11 Triangular Fibrocartilage Complex
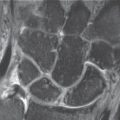
The triangular fibrocartilage complex (TFCC) is a differentiated fibroligamentary structure located between the ulnarhead, the lunate and the triquetrum on the ulnar side of the wrist. Approximately one-fifth of the axial load of the wrist is transferred by the TFCC, and it is the most important stabilizer of the distal radioulnar joint, as well as of theulnar side of the carpus. The triangular fibrocartilage (TFC) in the center is differentiated from the peripheral TFCCelements, consisting of the dorsal and palmar radioulnar ligaments, the ulnolunate and ulnotriquetral ligaments, the tendon sheath of the extensor carpi ulnaris muscle, and the ulnar collateral ligament. Arthroscopy and MRI are most appropriate for imaging these structures. The avascular TFCC center is best visualized with direct MR arthrography, and the vascularized TFCC periphery, with contrast-enhanced MRI.
Fundamental Anatomy
The triangular fibrocartilage complex (TFCC) (also known as the ulnocarpal complex) acts as a buffer and stabilizer between the ulnar head and the ulnar segment of the proximal carpal row (lunate, triquetrum). The triangular fibrocartilage complex is immediately adjacent to the distal radioulnar joint and constitutes a functional unit with this joint. Thedome-shaped TFCC is a complex anatomical and biomechanical structure consisting of fibrocartilaginous and ligamentary elements ( Fig. 11.1 ):
The most important component, the triangular fibrocartilage (TFC), is a centrally located cushion between the ulnar head and the ulnar carpus. With the exception of its periphery, the TFC is abradytropic tissue, and thus poorly vascularized (avascular segment).
The peripheral components of the TFCC consist of synovial folds, which are variable, and ligaments, which ensure fixation and stability. The ligaments are arranged on the palmar and ulnar sides of the TFCC. In comparison to the TFC, the peripheral components of the TFCC are relatively well vascularized (vascular segment).
|
Table 11.1 summarizes the individual components of the triangular fibrocartilage complex.
The triangular fibrocartilage complex has three important functions:
The TFCC is an important stabilizer for the distal radioulnar joint (Fig. 11.1e).
Moreover, the ligaments of the TFCC stabilize the ulnar side of the carpus during movement in the radiocarpal joint, as well as in the distal radioulnar joint (Fig. 11.1a, d).
Approximately 20% of the axial load of the wrist is transferred via the shock-absorbing TFC (about 80% is transferred via the radiocarpal compartment).
The topographic anatomy of the individual components of the TFCC is briefly described below.
Triangular Fibrocartilage (TFC)
The TFC consists of fibrous cartilage and originates with a broad base from the articular cartilage of the radius at the level of the ulnar notch (Fig. 11.1b). After following a horizontal course, it inserts on the ulna with two peripheral fascicles, which have a streaky appearance. One fascicle extends ulnobasal to the fovea in the ulnar head, and the other to the tip of the styloid process of the ulna (insertion type I). Well-vascularized connective tissue lies between the two ulnar fascicles. In rare cases, the TFC terminates in a single fascicle that broadly insertson the styloid process (insertion type II). In an axial crosssection, the TFC appears as an equilateral triangle. In the periphery (limbus), which consists of lamellar collagen fibers, the triangular fibrocartilage is thicker (up to 5 mm) than in the center. This difference in thickness causes a biconcave disk-shaped appearance in sagittal and coronal cross-sections. The relative length of the ulna must be considered when assessing the average thickness of the TFC. A short ulna (minus variant) is accompanied by a relatively thick TFC, and a long ulna (plus variant) by a relatively thin TFC. The TFC has a particular form of blood supply in that only the periphery is well vascularized by blood vessels that radiate into it, whereas the obviously larger central and radial segments are avascular. The radioulnar ligaments and, on thepalmar aspect, the ulnolunate and ulnotriquetral ligaments are attached to the edges of the TFC disc.

Palmar Radioulnar Ligament (PRUL) and Dorsal Radioulnar Ligament (DRUL)
In contrast to the TFC, these two “controlling” ligaments of the distal radioulnar joint originate directly from the compact bone of the distal radius (Fig. 11.1 a,d). These streaky-looking ligaments extend inside the joint capsule in veryclose relationship to the TFC, from which they are separated only by a thin layer of cells, and cannot be differentiated by imaging. Due to their fixation at the radius, the TFC, and the ulnar head, both radioulnar ligaments contribute essentially to the stabilization of the distal radioulnar joint and the TFCC. Because the two ligaments are woven into a spiral, they continually keep the distal radioulnar joint under tension during rotation of the forearm.
Meniscus Homologue (MH)
This structure, which consists of connective tissue, is a relic of evolution, i.e., of the articulation between the ulnar head and the triquetrum that is still evident in primates. This relatively poorly delineated structure consists of a fold of synovial mucous membrane and loose connective tissue. The meniscus homologue originates at the dorsoulnar border of the triangular fibrocartilage and extends obliquely to the palmar and ulnar aspects (Fig. 11.1a, c, d). In its course it swings around the styloid process of the ulna and forms the roof of the ulnar (prestyloid) recess. The meniscus homologue terminates on the palmar side of the triquetrum, the hamate, and the bases of metacarpals IV/V, as well as on the ulnar collateral ligament. It also stabilizes the pisotriquetral joint.
Ulnolunate Ligament (ULL)
This ligament is located in the joint capsule. It is one of two palmar TFCC stabilizers. It originates at the palmar radioulnar ligament and extends in a diagonal course to the palmar horn of the lunate (Fig. 11.1 a). Fibers often radiate into the lunotriquetral ligament. Like the ulnotriquetral ligament, the ULL contributes to the stability of the radiocarpaland the distal radioulnar joints.
Ulnotriquetral Ligament (UTL)
This second stabilizing ligament on the palmar aspect of the TFCC is located on the ulnar side. The UTL originates from the palmar radioulnar ligament either alone or together with the ULL (Fig. 11.1a). It extends steeply to a depression on the palmar side of the triquetrum.
Tendon Sheath of the Extensor Carpi Ulnaris (ECU) Muscle
The ECU tendon sheath, a very thin structure, is integrated into the dorsal segment of the TFCC, where it lies in a groove on the dorsal side of the ulnar head (Fig. 11.1 c, d). It is attached to the extensor retinaculum, which arches over the tendon.
Ulnar Collateral Ligament (UCL)
The UCL is a chordlike thickening of the ulnar side of the joint capsule (Fig. 11.1a, d). Its very existence and delineation from the capsule are controversial in the literature.
Pathoanatomic Principles
Traumatic lesions (partial and complete ruptures) or degenerative changes (mucoid inclusions and perforations) can bemanifested in the triangular fibrocartilage complex (TFCC). It is assumed that a rupture often occurs where there is already degeneration of the TFCC. From a therapeutic and prognostic point of view, alterations in the avascular segment of the triangular fibrocartilage (TFC) must be differentiated from those in the wellvascularized periphery:
Individuals at least 30 years of age generally already have degenerative lesions of the TFC. These begin with the formation of mucoid inclusions, which cause wide perforations in the radial and central segments of the TFC when they reach the surface.
After a short while the TFC perforation results in chondropathy of the articular cartilage lining the ulnar head, the lunate and triquetrum. The final stage is an ulnolunotriquetral impaction syndrome.
When a lesion of the TFCC is already present, it is often accompanied by damage to the lunotriquetral ligament with or without development of carpal instability.
Ruptures of the TFC generally occur in the immediate vicinity of the radial origin and also frequently on the ulnar attachment.
Injuries to the radioulnar ligaments always lead to instability in the distal radioulnar joint. If the palmar radioulnar ligament is involved, the radius dislocates to the palmar aspect. Conversely, an injury to the dorsal ligament leads to a dorsal shift of the radius in the distal radioulnar joint.
Injuries to the ulnolunate and the ulnotriquetral ligaments can promote radiocarpal instability of the carpus.
Diagnostic Imaging
The components of the TFCC can best be visualized with MRI. Arthroscopy, however, remains the diagnostic standard of reference. Since arthroscopy is an invasive procedure, therapeutic measures can be carried out in the same sitting.
Magnetic Resonance Imaging
Examination Techniques
Because extension of the TFCC is in the millimeter range, it can only be visualized with sufficient diagnostic quality if the following examining conditions are fulfilled.
Field strength and gradient field strength: To achieve a sufficient signal-to-noise ratio, as well as high spatial resolution within an acceptable scan time, high-capacity equipment with field strengths of 1.0 or 1.5 T and gradient field strengths of at least 20 mT/m must be used. Low-field scanners of 0.2 or 0.5 T visualize the bony morphology of the carpus, but the carpal ligaments and the TFCC always escape certain assessment.
Surface coils: The use of dedicated surface coils is obligatory on the carpus. Flexible wraparound coils and 2-, 4- or 8-channel coils in phased-array technology are available for this purpose. The latter provide the best images.
Application of contrastmedium: The accuracy of diagnostic assessment of the triangular fibrocartilage complex is significantly increased by the intravenous and/or intra-articular administration of contrastmedium. The surface contour and structural dehiscences accompanying perforations and ruptures of the intrinsic ligamentsand the triangular fibrocartilage are visualized with distension and a high contrast-to-noiseratio in MR arthrography. Fibrovascular regenerative tissue, which appears in the damaged TFCC periphery a few days after injury, can be identifiedand localized with high sensitivity by means of intensive enhancement after intravenous administration of contrast medium.
Appropriate sequences: As explained in Chapters 9 and 10, the sequences listed in Table 11.2 are best suited for visualization of the TFCC on MRI.
The fat-saturated PD-weighted FSE sequence (Fig. 11.2a, c) and the contrast-enhanced T1-weighted SE sequence (Fig. 11.2b) are best suited for two-dimensional imaging.
T2*-weighted GRE sequences (FLASH or FSPGR with an α of 15–30°) and a hybrid DESS-type sequence (with T1 and T2* fractions) are the best suited of the three-dimensional sequences (see Table 10.11). The 3D datasets with nearly isotropic voxels permit radial multiplanar reconstruction (MPR) of the TFC. The center of reconstruction is placed in the styloid process of the ulna, and the reconstruction segment extends between the dorsal and palmar borders of the sigmoid notch of the radius.
A scan field of 8 cm or 10 cm edge length and slice thicknesses of 2 mm for 2D sequences and 1 mm or less for 3D sequences are desirable. Three-dimensional imaging permits MPR in the direction of interest, e.g., parallel to the ulnobasal and ulnoapical fibers of the TFC or the ulnolunate and ulnotriquetral ligaments.
The following text briefly describes the normal anatomy of the triangular fibrocartilage complex as seen on MR images.
|

Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree