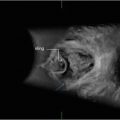
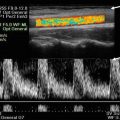
Fig. 4.1
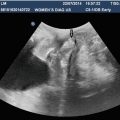
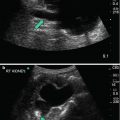
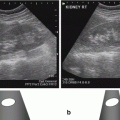
(a) Transabdominal ultrasound scan of pelvis. (b) Transperineal ultrasound scan. (c) Transrectal ultrasound scan (intracavity transducer)
Transabdominal Ultrasound
Transabdominal ultrasound of the pelvis can assist in the evaluation of bladder outlet obstruction, measurement of bladder volume, post-void residual, prostate volume, ureteric jets (Fig. 1.20) and other bladder pathology such as tumours or stones.
Technique of Transabdominal Ultrasound
The examination is easily performed using 2D ultrasound equipment and a curved transducer for abdominal scanning (for example, a 2–5 MHz transducer). It is important to identify the pubic symphysis and place the transducer above this level and angulate the transducer appropriately to avoid loss of field of view caused by shadowing behind the pubic bone (Fig. 4.2). Common measurements in the male patient with voiding dysfunction include pre and post void residual volumes (Fig. 4.3), prostate volume (Fig. 4.4), bladder wall thickness and intravesical prostatic protrusion (Fig. 4.5). The scanning technique is detailed in Tips 4.1.
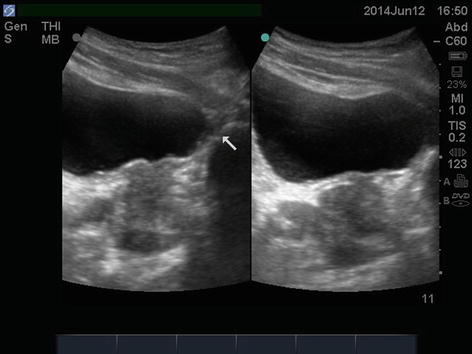
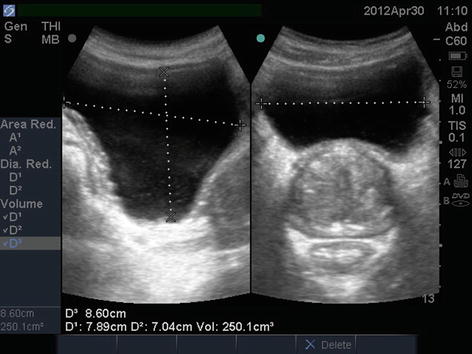
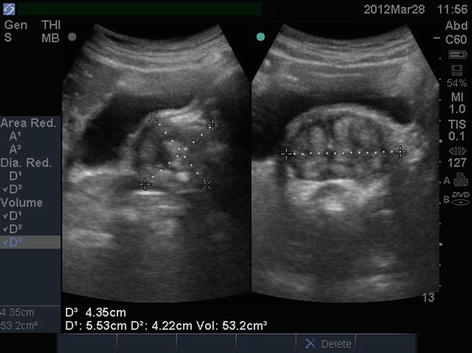
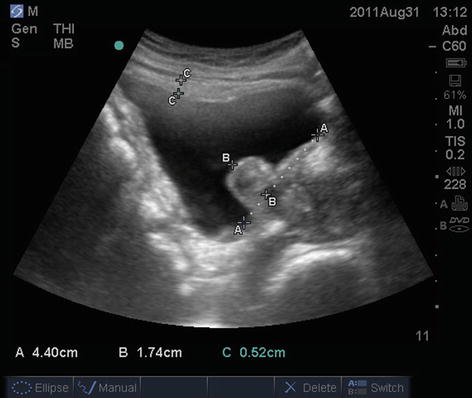

Fig. 4.2
Transabdominal ultrasound image of male pelvis (sagittal plane). It is important to identify the pubic symphysis and angulate the transducer appropriately to avoid loss of view caused by acoustic shadowing behind the pubic bone (arrow)

Fig. 4.3
Postvoid residual urine volume measurement. Ultrasound images of bladder in sagittal and transverse planes showing elevated residual urine and prostatomegaly

Fig. 4.4
Prostate volume measurement. Transabdominal ultrasound images of prostate in sagittal (left image) and transverse planes (right image)

Fig. 4.5
Measurement of intravesical prostatic protrusion (B) as a perpendicular line from the bladder base (A), and bladder wall thickness (C)
Transperineal Ultrasound
The male pelvis can also be imaged via the perineum. This approach (Fig. 4.6) has an emerging role in the evaluation of the pelvic floor in post-prostatectomy incontinence (see Cases 2 and 3). It also provides satisfactory imaging of the prostate for the measurement of prostate volume (which may be more acceptable than a transrectal route) given the difficulty in imaging the apex of the prostate for accurate volume measurement by the transabdominal route [1]. Transperineal ultrasound can also be used to image the prostate to guide biopsies in patients who have undergone abdominal-perineal (AP) excision of the rectum and thus are unable to have transrectal ultrasound. The scanning technique is detailed in Tips 4.2.
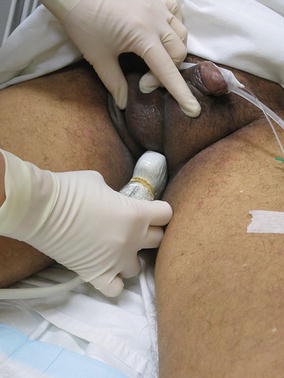

Fig. 4.6
Transducer placement for transperineal ultrasound in the male patient. The scrotum is lifted cephalad to allow placement of the transducer against the perineum
Applications of Pelvic Floor Ultrasound in Physiotherapy
Two useful applications for ultrasound imaging in the physiotherapy management of the urological patient are for stress urinary incontinence (SUI) post radical prostatectomy (RP) and in men presenting with chronic pelvic pain syndrome (CPPS).
Stress Urinary Incontinence (SUI)
Pelvic floor muscle strengthening has long been advocated for men as an intervention aimed at improving continence recovery post RP. Transperineal ultrasound gives a very clear field of view of the Anorectal junction (ARJ), Bulbar penile crus, and urethra. The striated urethral sphincter (SUS) can also be viewed (Fig. 4.7)
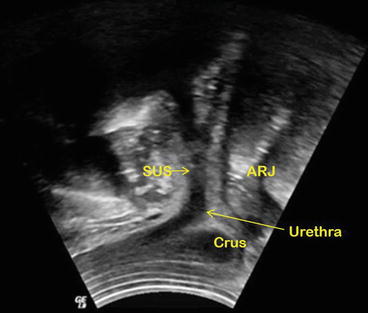

Fig. 4.7
Transperineal ultrasound imaging for pelvic floor muscle strengthening feedback
Prior to any kind of strength training accurate isolation of the correct muscles must first be achieved. Our aim is to reduce the dominant posterior levator ani action (anal component) of the pelvic floor contraction and instead educate the patient on a more anterior penile and SUS lift sensation.
Verbal cues are given to elicit less anterosuperior motion at the ARJ and more posterior slide of the SUS (a sensation of testicular vertical lifting) and an anterior slide of the bulbar penile crus (a sensation of penile indrawing – as if ceasing urination produced by the bulbocavernosus muscle).
The combination of posterior SUS motion and anterior bulbocavernosus contraction causes increasing urethral closure pressure and is therefore considered to be vital in improving continence outcomes [8].
Once evidence of high quality motor control is observed on ultrasound using verbal cueing then the patient may be encouraged to continue with a progressive hypertrophy program designed to further increase urethral closure pressure under progressive loads and functional movement patterns.
Male Chronic Pelvic Pain Syndrome (CPPS)
Also called Chronic Prostatitis, Proctalgia Fugax and Pudendal Neuraligia (amongst other names) this painful condition can often baffle the most experienced clinicians as there is often very little clinical evidence of an organic dysfunction. Cystoscopy, urinalysis, urodynamic and blood tests are often all within normal limits. The patient is often frustrated and frightened and is almost always in a state of high stress and anxiety.
Often the only clinical feature is an abnormally high anal sphincter tone and excessive discomfort during digital rectal examination (even though the prostatic tissue may feel within normal limits).
In these cases pelvic floor hypertonicity may be a contributing and perpetuating factor in this disabling condition.
Transabdominal ultrasound scanning can be a useful tool in evaluating bladder base rise/fall on contraction and release of pelvic floor contractions. Hypertonicity can be seen as a poor bladder base rise on volitional pelvic floor muscle activation and a slow return to a more rested/relaxed state following cessation of pelvic floor muscle activity (Fig. 4.8).
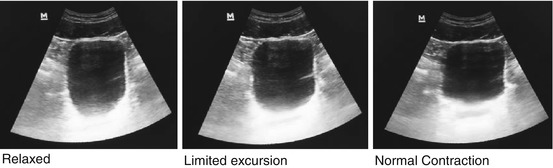

Fig. 4.8
Ultrasound of bladder base rise/fall on contraction and release of pelvic floor muscles
Relaxation of the pelvic floor musclulature can be taught whilst observing the bladder base during respiration. Hypertonic pelvic floors have a tendancy to prevent bladder base descent during inspiration. By giving patients cues to ‘release tension’ in the pelvic floor during the inspiratory phase of respiration (as intra-abdominal pressure increases) increased excursion of the bladder base in a caudad direction may be observed on ultrasound.
Continued practice of effective pelvic floor relaxation may be crucial in assisting in restoring normal pelvic floor tone to the patient with CPPS.
Cases
The following cases illustrate applications of pelvic floor ultrasound in assessment of the male patient with voiding dysfunction.
Case 1 Voiding Dysfunction
A 65-year-old man presented with reduced urinary flow, frequency, nocturia and a sensation of incomplete bladder emptying (Fig. 4.5, Video 4.1).
Comments
The images demonstrate prominent intra-vesical protrusion of the prostate. Various ultrasound imaging parameters have been investigated for the evaluation of bladder outlet obstruction in addition to functional parameters such as uroflow and pressure-flow urodynamic studies. These ultrasound measurements include prostate volume, post-void residual (PVR) urine measurement, bladder wall thickness and measurement of intravesical protrusion of the prostate. Prostate volume and residual urine has poor correlation with urodynamic outlet obstruction and the role of bladder wall thickness is controversial [2, 3]. Of all these parameters, the degree of intravesical protrusion of the prostate (Fig. 4.5) appears to have the best correlation with outlet obstruction [4].
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree