Stabilization and Immobilization Devices
Kim L. Light
Edward C. Halperin
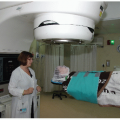
The management of pediatric radiotherapy patients is complex. The goal in radiation therapy is to achieve the desired tumor control while minimizing morbidity. This is especially important in children where late effects of the radiation treatments may include second malignancies and developmental delays. Even a small variation in dose can significantly influence the chance of tumor control and the risk of complications. Variations in dose to normal tissues have been greatly minimized by recent advances in diagnostic imaging, which accurately delineate the target volume. For example, the precise location of the target volume canbe determined with computed tomography (CT), magnetic resonance imaging (MRI), and more recently, with positron emission tomography (PET) (1). There have also been great advances in radiation treatment planning over the years, which allow more accurate delivery of the prescribed dose to the target area. Treatment techniques used for adult and pediatric patients include three-dimensional conformal therapy, intensity-modulated radiation therapy (IMRT), proton radiation therapy (PRT), carbon ion therapy, stereotactic radiation therapy (SRT), and image guided radiation therapy (IGRT) (2, 3, 4, 5, 6, 7). However, all of these technological advances in imaging, planning, and treatment will not be effective unless the patient holds still or is immobilized in a reproducible and comfortable position for each treatment session. The need for daily reproducibility is very important in pediatric patients because of the small margins that are used with the high-dose conformal techniques described. For the youngest patients, anesthesia may also be necessary to hold these patients still (a topic we reviewed in Chapter 21). In this chapter, we will consider psychological, educational, and mechanical aids for patient immobilization.
PSYCHOLOGICAL PREPARATION AND PATIENT AND FAMILY EDUCATION
Before beginning radiotherapy, many children have undergone multiple venipunctures, lumbar punctures, bone marrow biopsies, surgery, and chemotherapy. Therefore, they may fear medical personnel as well as any attempt to be immobilized for the radiation treatments. One important key to the child’s cooperation is the parents’ calm confidence. Because the child will sense their parents’ positive or negative attitude, it is important that the child’s parents feel comfortable with the treatment plan and express their confidence in the presence of the child. This confidence is gained by thoroughly informing the parents about the planning procedures and the daily treatment process.
In order to build the parents’ comfort level, the therapy team should give them a tour of the radiotherapy department and introduce them to the personnel involved in their child’s case. The parents should be given a chance to see and touch the equipment. Most important of all, the parents should be given an unhurried time to ask questions and have them answered. It is often advisable to conduct this initial visit without the child present so that conversation is not inhibited. The parents can also communicate ideas to the staff about making the child more comfortable. During the initial tour, the parents should be shown the type of immobilization device that will be used for the child. It is sometimes helpful for the parents to take home a picture of the device or a sample device to work with the child in their home setting. Later, the child must also be given a tour of the department and meet everyone involved in his or her case prior to starting the planning. The child should be encouraged to bring a favorite doll or stuffed toy animal for “treatment,” and the radiation therapist should be willing to demonstrate the simulation and treatment procedure on the toy (8). An unhurried atmosphere, pleasant background music, patience, and positive reinforcement are all important to ensuring the child’s cooperation.
Many pediatric inpatient services benefit from the expertise of trained play (or recreation) therapists. Because these therapists are often valuable allies in making a child more at ease in the treatment area, they should be made familiar with the routines of pediatric radiotherapy. Play therapists employ various techniques to prepare a child for treatment such as using special “toy” radiotherapy machines, art activities, and acting through the planned treatment. More specific behavioral techniques to improve patient cooperation with radiotherapy are discussed in Chapter 21.
Most children and parents are accustomed to receiving information from television. To meet this need, the physician may turn to specially prepared and commercially available videotapes/CDs that describe external-beam radiotherapy. Some of these videotapes/CDs are specifically targeted at a pediatric audience and use animation and professional actors designed to appeal to young children. Such videotapes/CDs can convey a significant amount of information in a short time and may be watched numerous times by the child and family, if necessary. Some clinics make it a routine to show such instructional films to children and families. In addition, some clinics use video systems during the radiation treatment to help relax and distract the child (9).
Music may also be a powerful tool. The radiotherapy department should have an audio system to play selections from a departmental library of children’s music and stories or be
prepared to play selections of the child’s choosing. Some children prefer a parent/sibling/grandparent to read aloud from a storybook during treatments.
prepared to play selections of the child’s choosing. Some children prefer a parent/sibling/grandparent to read aloud from a storybook during treatments.
ERRORS IN FIELD PLACEMENT
A field misalignment can result in a miss of some part of the tumor volume. With the use of conformal radiation fields, a setup error may result in a significant decrease in tumor control probability because of steep dose-response curve models. Furthermore, poor patient immobilization necessitates greater tumor margins. Improper immobilization will therefore result in treatment setup errors and increase the risk of normal tissue complications and compromised target coverage. To improve tumor control probability and reduce normal tissue complications, it is important to reduce setup error. Reducing setup errors can be facilitated by the proper use of immobilization devices.
Geometric misalignment of the patient relative to the incident beam can result from setup errors. These errors may persist throughout the course of treatment (systematic errors) or they may vary unpredictably around a mean value (random errors). A systematic error is probably of greater clinical significance than treatment-to-treatment variability or random error. The implicit conclusion is that errors in treatment delivery, including unsatisfactory immobilization, may be a significant cause of marginal recurrence of tumor after treatment (10, 11, 12).
No matter what precautions are taken, however, there will always be some uncertainties in the planning and delivery of external beam radiation therapy. The following discussion will explain some of these uncertainties. We are indebted to the well-known author and dosimetrist, Gunilla Bentel (1936-2000), for characterizing various treatment and delivery uncertainties (12).
In broad terms, treatment and delivery uncertainties are of two general types. The first are uncertainties related to the delivery of radiation. These include inhomogeneities in the beam, problems related to dosage calculations, variables in radiation machine output, instability of the beam-monitoring technique, and problems related to beam flatness. The second type of uncertainties in the delivery of radiation therapy can be divided into those related to mechanical inaccuracies in the equipment and those related to the patient. Mechanical uncertainties include errors in field size settings and rotational settings, errors in the crosshair alignment, errors in the arc rotation system (if one is used), deviations in the position of the isocenter, incongruence of the light beam with the actual beam, problems with the alignment system, couch-top difficulties, and errors in constructing the beam-shaping blocks or application of the multileaf collimator system. Patient-related uncertainties include uncertainty in target delineation, organ motion, movement of skin marks, day-to-day problems in repositioning, and patient motion. To reduce the detrimental impact of these uncertainties, effective immobilization techniques are essential.
To the authors’ knowledge, there are no large-scale mathematical evaluations of the effectiveness of immobilization in pediatric radiation oncology. This is not surprising because of the small number of pediatric cases and the wide variety of sites treated; it would be difficult to generate a large series of pediatric patient data. Fortunately, however, there are reports in the literature of the value of adult and pediatric immobilization and comparisons of various types of immobilization devices (13, 14, 15, 16, 17, 18, 19, 20, 21). It would be reasonable to conclude that using immobilization in the treatment of childhood cancers would show improvements in setup reproducibility that are similar to adult cases. Even with the use of anesthesia for daily treatments, immobilization of pediatric patients is worthwhile. One cannot be assured that the anesthetized child is placed in the same position every day. Only a customized immobilization device, adapted to the needs of the anesthesiologist, can minimize patient-related treatment uncertainties.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree