28 Enthesopathy
Enthesopathy is a pathologic process at the bony attachments of ligaments, tendons and joint capsules. Fibro-ostosis arising from degenerative, endocrine, or metabolic processes must be differentiated pathogenetically from fibro-ostitis having an inflammatory origin. Pathology of the latter is associated either with an osteoresorptive or osteoproliferative pattern. Characteristic radiographic signs may allow identification of the specific pathologic process among a multitude of disease entities.
Pathoanatomy and Clinical Symptoms
The term “enthesopathy” describes all lesions caused by a number of different diseases of the fibro-osseous junction, defined as the region where the ligaments, tendons, and joint capsules have their bony attachments. Two anatomic conditions must be differentiated:
On the diaphyses of the long tubular bones, the ligaments and tendons radiate directly into the bone matrix via a perosteal insertion. The fibers of the joint capsule also insert directly into the bone
In contrast, the periosteum is not involved in the epiphyseal and apophyseal insertions. A zone of fibrous cartilage, which buffers the mechanical load, lies between the bone and the attachments.
Chronic strain and inflammatory processes lead to neovascularization reactions at the fibro-osseous junctions of tendons and ligaments, the joint-capsule insertion, and the intermediate cartilaginous zone. This pathomechanism can trigger ossifications of the tendons, ligaments, and capsular attachments. Endocrine or metabolic osteoplastic diatheses can also cause calcium deposition at the fibro-osseous transitions.
classification
Two disease entities are differentiated according to their pathogenesis and morphology ( Table 28.1 ).
Diagnostic Imaging
Radiography
Radiographic views with a conventional film-screen combination (sensitivity 200) or with a storage-screen system (2K technique) are generally sufficient to depict enthesopathic lesions at the fibro-osseous junctions. When the etiology of the documented changes remainsambiguous, complementary views in mammography, soft radiation, and magnification techniques can provide additional information. Optimized techniques provide significantly better visualization of lesions of the fibro-osseous and the surrounding soft tissues, such as swellings, displaced or obliterated fat lines, and tiny calcifications. These procedures occasionally allow further differentiation of the underlying disease according to degenerative, metabolic, endocrine, or inflammatory etiology.
Ultrasonography, CT, and MR Imaging
Resorptive and proliferative bone lesions can be recognized with high sensitivity with CT. The enthesiopathic soft-tissue components in the fibro-osseous junction can, in principle, be identified with high-resolution ultrasonography as well as with MRI. An acute inflammatory process can be well differentiated from a “burned-out” fibro-ostitis or fibro-ostosis with fat-suppressed or STIR sequences. Intravenous administration of contrast agent can provide further valuable information, e.g., in the differentiation of stages of rheumatoid arthritis according to the degrees of activity. For further explanations of the very different (synovial) disease entities, see Chapters 27, 29, and 34–40.
Disease Entities
Predominantly Fibro-ostotic Changes
Degenerative Diseases
Osteoarthritis
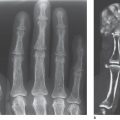
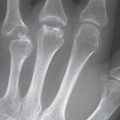
One of the characteristics of deforming osteoarthritis is the insertional spur, the enthesophyte. This has smooth contours, cortical margins, and a regular trabecular structure. Fibro-ostotic changes on the hand mainly affect the insertions of joint capsules on the proximal and distal interphalangeal joints ( Fig. 28.2 ). Tension on the proximal capsular insertion can cause very large spurs.
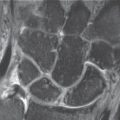
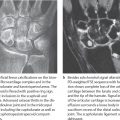
Carpal Humps
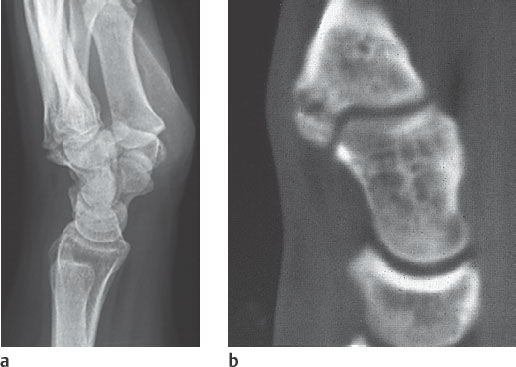
Synonymous terms for carpal humps are carpal bossing and carpe bossu. These are generally asymptomatic bony humps originating from the dorsal aspect of the metacarpals II and/or III and/or of the capitate and the hamate (Fig. 28.1a). Occasionally they cause pain and limited range of motion. These spurs can originate from an osteophyte (as fibro-ostosis) or a secondary ossification center (as os styloideum). Since the bony hump is often insufficiently visualized in the lateral radiograph, sagittal CT (Fig. 28.1b) should be performed in equivocal cases.
Endocrine Diseases
With the exception of forms of hyperparathyroidism, these are usually osteoplastic diatheses.
Diabetes Mellitus
Diabetes mellitus is associated with an increased incidence of fibro-ostotic changes, including diffuse idiopathic skeletal hyperostosis (DISH, Forestier disease) ( Fig. 28.2 ). The osteophytes are characterized by their occasionally grotesque size and shape. An enthesopathic component is also connsidered for periarthritis, Dupuytren’s contracture, and tenosynovitis of the flexor tendons, all of which occur with high incidence among diabetics. The diagnosis is generally made clinically and confirmed with MRI or ultrasonography. Radiographs are generally unremarkable, especially in the very painful early stages of diabetes. At most, a swelling of the soft tissue can be identified.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree