25 Metacarpal Fractures
Most metacarpal fractures can be adequately identified with radiographs in two planes. Further diagnostic imaging with high-resolution CT is only necessary for dislocated fractures of the bases and heads of the metacarpals. Functionally, the exact position of metacarpals II–V together with the transverse palmar arch is a prerequisite for undisturbed, convergent movement of the fingers, while the integrity of the trapeziometacarpal joint is essential for unrestricted abduction and opposition of the thumb. This makes detection of subtle displacements of fragments in the metacarpus especially important.
Pathoanatomy and Symptoms
Fractures of the metacarpals, including the thumb, are caused either by direct traumas (e.g., crush injuries) or indirect traumas (e.g., falls). Subcapital fractures usually occur during a fall on the closed fist, whereas fractures of the metacarpal heads are often the result of direct force applied to the extended hand. Clinical complaints, which are considerable in Bennett’s fractures, include pain, swelling, and usually limited range of motion in the fractured finger ray. Table 25.1 lists the different types of fractures, which are categorized according to their location and the fracture course.
Diagnostic Imaging
Radiography
If fracture of the metacarpals is suspected, radiographs of the metacarpus in dorsopalmar and oblique planes that include the carpometacarpal (CMC) and metacarpophalangeal joints should be taken. After a recent injury, the dorsopalmar view of the thumb often cannot be taken in hyperpronation. There are special views for visualizing the trapeziometacarpal joint of the thumb (Kapandji’s special trapezium view) (Chapter 1). Fractures of metacarpal shaft and neck can be readily identified identified in survey views, but not fractures of the metacarpal bases and heads. The following rules apply for assessment of the extent of dislocation:
The shortening of a metacarpal is assessed according to the connecting line along the heads of metacarpals III–V (so-called “metacarpal sign”). Normally the line connects the metacarpals III–V, whereas the metacarpal II is considerably below these straight lines.
A strictly lateral view of the metacarpus is required to assess a palmar tilt in the axis of the peripheral metacarpal fragment. Clinically, remaining fragment dislocations on the ulnar side of the metacarpals are tolerated better than those on the radial side.
To check for malrotation after a fracture, it must be clinically assured that, when all finger joints are flexed, the pulps of the individual fingers converge in the direction of the scaphoid tubercle and do not cross. Malrotation cannot be diagnosed on radiographs, but with clinical examination, and usually indicates surgical treatment.
|
Computed Tomography
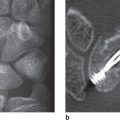
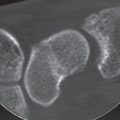
As explained in Chapter 24, fractures of the metacarpal bases often require CT imaging to provide clarity when radiographic findings are uncertain and to determine the pattern of injury ( Figs. 25.2 , 25.3 ). Computed tomography is also generally indicated in comminuted fractures of the metacarpal heads, whose extent and displacement often can be identified only in 2D and 3D image reconstructions ( Fig. 25.6 ).
If the patient tolerates the positioning, sagittal CT slices are useful. To avoid streaky artifacts on the forearm (off-center artifacts), the metacarpals II and III are scanned in ulnar inclination of the wrist and the metacarpals IV and V in radial inclination. The slice thickness should be between 0.5 and 1.0mm, with overlapping increment. Coronal multiplanar reconstruction (MPR) images are computed from sagittal source images. If necessary, axial MPR images can also be computed. Three-Dimensional surface images are useful for planning surgery for complex fractures of the metacarpal head, espe especially when they depict the fracture area after electronic exarticulation of the less-affected joint partner (Fig. 25.1c).
Magnetic Resonance Imaging
MRI is of no importance in metacarpal fractures. Contrast-enhanced MRI is the method of choice to identify injuries to the collateral ligaments on the metacarpophalangeal joints (see Fig. 29.18 ) and the palmar plate.
Pattern of Injury
Fractures Close to the Base of Metacarpal I
Fractures of the base of the metacarpal I are of special interest since the trapeziometacarpal joint of the thumb is extremely mobile because of the shape of the joint surfaces and tension exerted by the attached muscles. Intraarticular fractures are differentiated from extra-articular fractures:
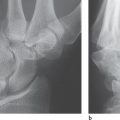
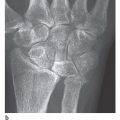
Bennett’s fracture: This describes an intra-articular, single-fragment fracture of the metacarpal I (Fig. 25.1a). Radiographs show the fracture through the base of the metacarpal I. The large shaft fragment dislocates in dorsoradial direction, whereas a small ulnar fragment remains in place because of its ligamentary fixation on the trapezium. The displacement is maintained by tension from the abductor pollicis longus muscle, which is attached to the base of the metacarpal I. Therefore, surgical stabilization is required after reduction, as immobilization in a cast is generally insufficient. Intraoperative and postoperative radiographic follow-up, sometimes with oblique views, is necessary to check that the fragments remain correctly reduced.
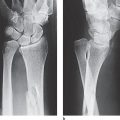
Rolando’s fracture: This describes an intra-articular multiple-fragment fracture of the base of the metacarpal I (Fig. 25.1b, c). There are Y-shaped, T-shaped, and often comminuted compression fractures. Tension from the attached muscle generally causes considerable dislocation, which requires open reduction and stabilization.
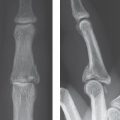
Winterstein’s fracture: In contrast to Bennett’s and Rolando’s fractures, this is an extra-articularfracture of the base of the metacarpal I (Fig. 25.1d). The distal shaft fragment mostly has a rather severe palmar tilt.

Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree