle) (Fig. 14.2). While biceps tendon deep subluxation was not noted in this patient (not shown), in the presence of subscapularis tearing, either partial or full thickness, biceps instability/subluxation should be presumed to be present and should be specifically looked for during review of axial images. Anterior humeral head subluxation should also be investigated on both plain radiographs and MRI since this is typically prognostic for a very large, chronic subscapularis injury that may not be completely reparable.
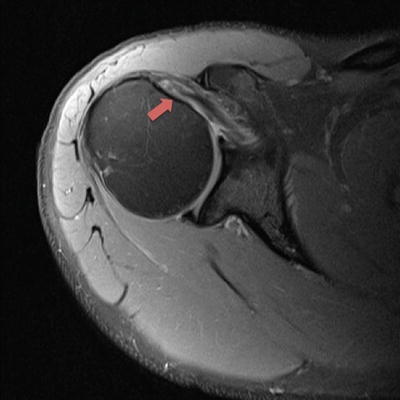
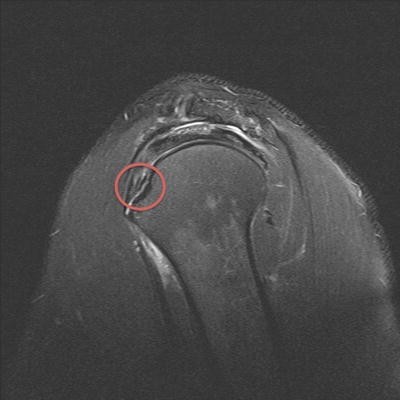

Fig. 14.1
Axial T2 MRI image with a partial-thickness undersurface upper third subscapularis tear (arrow)

Fig. 14.2
Sagittal T2 MRI image showing exposed lesser tuberosity footprint of undersurface partial-thickness subscapularis tear (circle)
Arthroscopy
The patient was considered a group I patient and was initially treated conservatively. Due to failure of conservative treatment, the patient was indicated for arthroscopic subscapularis repair and open subpectoral biceps tenodesis.
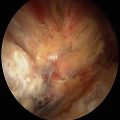
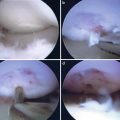
At the time of arthroscopic subscapularis repair, the biceps tendon was noted to have significant fraying and partial-thickness tearing; therefore, it was cut for later tenodesis (Fig. 14.3). The upper third of the subscapularis was noted to have undersurface tearing although the footprint was not obviously visible using a 30° arthroscope (Fig. 14.4). After application of a “posterior level push” and the switching to a 70° scope, the lesser tuberosity footprint was well visualized [16] (Fig. 14.5). A single triple-loaded 5.5 mm metal anchor was placed into the bed of the lesser tuberosity, and three stitches were passed (inferior two as simple stitches and superior stitch as a lasso loop) and tied completing the all intra-articular repair [17] (Fig. 14.6).
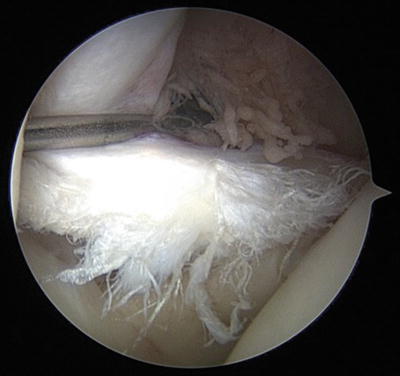
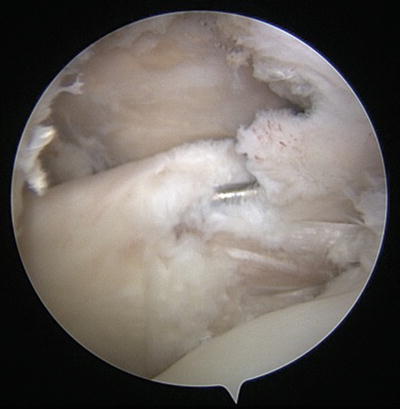
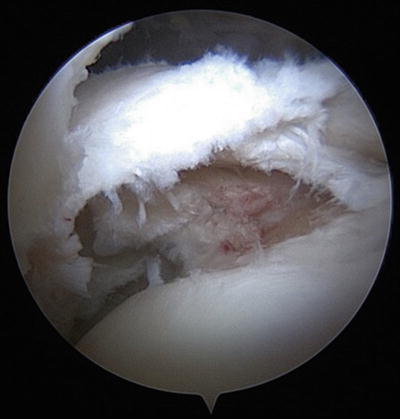
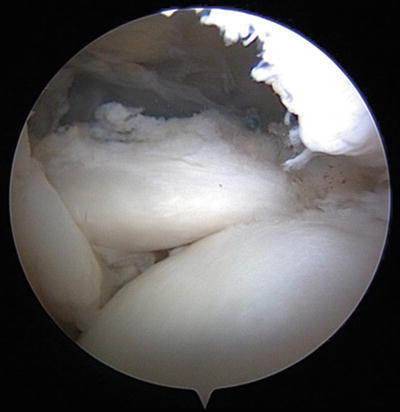

Fig. 14.3
High-grade partial-thickness tear of the intra-articular portion of the biceps tendon long head

Fig. 14.4
Arthroscopic view of the partial undersurface subscapularis tear utilizing a 30-degree arthroscope

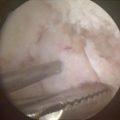
Fig. 14.5
Improved arthroscopic visualization of the lesser tuberosity footprint of the partial undersurface subscapularis tear using a 70-degree arthroscope and a “posterior lever push”

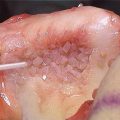
Fig. 14.6
Arthroscopic view of the final subscapularis tendon repair
Discussion
All partial-thickness rotator cuff tears can be initially treated conservatively and are therefore considered group I patients. In general, partial-thickness tears have shown good response to conservative treatment and have also shown a very slow, low risk for tear enlargement or progression making nonoperative treatment safe and effective [4]. Maman et al. evaluated 26 symptomatic partial-thickness rotator cuff tears and determined that 8 % of tears had increased in tear size over 5 mm at an average of 1.5 years with 92 % having no change [4]. Consequently, it is reasonable to consider nonoperative treatment for partial thickness tears and proceed with surgical repair only if there is a failure of conservative management.
Arthroscopic repair of subscapularis tears has shown excellent outcomes in improving pain and function with very high healing rates [18, 19]. MRI can sometimes be difficult to clearly define injuries, especially partial thickness undersurface tears. A tip on identifying these injuries is to be aware of waviness in the subscapularis tendon and deep subluxation of the biceps tendon on axial views as well as evaluating the lesser tuberosity footprint on the sagittal MRI views which can often more clearly show the detachment as in this case. Tips to improve visualization and access to the lesser tuberosity during the procedure include a “posterior lever push” and use of the 70-degree scope.
Case 2: Group II—Chronic Full-Thickness Rotator Cuff Tear in a Young (<65 Years Old) Patient and Failed Arthroscopic Rotator Cuff Repair: Lateral Failure
History and Exam
This is a 54-year-old right-hand-dominant female with six months of chronic shoulder pain. She reports no recent trauma to her shoulder. Her pain is in the anterolateral location worsened by overhead activities. She cannot sleep due to shoulder pain. She has only tried anti-inflammatory medications without improvement.
On physical examination, she has symmetric scapular plane elevation to 160° and external rotation to 50°. She has pain with resisted rotator cuff testing in thumbs-down forward elevation at 90° of scapular plane elevation as well as weakness. She has mild weakness in external rotation at the side as well. She has a positive Neer impingement test as well as Hawkins test. She has no tenderness over either her biceps tendon or acromioclavicular joint.
Imaging
Plain radiographs of the shoulder show no signs of glenohumeral or acromioclavicular joint arthritis with a well-centered humeral head. Coronal T2 MRI images of the shoulder show a 2.5 cm full-thickness, mildly retracted rotator cuff tear of the supraspinatus tendon with grade I Goutallier changes of the supraspinatus muscle (Fig. 14.7). She has limited signal heterogeneity of the tendon on MRI. The tendon length is over 25 mm, and the musculotendinous junction of the supraspinatus is laterally positioned to the glenoid face.
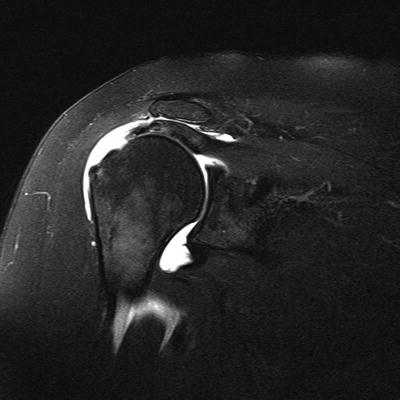

Fig. 14.7
Coronal T2 MRI image of a full-thickness supraspinatus tear with mild retraction
Arthroscopy
Because this is a full-thickness symptomatic rotator cuff tear of substantial size in a young (<65 years old) patient, this was considered a group II patient therefore indicated for early surgical repair.
The patient had an arthroscopy in the beach chair position and was viewed through both posterior and lateral portals while in the subacromial space during the repair. Intra-articular exam revealed no significant pathology, and the subscapularis was normal. A mobile crescent-shaped tear was found of the supraspinatus with mild tendinopathic changes (Fig. 14.8). A double-row transosseous-equivalent repair was performed with limited tension (Fig. 14.9).
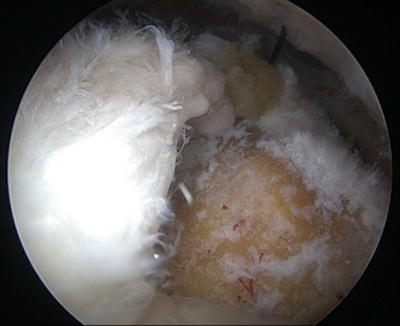
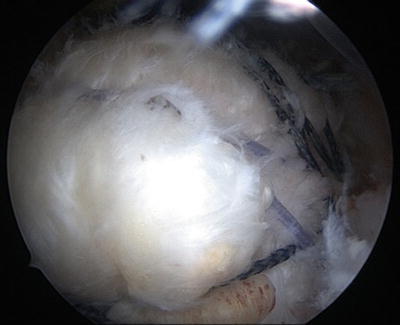

Fig. 14.8
Arthroscopic view from the posterior portal of a crescentic full-thickness supraspinatus tear. There are obvious tendinopathic changes of the rotator cuff tissue

Fig. 14.9
Arthroscopic view from the posterior portal of the complete transosseous equivalent double-row rotator cuff repair
Postoperative Course
The patient underwent conservative postoperative care including sling wear for 6 weeks as well as passive motion starting at 2 weeks. Active and active-assisted motion started at 6 weeks, and strengthening commenced at three months postoperative. At 6 months postoperative, the patient still had lateral-based pain and pain with resisted cuff testing. Her motion had returned to normal and had reasonable strength with rotator cuff testing.
Imaging
Repeat MRI was performed which showed evidence of repair failure with scar tissue interposed between the tendon edge and the tuberosity (Fig. 14.10). The supraspinatus had waviness of the tendon also suggesting the tissue at the footprint was only scar and not healed tendon. Sagittal T1 MRI image of the shoulder shows Goutallier grade II changes to the supraspinatus and infraspinatus muscles (Fig. 14.11). The residual tendon length was still 25 mm although the musculotendinous junction of the supraspinatus was now approximately at the level of the glenoid face.
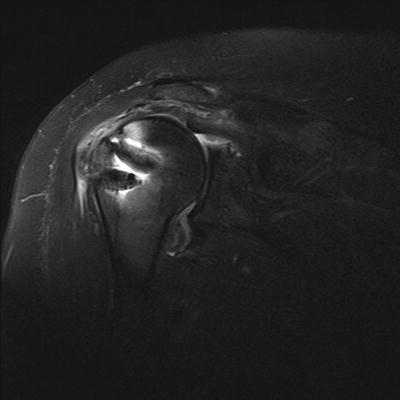
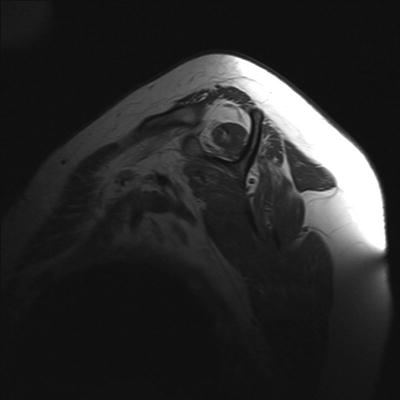

Fig. 14.10
Coronal T2 MRI image of a full-thickness retear of the supraspinatus repair with increased retraction compared to preoperative imaging but preserved tendon length

Fig. 14.11
Sagittal T1 MRI image showing Goutallier grade II changes to the supraspinatus and infraspinatus muscles
Arthroscopy
The patient returned for revision rotator cuff repair and was found to have only fibrous tissue overlaying the greater tuberosity (Fig. 14.12). The tissue was debrided, and anchors were removed leaving moderate amounts of tuberosity cavitation at the site of the prior anchors (Fig. 14.13). A single-row repair was performed with limited tension with three triple-loaded anchors placed at the anatomic neck using nine simple stitches (Fig. 14.14). Microfracture of the greater tuberosity was also performed to stimulate repair healing.
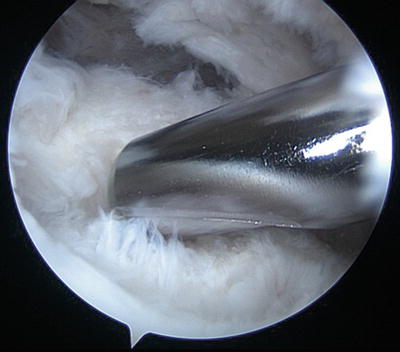
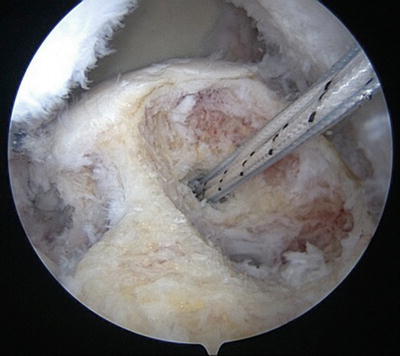
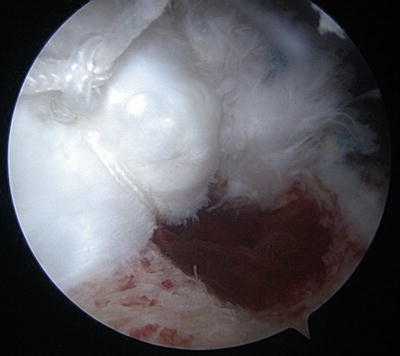

Fig. 14.12
Fibrous scar tissue being debrided from the greater tuberosity footprint in the location of the prior repair

Fig. 14.13
Arthroscopic view from the lateral portal after preparation of the footprint and tendon for re-repair. The cavitary defect left from the prior anchor is obvious, and a new anchor was placed near the articular margin for the re-repair

Fig. 14.14
Arthroscopic view from the posterior portal of the final revision repair construct using a single-row technique and triple-loaded suture anchors
Discussion
Rotator cuff repair was indicated in both instances because each time the patient had a reparable chronic rotator cuff tear in a young (<65-year-old) patient (group II). Substantially sized (>1 cm) chronic reparable full-thickness rotator cuff tears in young patients are indicated for early surgical repair due to the risk for tear progression as well as the high chance for healing if repair is performed [5, 9, 14]. Safran et al. followed 51 patients under the age of 60 with symptomatic full-thickness rotator cuff tears treated conservatively and found that 49 % of tears increased in size at an average of 29 months [5]. Pain at the time of follow-up correlated with significant tear progression. They recommended that young patients with conservatively treated full-thickness tears be monitored with an ultrasound for increases in tear size especially if they remain symptomatic. Tashjian et al. and Boileau et al. determined that younger age correlated with significantly improved healing rates after arthroscopic double-row and single-row repairs, respectively [9, 14]. Given the increased risk for tear progression and the improved chance for healing in a young aged population, early surgical repair was indicated in this patient.
Failure of rotator cuff healing can occur despite healing rates after transosseous equivalent arthroscopic rotator cuff repairs being reported to be very high (<3 cm—92 % healing; >3 cm—83 %) [20, 21]. Not all patients with failure of rotator cuff healing have significant disability. Maintenance of clinical improvement has been documented even after repair failure at long term with 95 % satisfaction [22]. Despite these promising results, there are likely subgroups of patients that do poorly including younger patients, patients with a worker’s compensation claim, patients with lower education levels, and patients with labor-intensive jobs [23, 24]. This patient was younger than the average rotator cuff repair patient although otherwise she didn’t have any other risk factors for a clinical failure.
In the setting of full-thickness recurrent tears in young patients, the major factor that might influence the indication of revision repair is the residual quality of the rotator cuff—both muscle and tendon. In this case, the patient had Goutallier stage II changes to the supraspinatus and infraspinatus muscles and a preoperative tendon length of 25 mm with minimal retraction (Fig. 14.11). Goutallier originally described the quality of the rotator cuff muscles on CT scan, and Fuch’s et al. translated the grading to MRI [25, 26]. The Goutallier grades are as follows: 0, normal muscle; I, streaks of fat; II, less fat than muscle; III, equal fat and muscle; and IV, more fat than muscle. Liem et al. have previously shown a correlation of healing after rotator cuff repair with quality of the rotator cuff muscle with worse healing rates with Goutallier stage II and above [13]. Despite having slightly worsened fatty degeneration, re-repair was still indicated in this young patient.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree