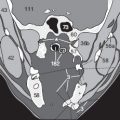
Abdominal CT
In general, all soft-tissue organs should appear uniform and be well defined, except when partial volume effects occur (cf. p.14) or during the early arterial phase of CM enhancement in a helical scan (cf. pp.120 and 126). Structures such as blood vessels and bowel loops should be clearly defined in intra-abdominal fat. The same applies to the fat in muscles.
Poorly defined connective-tissue spaces may indicate edema or an inflammatory or malignant infiltration. If the anatomy cannot be clearly resolved, additional information can be gained by measuring the density of specific areas or by comparing unenhanced with CM-enhanced scans (cf. pp. 15 and 121).
Again, the proposed checklist is not intended to be “prescriptive”, but to give an useful tool for the novice in order to reduce the number of missed pathological findings.
Selection of Image Plane
The sections of the abdomen are also acquired transversally (=axially). If the table advance is set at 8 mm with a slice thickness of 10 mm, there will be an overlap of 1 mm on each side of the section. In recent years, there is a trend towards thinner slices with a slice thickness between 5 and 8 mm.
The small topograms on the following pages (based on Fig. 102.1 ) clearly show the slice positions as related to the anatomy of major structures for each series of images.

Systematic Sequence for Readings
Analogous to interpreting chest CTs, we suggest you begin with the tissues of the abdominal wall. Considerable time is saved if you consistently look at them from cranial to caudal. For beginners a systematic inspection of each organ or system from cranial to caudal is recommended, so that you do not need to concentrate on too many structures at once. The proposed procedure encompasses two or three passages through the images. As you become experienced, you may wish to devise your own method. Experienced readers are more easily able to detect all pathologic changes in one passage from cranial to caudal.
It is sensible to evaluate internal organs that lie in the same transverse plane. The uniformity of the parenchyma, the size and the smooth surface of liver and spleen should be checked together. The same is true for the assessment of the pancreas and the adrenal glands: they also lie at the same level (cf. pp. 104/105). If the entire urinary system is to be examined, it saves time to inspect the reproductive organs and bladder in the lesser pelvis before looking at the cranial parts of the GIT, or the regional lymph nodes and the retroperitoneal vessels (see checklist on the right).
Finally, the presence of sclerotic and lytic bone lesions and the state of the spinal canal should be checked (cf. p.155).
Checklist for Abdominal Readings
The images of the abdominal organs include the costodiaphragmatic recesses of the lungs (84), which extend quite far caudally, laterally, and dorsally. Liver (122) and spleen (133) parenchyma usually appear homogeneous without focal lesions in the venous phase of CM enhancement: branches of the hepatic veins (103) can be distinguished. In order to assess the gastric wall (129a), the stomach (129) can be filled with water, which acts as a low-density CM, after an i.v. injection of Buscopan. The diaphragm (30) between the thoracic and abdominal cavities has an attenuation similar to the parenchyma of the liver and spleen and can therefore not be differentiated from these organs if its thin dome is sectioned obliquely.






The right adrenal gland usually lies cranial to the upper pole of the kidney (135), whereas the left adrenal gland lies ventral to the upper pole of the kidney. Consequently, the two adrenal glands (134) are seen on the same sections.
Note the position of the diaphragm (30) between the lung (84) and the inferior vena cava (80). The vessels on the lesser curvature of the stomach (109) and the gastric walls (129a) are usually well defined and clearly demarcated in the surrounding fat and connective tissue (2).







Typically the pancreas (131) has well-defined parenchyma with an irregular outline. The head and uncinate process of the pancreas extend quite far caudally (down to Fig. 107.3 ).
The left adrenal gland (134) is often Y-shaped, whereas the right adrenal gland may look like an arrow or a comma. Note the origin of the celiac trunk (97) and the SMA (106) from the abdominal aorta (89). Enlarged lymph nodes may frequently be found in this vicinity. Branches of the portal vein (102) and the falciforme ligament (124) can be distinguished.






Look for arterial calcifications in the origins of the renal arteries (110) at the level of the renal veins (111). The left renal vein does not always pass between the aorta (89) and the SMA (106) to the inferior vena cava (80), as it does in Figure 106.1 . Anatomic variations are not unusual (cf. p.116). Benign cysts frequently occur in the renal pelvis (136) next to the ureter (137) or in the renal parenchyma (135) ( Figs. 106.2 and 106.3 ). Such cysts do not enhance after CM injection (cf. p.133).
In Fig. 106.2 the superior mesenteric artery (106) originates from the aorta (89) and can be followed down next to the SMV (107).







Close to the gallbladder (126), you can sometimes see partial volume effects ( Fig. 107.1 ) of the adjacent colon (143/144), the walls of which (152) should normally be thin and well defined in contrast to the root of the small bowel mesentery (as in Fig. 107.3 ). The duodenum (130) can only be distinguished from the other intestinal loops (140) on the basis of its position. At this level, you should also check the kidneys (135) for smooth margins and possible parenchymal scarring. The presence of fat makes it easier to identify the rectus abdominis muscle (29) as well as the oblique muscles of the abdominal wall (28a–c).






Note the typical position of the proximal parts of the ureters (137), medial to the inferior poles of the kidneys (135) and anterior to the psoas muscle (31).
In Figures 108.2 and 108.3 , the lumina of both ureters could also appear hyperdense if CM is being excreted in the urine. Haustrations caused by the semilunar folds (haustral folds) (149) are typical of the colon (142-144 in the figures below).







In Figure 109.1 , the branching pattern of the superior mesenteric vessels (108) which supply the small bowel (140) can be seen. At the bifurcation of the aorta (89) (usually at L4 vertebral body, Fig. 109.1 ), the common iliac arteries (113) are anterior to the corresponding veins (116). The two ureters (137) are located more laterally in front of the psoas muscles (31). Along with the iliac bones (58) the gluteus medius muscles (35a) appear ( Fig. 110.2 ) and sometimes contain calcified intramuscular injections sites.






In order to exclude the presence of an abdominal hernia you should check for a normal width of the linea alba (47) between the rectus abdominis muscles (29). More caudally ( Fig. 110.3 ) there is a site of predilection for enlarged LNs at the division of the iliac vessels into external artery/vein (115/118), which pass anteriorly, and internal artery/vein (114/117), which are located more posteriorly. The transition from the lumbar spine (50) to the sacrum (62) lies at this level.
Further down we find predominantly small bowel loops of jejunum and ileum (140) which can be distinguished from sigmoid colon (145) by its haustrations and semilunar folds (cf. p. 111).















In the following images, the ureters (137) pass posteriorly to approach the lateral aspects of the base of the bladder (138). Within the bladder, differences in the concentration of excreted might be recognized as fluid–fluid levels of different densities without any clinical significance.
The ovaries (159) lie more laterally. Depending on age and the phase of the menstrual cycle, ovarian follicles (169) might be misinterpreted as cystic lesions ( Fig. 112.3 ).







In the female pelvis, the size and position of the uterus (158) relative to the urinary bladder can vary considerably from patient to patient. The uterus may lie cranial or lateral to the bladder ( Figs. 113.1–114.1 ). The cervix and the vagina (160) are situated between the bladder (138) and the rectum (146). Depending on age and the phase of the menstrual cycle, changing thicknesses of endometrium (*) can be seen within the uterus (158 in Fig. 113.1 ).







Free intra-abdominal fluid (ascites or hemorrhage) may occur in the rectouterine pouch between rectum and uterus, as well as in the vesicouterine space. In the inguinal region, lymph nodes (6) can be up to 2 cm in diameter and be normal ( Figs. 114.2 and 114.3 ). The size of normal abdominal lymph nodes does not usually exceed 1 cm. It is not possible to examine the hip joints on soft-tissue windows ( Fig. 114.3 ); the heads of the femurs (66a) in the acetabular fossae (59/61) can best be analyzed on bone windows (not shown here).
On the next pages, a male pelvis is shown, demonstrating the prostate (153), seminal vesicles (154), spermatic cord (155), and root of penis (156). Note in particular the internal obturator muscles (41a) and the levator ani muscles (42) lateral to the anal canal (146a). An assessment of bone windows completes the examination of the abdominal and pelvic images.






















Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree