Outline
Embryology of Twins, 132
Pregnancy Dating, 133
Chorionicity, 135
Nuchal Translucency, 137
Anatomic Survey, 138
Placental Evaluation, 139
Cervical Length, 140
Fetal Growth Studies, 140
Serial Surveillance, 143
Monoamniotic Twins, 143
Conjoined Twins, 144
Twin Reversed Arterial Perfusion Syndrome, 144
Twin-Twin Transfusion Syndrome, 145
Twin Anemia-Polycythemia Sequence, 147
Unequal Placental Sharing With Discordant Twin Growth or Selective Fetal Growth Restriction, 148
Single Twin Demise, 148
Conclusion, 150
Summary of Key Points
- •
Early diagnosis and determination of chorionicity in the first trimester are critical for the optimal management of multiple gestations.
- •
Dichorionic twins may be either monozygotic or dizygotic, whereas essentially all monochorionic twins are monozygotic.
- •
In addition to risks for aneuploidy and malformations, increased nuchal translucency (NT) in monochorionic twins reflects the potential for complications related to inter-twin anastomoses within a shared placenta.
- •
Pregnancy risk for fetal structural anomalies is increased in multiple gestations, being highest in those with monochorionic placentation.
- •
Even with monozygotic twins, most structural anomalies are discordant and uncommonly affect both fetuses.
- •
Transvaginal sonography may be useful to assess for placenta previa, vasa previa, and cervical shortening, which are all increased in multiple pregnancies.
- •
Because of limitations of the physical examination and risks associated with abnormal fetal growth and amniotic fluid volume, monthly ultrasound examinations are recommended in multiple gestations.
- •
Multiples with monochorionic placentation require increased scrutiny and serial surveillance for a variety of unique complications such as twin-twin transfusion syndrome (TTTS), unequal placental sharing with discordant twin growth or selective fetal growth restriction (FGR), and twin anemia-polycythemia sequence (TAPS).
Ultrasound technology plays a critical role in the management of multiple gestations, which now compose over 3% of all live births in the United States ( Figs. 7-1 and 7-2 ). Advances in reproductive technologies have contributed to this increase, and, fortunately, these cases are detected early owing to the routine use of sonography in practices that provide these services. In contrast, half of all of twin pregnancies were undiagnosed until delivery in the years before sonography was integrated into obstetric practice. Today, with wide availability of sonography, most multiple gestations are identified in the first trimester, providing the opportunity to individualize and optimize the care of these complicated pregnancies.


Multiple gestations pose special considerations as well as unique conditions that may necessitate additional imaging studies. Standard indications for sonography in multiple gestations include pregnancy dating, determination of chorionicity, nuchal translucency (NT) assessment, anatomic survey, placental evaluation, cervical length assessment, routine fetal growth studies, and serial surveillance of pregnancies complicated by anomalies, fetal growth disturbances, and amniotic fluid abnormalities. Multiples with monochorionic placentation require increased scrutiny for monoamnionicity, conjoined twins, twin reversed arterial perfusion (TRAP) syndrome, twin-twin transfusion syndrome (TTTS), unequal placental sharing with discordant twin growth or selective fetal growth restriction (FGR), twin anemia-polycythemia sequence (TAPS), and single fetal demise. Undoubtedly, ultrasound evaluation is essential for the supervision of multiple gestations in modern obstetrics.
Embryology of Twins
The embryology of twin gestations includes the added complexity of the development of two embryos and either one or two placentas. Twins may be monozygotic or dizygotic, depending on the number of ova that are fertilized at conception ( Fig. 7-3 ). Monozygotic twins result from fertilization of one ovum by one sperm with subsequent division into two embryos. Because they have the same genome, they are often referred to as “identical” twins, although influences on development after conception mean that monozygotic twins are not truly identical. Dizygotic twins result from fertilization of two ova by two sperm ( Figs. 7-3 and 7-4 ). These fetuses are no more closely related than other siblings and are therefore sometimes referred to as “fraternal twins.”


Unlike dizygotic twinning, the rate of monozygotic twinning is constant worldwide and occurs in approximately 1/250 pregnancies ( Table 7-1 ). The timing of cleavage in monozygotic twins determines the type of placentation and the likelihood of additional complications. This effect is depicted in Figure 7-5 and Table 7-2 , which demonstrate the timing and types of placentation. Dichorionic placentation is present in approximately 1/3 of monozygotic twins and results from cleavage very early, in the first 3 days after conception. Monochorionic placentation occurs in 2/3 of monozygotic twins and results from cleavage between days 4 and 8 after conception. Monoamniotic pregnancies are much less common, reported in fewer than 1% of monozygotic gestations, and result from splitting on days 9 to 12. Finally, conjoined twins result from very late attempts at cleavage on day 13 or later. With very rare exceptions, dizygotic twins always have dichorionic-diamniotic placentation.
| Geographic Area | Monozygotic | Dizygotic |
|---|---|---|
| Nigeria | 5.0 | 49.0 |
| United States | ||
| Black | 4.7 | 11.1 |
| White | 4.2 | 7.1 |
| England and Wales | 3.5 | 8.8 |
| Japan | 3.0 | 1.3 |

| Chorion | Amnion | Time to Division (Days) | Frequency |
|---|---|---|---|
| Dichorionic | Diamniotic | 0-3 | 25% |
| Monochorionic | Diamniotic | 4-8 | 75% |
| Monochorionic | Monoamniotic | 9-12 | ~1% |
| Monochorionic | Monoamniotic (conjoined twins) | 13-15 | Rare |
Although the rate of monozygotic twinning is relatively constant in spontaneous twin gestations, it is increased by assisted reproductive technologies (ARTs), particularly those that involve embryo manipulation or later embryo transfer. The rate of monozygotic twinning with ART is increased approximately 2- to 12-fold. The frequency of dizygotic twinning, in contrast, varies and is associated with maternal age, race, geography, and use of fertility treatment. Prior to the widespread use of assisted reproduction, the highest rates of dizygotic twinning were in Nigeria, where 49/1000 live births were twin pregnancies, and lowest in Japan at 1.3/1000 live births (see Table 7-1 ). It is thought that the high rate in Nigerian women results from higher baseline levels of follicle-stimulating hormone. The peak maternal age for spontaneous multiple gestations is 37 years old.
With greater use of fertility treatments, including ovulation induction as well as ARTs, the geographic differences in rates of twinning have changed over time. In one survey in the United Kingdom in 2003, it was reported that 1.4% of deliveries were twins and 0.01% were triplets. ARTs were used in 1.9% of all pregnancies, with 13.5% of ART pregnancies associated with multiple gestations versus 1.2% in spontaneous conceptions. Recognition of the higher perinatal morbidity and mortality risks in multifetal pregnancies has resulted in efforts to decrease the rate of this complication by judicious use of ovulation induction as well as an emphasis on single embryo transfer in ART pregnancies.
Pregnancy Dating
Accurate pregnancy dating is important for the timing of screening and diagnostic testing as well as the correct interpretation of fetal growth in multiple gestations. Experts now recommend that uncomplicated dichorionic twins be delivered at 38 weeks, monochorionic twins at 36 weeks, and monoamniotic twins at 34 weeks. Early confirmation of gestational age, with establishment of a fixed due date, is necessary for delivery planning in multiple pregnancies.
As in singletons, determining gestational age is best accomplished in the first trimester using the crown-rump length (CRL) ( Fig. 7-6 ). Accuracy of the CRL, obtained prior to 14 weeks, to predict the due date is ± 5 to 7 days. After the first trimester, multiple biometric measurements should be used to date the pregnancy but this approach is less precise. For multiples conceived by in vitro fertilization (IVF), dating by embryo transfer is comparable to dating by CRL in the first trimester. In both spontaneous and IVF conceived multiple gestations, dating can be uncertain if there is a significant discrepancy in size between the fetuses. In these cases, dating based on the size of the larger fetus decreases the risk of overlooking early FGR, although the smaller CRL has been shown to be more accurate in the estimation of gestational age.

Chorionicity
Chorionicity impacts obstetric management as well as the risk of possible complications and adverse perinatal outcomes in multiple pregnancies. Selective reduction of an abnormal fetus or multifetal reduction in higher-order multiple pregnancies relies on accurate determination of chorionicity to inform procedural decisions. Correct assignment of chorionicity using sonography is nearly 100% when done in the first trimester compared to an approximate 10% likelihood of error in the second trimester. A 2014 study found that before 20 weeks, sonography incorrectly assigned chorionicity in 6.4% of twins overall, with 4% of dichorionic twins and 19% of monochorionic twins misclassified. Although dizygotic twins are always dichorionic, placentation in monozygotic twins varies, depending on the timing of embryo division after fertilization, and is more difficult to assess with advancing gestational age ( Table 7-3 ). Therefore, chorionicity should be established at the time of the initial sonogram, optimally in the first trimester.
| Embryo Division After Fertilization | Chorion | Amnion | Frequency |
|---|---|---|---|
| 0-3 days | Dichorionic | Diamniotic | 25% |
| 4-8 days | Monochorionic | Diamniotic | 75% |
| 9-12 days | Monochorionic | Monoamniotic | 1% |
| 13-15 days | Monochorionic | Monoamniotic (conjoined twins) | Rare |
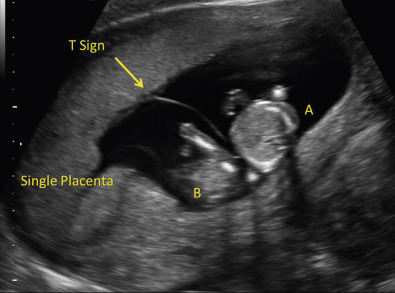
The approach to assigning chorionicity depends on gestational age. Early in the first trimester, the number of gestational sacs equals the number of chorions ( Fig. 7-7 and Table 7-4 ). Late in the first trimester, the visualization of two separate placentas can be used to diagnose dichorionicity ( Fig. 7-8 ). In cases with a single placenta or adjacent apparently “fused” placentas, evaluation of the intervening membrane can help distinguish between monochorionic and dichorionic placentation. Membrane thickness, number of membrane layers, and presence of either the lambda sign or T-sign at the base on the intervening membrane can be evaluated using ultrasound imaging. In dichorionic twins, the separating membrane tends to be thicker, as it is composed of two layers of amnion and two layers of chorion, compared to only two layers of amnion in monochorionic twins. Although a membrane thickness of 2 mm has been used as a threshold to distinguish between dichorionic and monochorionic twins, it does not perform reliably as a diagnostic test. The lambda sign, consisting of a small triangular wedge of echogenic chorionic tissue observed between layers of the intervening membrane at its base, where it meets the fetal surface of the placenta, is diagnostic of dichorionicity ( Figs. 7-9 and 7-10 ). The lambda sign is best visualized in the late first and early second trimesters of pregnancy. It is important to remember that this sign does not necessarily persist on follow-up scans later in pregnancy, but when seen, it helps confirm dichorionicity. The T-sign, which appears as a thin linear structure, composed of two opposing layers of amnion, forming a perpendicular angle where it intersects the fetal surface of the shared placenta, is characteristic of monochorionic placentation ( Figs. 7-10 and 7-11 ). Toward the end of the first trimester and beyond, fetal sex can also be assessed to aid in determination of chorionicity. Although this finding is not useful if both twins appear to be the same sex, different phenotypic findings (one with male and one with female external genitalia) imply dichorionicity except in very rare cases. These principles also apply when evaluating higher-order multiple gestations.

| Placentation | Gestational Sacs | Yolk Sacs | Embryos/Sac | Amniotic Cavities |
|---|---|---|---|---|
| DC, DA | 2 | 2 | 1 | 2 |
| MC, DA | 1 * | 2 | 2 * | 2 |
| MC, MA | 1 * | 1 or partially divided * | 2 * | 1 |



Establishing amnionicity is also important in the evaluation of multiples with monochorionic placentation because fetuses that share a single amniotic sac face increased risks and are managed differently. This is particularly true when caring for higher-order multiple gestations that include a monochorionic twin pair. Although the number of yolk sacs seen early in gestation tends to equal the number of amnions, this is not a reliable diagnostic criterion. A transvaginal sonogram early in gestation can often demonstrate the two amnions of a monochorionic twin pregnancy ( Fig. 7-12 ). Visualization of a separating inter-twin membrane ensures the presence of two amnions in both dichorionic and monochorionic gestations. In monochorionic twins, the intervening membrane can be very thin and difficult to identify, possibly leading to an incorrect diagnosis of monoamnionicity ( Fig. 7-13 ). A transvaginal sonogram and repeat imaging in the first trimester may be required to distinguish between monochorionic diamniotic and monochorionic monoamniotic twin gestations ( Fig. 7-14 ).



Nuchal Translucency
In both singleton and multiple gestations, NT measurements have been used in the evaluation of risk for aneuploidy and fetal anomalies. Overall, the sensitivity of NT combined with maternal age for detection of trisomy 21 in twins is comparable to that in singletons at over 70%, but the screen positive rate is higher, particularly in monochorionic twins. Monochorionic twins have been observed to have increased NT measurements compared to dichorionic twins ( Fig. 7-15 ). This difference may reflect the higher likelihood of structural malformations in monozygotic twins as well as the potential for complications related to inter-twin vascular anastomoses within a shared placenta. The detection rate for Down syndrome in twin pregnancies can be increased by combining maternal age and NT with maternal serum analytes, although it is important that chorionicity be taken into consideration. Because maternal serum screening has not been adequately studied in higher-order multiples and there are likewise limited data regarding the utility of cell-free DNA screening in multiple pregnancies, NT screening is still worthwhile for identifying a potentially abnormal fetus in a multiple gestation warranting further investigation.

Cystic hygroma or hydrops identified at the time of NT assessment may reflect chromosomal or structural abnormalities in both singletons and multiples ( Fig. 7-16 ). Although many different malformations have been associated with enlarged NT and first trimester cystic hygroma, both are recognized risk factors for major cardiac anomalies. Furthermore, both structural and functional types of heart disease are more common in monochorionic twins, and an increased NT may identify those cases most at risk. An added benefit of assessing NT in monochorionic twins is that a 20% inter-twin difference in NT measurement is associated with a greater than 30% risk of fetal death or subsequent development of severe TTTS, thereby identifying those cases that warrant increased scrutiny during follow-up sonographic surveillance. Observation of enlarged NT, cystic hygroma, or early hydrops in a monochorionic pair of a higher-order multiple gestation may also influence recommendations and clinical decisions.

Anatomic Survey
The main objective of the anatomic sonographic survey in multiples is the same as that in singletons: to provide reassurance that the fetuses are developing normally with no evidence of structural abnormalities. Overall, twin and triplet pregnancies have a higher background risk of major malformations, greater than the 2% reported in singletons. Although the rate per fetus remains roughly the same in dizygotic twins or trizygotic triplets, this amounts to an overall rate of 4% and 6% for such pregnancies, respectively ( Fig. 7-17 ). The prevalence of birth defects in monochorionic twins is even higher, nearly twice that observed in dichorionic twins. Interestingly, when both twins are found to have a structural malformation, only 10% of dichorionic and 20% of monochorionic twin pairs have the same defect. Of twin pregnancies with congenital anomalies, only one twin is affected in about 90% of cases. Heightened awareness with careful inspection for malformations is warranted whenever scanning twins and higher-order multiples.

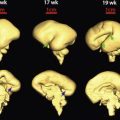
Approximately one third to one half of all birth defects are identified prenatally in singleton pregnancies, and the detection rate in twins and triplets is expected to be even lower. Certain anomalies, such as those involving the central nervous system, are often recognized prenatally, whereas major cardiac abnormalities are frequently missed in twins ( Fig. 7-18 ). This difference is of clinical importance because congenital heart disease is more common in monochorionic twins, in which the prevalence is reported to be about 7.5%. Although controversial, there are some data to suggest that fetuses conceived by IVF are also at increased risk for cardiac defects. The standard cardiac screening examination, consisting of the four-chamber view of the heart and views of the great vessels and outflow tracts, identifies about one third of major heart defects prenatally. Today, IVF, monochorionicity, and increased NT are all accepted indications for fetal echocardiography, which when done in experienced centers can detect close to 100% of major cardiac anomalies. Given the challenge of imaging multiple fetuses in variable positions at midgestation, repeat ultrasound examinations may be necessary to complete the anatomic sonographic surveys in these pregnancies. The management of discordant anomalies in multiples depends upon the gestational age at diagnosis, placentation, type of defect, and potential for associated pregnancy complications. Prenatal diagnosis in twin pregnancies is discussed in Chapter 2 .

Placental Evaluation
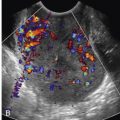
The ultrasound evaluation of each placenta is essential in the assessment of multiple pregnancies. Placenta previa is 40% more common in twin and triplet gestations than in singletons, related in part to the greater placental mass and larger implantation site. Vasa previa is also more common, secondary to the higher proportion of velamentous placental cord insertions (PCIs) noted in multiples, particularly those with monochorionic placentation. Color flow Doppler ultrasound imaging during transvaginal sonography can help identify the presence of placental tissue or a fetal vessel overlying the cervix ( Fig. 7-19 ).

Color flow Doppler sonography can also be used to identify and evaluate the PCI of each fetus, an important component of the ultrasound examination ( Fig. 7-20 ). Both sonographic and pathologic studies have reported that marginal and velamentous cord insertions are more frequent in monochorionic diamniotic twins and that velamentous cord insertion, in particular, is associated with an increased likelihood of TTTS, unequal placental sharing with discordant twin growth, and selective FGR ( Fig. 7-21 ). With velamentous insertion, fetal vessels are devoid of protective Wharton jelly as they traverse the membranes; this lack may contribute to the threefold increase in perinatal mortality rate observed in pregnancies with monochorionic placentation and velamentous PCI ( Fig. 7-22 ). PCI determination early in gestation can help identify those monochorionic diamniotic twins or higher-order multiples with a monochorionic twin pair that merit increased sonographic surveillance for TTTS and disturbances in twin growth. Early detection of these complications should trigger adjustments in clinical management that may help decrease the risk of perinatal morbidity and mortality.