17 Management of Liver Metastases
Terence P. F. Gade and Gregory J. Nadolski
17.1 Introduction
The liver is a frequent site of metastatic disease. Although extra-abdominal malignancies can spread to the liver, these tend to be late manifestations of the disease process. On the other hand, intra-abdominal malignancies frequently metastasize to the liver at an early time in the disease course and may be present at the time of diagnosis. This chapter will focus on the management of liver metastases with a focus on two malignancies commonly encountered in the interventional oncology practice: colorectal cancer (CRC) and neuroendocrine tumors (NETs). Other types of metastatic disease to the liver will be briefly discussed at the end of the chapter. A more detailed review of the treatment of cholangiocarcinoma and pancreatic adenocarcinoma metastases can be found in Chapters 18 and 21, respectively, of this book.
17.2 Colorectal Cancer
17.2.1 Incidence, Demographics, and Epidemiology
Among all cancers, CRC has the fourth highest incidence in the United States, with approximately 130,000 new cases diagnosed annually and over 1 million people living with the disease. Worldwide, it is the third most commonly diagnosed cancer and the fourth leading cause of cancer death. Of newly diagnosed patients, nearly 25% will present with distant metastases (stage IV disease, as defined by the American Joint Committee on Cancer). 1 Additionally, up to 50% of patients will develop liver metastases in their lifetime. 1 , 2 The median 5-year survival for metastatic CRC is less than 15%.
CRC incidence varies with geographical location; more than half of all cases occur in more developed nations, with the highest incidence rates occurring in Australia/New Zealand, Europe, and North America. The increased incidence in these regions is partially related to higher rates of physical inactivity, unhealthy diet, smoking, and obesity. 3 Incidence of CRC is higher among people of lower socioeconomic background and educational level in the United States, even when controlling for other known risk factors of the disease, reflecting differences in screening rates among these groups. Racial and sex differences also exist in the United States, with lower rates of CRC among Caucasians and women. Similarly, men worldwide are significantly more likely to develop CRC than women. These differences in incidence are believed to be the result of complex interactions among etiological factors and differences in screening rates. 4 Regardless of race, sex, and socioeconomic status, the incidence of CRC increases with age beginning in the fifth decade of life.
Approximately 90% of CRCs are sporadic, whereas 10% occur in association with one of several genetic conditions predisposing one to CRC. Of these genetic predispositions, the two most common and well understood are familial adenomatous polyposis (FAP) and hereditary nonpolyposis colorectal cancer (HNPCC), formerly referred to as Lynch′s syndrome. In FAP, carcinogenesis is driven by chromosomal instability involving chromosomes 5q, 17p, and 18q. 5 Alterations of these chromosomes lead to deletions and loss of function of the tumor suppressor genes adenomatous polyposis coli (APC), tumor protein P53 (p53), and deleted in colorectal carcinoma (DCC) with subsequent mutational activation of the oncogene KRAS. HNPCC is characterized by microsatellite instability with alterations in mismatch repair genes, leading to accumulation of mutations and carcinogenesis. Both of these patterns of carcinogenesis are observed in sporadic cancers as well, although microsatellite instability in sporadic cancer is an epigenetic phenomenon regulated by methylation of mismatch repair genes as opposed to mutational loss of function of the genes encoding the proteins involved in this deoxyribonucleic acid (DNA) repair mechanism.
17.2.2 Diagnosis and Prognosis
CRC may be suspected when a patient presents with a gradual change in bowel habits, gastrointestinal bleeding, or bowel obstruction. For symptomatic CRC, colonoscopy is usually performed first, as this procedure allows tissue sampling for diagnostic purposes and tissue staging. Alternatively, CRC may be discovered by routine screening. The American College of Gastroenterologists recommends performing screening colonoscopy every 10 years beginning at age 50 (45 years of age for African Americans) in patients at average risk for CRC. Alternative strategies for individuals at average risk include flexible sigmoidoscopy every 5 years, computed tomography (CT) colonography every 5 years, or a fecal immunochemical test for blood annually. Screening strategies for patients with above-average risk because of family history, prior adenomatous polyp, or genetic predisposition to CRC are beyond the scope of this chapter but may be reviewed elsewhere. 6 , 7
Once a diagnosis of CRC has been established based on histological evaluation of the endoscopic biopsy, clinical staging is performed with cross-sectional imaging to evaluate for distant metastases. The National Comprehensive Cancer Network (NCCN) supports the use of CT of the chest, abdomen, and pelvis for all patients with CRC before resection of the primary tumor. Alternatively, contrast-enhanced magnetic resonance imaging (MRI) of the abdomen and pelvis combined with unenhanced CT of the chest can be performed for clinical staging. MRI is more sensitive to detecting liver metastases in treatment-naïve patients and may be particularly advantageous when steatosis of the liver makes the detection of hypoattenuating metastases difficult on CT. The NCCN recommends the use of positron emission tomography (PET)/CT only in the setting of equivocal findings on CT or MRI. In a study comparing preoperative PET/CT with CT, PET/CT was similar to conventional CT in regard to tumor detection rate (100% with PET/CT vs. 95% with CT) and nodal accuracy (59% with PET/CT vs. 62% with CT). Furthermore, findings on PET/CT resulted in treatment changes in only one patient (2%). 8
Overall, the 1- and 5-year survival rates for patients with CRC are 83 and 65%, respectively. A modest decrease in survival is observed at 10 years after diagnosis (~58%). For stage I and IIa CRCs, the 5-year survival rate can exceed 90%. Unfortunately, less than 40% of tumors are diagnosed at these stages, likely because of underuse of screening. For more advanced stage cancers with involvement of regional lymph nodes, the 5-year survival rate decreases to approximately 70%, and this rate further decreases to 13% when the disease has metastasized to distant organs. 9 , 10
Although the colon and rectum will be treated as a single entity in this chapter for simplicity, several factors distinguishing the two entities are worth noting. First, the molecular pathways leading from adenoma to carcinoma differ between the two entities. Colon cancer carcinogenesis is characterized by the two mechanisms mentioned earlier. However, rectal cancer rarely exhibits microsatellite instability, is less KRAS dependent for carcinogenesis, and overall develops more genetic mutations than colon cancer. 11 Second, the pattern of metastatic spread is different with rectal cancer; disease more commonly spreads to the lungs without metastatic involvement of the liver, presumably because of the rectum′s drainage to the systemic venous circulation through the inferior rectal veins. 12 , 13 Additionally, rectal cancers tend to present earlier with a change in bowel habits or visible blood in the stool and can be more readily detected with flexible sigmoidoscopy or digital rectal examination. The combination of these factors culminates in diagnosis at an early stage of the disease compared to colon cancer; this ultimately results in slightly better overall survival. Lastly, treatment for these two entities is different, as treatment for rectal cancer involves neoadjuvant and/or adjuvant radiation to the primary site of disease, whereas treatment for colon cancer does not.
17.3 Therapy for Metastatic Colorectal Cancer
17.3.1 Systemic Chemotherapy
Systemic chemotherapy for metastatic CRC (mCRC) has rapidly evolved over the past 25 years and resulted in a near doubling of the median survival from approximately 12 months to nearly 24 months in some clinical trials. 14 For mCRC, chemotherapy regimens are based on the antimetabolite 5-fluoruracil (5-FU), which directly inhibits thymidylate synthase, in combination with the adjuvant folinic acid, also known as leucovorin (L), which augments 5-FU inhibition of thymidylate synthase. In the late 1990s, several trials demonstrated that the addition of the cytotoxic agent oxaliplatin (XELOX) improved progression-free survival in patients with mCRC compared to 5-FU/L alone (from 6.2 to 9 months). 15 Further studies demonstrated the addition of XELOX with 5-FU/L, known commonly as FOLFOX, significantly improved the disease-free survival rate for patients with stage II or III CRC compared to 5-FU/L alone (from 73 to 78%; hazard ratio [HR]: 0.77; confidence interval [CI]: 0.65–0.91, p = 0.002). 16 , 17
Noninferiority studies of the 5-FU prodrug capecitabine (Xeloda) established its efficacy in intermediate-stage CRC. Subsequently, the use of capecitabine plus XELOX compared to FOLFOX validated the use of this combination for mCRC. 18 In this noninferiority study, XELOX had a similar overall response rate (42%) to FOLFOX (46%). Additionally, progression-free and median overall survivals in the XELOX arm were similar (8.8 and 19.9 months, respectively) to FOLFOX (9.3 and 20.5 months, respectively) with significantly less neutropenia and neuropathy.
Further refinements to the medical treatment of mCRC have involved the addition of the topoisomerase inhibitor irinotecan to 5-FU/L. Initial studies of irinotecan plus 5-FU/L, a combination known as FOLFIRI, demonstrated improved survival with this regimen versus 5-FU/L alone. 19 , 20 FOLFIRI gained widespread acceptance for treating mCRC after a crossover design trial demonstrated that the outcomes with this regimen were equivalent to the outcomes seen with six cycles of FOLFOX. 21 In this study, patients assigned to FOLFIRI first had a median survival of 21.5 months compared to 20.6 months for those allocated to FOLFOX6 before FOLFIRI. Importantly, the response rate to either regimen as the first-line agent was similar (56% with FOLFIRI and 54% with FOLFOX). The only differences in outcomes noted by the investigators were the types of toxicity observed, with more mucositis and nausea/vomiting occurring with irinotecan and more neutropenia and neuropathy occurring with XELOX. 21 The success of FOLFIRI has led some investigators to consider treating mCRC with FOLFIRI plus XELOX, a triplet regimen termed FOLFOXIRI.
Monoclonal antibodies to vascular endothelial growth factor (VEGF) and epidermal growth factor receptor (EGFR) have been used in combination with FOLFOX or FOLFIRI to treat mCRC, particularly in patients who do not carry mutations in KRAS. 22 , 23 , 24 In one trial, patients with mCRC were randomized to FOLFIRI plus the EGFR antagonist cetuximab or to FOLFIRI plus bevacizumab, a monoclonal antibody to VEGF. The objective response rate was similar for the two groups (62% for cetuximab and 58% for bevacizumab). The median overall survival was nearly 29 months in the cetuximab group, about 3 months longer than overall survival in the bevacizumab group, suggesting the potential superiority of cetuximab as a first-line biologic in combination with FOLFIRI. 22
Within the past 15 years, chemotherapy regimens for mCRC have been repeatedly refined increasing overall survival from the time of diagnosis. As a result, surgical and minimally invasive therapies to enhance survival have become more common in the care of these patients. Therefore, knowledge of the toxicities of mCRC chemotherapies that may alter or preclude the use of invasive procedures is mandatory. One well-recognized phenomenon that can occur after treatment with XELOX is hepatic sinusoidal dilation and congestion, which may be seen in up to 19% of patients undergoing liver resection after receiving this agent; however, this effect is not associated with a significant increase in mortality after surgery. 25 5-FU and its prodrug capecitabine are known to cause fatty liver disease, found in nearly half of patients on CT follow-up of hepatic metastases. Unfortunately, the exact relationships among the cumulative dose of 5-FU, changes in liver function tests, and progression to steatohepatitis remain unclear. Although steatosis has been linked to increased complication rates after hepatic resection of colon cancer metastases, mortality is not affected by this condition. 26 , 27 Steatohepatitis is most commonly observed in patients treated with irinotecan (~8%). Unlike steatosis, steatohepatitis is associated with increased 90-day mortality after liver resection (14.7 vs. 1.6% 90-day mortality in patients without steatohepatitis). 25 Lastly, bevacizumab has been found to impair wound healing. Although recommendations regarding bevacizumab treatment differ based on the type of intervention used and other health parameters, in general, the drug must be held both before and after interventions to prevent an increased risk of wound complications. Generally, incisions should be fully healed before bevacizumab therapy is reinitiated. 28
17.3.2 Surgical Management
For patients with liver-only mCRC, surgical resection and/or ablation is the only potentially curative therapy. Many studies have demonstrated a survival benefit with resection including 5-year overall survival of 30 to 60% and 10-year survival of approximately 20%. 29 , 30 However, this treatment strategy has two major limitations. First, the number of patients whose distribution of hepatic metastases is considered resectable at the time of diagnosis is limited, constituting approximately 15% of all patients with mCRC. Second, the eventual failure rate of hepatic resection alone is high, with up to 75% of patients relapsing in some studies and approximately half of all recurrences occurring in the liver. 31 Thus, treatment of mCRC becomes truly multidisciplinary, as the use of neoadjuvant or adjuvant chemotherapy can mitigate both limitations and potentially prolong survival after resection.
Just as the medical management of chemotherapy has evolved over the past three decades, so has the selection of patients for treatment with surgery and neoadjuvant and adjuvant chemotherapy. Although once patients with greater than three hepatic metastases were excluded from resection because of an increased risk of recurrence, current data suggest that although the absolute number of metastases may reflect the likelihood of recurrence, the absolute number of metastases is no longer a contraindication to resection. 32 , 33 Additionally, the presence of bilobar metastases is no longer an absolute contraindication to resection. 34 In both scenarios, the most critical factor is whether all tumors can be completely resected or ablated while preserving adequate liver function. Complete resection (R0 resection) has been shown to be one of the most powerful predictors of overall survival. For example, John et al observed a 5-year survival rate of 46.7% with R0 resection of liver metastases from CRC compared with a 14.6% rate in patients with incomplete resection. 35 To obtain adequate volume of the future liver remnant, portal vein embolization may need to be performed before resection or after ablation in preparation for two-stage hepatectomy. 36 , 37 The details of portal vein embolization indications, techniques, and outcomes are covered in Chapter 19.
The use of postoperative chemotherapy after curative resection improves overall survival compared to surgery alone. However, the optimal timing of chemotherapy relative to resection still remains unclear. There is a strong rationale for preoperative neoadjuvant chemotherapy. First, neoadjuvant therapy can be used to treat micrometastases, preventing further spread to other organs. Second, response assessment to chemotherapy before surgery may allow optimization of therapy after surgery or prevent the need for surgery in patients with early-stage disease. However, it should be noted that several clinical trials and retrospective studies have shown that response before resection is not predictive of overall survival. 38 , 39 , 40 Lastly, neoadjuvant chemotherapy offers the potential to convert unresectable cases to resection candidates. The rate of conversion varies based on the chemotherapy regimen used but has ranged from 20 to 30% in most trials. 41 One potential risk of neoadjuvant therapy is liver injury precluding resection. The primary concern is steatohepatitis secondary to irinotecan or 5-FU treatment. Sinusoidal injury from XELOX is more common, but this occurrence has not been shown to be predictive of postoperative liver failure. 42
17.3.3 Hepatic Artery Infusional Chemotherapy
Like other forms of locoregional therapy, hepatic artery infusional (HAI) chemotherapy is based on the premise that hepatic metastases derive the majority of their blood supply and nutrients from the hepatic artery, whereas hepatocytes rely more on portal venous blood flow. Therefore, the tumoricidal effects of direct infusion of chemotherapy can be maximized while minimizing the systemic toxicity from intravenous administration.
To deliver this therapy, a fully implanted pump is typically placed during a usually open abdominal surgery with the infusion catheter placed into the gastroduodenal artery. 43 5-fluoro 2-deoxyuridine (FUDR), a deoxyribonucleoside derivative of 5-FU, is the typical chemotherapeutic agent infused through HAI pumps. This agent is administered as a continuous infusion in cycles of 2 weeks on and 2 weeks off therapy. FUDR is considered ideal for HAI because it has high first-pass extraction by the liver and, when administered intra-arterially, can reach concentrations in hepatic tumors 400 times greater than the concentrations seen with systemic delivery. 44 , 45
Multiple clinical trials have demonstrated the efficacy of HAI in treating mCRC within the liver. A multicenter German study demonstrated similar overall survival for patients treated with HAI 5-FU/L, systemic 5-FU/L, and HAI FUDR. 46 A study by Kemeny et al 47 assessed HAI FUDR versus systemic 5-FU/L and found that overall survival was significantly longer for the HAI therapy group (median: 24 months) than for the systemic therapy group (median: 20 months; p = 0.0034). This trial was the first to show a survival benefit for HAI chemotherapy despite not allowing crossover between arms. Despite the limited data showing superiority of HAI over systemic therapy, proponents of HAI point to the high rate of conversion from unresectable disease to resectable or ablatable hepatic metastases as a rationale for using HAI in patients with liver-only mCRC. Overall, the rate of conversion is slightly higher with HAI than with systemic therapy, ranging from 25 to 45% in most studies. 48 The rate of conversion may be further increased by combining HAI with systemic chemotherapy. Phase I studies have demonstrated the safety of combining FUDR HAI with irinotecan, XELOX, and FOLFOX as first- and second-line therapy, with observed response rates near 90% and median overall survival ranging from 17 to 36 months. 49 , 50
The most common toxicity observed with HAI therapy is biliary toxicity from FUDR infusion. Mild hyperbilirubinemia is often self-limited and may resolve when the dose is reduced or the infusion is held. Severe or progressive hyperbilirubinemia is often a sign of irreversible biliary toxicity with stricture formation that may require biliary stenting. The addition of dexamethasone to FUDR infusion decreases the rate of biliary toxicity from 30 to less than 10%. 51 Technical complications related to the HAI pump or catheter have been reported to occur in 12 to 41% of patients. 52
17.3.4 Percutaneous Ablation
Ablation may be performed in conjunction with open resection or may be performed laparoscopically or percutaneously. This technique may be offered in many clinical scenarios, but the most commonly encountered scenarios involve patients with limited hepatic disease (typically defined as < 3 lesions), those who are not surgical candidates, those with unresectable mCRC (in an attempt to treat lesions in the remnant liver after resection), and those with recurrent hepatic metastases. Multiple ablation modalities are available for treating tumors within the liver, including radiofrequency ablation (RFA), cryoablation, microwave ablation (MWA), and irreversible electroporation (IRE). Of these modalities, RFA has been the most extensively discussed in the literature.
RFA works by delivering thermal energy into the tissue using high-frequency alternating current, causing thermal coagulation. Cellular death occurs instantaneously at temperatures in excess of 60 °C. Most retrospective studies in the surgical literature comparing resection to RFA alone found RFA to be inferior to resection. 53 For example, RFA alone was found to have a recurrence rate of 84% and a 4-year survival rate of 22% compared to 52 and 65%, respectively, for resection. 54 Studies from the radiology literature have also reported poorer survival outcomes with RFA than with resection. 55 The median survival after RFA was found to be approximately 3 years, with a 5-year overall survival rate of approximately 25%. 53 , 56 In a comparison of RFA versus resection of solitary metastases, the two techniques demonstrated similar 3-year overall survival rates (approximately 55%). 57 As technique and patient selection have improved such that patients undergoing RFA have become similar to those undergoing resection, 5- and 10-year overall survival rates with RFA have begun to approach the rates seen with surgery. 58
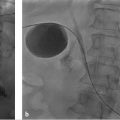
RFA remains the second best option after surgical resection in terms of recurrence and overall survival (▶ Fig. 17.1). However, given the high incidence of recurrence after resection, many clinicians support the use of ablation for oligometastatic disease because patients are spared unnecessary surgery. For example, Livraghi et al 59 found that 98% of patients with oligometastatic mCRC to the liver could be spared surgical resection by undergoing percutaneous ablation; 2% went on to surgery because of incomplete ablation. In this study, approximately half of the patients were disease free at follow-up, whereas the other half had disease that recurred within the liver or elsewhere. The authors suggested that the patients who had disease recurrence would have experienced this recurrence regardless of whether resection or ablation was used and that these individuals therefore benefited by avoiding the morbidity of hepatic resection.

Rather than considering RFA a competitor of resection, many use RFA as a complementary tool for patients with unresectable mCRC. For example, in one trial, RFA was used in combination with resection in patients with unresectable mCRC to potentially cure all metastatic disease. The 5-year overall survival rate for treated patients was 43%, which is similar to the survival achieved with resection alone. 60 Similar results have been seen in the treatment of bilateral unresectable mCRC with ablation. RFA has also been used in combination with chemotherapy for the treatment of unresectable mCRC. Ruers et al 61 found improved progression-free survival in patients randomized to receive RFA in conjunction with systemic chemotherapy (17 months) compared to those treated with systemic chemotherapy alone (10 months).
Despite the success of RFA in some studies and in different applications, this technique remains limited by the size of individual metastases. In general, tumors greater than 3 cm are more difficult to completely ablate with a single probe, and lesions greater than 4 cm almost always require the use of overlapping ablations. These size limitations affect the outcomes of RFA. For example, Livraghi et al 59 observed that the median survival for patients with hepatic mCRC lesions was 38 months for tumors less than 3 cm, 34 months for tumors between 3 and 5 cm, and only 21 months for tumors less than 5 cm. Similarly, the recurrence rate for tumors greater than 4 cm can exceed 70%. 62 An additional limitation of RFA is the potential for incomplete ablation of tumors adjacent to large blood vessels that dissipate heat from the area, the so-called heat sink effect. Also, as tissue desiccates and becomes charred, radiofrequency energy becomes less effective in heating tissue at the periphery, which may result in incomplete ablation. Furthermore, ablation near large central biliary structures is not recommended because of the potential for fistula or biliary stricture. Overall, the major complication rates for RFA are low, with complications occurring in approximately 6% of cases and death occurring in 1%. 63 The most frequently reported major complication is abscess formation in the ablation cavity. Other less common major complications include portal vein thrombosis, pleural effusion, and injury to adjacent bowel. Tract seeding from RFA is extremely rare, occurring in less than 0.2% of ablated tumors. 56 , 63
MWA uses a needle-based probe with a microwave antenna near the tip, which is inserted through a tumor under imaging guidance. When microwave energy is applied to the tissue, rapid oscillation of water molecules raises the temperature of the tissue, resulting in coagulative necrosis. This transfer of energy is more rapid and varies less with tissue composition and density compared with RFA because of the shorter wavelength used with MWA. 64 In animal models of ablation, these properties of MWA allow it to be less susceptible to heat sink and to incomplete ablation secondary to charring. 65 , 66 , 67 Although this suggests that MWA would be effective in treating larger tumors, several studies have shown that recurrence rates with MWA are higher for lesions greater than 3 cm. 68
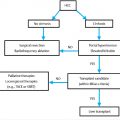
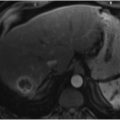
Ablation is not limited to patients with newly diagnosed mCRC or those with liver-only disease (▶ Fig. 17.2). When disease recurs after resection or ablation, survival decreases to approximately 36 months regardless of whether the recurrence is local tumor progression or new metastatic disease. 58 Treatment of these recurrences, particularly local progression, improves survival to approximately 46 months, which is still poorer than the 63-month median survival seen in those without local tumor progression. 58 Although extrahepatic disease is a poor prognostic factor, ablation should still be considered in these patients if the bulk of mCRC is within the liver. Gillams et al 56 demonstrated a median survival of approximately 2 years in patients with extrahepatic mCRC who underwent RFA of liver metastases. Although this is a year less than those without extrahepatic disease, these outcomes may still justify ablation in select cases.

17.3.5 Transarterial Embolotherapy
Multiple transarterial therapies are currently being used to treat mCRC. These interventions were initially reserved for cases of unresectable multifocal disease that had become refractory to systemic chemotherapy. However, the use of transarterial embolotherapy to treat mCRC has progressed over the past two decades.
Conventional lipiodol-based transarterial chemoembolization (cTACE) was the initial embolotherapy used to treat chemorefractory mCRC. This embolization approach uses a variety of chemotherapy agents, typically mitomycin-C, cisplatin, doxorubicin, or irinotecan, in an emulsion with ethiodized oil. Gelfoam- or starch-based embolization material may be mixed with or delivered immediately after the emulsion. 69 One randomized trial suggested that differences in the infused therapy had little effect on response. 70 , 71 Early experiences with this technique in chemorefractory disease demonstrated a positive effect, with radiologic response in 63% of cases, a median survival of approximately 8 months, and acceptable rates of mild and moderate toxicity. 72 Attempts at using cTACE as a first-line therapy for patients with mCRC with liver-only metastases have been less successful. In an early phase trial of patients with liver-only mCRC, chemoembolization before systemic 5-FU therapy was associated with an overall response rate of only 29%. Furthermore, time to progression was approximately 8 months, and median survival was only 14 months. 73 Subsequent studies of cTACE as a second-line therapy have demonstrated that cTACE leads to results that are similar to those seen with other second-line systemic therapies, although trials directly comparing systemic chemotherapy to cTACE have not been performed. 71 , 74
The evolution of TACE has brought about the development of drug-eluting beads (DEBs). DEBs contain sulfonate binding sites on polyvinyl alcohol beads, which can be loaded with doxorubicin or irinotecan via an ion-exchange mechanism. 75 The rationale behind DEB-TACE is that more controlled chemotherapy release can be achieved with this technique, resulting in a more reproducible therapy. DEBs bound with irinotecan (commonly called DEBIRI) were introduced in 2006 for the treatment of mCRC. Preclinical testing of this device in a porcine model demonstrated sustained release of irinotecan into the hepatic parenchyma with systemic plasma levels reduced by 75% when compared with bolus infusion of intra-arterial irinotecan. 75
DEBIRI has been compared to systemic therapy either alone or in conjunction with systemic chemotherapy. In a randomized trial comparing DEBIRI to FOLFIRI, the DEBIRI group had improved survival and imaging response rate (22 months and 69%, respectively) versus the FOLFIRI group (15 months and 20%, respectively). 76 A recent phase II study evaluating DEBIRI with capecitabine demonstrated the safety of this combination. 77 More recently, a trial comparing FOLFOX plus bevacizumab to FOLFOX plus bevacizumab plus DEBIRI for the treatment of mCRC demonstrated that the overall response rate was significantly higher (by 15–30%) in the DEBIRI arm at 2, 4, and 6 months (p = 0.02, 0.03, and 0.05, respectively). 78 The frequency of patients being converted to resectability more than doubled in the DEBIRI arm (to 35%) despite 56% of patients in the DEBIRI arm having extrahepatic disease compared to 32% of patients in the chemotherapy arm. Progression-free survival also doubled to 15.3 months in the DEBIRI arm. The rate of toxicity was similar between the two groups (~50%). 78
The most common side effects and adverse events associated with DEBIRI are similar to those seen with cTACE and seem to be related to postembolization syndrome. These adverse events include nausea/vomiting and abdominal pain, occurring in up to 55 and 60% of patients, respectively. Fatigue is also common. However, liver dysfunction or failure is rare, occurring in less than 5% of cases. 78 , 79 Factors associated with adverse events are embolization to complete stasis, treatment with greater than 100 mg of irinotecan in a single session, repeated embolization, degree of liver involvement by tumor, and pre-embolization bilirubin level greater than 2.0 g/dL. 79
An alternative form of transarterial embolotherapy is intra-arterial injection of nondegradable glass or resin microspheres loaded with the nearly pure beta-emitter yttrium-90 (Y-90). This technique was first introduced in the early 1980s and has evolved from being used in a single whole liver treatment session to being used in multisession lobar or segmental treatments. Y-90 has a half-life of 2.67 days, has an energy level of 0.94 MeV, and demonstrates mean and maximum soft-tissue penetration of 2.5 and 11 mm, respectively. 80 No clinically significant leaching of the Y-90 from either type of microsphere has been observed. Although a greater median radiation dose is delivered with glass microspheres, largely because the ratio of radioactivity per bead is higher for glass spheres (3–10 GBq on 4 million glass spheres) than for resin microspheres (0.75–3.03 GBq on 50 million resin spheres), no difference in response between the two bead types has been reported. 81
Radioembolization of mCRC was originally almost exclusively performed for chemorefractory disease or in patients who had developed severe toxicity to systemic therapy. Compared to patients treated with best supportive care for chemorefractory disease, which provides an overall survival of less than 6 months, patients treated with radioembolization typically experience an overall survival of 10.5 months and a 2-year survival rate of approximately 20%. 82 Prospective phase II studies of chemorefractory mCRC have demonstrated a median overall survival of approximately 12 months even though most patients in these studies had received ≥ 4 lines of chemotherapy before radioembolization. In this heavily treated cohort, liver failure after embolization was rare, occurring in only a single patient. 83 Factors associated with improved outcomes after radioembolization of chemorefractory mCRC are smaller tumor volume, liver-only disease, and response to radioembolization. 84 , 85 In this population, patients who demonstrate an imaging response to radioembolization can have an overall survival that is twice as long as those who have progression or no response after therapy. 83
Researchers have also begun to explore the combination of radioembolization and systemic therapy. A phase I trial of radioembolization plus second-line systemic therapy with irinotecan failed to reach the maximum tolerated dose. 86 Although approximately 50% of patients had grade 3 (G3) toxicities or greater, these toxicities were similar to those previously reported for irinotecan-based therapies. The outcomes of this early phase trial were promising, with progression-free and overall survival of 6 and 12 months, respectively. 86 Radioembolization has also been studied in combination with first-line systemic therapy. 87 , 88 Based on the promise of early phase studies using radioembolization with 5-FU/L or FOLFOX, two large phase III trials were planned: the SIRFLOX trial, which examined progression-free survival, and the FOXFIRE trial, which aims to examine overall survival and has just completed enrollment. 89 Although the addition of radioembolization to FOLFOX first-line chemotherapy did not improve progression-free survival overall (~10 months) in the SIRFLOX trial, a significant delay in tumor progression within the liver was seen with the addition of radioembolization (20.5 months) compared to chemotherapy only (12.6 months) in patients with mCRC that was either liver-only (60%) or liver-dominant (40%) disease (HR: 0.69; 95% CI: 0.55–0.90; p = 0.002). 89
As with cTACE and DEBIRI, the toxicity and complications of radioembolization are caused by the treatment itself, destruction of normal hepatocytes, and improper delivery to extrahepatic viscera. Postradioembolization syndrome is similar to postembolization syndrome but consists of fatigue and cachexia more commonly than nausea/vomiting or abdominal pain. Reported rates of toxicity range from 20 to 70%. Despite this frequency, toxicity from radioembolization is only rarely severe enough to necessitate hospitalization. 90 , 91 The most feared complication of radioembolization is liver failure from destruction of normal hepatocytes, termed radioembolization-induced liver disease. 92 Severe radioembolization-induced liver disease, which is most often fatal or at the least will cause severe enough toxicity to prevent additional systemic therapy, occurs in 2 to 13% of cases. The factor most commonly associated with radioembolization-induced liver disease in noncirrhotic patients is prior systemic chemotherapy in the 2 months preceding radioembolization. 92
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree