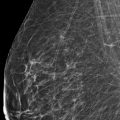
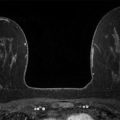
Presentation and Presenting Images
( ▶ Fig. 98.1, ▶ Fig. 98.2, ▶ Fig. 98.3, ▶ Fig. 98.4, ▶ Fig. 98.5)
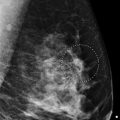
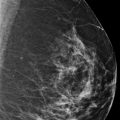
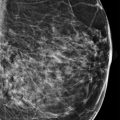
A 46-year-old female with invasive ductal carcinoma of the right breast recently diagnosed at an outside institution presents for second opinion regarding treatment options.
98.2 Key Images
( ▶ Fig. 98.6, ▶ Fig. 98.7, ▶ Fig. 98.8, ▶ Fig. 98.9, ▶ Fig. 98.10, ▶ Fig. 98.11, ▶ Fig. 98.12, ▶ Fig. 98.13, ▶ Fig. 98.14)
98.2.1 Breast Tissue Density
There are scattered areas of fibroglandular density.
98.2.2 Imaging Findings
The imaging of the left breast is normal (not shown). The right breast demonstrates a 2-cm irregular mass (circle in ▶ Fig. 98.6, ▶ Fig. 98.7, ▶ Fig. 98.8, ▶ Fig. 98.9, and ▶ Fig. 98.10) with associated heterogeneous calcifications and the ribbon postbiopsy clip in the lower outer quadrant at the 8 o’clock position, 6 cm from the nipple. This finding is the known malignancy. This finding is seen on the craniocaudal (CC) tomosynthesis movie slice 12 of 86 (circle in ▶ Fig. 98.13) and on the lateromedial (LM) tomosynthesis movie slice 62 of 83 (circle in ▶ Fig. 98.14).
There is a T-shaped postbiopsy clip (arrow in ▶ Fig. 98.6, ▶ Fig. 98.7, ▶ Fig. 98.8, ▶ Fig. 98.9, and ▶ Fig. 98.10) at the 9 o’clock position, 7 cm from the nipple, that denotes the site of the atypical ductal hyperplasia. This finding is seen on right CC tomosynthesis movie slice 28 of 86 (see tomosynthesis movie). This finding is seen on right LM tomosynthesis movie slice 51 of 83 (see tomosynthesis movie).
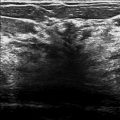
The tomosynthesis movies demonstrate a 1-cm spiculated mass (box in ▶ Fig. 98.11 and ▶ Fig. 98.12) in the upper inner quadrant at the 1 to 2 o’clock position, 7 cm from the nipple. This finding is not well seen on the conventional mammogram. It is seen on the CC tomosynthesis movie slice 36 of 86 (square in ▶ Fig. 98.11) and on the LM tomosynthesis movie slice 32 of 83 (square in ▶ Fig. 98.12). This finding was not seen on ultrasound, so tomosynthesis-directed biopsy was performed.
98.3 BI-RADS Classification and Action
Category 5: Highly suggestive of malignancy
Category 6: Known biopsy-proven malignancy
98.4 Biopsy and Postbiopsy Images
( ▶ Fig. 98.15, ▶ Fig. 98.16, ▶ Fig. 98.17, ▶ Fig. 98.18, ▶ Fig. 98.19, ▶ Fig. 98.20)
98.4.1 Imaging Findings
There is an overlap of findings seen on the right LM view, so targeting was performed in the CC view. The prefire view ( ▶ Fig. 98.15 and ▶ Fig. 98.16) shows the abnormality and adequate biopsy-needle placement (circle). The postfire view ( ▶ Fig. 98.17 and ▶ Fig. 98.18) confirms the needle position is adequate after it has been fired.
A biopsy clip was placed and a postbiopsy mammogram was obtained to demonstrate the location of the clips ( ▶ Fig. 98.19 and ▶ Fig. 98.20). The circle at the 8 o’clock location represents the previously biopsied carcinoma, the arrow at the 9 o’clock location represents the clip placed at the site of the ADH, and the square at the 1 to 2 o’clock location represents the newly placed biopsy clip.
98.5 Differential Diagnosis
Breast cancer (invasive ductal carcinoma [IDC]): The patient has a known invasive ductal carcinoma at one site and biopsy-proven atypical ductal hyperplasia at a second site. She is at increased risk for developing a second primary malignancy. This irregular mass is concerning for a second primary malignancy. It is located in a different quadrant from the original diagnosis, thus this represents multicentric cancer.
Radial scar: This mass is irregular. The typical presentation of a radial scar is a spiculated mass or architectural distortion. Although this finding could represent a radial scar, malignancy must be excluded.
Fat necrosis: There are many appearances of fat necrosis and this patient has undergone two recent biopsies. Although this finding could represent fat necrosis, malignancy must be excluded.
98.6 Essential Facts
Patients with a primary breast cancer may have other sites of malignancy in the same breast.
Multifocal breast cancer is defined as the presence of two more foci of cancer within the same quadrant of the breast.
Multicentric breast cancer is defined as the presence of two or more foci of breast cancer in different quadrants of the same breast.
Since patients with multifocal breast cancer are typically eligible for breast conservation surgery, it is important to exclude additional foci of malignancy prior to definitive treatment.
98.7 Management and Digital Breast Tomosynthesis Principles
Overlapping breast parenchyma on mammography is one factor that limits interpretation, particularly in patients with denser breast tissue.
Overlapping breast parenchyma may obscure cancers resulting in missed cancer diagnosis. Conversely, overlapping parenchyma or superimposed normal structures may create pseudomasses or summation artifacts, resulting in false-positive diagnoses and unnecessary biopsies.
Digital breast tomosynthesis is not just helpful in finding abnormalities in patients with denser breast tissue but also in patients with scattered breast parenchyma, as in this case.
This finding was not seen on ultrasound, so tomosynthesis-directed biopsy was performed.
98.8 Further Reading
[1] Friedewald SM, Rafferty EA, Rose SL, et al. Breast cancer screening using tomosynthesis in combination with digital mammography. JAMA. 2014; 311(24): 2499‐2507 PubMed
[2] Rose SL, Tidwell AL, Bujnoch LJ, Kushwaha AC, Nordmann AS, Sexton RJr. Implementation of breast tomosynthesis in a routine screening practice: an observational study. AJR Am J Roentgenol. 2013; 200(6): 1401‐1408 PubMed
[3] Taboada JL, Stephens TW, Krishnamurthy S, Brandt KR, Whitman GJ. The many faces of fat necrosis in the breast. AJR Am J Roentgenol. 2009; 192(3): 815‐825 PubMed
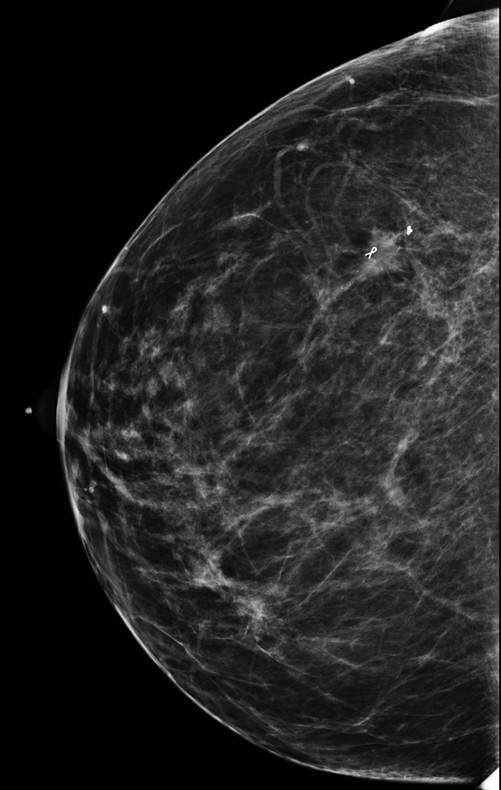
Fig. 98.1 Right craniocaudal (RCC) mammogram.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree