21 Pancreatic Cancer
Govindarajan Narayanan, Elizabeth Anne Hevert, and Shree Ramanan Venkat
21.1 Introduction
Pancreatic cancer is an uncommon condition, accounting for approximately 3% of all cancer cases in the United States; however, this disease is the third leading cause of cancer-related deaths. 1 , 2 Pancreatic cancer has a dismal prognosis with a median survival of approximately 4 to 6 months. 3 This prognosis is in part related to difficulties in diagnosis, with clinical symptoms that do not manifest until the later stages of the disease. Although mortality rates for the other major cancer types in the United States have decreased over the past decade, overall survival for patients with pancreatic cancer has not significantly improved despite technological improvements in diagnosis and surgical improvements in management. 1
21.2 Types of Pancreatic Cancer
Pancreatic cancer can arise from the exocrine and endocrine portions of the pancreas. The majority of cases (96%) develop from the exocrine portion of the gland, which includes the ductal epithelium, the acinar cells, the connective tissue, and the lymphatics. 4 The remaining 4% arise from the endocrine portion of the pancreas or the islet cells; these cases are referred to as pancreatic neuroendocrine tumors. 5 Of the pancreatic exocrine neoplasms, approximately 90% are adenocarcinomas of the ductal epithelium. 6
21.3 Epidemiology
It is estimated that more than 48,000 new cases of pancreatic cancer are diagnosed each year. 4 The incidence of pancreatic cancer is comparable between men and women but is remarkably higher in African Americans than in Caucasians. 4 , 7 An increased incidence of pancreatic cancer has also been observed in less developed countries, which is postulated to be related to the adoption of cancer-causing behaviors such as tobacco use (increases risk by 20%) and high-calorie diets. 4
21.4 Risk Factors
Multiple modifiable and nonmodifiable risk factors have been implicated in the development of pancreatic cancer, and these factors may act in an additive or synergistic fashion. Research into these risk factors has provided insight into the disparities of cancer incidence among patients of different sexes and backgrounds. 8 , 9
The modifiable risk factor most highly associated with pancreatic cancer is tobacco use, which has an attributable risk of approximately 20 to 25%. 7 Although smoking is often accompanied by excessive alcohol use, there is only a weak association between alcohol consumption and pancreatic cancer risk. 7 Type 2 diabetes is a moderate risk factor for pancreatic cancer; patients with long term (> 10 years) diabetes have a twofold increased risk of developing pancreatic cancer. 7 , 10 Obesity and dietary practices have also been suggested as modifiable risk factors but research into these factors has produced mixed results. 11 The risk of developing pancreatic cancer has also been related to chronic pancreatitis; patients with chronic pancreatitis have as high as a 14-fold increased risk of developing pancreatic cancer. The risk of cancer development among these patients increases linearly over time because of the accumulation of genetic mutations (e.g., mutations of the KRAS gene). 7 , 12 , 13
21.5 Genetics
Investigations into the molecular genetics of pancreatic cancer have highlighted the highly complex and heterogeneous nature of this disease. Only 5 to 10% of pancreatic cancers are categorized as hereditary in nature, meaning that the vast majority of cases are sporadic. 7 , 12 The occurrence is believed to be due to an accumulation of germ line and somatic genetic mutations as dysplasia progresses to carcinoma. 12
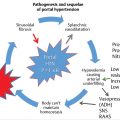
More than 90% of patients with pancreatic cancer have mutations in the KRAS2 gene, which encodes a GTPase that mediates downstream signaling for growth factor receptors. 13 In addition to KRAS mutations, three-tumor suppressor genes are frequently mutated in the setting of pancreatic cancer. The tumor suppressor gene CDKN2 encodes a cell cycle regulator and is inactivated in more than 90% of pancreatic cancer cases, leading to increased cell proliferation. 12 P53 tumor suppressor gene mutations are encountered in approximately 75% of pancreatic cancer cases. In addition to this, somatic inactivation of SMAD4 occurs in approximately 55% of pancreatic cancer cases. The heterogeneity of this disease is further highlighted by the fact that although these four mutations are the most commonly encountered mutations in the setting of pancreatic adenocarcinoma, only 37% of patients have all the four mutations. 14 The activation of growth factors causes pancreatic stellate cells (myelofibroblasts) to produce the extensive desmoplastic reaction implicated in causing poor vascularization of the tumor. 12
The genetic complexity of pancreatic cancer complicates the treatment of this disease and may partially explain the high incidence of chemotherapy and radiation resistance seen in this setting. However, this genetic complexity also offers possible future targets for molecular therapy.
21.6 Presentation
The signs and symptoms of pancreatic cancer are nonspecific and subtle in onset, frequently leading to a delay in diagnosis and more advanced stage at presentation. The median age of patients at diagnosis is 70 years. 1 One of the more commonly encountered clinical symptoms is abdominal pain; however, because of the vague nature of this complaint, it is commonly erroneously attributed to a different pathology. More than one-fourth of patients with pancreatic cancer will have no pain at diagnosis. Symptoms of pancreatic cancer, including significant weight loss, painless obstructive jaundice, ascites, and migratory thrombophlebitis, become more clinically apparent with more advanced disease. 4 , 12
The laboratory findings in pancreatic cancer are also nonspecific; these findings may include normochromic anemia or thrombocytosis. As with the clinical presentation, laboratory findings are often not abnormal until the more advanced stages of the disease. Such abnormal findings may include elevations of bilirubin, alkaline phosphatase, and gamma-glutamyl transpeptidase levels in the setting of obstructive jaundice. Serum amylase and lipase levels are increased in less than half of patients with resectable pancreatic cancers and are increased in only one-fourth of patients with nonresectable tumors. The presence of liver metastasis may lead to mild elevations of aspartate aminotransferase and alanine aminotransferase levels.
Approximately 5% of patients with pancreatic cancer will initially present with acute pancreatitis; therefore, pancreatic cancer should be included in the differential diagnosis for an elderly patient with new-onset pancreatitis without other known precipitating factors. The sudden onset of type 2 diabetes mellitus in a patient aged more than 50 years may also suggest that pancreatic cancer is the underlying etiology for pancreatic dysfunction. 10
Considerable research has been conducted to identify reliable biomarkers that will aid in early detection and provide information regarding prognosis and potential treatment response. At present, CA 19–9 is the only FDA-approved blood test for the assessment of pancreatic ductal adenocarcinoma. CA 19–9 is a sialylated oligosaccharide that is frequently found on circulating mucins in patients with cancer. Unfortunately, the antibody for CA 19–9 targets Lewis antigens with a specific fucosylation pattern; approximately 10% of patients have these antigens (Lewis a and b) and therefore cannot express CA 19–9 and will not test positive for CA 19–9 even in the setting of a high tumor burden. 12
21.7 Imaging Diagnosis
The role of imaging in the setting of pancreatic cancer goes well beyond diagnosis and can include both disease staging and determination of resectability of local disease. Transabdominal ultrasonography (US) has limited utility in the diagnosis of pancreatic carcinoma because the pancreas can be obscured on these scans by overlying gas in the stomach or bowel. The overall sensitivity for the detection of pancreatic cancer with US is approximately 60 to 70%, and the sensitivity is considerably lower for smaller lesions. 15 Endoscopic US obviates the physical limitations of abdominal ultrasound through the use of a high-frequency transducer that is positioned within the stomach or duodenum in close proximity to the pancreas. 15 This technique has demonstrated superiority to computed tomography (CT) for the detection of pancreatic cancer, particularly for small tumors, and offers the diagnostic advantage of simultaneous US-guided biopsy and sampling of adjacent lymph nodes. 16
The imaging mainstay for the assessment of suspected pancreatic cancer is CT. Advances in multidetector CT technology have dramatically improved the sensitivity of this modality for the detection of pancreatic cancer to approximately 97%. 15 , 17 One of the advantages of CT scanning is its accuracy in delineating the arterial and venous vascular involvement. This is important in the evaluation of locally advanced disease, as there is a distinct subset of tumor that blurs the distinction between resectable and locally advanced disease (deemed “tumors of borderline resectability” or borderline LAPC). Pancreatic adenocarcinomas on CT imaging are typically ill defined, hypovascular tumors that are poorly enhancing, appearing on arterial phase imaging as hypoattenuating lesions juxtaposed on the background of avidly enhancing normal pancreatic parenchyma. Approximately 5% of tumors are isodense to parenchyma on CT because of relatively lower tumor cellularity and a lesser degree of necrosis. 18
Magnetic resonance imaging (MRI) offers soft tissue contrast superior to that of CT for pancreatic imaging. On MRI, the normal parenchyma demonstrates increased T1 signal intensity secondary to the high quantity of acinar proteins, and the pancreas demonstrates homogeneous avid arterial enhancement. The dense fibrous stroma of pancreatic adenocarcinoma results in hypointense T1 signal on T1 fat-saturation sequences; these hypovascular, poorly enhancing characteristics make the lesions more conspicuous on contrast-enhanced examinations. 15 Diffusion-weighted imaging is also helpful in identifying solid masses as compared with cystic masses. Due to the closely packed cellularity and dense fibrous stroma of pancreatic adenocarcinomas, these lesions will typically restrict diffusion and demonstrate low apparent diffusion coefficient (ADC) values. 19 MRI provides an advantage over CT in the setting of small tumors, particularly those smaller than 2 cm, and in the identification of the 5% of pancreatic cancers that are the same attenuation of background parenchyma on CT. 19
Positron emission tomography (PET) using 18F-FDG to serve as a marker for glucose metabolism can also be used to assess pancreatic cancer. The loss counts from attenuation as PET images are acquired results in increased noise and image distortion therefore integrated PET-CT scans are simultaneously acquired and co-registered, allowing for accurate localization of abnormal radiotracer uptake. PET-CT is useful in differentiating between benign and malignant pancreatic lesions, with a positive predictive value of 91%. 20 Unfortunately, PET-CT is associated with a high number of false negatives, and imaging resolution is poor for lesions sized smaller than 8 mm. However, PET-CT is effective in distinguishing between autoimmune pancreatitis, which demonstrates a diffuse radiotracer uptake pattern, and malignancies, which typically demonstrate a more focal area of radiotracer uptake.
21.8 Tumor Staging
Based on the TNM classification, tumors are categorized as locally resectable (stage I or II), locally advanced (stage III), or unresectable for metastatic disease (stage IV). 12 Approximately 20% of patients with pancreatic adenocarcinoma present with stage I or II disease. 4 T1 tumors are no more than 2 cm in size, whereas T2 tumors are larger than 2 cm in their greatest dimension. T3 disease describes tumor extension beyond the pancreas but not involving the celiac axis or superior mesenteric artery. 21
Resectable tumors are traditionally those that do not involve the arterial or venous vasculature. Truly unresectable disease demonstrates greater than 180° involvement by the tumor of the superior mesenteric artery, greater than 180° involvement of the celiac or hepatic artery, and occlusion of the superior mesenteric vein/portal vein without surgical options for reconstruction. 15 , 21 Borderline resectable tumors include those tumors that involve less than 180° of the superior mesenteric artery circumference, short segment encasement or abutment of the hepatic artery, and short segment occlusion of the superior mesenteric vein/portal vein with technical options for surgical reconstruction. 17 Accurately distinguishing between these entities is of paramount importance to describe the tumor vessel interface, as the treatment strategies will differ accordingly. 3D reconstruction tools, including the generation of 3D maximum intensity projection (MIP) and 3D volume-rendered images, are being increasingly used for tumor staging with respect to vascular involvement. These tools also offer additional information that can be important for surgical planning. 22
The presence of lymphadenopathy is becoming less important in the imaging evaluation of pancreatic adenocarcinoma, as peripancreatic lymph nodes are frequently resected with the specimen during surgery. Cases are rarely deemed unresectable at the time of surgery because of the presence of lymphadenopathy.
A significant factor contributing to the very poor prognosis in patients with pancreatic adenocarcinoma is the early extrapancreatic invasion of this disease and its tendency for metastatic spread. Pancreatic cancer first metastasizes to regional lymph nodes, with the liver serving as the most common primary site of metastatic disease. One of the characteristic modes of disease spread is perineural invasion resulting from malignant infiltration along the neural fascicles; neurotropic factors found within the pancreatic stroma appear to facilitate this process. Even small pancreatic cancers (< 2 cm) have demonstrated a high frequency of perineural invasion. The presence of extrapancreatic disease portends a worse prognosis, often resulting in positive surgical margins and increasing the likelihood of recurrence. Assessment for extrapancreatic disease should include evaluation for confluent soft tissue invasion along a known pathway of the peripancreatic neural plexus. 23
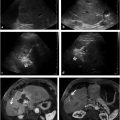
A typical CT imaging finding in cases of liver metastasis from pancreatic adenocarcinoma is the presence of a hypovascular lesion that is usually best visualized during the portal venous phase. 15 , 22 MRI is substantially more sensitive for the detection of small liver metastases and can more readily differentiate between malignant and benign entities. 22 Metastatic lesions in the liver are typically hypointense on T1-weighted images and mildly hyperintense on T2-weighted images as opposed to cystic lesions, which demonstrate increased signal on fluid-sensitive sequences. Most metastatic lesions will demonstrate peripheral contrast enhancement on arterial phase imaging, which can help to delineate the pathology. 22 PET-CT has a sensitivity as high as 88% for the evaluation of metastatic disease. 20
In the setting of metastatic disease, especially in the liver, US-or CT-guided biopsy may be performed. Endoscopic US is favored for biopsy of the primary lesion. 18 This technique used with fine needle aspiration has a negative predictive value of 100%. 15 Complications with this procedure are rarely reported (< 3%), with the greatest risks including bleeding and pancreatitis. 15
21.9 Treatment
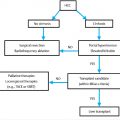
Consensus guidelines for pancreatic cancer suggest that the initial approach to disease evaluation should include diagnosis, staging, and evaluation of performance status followed by multidisciplinary treatment strategies including chemotherapy and/or radiotherapy combined with surgical resection or percutaneous ablative techniques.
21.9.1 Chemotherapy
As indicated above majority of patient present at advanced stages with approximately 35% of patients with pancreatic cancer present with locally advanced (stage III) disease more than 50% of patients present with metastatic disease. In these patients, chemotherapy-based regimens are the treatment of choice, with the patient′s Eastern Cooperative Oncology Group (ECOG) performance status directing the choice of regimen. Despite the advances that have been made in chemotherapy, the average median survival for patients with metastatic disease is approximately 11.1 months with first-line FOLFIRINOX (leucovorin and fluorouracil plus irinotecan and oxaliplatin) therapy. 24 This is an improvement over the median survival in patients treated with gemcitabine, which is approximately 7 months. 24 In patients aged older than 75 years, the combination of gemcitabine and nab-paclitaxel has been shown to increase median survival to 8.5 months. 25 Current guidelines for patients with metastatic disease recommend the use of systemic chemotherapy. If FOLFIRINOX can be tolerated (common side effects include neutropenia, fatigue, diarrhea, neuropathy, and thrombocytopenia), this agent is favored over a regimen of gemcitabine plus nab-paclitaxel. Second-line therapy is not well defined in this patient population.
In patients with locally advanced disease, the goal of therapy is to downstage the disease to make the case eligible for resection. In a recent meta-analysis evaluating the use of FOLFIRI-NOX for locally advanced disease, the median overall survival was 24.2 months with FOLFIRINOX compared with 13 months with gemcitabine. 24 Rates of resection after treatment with FOLFIRINOX ranged from 0 to 43%. 24 Negative margins (R0) were achieved in 74% of the patients who underwent resection after receiving FOLFORINOX suggesting that there may be a role for neoadjuvant FOLFIRINOX even in resectable cases. 24 , 25 Multiple phase 2 trials exploring the role of FOLFIRINOX and nab-paclitaxel/gemcitabine in the neoadjuvant setting are currently under way for example the NEPAFOX and NEONAX studies. 26
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree