28 Ultrasound Imaging Assessment Following Endovascular Aortic Aneurysm Repair
Color Doppler ultrasound has been used for aortic endovascular graft evaluation and has the advantage of being noninvasive, inexpensive, rapid, safe, nontoxic, easily repeatable, and well tolerated by patients. This technique has already become an important tool in both the planning and the postoperative evaluation of endovascular grafts placed for a variety of vascular lesions and complications.1–9 Color Doppler imaging combines many of the ideal features of both angiography and spiral computed tomography (CT). It allows the examiner to make both quantitative and qualitative assessments of blood flow through the endovascular graft, and via a combination of pulsed-wave and color flow Doppler, can easily demonstrate normal blood flow patterns or abnormal flow patterns associated with specific pathologies. Because color Doppler is relatively inexpensive, easily repeatable, and without known risks, it has become a primary means of surveillance for endovascular interventions.2,4,5,7,10
The primary objectives of the color Doppler examination following endovascular AAA repair are to:
1. Determine whether there is any persistent perigraft flow in the aneurysm sac (endoleak)
2. Characterize the type of endoleak, if present
3. Measure maximal residual aneurysm sac diameter.
4. Assess flow through the graft, including the identification of any kinking, stenosis, or thrombosis
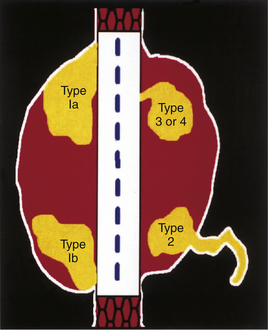
It is important to determine the origin of any blood flow signals identified within the aneurysm sac (endoleak source, Table 28-1) because the source of the blood flow signals and their characteristics may determine subsequent treatment.
| Type 1a, 1b | Endoleak whose origin is at the proximal (1a) or distal (1b) stent attachment site. |
| Type 2 | Endoleak originating from a branch vessel. Possible sources include patent lumbar (posterior to the endovascular graft sonographically), inferior mesenteric (anterolateral to the endovascular graft sonographically), accessory renal or hypogastric arteries, or other patent branches of the abdominal aorta. These are best seen in the transverse orientation. |
| Type 3 | Endoleak that originates at the junctions between components of modular devices or from fabric tears within the graft. |
| Type 4 | Transgraft flow or flow that fills the aneurysm sac because of porosity of the graft. |
| Endotension | Increase in aneurysm size in the absence of endoleak. |
Cross-sectional diameter measurements are recorded at each visit to determine maximum aneurysm size. When an aneurysm sac is excluded from the circulation, an aneurysm should remain stable or decrease in size over time.10,11 Any increase in size suggests that there is preserved blood flow into the aneurysm sac (endoleak) and because of the associated increase in blood pressure, a continued risk for rupture.11,12 However, increases in size have been reported without CT, angiographic, or color Doppler evidence of endoleak (endotension) and proven by direct pressure measurements in the aneurysm sac.13–15
It is also important to determine that the distal arterial circulation has been preserved by ensuring that there are no graft-threatening abnormalities within the body of the endovascular graft, the graft limb(s) or in the inflow and outflow arteries. We previously described a protocol for evaluation of endovascular grafts placed at the aortoiliac level.2
Endovascular Grafts: Overview and General Considerations
The endoluminal placement of stent-grafts, at sites remote from where the graft is introduced, allows for repair of a variety of complex lesions while reducing the relatively high morbidity and mortality associated with traditional open operative repair. The first series of transluminally placed endovascular grafts for the repair of abdominal aortic aneurysms in high-risk patients was reported in 1991.16 Since that time, significant advances in the design of endovascular stents and grafts have facilitated their deployment in aortic and aortoiliac aneurysms, permitting a greater number of patients to be treated with these devices.17–20 We have extensive experience with the Montefiore Endovascular Graft System (MEGS), which has now expanded to include a number of commercially available endografts (Figure 28-1).
Currently several devices (Table 28-2) have been granted U.S. Food and Drug Administration approval for the treatment of aortoiliac aneurysms and are available for widespread use in the United States. Many other devices are undergoing clinical trials in the United States and abroad.21–23
TABLE 28-2 Food and Drug Administration–Approved Grafts for Endovascular Abdominal Aortic Aneurysm Repair
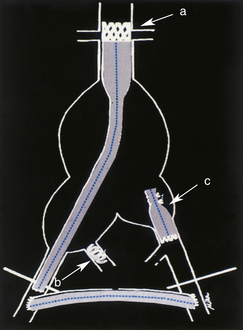
Endovascular grafts are a combination of intravascular metallic stents and prosthetic graft materials. The stent functions as the fixation component of the endovascular graft, anchoring it to normal portions of the aorta and iliac arteries in lieu of standard suture anastomotic techniques. Fixation of the graft can be based on the column strength of the device, the net radial force that pushes outward onto the neck of the aneurysm, or the suprarenal stent components. The stent can be made of nitinol, stainless steel, or a cobalt-chromium alloy. Gore-Tex (polytetrafluoroethylene [PTFE]) and Dacron are the fabrics most commonly used as the prosthetic graft material component of the endograft. Once the endovascular graft is fixed into position, blood should flow only through the endovascular graft, thereby excluding the aneurysm sac from the effects of blood pressure and blood flow. Endovascular grafts come in many types and configurations (Figure 28-2). It is not uncommon for endovascular aortic aneurysm repair to be supplemented by other ancillary procedures such as femorofemoral artery bypass, intra-arterial coil vessel occlusion, or other vessel occlusion procedures (Figure 28-3). Newer endovascular grafts can treat a variety of complex arterial pathologies, and their surveillance becomes more complex. Examples include grafts with hypogastric branches and endografts with incorporated proximal fenestrations and branches.
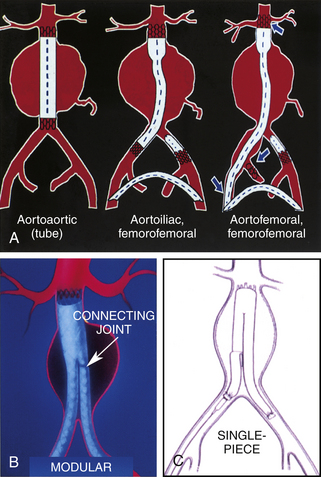
FIGURE 28-2 Examples of the various configurations of endovascular grafts that may be encountered. A, On the left is a simple tube graft with stent attachments at the proximal and distal aneurysm necks. In the center is an aortoiliac endovascular graft, and on the right, an aortofemoral endovascular graft (used for complex aortoiliac aneurysm repair), with the top blue arrow indicating use of an occluding device and the bottom blue arrow an anastomotic site to a femoro-femoral by pass graft. Note the use of occluder devices and coils in the grafts in the center and right of the figure (also see Figure 28-3). The proximal stent crosses the renal arteries in the figure on the far right (top blue arrow). B, A bifurcated modular device with a connecting joint. C, A single-piece, aorto-bi-iliac design.
Since most aortic aneurysms are infrarenal, the proximal component of the endovascular graft is deployed immediately below the lowest renal artery and extends distally as close as possible to the common iliac bifurcation. The device has an uncovered metal component when there is need for suprarenal fixation. The uncovered part of the stent crosses the orifices of the renal arteries. This design is thought to provide better fixation of the graft to the surrounding arterial wall, thereby reducing the potential for proximal graft migration and providing for a better proximal seal (Figure 28-4).
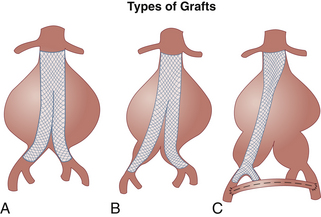
FIGURE 28-4 Various configurations seen in patients with coexisting aortic and iliac artery aneurysms. In type 2A, there is no distal iliac involvement, and an aorto-bi-iliac bifurcated endovascular graft to the proximal common iliac artery is used. In type 2B, there is common iliac artery involvement, and the bifurcated graft is extended to the distal common iliac artery bifurcation. In type 2C, there is extensive iliac artery involvement, and the endovascular graft configuration described in Figure 28-3 is used.
While the endovascular repair of AAAs offers many benefits (Table 28-3), there are several potential complications specific to this technique. The most significant of these complications are endoleaks24,25 and graft migration. These two complications have been seen in all of the endovascular graft designs that have been used for endovascular AAA repair.
TABLE 28-3 Advantages of Endovascular Graft Exclusion of Abdominal Aortic Aneurysms
An endoleak is defined as blood flow outside of the endovascular graft into the aortic aneurysm sac. This leak pressurizes the aneurysm sac and leads to continued risk for aneurysm enlargement and rupture. The presence of an endoleak, therefore, negates the primary goal of the endovascular procedure and results in an aneurysm that remains inadequately treated.11,24–30 Considerable progress in patient selection and surgical technique has reduced the overall rate of all types of complications seen after endovascular AAA repair (Table 28-4). Traditionally the optimal method for postendovascular graft screening and the most reliable method for detecting complications is a contrast CT scan. However, this method is invasive, expensive, and involves radiation exposure to the patient and risk for possible contrast nephrotoxicity. Color Doppler ultrasound has been increasingly and successfully used to follow patients after endograft placement. It can be used to identify patients who may require further intervention with or without the need for additional preprocedural imaging.31,32
TABLE 28-4 Complications Associated With Endovascular Repair of Abdominal Aortic Aneurysms
| Aneurysm growth |
| Embolization |
| Endoleak* |
| Fabric tears |
| Graft infection |
| Graft migration* |
| Limb thrombosis |
| Limb separation |
| Stent and/or attachment site fracture |
Color Doppler Ultrasound Technique
Technologist Preparation
To this end, a review of all previous imaging studies is mandatory. This includes any preoperative or postoperative CT scans, color Doppler scans, or angiograms, as well as any intraoperative imaging studies that have been performed. This review is important because the examiner must be familiar with the configuration and specific anatomy of the endovascular graft,17,33,34 including the locations of the proximal and distal attachment sites. This information is used to document endovascular graft migration (if it occurs) and to identify all possible endoleak sources in advance of the color Doppler examination (Figure 28-5). In addition, review of the operative report or discussion with the operating surgeon is recommended to determine if the following apply: (1) coil embolization of branch vessels or use of other vessel occlusion devices, (2) supplemental proximal or distal arterial reconstructive procedures, and (3) other vessels have been treated with stents, either within the endovascular graft to support a portion of the graft or in the native artery to treat occlusive disease. The sonographic examination includes not only the aortic/iliac stent graft but also all other related arterial occlusion/reconstruction procedures.