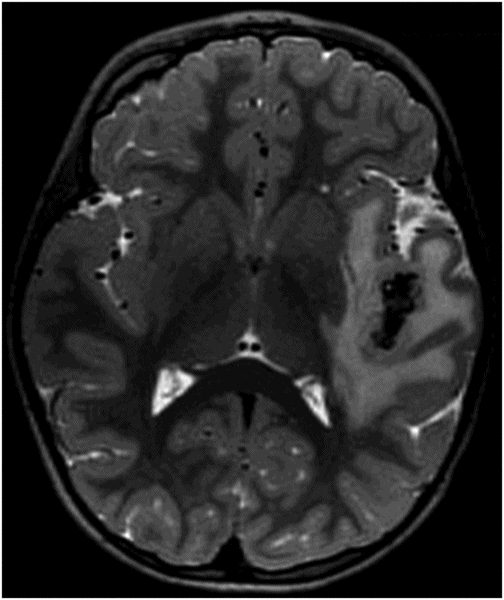
Axial T2WI.
Meningioangiomatosis
Primary Diagnosis
Meningioangiomatosis
Differential Diagnoses
Meningioma
Cavernous malformation
Arteriovenous malformation
Imaging Findings
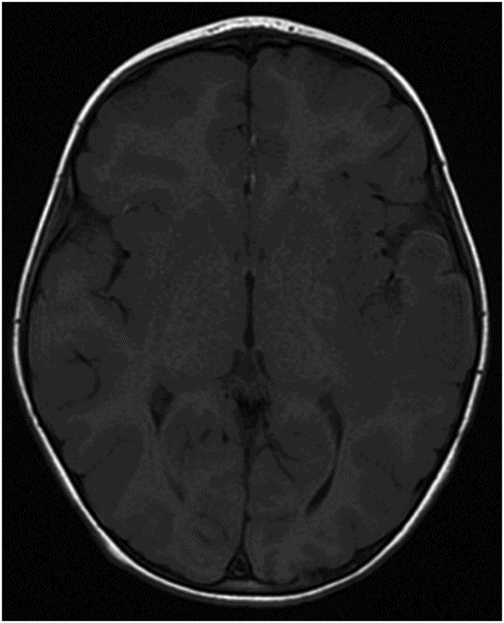
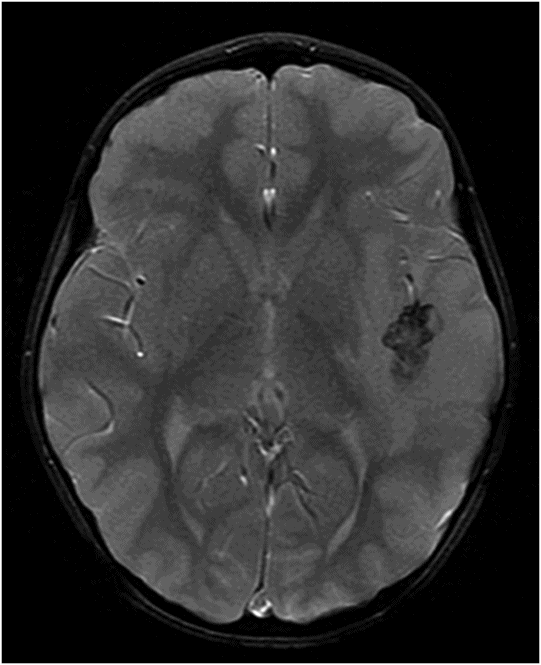
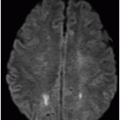
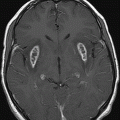
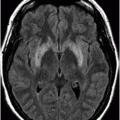
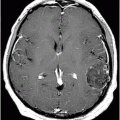
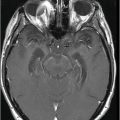
Fig. 84.1: Axial CT image showed a peripheral serpiginous/gyriform calcified lesion, associated with adjacent moderate vasogenic edema, located in the posterior left insular cortex/subcortical tissue, subjacent to the left sylvian fissure. Fig. 84.2: Axial T1WI demonstrated an ill-defined, isointense mass, with edematous adjacent white matter in the left sylvian fissure and adjacent cortex. Fig. 84.3: Axial T2WI better demonstrated the edema involving the left temporal and insular regions, and the signal loss from the calcified lesion. Fig. 84.4: Axial T2* gradient: Axial T1WI postcontrast image demonstrated an irregular ring-enhancing lesion adjacent to the cortex in the temporal and insular region. Note that the nodule has irregular contours.
Discussion
The clinical presentation of generalized tonic-clonic seizures in a young person, combined with characteristic gyral calcifications, and an enhancing lesion on imaging, is very suggestive of meningioangiomatosis (MA).
Meningioma is usually a dural-based tumor that frequently presents with thickening of the adjacent dura (dural tail sign), rather than as a cortical/subcortical lesion, such as MA. However, if the MA lesion is focal and nodular, then meningioma should be considered in the differential diagnosis. Venous vascular malformation or cavernous malformation can affect any areas of the brain, including the cortical/subcortical areas. However, on both T1WI and T2WI MR imaging, they are usually heterogeneous in appearance because of the presence of hemorrhage of different ages and have a characteristic surrounding hypointense rim on T2WI and GRE images due to hemosiderin deposition. None of these features is present in this patient’s images. No prominent vascular flow void or nidus was noted on imaging to suggest arteriovenous malformation.
Meningioangiomatosis is a benign and rare hamartomatous lesion that typically involves the leptomeninges and adjacent cortical tissue. Previously, MA was thought to represent either atypical vascular malformations or direct brain infiltration of a leptomeningeal meningioma. More recently, authors have defined MA masses as congenital hamartomatous lesions with meningothelial cell proliferation of the leptomeninges and underlying cortex. Meningioangiomatosis may occur sporadically and in association with neurofibromatosis type 2 (NF2), meningiomas, oligodendroglioma, and/or arteriovenous malformation.
Meningioangiomatosis is more frequent in males than in females, with no propensity to grow. It more commonly affects children and young adults, with up to 85% of the patients being less than 30 years of age. Sporadic MA is at least four times more common than if associated with NF2. Headaches and seizures (typically refractory to treatment) are the most common clinical presentation of MA, with seizures alone being the more prevalent clinical problems, occurring in 81% of patients with MA.
Lesions are more frequently located in the frontal and temporal regions and more commonly in the right hemisphere. Some MA lesions may not be depicted in non-contrast-enhanced CT, as they may not present with calcification. Varying degrees of lesional calcification are identified in up to 90% of cases. Lesional calcification may be focal, extensive, or patchy. Approximately 50% of cases present as hypodense lesions, which enhance after contrast administration. These lesions are typically nodular in appearance (less frequently irregular in contour), firm and well circumscribed, measuring around 3 cm in diameter.
Meningioangiomatosis almost always demonstrates abnormal MRI. These lesions are typically hypointense on T1 and hyperintense on T2 with gyriform FLAIR hyperintensities. Cystic changes and T2* susceptibility artifacts have also been described. The most common and typical imaging findings include intense contrast enhancement in up to 80% and variable calcification in up to 90% of cases. Another important imaging characteristic of MA is variable amount of perilesional edema and mass effect, which can occur in up to one-half of the cases. These lesions are not seen on catheter angiogram.
Besides its rarity, MA poses a significant challenge in diagnosis, based solely on imaging findings. The main differential diagnosis includes meningiomas, cavernous malformations, and other vascular pathologies. The most typical clinical and imaging scenario is of a young individual with headache and difficult-to-control seizures, who presents with a calcified lesion identified on CT and a puzzling mass on MRI.
Microscopic pathology findings include meningovascular proliferation with or without leptomeningeal calcification, which can extend into the perivascular spaces, sparing the white matter. The hallmarks of MA lesions include proliferation of small vessels within the cortex, concentric perivascular proliferation of spindle-shaped cells with fibrosis (perivascular cuffing), and calcification.
Meningioangiomatosis is typically treated with en bloc resection, with 100% seizure control. There is no need for an expanded excision of the surrounding brain tissue. No adjuvant therapy is usually needed. Recurrence does not usually occur.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree