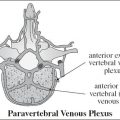
Ia extradural arachnoid cyst
Ib sacral meningocele
Pitfalls of CT myelography / MRI:
(1) Nonopacification of noncommunicating arachnoid cyst → misidentification as a different type of lesion
(2) Absence of mass effect on cord → failure to detect additional cysts / small CSF-isointense arachnoid cyst
DDx: traumatic / lateral thoracic meningoceles
Cx: spinal cord myelopathy, nerve root radiculopathy
Extradural Arachnoid Cyst
Cause: congenital / acquired dural defect
Age: 2nd decade of life; M>F
Location: thoracic (80%) > cervical (15%) > lumbar (5%)spine; extending over 3.7 vertebral bodies
Site: posteriorly / posterolaterally to cord
√ scalloping of vertebral body
√ thinning / erosion of pedicles
√ widening of interpeduncular distance
Intradural Arachnoid Cyst
Cause: congenital deficiency within arachnoid (= true arachnoid cyst) / adhesion from prior infection or trauma (= arachnoid loculation)
√ focal displacement and compression of spinal cord
√ widened dorsal subarachnoid space with diminished CSF flow artifact
ARACHNOID DIVERTICULUM
= widening of root sheath with arachnoid space occupying > 50% of total transverse diameter of root + sheath together
Cause: ? congenital / traumatic, arachnoiditis, infection
Pathogenesis: hydrostatic pressure of CSF
√ scalloping of posterior margins of vertebral bodies
√ myelographic contrast material fills diverticula
ARTERIOVENOUS MALFORMATION OF SPINAL CORD
Classification:
1. True intramedullary AVM
= nidus of abnormal intermediary arteriovenous structure with multiple shunts
Age: 2nd–3rd decade
Cx: subarachnoid hemorrhage, paraplegia
Prognosis: poor (especially in midthoracic location)
2. Intradural arteriovenous fistula
= single shunt between one / several medullary arteries + single perimedullary vein
3. Dural arteriovenous fistula
= single shunt between meningeal arteries + intradural vein
4. Metameric angiomatosis
ARTERIOVENOUS MALFORMATION OF JAW
• occasionally pulsatile soft-tissue swelling
Location: ramus + posterior body of mandible
√ cystlike due to bone resorption ± calcifications
√ ± multilocular ± bone expansion
√ ± erosive margins
√ angiogram confirms diagnosis
Cx: Tooth extraction can result in lethal exsanguination!
DDx: traumatic bone cyst, central giant cell granuloma, ossifying fibroma
ATLANTOAXIAL ROTARY FIXATION
= AARF = ATLANTOAXIAL ROTATORY SUBLUXATION (AARS)
= ATLANTOAXIAL ROTATORY FIXATION (AARF)
= SPONTANEOUS HYPEREMIC DISLOCATION
= ATLANTOAXIAL ROTATORY / ROTARY DISLOCATION
= DISTENTION LUXATION = NASOPHARYNGEAL TORTICOLLIS
= nontraumatic subluxation / rotational disorder of atlantoaxial joint leading to limited rotation / fixation of neck comprising many different entities
Cause: idiopathic spontaneous
(a) increased ligamentous laxity: rheumatoid arthritis, Marfan syndrome, Down syndrome, Morquio syndrome
(b) congenital abnormality: incomplete odontoid process, incomplete transverse ligament
(c) infection: sinusitis, otomastoiditis, otitis media, pharyngitis, adenotonsillitis, cervical / retropharyngeal / tonsillar abscess = Grisel syndrome
(= not associated with trauma or bone disease primarily in children) ← hyperemia + pathologic ligamentous relaxation
Predisposed: cervical dystonia, post surgery
May be associated with: ipsilateral contracted SCMM
• history of insignificant cervical spine trauma / upper respiratory tract infection
• limited painful neck motion = painful torticollis
• head held in “cock-robin” position = rotation + flexion + tilt of head contralateral to direction of rotation with inability to turn head that does not resolve within 5–7 days after injury
X-ray (Dx difficult to make):
√ atlanto-odontoid asymmetry (open mouth odontoid view):
√ decrease in atlanto-odontoid space + widening of lateral mass on side ipsilateral to rotation
√ increase in atlanto-odontoid space + narrowing of lateral mass on side contralateral to rotation
√ atlantoaxial asymmetry remains constant with head turned into neutral position
√ posterior arch of C1 not identified in true lateral projection
√ obscuration of craniovertebral junction in true lateral view
CT (dynamic with 3D reconstruction [a] with head in resting position [b] with maximal contralateral rotation):
√ facet displacement in neutral head position
√ asymmetrically fixed C1-C2 rotation
Rotation up to an average of 79° in adult volunteers, loss of contact of articular facets of C1 and C2 during rotation as high as 74–85% in physiologic conditions. Therefore, a diagnosis of subluxation of the atlanto-occipital joint should not be made based solely on the CT appearance of this joint.
MR:
√ disruption of alar + transverse ligg.
√ spinal cord compression (rare)
Types:
I < 3 mm anterior displacement of atlas on axis = rotatory fixation within normal range of movement (most common)
Injury: intact alar + transverse ligaments
√ pivot around dens, NO anterior displacement of atlas
II 3–5 mm anterior displacement of atlas + unilateral displacement of lateral mass of atlas ← restraint by alar lig.
Injury: transverse ligament

√ center of rotation shifted to one of lateral masses
III > 5 mm anterior displacement of atlas + anterior displacement of both lateral masses
Injury: deficiency of both (alar + transverse) ligaments
IV posterior displacement of atlas on axis (rare)
Injury: deficiency of both (alar + transverse) ligaments
DDx: torticollis (atlantoaxial symmetry reverts to normal with head turned into neutral position)
Traumatic Rotatory Subluxation
Cause: injury of alar ligaments ← flexion + rotation forces
Age: more prevalent in children than in adults ← mostly flat articular facets allow ample movement in multiple directions
BRACHIAL PLEXUS INJURY
= most severe nerve injury of extremities
Cause: severe traction force on upper limb at birth / in traffic accident (motorcycle)
1. Erb-Duchenne palsy: adduction injury affecting C5-6 ← downward displacement of shoulder
• paralysis of shoulder muscles + biceps
2. Klumpke palsy: abduction injury at C7, C8, T1 ← arm stretched over head
• paralysis of forearm flexors + intrinsic hand muscles
CT myelography (preferred method):
◊ Shoulder artifacts may be problematic at C8–T1 level
√ displacement of spinal cord to contralateral side ← absence of normal nerve root traction on cord
√ pouchlike nerve root sleeve at site of avulsion
√ asymmetric slightly deformed root sleeve + nerve roots
√ obliteration of tip of root sleeve
√ traumatic meningocele
√ contrast extravasation collecting in axilla
√ metrizamide in neural foramina
MR:
◊ Conventional MR only in 50% accurate!
Pitfalls: partial root avulsion, intradural fibrosis, traumatic meningocele, movement artifacts (respiration, swallowing, blood flow)
√ focal T2-hyperintense cord changes ← edema of acute phase / myelomalacia in chronic phase
√ focal T2-hypointense cord changes ← hemosiderin
√ enhancement of morphologically normal intradural nerve root / root stump ← functional impairment (mostly preganglionic)
√ abnormal enhancement of paraspinal (multifidus) muscle ← muscle denervation = indirect sign of root avulsion
√ thickening of postganglionic brachial plexus ← edema + fibrosis
CAUDAL REGRESSION SYNDROME
= SACRAL AGENESIS = CAUDAL DYSPLASIA SEQUENCE
= midline closure defect of neural tube with a spectrum of anomalies including complete / partial agenesis of sacrum + lumbar vertebrae and pelvic deformity
Etiology: disturbance of caudal mesoderm < 4th week of gestation from toxic / infectious / ischemic insult
Prevalence: 1÷60,000 births; 0.005–0.01% of population; in 0.1–1% of pregnancies in diabetic women; M÷F = 2.7÷1
Predisposed: infants of diabetic mothers; risk increases 200–400 times in women dependent on insulin
◊ 16–22% of children with sacral agenesis have mothers with diabetes mellitus
◊ NOT associated with VATER syndrome!
A. Musculoskeletal anomalies
@ Lower extremity
• symptoms from minor muscle weakness to complete sensorimotor paralysis of both lower extremities
√ hip dislocation
√ hypoplasia of lower extremities
√ flexion contractures of lower extremities
√ foot deformities
@ Lumbosacral spine = SACRAL AGENESIS
Spectrum:
| Type 1 = | unilateral partial agenesis localized to sacrum / coccyx |
| Type 2 = | bilateral partial symmetric defects of sacrum + iliosacral articulation |
| Type 3 = | total sacral agenesis + iliolumbar articulation |
| Type 4 = | total sacral agenesis + ilioilial fusion posteriorly |
√ nonossification of lower spine
√ fusion of caudal-most 2 or 3 vertebrae
√ spina bifida (lipomyelomeningocele often not in combination with Arnold-Chiari malformation)
√ narrowing of spinal canal rostral to last intact vertebra
√ hypoplastic iliac wings
B. Spinal cord anomalies
√ characteristic club- / wedge-shaped configuration of conus medullaris (= hypoplasia of distal spinal cord)
√ ± tethered spinal cord
√ ± dural sac stenosis with high termination
√ ± spinal cord lipoma, teratoma, cauda equina cyst
√ ± syrinx
C. Genitourinary anomalies
• neurogenic bladder (if > 2 segments are missing)
• malformed external genitalia
√ ± bilateral renal aplasia with pulmonary hypoplasia and Potter facies
D. Hindgut anomalies
• lack of bowel control
√ anal atresia
OB-US:
• normal / imperforate anus
√ short CRL in 1st trimester ← diabetic embryopathy
√ normal / mildly dilated urinary system
√ normal / increased amniotic fluid
√ 2 umbilical arteries
√ 2 hypoplastic nonfused lower extremities in a CHARACTERISTIC froglike position
√ fusion of pelvic bones
√ sacral agenesis, absent vertebrae from lower thoracic / upper lumbar spine caudally
N.B.: brain, proximal spine, and spinal cord are notably spared!
Sirenomelia
= fused lower extremities resembling a mermaid (siren)
Cause: aberrant vessel that shunts blood from the high abdominal aorta to the umbilical cord (steal phenomenon) → severe ischemia of caudal portion of fetus
◊ NOT associated with maternal diabetes mellitus!
• pulmonary hypoplasia + Potter facies
• absence of anus; absent genitalia
√ bilateral renal agenesis / dysgenesis (lethal)
√ marked oligohydramnios
√ single aberrant umbilical artery
√ two-vessel umbilical cord
√ single / fused lower extremity often with fewer leg bones than normal
√ sacral agenesis, absent pelvis, lumbosacral “tail”, lumbar rachischisis
Prognosis: incompatible with life
CEMENTOBLASTOMA
= rare benign periapical lesion
Origin: true neoplasm of cementum
Prevalence: <1% of all odontogenic tumors
Age: < 20 years (50%); < 30 years (75%)
Associated with: erupted permanent tooth (common); near impacted / unerupted tooth (rare)
Location: mandible (>75%): 90% molar / premolar region
Site: fusion with root of tooth(s); invasion of root canal / pulp chamber (occasionally)
√ periapical sclerotic sharply marginated round opaque sunburst lesion
√ surrounded by thin halo of low attenuation
Rx: complete removal of tooth to avoid recurrence
DDx: condensing osteitis (periodontal ligament space not obscured)
CEMENTO-OSSEOUS DYSPLASIA
= CEMENTOMA = FIBROOSTEOMA
= nonneoplastic benign hamartoma associated with tooth apex
Histo: proliferation of connective tissue within periodontal membrane
Age: 4th–5th decade; in woman: black / Asian descent
• asymptomatic / dull ache
Associated with: vital nonrestored tooth + intact lamina dura
Location: mandible >> maxilla
Site: usually apex of vital tooth
√ one / more, closely apposed / confluent, round / ovoid lucent lesion with varying amounts of opacity:
√ initially lytic lesion
√ later mixed lysis + sclerosis with varying amounts of opacity; little expansion
√ calcifies centrally with time
√ periapical sclerotic sharply marginated area NOT fused to tooth
√ ± low-attenuation halo
√ adjacent lesions may coalesce
Cementoblastoma and cemento-osseous dysplasia are both periapical sclerotic sharply marginated lesions with low-attenuation halo.
DDx: (1) Cementoblastoma (in child + young adult, fuses directly to tooth root)
(2) Cemento-osseous dysplasia (common in black woman + woman of Asian descent during 4th / 5th decade of life, does not fuse to tooth root)
Periapical Cemento-osseous Dysplasia
Site: anterior mandible between mandibular canine teeth involving one / a few teeth
√ often multicentric
DDx: ossifying fibroma, fibrous dysplasia, Paget disease
Focal Cemento-osseous Dysplasia
Site: posterior mandible involving molar teeth
√ no extension into adjacent bone
√ no cortical expansion
DDx: periapical periodontitis, ossifying fibroma
Florid Cemento-osseous Dysplasia
= diffuse form of periapical cemento-osseous dysplasia
Location: involving ≥ 2 jaw quadrants / entire mandible
May be complicated by: osteomyelitis with drainage of necrotic bone debris into oral cavity
CENTRAL GIANT CELL GRANULOMA (COMMON)
= single lesion of altered vascular + reactive response within bone
Age: < 30 years (75%); in girls + young women
• painless swelling, tenderness on palpation
Location: mandible÷maxilla = 2÷1
Site: anterior to 1st molar (= deciduous teeth); propensity for crossing midline (especially in maxilla)
√ small unilocular area of lucency (early)
√ multilocular honeycomb with wispy internal septa (later)
√ expansion of bone + erosion / remodeling of cortex
√ displacement of teeth + root resorption
√ usually well-defined border
DDx: brown tumor of HPT (histologically similar)
CHONDROSARCOMA OF SPINE
= 2nd most common nonlymphoproliferative primary malignant tumor of spine in adults
Peak age: 30 and 70 years; M÷F = 2÷1 to 4÷1
Location: thoracic + lumbar spine > sacrum
Site: posterior element (40%), vertebral body (15%), both (45%)
√ large calcified mass with bone destruction
√ ± true ossification ← residual osteochondroma
CT:
√ low attenuation of nonmineralized portion of tumor
√ chondroid matrix mineralization
MR:
√ nonmineralized portion of tumor = high water content:
√ low to intermediate SI on T1WI
√ very high signal intensity on T2WI
√ rings and arcs enhancement pattern ← lobulated growth
√ extension through intervertebral disk (in 35%)
Rx: en bloc resection
CHORDOMA
Prevalence: 1÷2,000,000; 2–4% of all primary malignant bone tumors; 1% of all CNS tumors
◊ 2nd most common primary malignant tumor of spine in adults after lymphoproliferative neoplasms! Highly malignant in children.
Etiology: originates from embryonic remnants of notochord / ectopic cordal foci between Rathke pouch + coccyx (notochord appears between 4th and 7th week of embryonic life and forms nucleus pulposus)
Mean age: 50 (range, 30–70) years; peak in 5th decade; M÷F = 2÷1
Path: lobulated tumor with fluid, gelatinous mucoid substance, recent + old hemorrhage, necrotic areas, occasionally calcifications + sequestered bone fragments contained within pseudocapsule
Histo: [physallis, Greek = bladder, bubble; phoros = bearing]
(1) typical chordoma: cords + clusters of physaliferous cells (PAS-positive stain) in a lobular arrangement with a large bubblelike multivacuolated cytoplasm containing intracytoplasmic mucous droplets; abundant extracellular mucus deposition + areas of hemorrhage
(2) chondroid chordoma: cartilage instead of mucinous differentiation of extracellular matrix
Location: (a) 50–60% in sacrum (sacrococcygeal chordoma)
(b) 30–35% in clivus (sphenooccipital chordoma)
(c) 15% in vertebrae (vertebral chordoma): cervical > thoracic / lumbar spine; vertebral body with sparing of posterior elements
(d) other sites (5%) in mandible, maxilla, scapula
Site: midline / paramedian
√ amorphous calcification (50–75%)
√ heterogeneous enhancement
CT:
√ low-attenuation within soft-tissue mass ← myxoid-type tissue
√ higher attenuation fibrous pseudocapsule
MR (modality of choice):
√ low to intermediate intensity on T1WI, occasionally hyperintense ← high protein content:
√ heterogeneous internal texture ← calcification, necrosis, gelatinous mucoid collections
√ very high SI on T2WI ← physaliferous cells similar to nucleus pulposus with high water content
Angio:
√ prominent vascular stain
NUC:
√ cold lesion on bone scan
√ no uptake on gallium scan
Metastases (in 5–43%) to: liver, lung, regional lymph nodes, peritoneum, skin (late), heart
Prognosis: poor in spite of low grade + slow growth; almost 100% recurrence rate despite radical surgery
DDx: giant notochordal rest (nonprogressive indistinct lesion, normal bone / variable degree of sclerosis, no soft-tissue involvement)
Intracranial Chordoma (35%)
= locally invasive + destructive lesion of clivus
Location: infrasellar midline
√ mass of usually T1 hypointensity + T2 signal hyperintensity
√ hypointense intratumoral septations
√ foci of T1 signal hyperintensity within tumor / periphery ← residual ossified fragments / tumor calcifications, / small collections of proteinaceous fluid / hemorrhage
√ posterior extension indenting pons
DDx: cartilaginous tumor (more lateral location, at petrooccipital synchondrosis, curvilinear calcifications)
Sacrococcygeal Chordoma (50–70%)
= large destructive sacral mass with 2ndary soft-tissue extension
◊ Most common primary sacral tumor after giant cell tumor!
Peak age: 40–60 years; M÷F = 2–3÷1
Path: slow-growing tumor → large size at presentation
• clinically indolent and subtle; rectal bleeding (42%)
• low back pain (70%); sciatica + weakness in hip / lower limbs ← sacral root compression
• constipation, frequency, urgency, straining on micturition ← compression by tumor
• autonomic dysfunction → urinary / fecal incontinence
• palpable sacral mass on digital examination (17%)
Location: predominantly in 4th + 5th sacral segment
√ presacral mass with average size of 10 cm extending superiorly + inferiorly; rarely posterior location
√ displacement of rectum + bladder
√ solid tumor with cystic areas (in 50%)
√ amorphous peripheral calcifications (15–89%)
√ secondary bone sclerosis in tumor periphery (50%)
√ honeycomb pattern with trabeculations (10–15%)
√ may cross sacroiliac joint
X-ray:
√ osteolytic midline mass in sacrum + coccyx associated with soft-tissue mass and calcifications
CT (useful for defining extent of bone involvement):
√ bone destruction associated with lobulated midline soft-tissue mass
√ areas of low attenuation within mass ← high water content of myxoid properties
MR:
√ hypo- / isointense mass relative to muscle on T1WI:
√ intrinsic hyperintense areas on T1WI ← hemorrhage or myxoid / mucinous collections
√ hyperintense mass similar to nucleus pulposus on T2WI ← high water content:
√ dividing septa + hemosiderin of low signal intensity
√ heterogeneous often moderate enhancement
The combination of high T2 signal intensity in a lobulated sacral mass that contains areas of hemorrhage and calcification is strongly suggestive of a chordoma!
Prognosis: 7–10 years average survival; 50–74% 5-year survival rate (in adulthood); 52–64% 10-year survival; 52% 20-year survival
Dx: fine-needle aspiration biopsy
Rx: radical surgical excision (most critical); radiation therapy; 70% rate of local recurrence after excision
DDx:
› Primary neural tumor: schwannoma, neurofibroma, meningioma, myxopapillary ependymoma (from within spinal canal, more intense enhancement)
› Primary bone tumor:
(1) Giant cell tumor (2nd most common primary, upper sacrum, may be eccentric, ± extension across SI joint, low-to-intermediate T2 intensity ± fluid-fluid levels)
(2) Chondrosarcoma (off midline from sacroiliac joint space cartilage, heterogeneous T2 SI, no hemorrhage)
(3) Aneurysmal bone cyst
(4) Osteoblastoma
(5) Lymphoma
› Metastasis, plasmacytoma
› Soft-tissue neoplasm: atypical hemangioma, prostatic carcinoma, osteosarcoma, osteomyelitis
Sphenooccipital Chordoma (15–35%)
Age: younger patient (peak age of 20–40 years); M÷F – 1÷1
• orbitofrontal headache
• visual disturbances, ptosis
• 6th nerve palsy / paraplegia
Location: clivus, sphenooccipital synchondrosis
√ bone destruction (in 90%): clivus > sella > petrous bone > orbit > floor of middle cranial fossa > jugular fossa > atlas > foramen magnum
√ reactive bone sclerosis (rare)
√ calcifications / residual bone trabeculae (20–70%)
√ soft-tissue extension into nasopharynx (common), into sphenoid + ethmoid sinuses (occasionally), may reach nasal cavity + maxillary antrum
√ variable degree of enhancement
MR:
√ large intraosseous mass extending into prepontine cistern, sphenoid sinus, middle cranial fossa, nasopharynx
√ posterior displacement of brainstem
√ usually hypo- / isointense to brain / occasionally inhomogeneously hyperintense on T1WI
√ hyperintense on T2WI
√ ± CHARACTERISTIC honeycomb enhancement pattern
Prognosis: 4–5 years average survival
DDx: meningioma, metastasis, plasmacytoma, giant cell tumor, sphenoid sinus cyst, nasopharyngeal carcinoma, chondrosarcoma
Vertebral / Spinal Chordoma (15–20%)
◊ More aggressive than sacral / cranial chordomas
Age: younger patient; M÷F = 2÷1
• low back pain + radiculopathy + retention of urine
Location: cervical (8% – particularly C2), thoracic spine (4%), lumbar spine (3%)
Site: midline centra sparing posterior elements; arising in perivertebral musculature (uncommon)
√ destructive expansile lesion of vertebral body:
√ + epidural soft-tissue mass of collar button / mushroom / dumbbell shape over several segments
√ often incomplete sparing of disk spaces to involve adjacent bodies (10–14%) simulating infection
√ exophytic anterior soft-tissue mass
√ expansion into neural foramen mimicking nerve sheath tumor
√ solitary midline spinal mass
√ sclerosis / “ivory vertebra” in 43–62%
√ total destruction of vertebra, initially without collapse
√ amorphous peripheral calcifications in 40%
Cx: complete spinal block
Prognosis: 4–5 years average survival
DDx: metastasis, primary bone tumor, primary soft-tissue tumor, neuroma, meningioma
CONDENSING OSTEITIS OF JAW
= reactive osteitis surrounding apex of tooth with pulpitis / pulpal necrosis
Associated with: carious tooth
√ periapical inflammatory lesion: granuloma / cyst / abscess
√ periapical poorly marginated nonexpansile sclerosis
CSF FISTULA
= characterized by egress of CSF from intracranial cavity through abnormal communication between subarachnoid space and pneumatized structure within skull base (= osteodural defect)
Cause:
A. CONGENITAL: ENCEPHALOCELE
B. ACQUIRED
(a) traumatic (80–90% of all cases)
◊ 2% of all head injuries develop CSF fistula
(b) nontraumatic:
› infection
› tumor (esp. those arising from pituitary gland)
(c) spontaneous: idiopathic intracranial hypertension
• rhinorrhea / otorrhea (may be exacerbated by Valsalva maneuver)
• “serous otitis media” with conductive / sensory hearing loss
• presence of β-2 transferrin (= polypeptide specific for CSF) / β-trace protein
Technique:
(a) invasive techniques (time-consuming, poorly tolerated)
1. Radionuclide cisternography
2. CT cisternography
◊ Contraindicated in active meningitis / elevated intracranial pressure!
Disadvantage:
› requires poorly tolerated lumbar puncture
› time-consuming
› slight risk of complications (low-tension headache, infection, bleeding at puncture site)
› hypersensitivity reaction to contrast
› high dose of radiation
› requires active CSF leak
(b) noninvasive techniques (best used in combination)
1. Multidetector CT (92% sensitive, 100% specific)
√ bone defect / dehiscence at skull base
√ adjacent prominent arachnoid granulations
√ air-fluid level / opacification of contiguous sinus / middle ear / mastoid
√ pneumocephalus
√ lobular / nondependent area of soft-tissue opacification (meningocele, meningoencephalocele)
DDx: mucosal reaction, cholesteatoma, granulation tissue, cholesterin granuloma
2. MR cisternography (87–100% sensitive, 57–100% specific, 78–89% accurate)
√ hyperintense CSF fistulous tract
√ CSF collection = meningocele
DDx: inflammatory paranasal secretions
√ extradural brain = meningoencephalocele
√ secondary gliosis of herniated brain
√ dural enhancement in stalk of meningoencephalocele
Spontaneous CSF Fistula
Location: cribriform plate along course of anterior ethmoid artery (most common), lateral lamella, perisellar region (sphenoid roof > floor of sella > posterior wall), lateral recess of sphenoid, tegmen tympani, tegmen mastoideum, skull base foramina
Traumatic CSF Fistula
• traumatic leak: usually unilateral; onset within 48 hours after trauma, usually scanty; resolves in 1 week
• nontraumatic leak: profuse flow; may persist for years
• anosmia (in 78% of trauma cases)
Location: fractures through frontoethmoidal complex + middle cranial fossa (most commonly)
Cx: (1) meningitis / encephalitis / brain abscess (in 25–50% of untreated cases)
(2) pneumocephalus
CURRARINO TRIAD
= triad of anorectal malformation + sacrococcygeal osseous defect + presacral mass (= ASP triad)
= rare syndrome characterized by autosomal dominant genetic inheritance (in > 50%)
Path: presacral mass consists of teratoma, anterior sacral meningocele > dermoid cyst, hamartoma, enteric duplication cyst
Age: < 16 years at diagnosis (in 80%)
• constipation
DEGENERATIVE DISK DISEASE
◊ Therapeutic decision-making should be based on clinical assessment alone!
◊ There are no prognostic indicators on images in patients with acute lumbar radiculopathy!
◊ 35% of individuals without back trouble have abnormal findings (HNP, disk bulging, facet degeneration, spinal stenosis)
◊ Imaging is only justified in patients for whom surgery is considered!
Pathophysiology:
loss of disk height leads to stress on facet joints + uncovertebral joints (= uncinate process), exaggerated joint motion with misalignment (= rostrocaudal subluxation) of facet joints, spine instability with arthritis, capsular hypertrophy, hypertrophy of posterior ligaments, facet fracture
Plain film:
√ intervertebral osteochondrosis = disease of nucleus pulposus (= desiccation = loss of disk water):
√ narrowing of disk space
√ vacuum disk phenomenon
√ disk calcification
√ bone sclerosis of adjacent vertebral bodies
√ spondylosis deformans = degeneration of the outer fibers of the annulus fibrosus:
√ endplate osteophytosis growing initially horizontally and then vertically several millimeters from diskovertebral junction ← displacement of nucleus pulposus in anterior + anterolateral direction producing traction on osseous attachment of annulus fibrosus [= fibers of Sharpey])
√ enlargement of uncinate processes
√ osteoarthritis = degenerative disease of synovium-lined apophyseal / costovertebral joints:
√ degenerative spondylolisthesis
√ cartilaginous node = intraosseous disk herniation
Myelography:
√ delineation of thecal sac, spinal cord, exiting nerve roots
CT (accuracy > 90%):
√ facet joint disease (marginal sclerosis, joint narrowing, cyst formation, bony overgrowth)
√ uncovertebral joint disease of cervical spine (osteophytes project into lateral spinal canal + neuroforamen)
MR:
√ scalloping of cord (T2WI FSE / GRE images):
√ anterior encroachment by disk / spondylosis
√ posterior encroachment by ligamentum flavum hypertrophy
√ loss of disk signal ← desiccation ←decrease in water-binding proteoglycans + increase in collagen within nucleus pulposus) on T2WI
√ annular tear:
(1) concentric tear – separation of annular lamellae
(2) transverse tear
(3) radial tear – crossing multiple annular lamellae with greater vertical dimension + more limited horizontal extent
• diskogenic pain
◊ does NOT imply disk herniation
√ gap near middle of annulus

Modified Dallas Diskogram Classification | |
Grade | Description |
0 | contrast confined within nucleus pulposus |
1 | contrast extends to inner third of annulus |
2 | contrast extends to middle third of annulus |
3 | outer third of annulus + < 30° of circumference |
4 | outer third of annulus + > 30° of circumference |
5 | extension of contrast beyond annulus |
√ cleft of high SI in a normally hypointense outer annulus on T2WI
√ contrast enhancement ← granulation tissue / hyperemia / inflammation
√ reduction in disk height (late):
√ Schmorl’s node
√ moderate linear uniform enhancement on T1WI
√ vacuum phenomenon with low signal on T1WI
√ endplate + marrow changes (Modic & DeRoos):
= linear signal alterations paralleling adjacent endplates
(a) Type 1 (4%) = edema pattern
Cause: replacement of bone marrow with hyperemic fibrovascular tissue + edema ← acute disk degeneration
√ hypointense on T1WI + hyperintense on T2WI
√ contrast-enhancement of marrow
(b) Type 2 (16%) = fatty marrow pattern
Cause: replacement of bone marrow with fat ← chronic disk degeneration
√ hyperintense marrow signal on T1WI
√ iso- to mildly hyperintense on T2WI
√ hypointense on STIR
(c) Type 3 = bony sclerosis pattern
Cause: replacement of bone marrow with sclerotic bone ← chronic disk degeneration after a few years
√ hypointense marrow signal on T1WI + T2WI
√ juxtaarticular synovial cyst in posterolateral spinal canal (most frequently at L4-5):
√ smooth well-defined extradural mass adjacent to facet joint
√ variable signal pattern ← serous, mucinous, gelatinous fluid components, air, hemorrhage
√ contrast-enhancing hypointense perimeter ← fibrous capsule with calcium + hemosiderin
NUC:
SPECT imaging of vertebrae can aid in localizing increased uptake to vertebral bodies, posterior elements, etc.
√ eccentrically placed increased uptake on either side of an intervertebral space (osteophytes, diskogenic sclerosis)
Sequelae: (1) Disk bulging
(2) Disk herniation
(3) Spinal stenosis
(4) Facet joint disease
(5) Instability
√ dynamic slip > 3 mm on flexion-extension
√ static slip > 4.5 mm
√ traction spurs
√ vacuum phenomenon

DDx: Idiopathic segmental sclerosis of vertebral body (middle-aged / young patient, hemispherical sclerosis in anteroinferior aspect of lower lumbar vertebrae with small osteolytic focus, only slight narrowing of intervertebral disk; unknown cause)
Bulging Disk = Disk Bulge
= concentric smooth expansion of softened disk material beyond the confines of endplates with disk extension outward involving > 50% of disk circumference
Cause: weakened and lengthened but intact annulus fibrosus + posterior longitudinal ligament
Age: common finding in individuals > 40 years of age
Location: L4-5, L5-S1, C5-6, C6-7
√ rounded symmetric defect localized to disk space level
√ smooth concave indentation of anterior thecal sac
√ encroachment on inferior portion of neuroforamen
√ accentuated by upright myelography
MR:
√ nucleus pulposus hypointense on T1WI + hyperintense on T2WI ← desiccation (= water loss through degeneration + fibrosis)
Herniation of Nucleus Pulposus
= HNP = protrusion of disk material > 3 mm beyond margins of adjacent vertebral endplates involving < 50% of disk circumference
Cause: rupture of annulus fibrosus with disk material confined within posterior longitudinal ligament
◊ 21% of an asymptomatic population has a herniated disk!
• local somatic spinal pain = sharp / aching, deep, localized
• centrifugal radiating pain = sharp, well-circumscribed, superficial, “electric,” confined to dermatome
• centrifugal referred pain = dull, ill-defined, deep or superficial, aching or boring, confined to somatome (= dermatome + myotome + sclerotome)
Site:
(a) posterolateral (49%) = weakest point along posterolateral margin of disk at lateral recess of spinal canal

◊ The posterior longitudinal ligament is tightly adherent to posterior central margins of disk!
(b) posterocentral (8%)
(c) bilateral (to both sides of posterior ligament)
(d) lateral / foraminal (< 10%)
(e) extraforaminal = anterior (commonly overlooked) (29%)
(f) intraosseous / vertical = Schmorl node (14%)
Myelography:
√ sharply angular indentation on lateral aspect of thecal sac with extension above / below level of disk space (ipsilateral oblique projection best view)
√ asymmetry of posterior disk margin
√ double contour ← superimposed normal + abnormal side (horizontal beam lateral view)
√ narrowing of intervertebral disk space (most commonly a sign of disk degeneration)
√ deviation of nerve root / root sleeve
√ enlargement of nerve root (“trumpet” sign) ← edema
√ amputated / truncated nerve root (= nonfilling of root sleeve)
MR:
√ herniated disk material of low SI displaces the posterior longitudinal ligament and epidural fat of relative high SI on T1WI
√ “squeezed toothpaste” effect = hourglass appearance of herniated disk at posterior disk margin on sagittal image
√ asymmetry of posterior disk margin on axial image
Cx: (1) spinal stenosis mild = < ⅓
moderate = ⅓ to ⅔
severe = > ⅔
(2) neuroforaminal stenosis
Prognosis:
conservative therapy reduces size of herniation by
| 0–50% | in 11% of patients, |
| 50–75% | in 36% of patients, |
| 75–100% | in 46% of patients |
(secondary to growth of granulation tissue)
Broad-based Disk Protrusion
√ triangular shape of herniation with a base wider than the radius of its depth
√ 25–50% of disk circumference
Focal Disk Protrusion
√ triangular shape of herniation with a base wider than the radius of its depth
√ < 25% of disk circumference
Disk Extrusion
= prominent focal extension of disk material through the annulus with only an isthmus of connection to parent disk through intact / ruptured posterior longitudinal ligament
√ mushroom-shaped herniation with base narrower than the radius of its depth
√ “toothpaste” sign

Disk Sequestration
= FREE FRAGMENT HERNIATION
= complete separation of disk material from parent disk with rupture through posterior longitudinal ligament into epidural space
◊ Missed free fragments are a common cause of failed back surgery!
√ migration superiorly / inferiorly away from disk space with compression of nerve root above / below level of disk herniation
√ disk material > 9 mm away from intervertebral disk space = NO continuity
√ soft-tissue density with higher value than thecal sac
DDx: (1) Postoperative scarring (retraction of thecal sac to side of surgery)
(2) Epidural tumor
(3) Tarlov cyst (dilated nerve root sleeve)
(4) Conjoined nerve root (2 nerve roots arising from thecal sac simultaneously representing mass in ventrolateral aspect of spinal canal; normal variant in 1–3% of population)
Free Fragment Migration
= separated disk material travels above / below intervertebral disk space
√ ± continuity
Cervical Disk Herniation
Peak age: 3rd–4th decade
• neck stiffness, muscle splinting; dermatomic sensory loss
• weakness + muscle atrophy; reflex loss
Sites: C6-7 (69%); C5-6 (19%); C7-T1 (10%); C4-5 (2%)
Sequelae:
(1) compression of exiting nerve roots with pain radiating to shoulder, arm, hand
(2) cord compression (spinal stenosis + massive disk rupture)
Thoracic Disk Herniation
Prevalence: 1% of all disk herniations
Sites: T11-12
√ calcification of disk fragments + parent disk (frequent)
Lumbar Disk Herniation
• sciatica =
(1) Stiffness in back
(2) Pain radiating down to thigh / calf / foot
(3) Paresthesia / weakness / reflex changes
• pain exaggerated by coughing, sneezing, physical activity + worse while sitting / straightening of leg
Sites: L4-5 (35%) > L5/S1 (27%) > L3-4 (19%) > L2-3 (14%) > L1-2 (5%)

DIASTEMATOMYELIA
= SPLIT CORD = MYELOSCHISIS [diastema, Greek = slit, cleft]
= sagittal division of spinal cord into two hemicords, each containing a central canal, one dorsal horn + one ventral horn
Etiology: congenital malformation as a result of adhesions between ectoderm and endoderm; M÷F = 1÷3
Path:
(a) 2 hemicords each covered by layer of pia within single subarachnoid space + dural sac (60%); not accompanied by bony spur / fibrous band
(b) 2 hemicords each with its own pial, subarachnoidal + dural sheath (40%); accompanied by fibrous band (in 25%), cartilaginous / bony spurs (in 75%)
Associated with: myelomeningocele
• hypertrichosis, nevus, lipoma, dimple, hemangioma overlying the spine (26–81%)
• muscle wasting, ankle weakness in one leg; clubfoot (50%)
Location: lower thoracic / upper lumbar > upper thoracic > cervical spine
√ sagittal cleft in spinal cord resulting in 2 asymmetric hemicords which usually reunite caudal to cleft
√ occasionally 2 coni medullaris
√ eccentric central canal within both hemicords
√ bony spur through center of spinal canal arising from posterior aspect of centra (< 50%)
√ thickened filum terminale > 2 mm (> 50%)
√ tethered cord (> 50%)
√ low conus medullaris below L2 level (> 75%)
√ defect in thecal sac on myelogram
@ Vertebrae
√ congenital scoliosis (50–75%)
◊ 5% of patients with congenital scoliosis have diastematomyelia
√ spina bifida over multiple levels
√ anteroposterior narrowing of vertebral bodies
√ widening of interpediculate distance
√ narrowed disk space with hemivertebra, butterfly vertebra, block vertebra
√ fusion + thickening of adjacent laminae (90%)
(a) fusion to ipsilateral lamina at adjacent levels
(b) diagonal fusion to contralateral adjacent lamina = intersegmental laminar fusion
Cx: progressive spinal cord dysfunction
DISKITIS
◊ Most common pediatric spine problem!
Etiology:
(1) Bloodborne bacterial invasion of vertebrae infecting disk via communicating vessels through endplate
◊ Vertebral osteomyelitis + diskitis may be the same entity!
(2) Invasive procedure / trauma: surgery, diskography, myelography, chemonucleolysis
(3) Extension of adjacent infection
Organism:
(a) pyogenic: Staphylococcus aureus (> 50%), gram-negative rods (in IV drug abusers / immunocompromised patients)
(b) nonpyogenic: tuberculosis, coccidioidomycosis
◊ TB has a propensity to extend beneath longitudinal ligaments with involvement of multiple vertebral levels
Pathogenesis: infection starts in disk (still vascularized in children) / in anterior inferior corner of vertebral body (in adults) with spread across disk to adjacent vertebral endplate
Age peaks: 6 months to 4 years; 10–14 years; 6th–7th decade
• over 2–4 weeks gradually progressing irritability, malaise, low-grade fever; refusal to bear weight; myelopathy
• neck / back / referred hip pain, limp, focal tenderness
• elevated sedimentation rate, WBC count often normal
• positive blood culture (in 58%)
Location: L3-4, L4-5, unusual above T9
Distribution: 2 adjacent vertebrae + intervening disk
Plain film (positive 2–4 weeks after onset of symptoms):
√ decrease in disk space height (earliest sign) = intraosseous herniation of nucleus pulposus into vertebral body through weakened endplate
√ indistinctness of adjacent endplates with destruction
√ endplate sclerosis (during healing phase beginning anywhere from 8 weeks to 8 months after onset)
√ bone fusion (after 6 months to 2 years)
CT (SAG / COR reformatted images more sensitive!):
√ early loss of disk height
√ endplate irregularities ← destruction
√ vertebral body collapse
√ paravertebral inflammatory mass / abscess
√ epidural soft-tissue extension with deformity of thecal sac
MR (preferred modality; 93% sensitive, 97% specific, 95% accurate):
◊ Very sensitive modality early on in disease process!
√ ↓ marrow intensity on T1WI in 2 contiguous vertebrae
√ signal intensity of disk decreased on T1WI + increased on T2WI compared to skeletal muscle
◊ Fluid-sensitive sequence with fat suppression!
√ progressive destruction of vertebral body
√ in early stage preserved disk height with variable intensity on T2WI (often increased)
√ in later stages loss of disk height with increased intensity on T2WI (= intradiskal fluid)
CEMR:
√ focal enhancement of involved disk + adjacent vertebral endplates ± bone marrow
NUC (41% sensitive, 93% specific, 68% accurate on 99mTc-MDP + 99mTc WBC scans):
√ positive before radiographs
√ increased uptake in vertebral endplate adjacent to disk
√ bone scan usually positive in adjacent vertebrae (until age 20) ← vascular supply via endplates; may be negative after age 20
Dx: needle biopsy (77% positive) before IV antibiotics
Cx: (1) epidural / paravertebral abscess ← extension of infection
(2) kyphosis
Rx: immobilization in body cast for ~ 4 weeks
DDx: neoplastic disease (no breach of endplate, disk space often intact)
Postoperative Diskitis
Frequency: 0.75–2.8%
Organism: Staphylococcus aureus; many times no organism recovered
• severe recurrent back pain 7–28 days after surgery accompanied by decreased back motion, muscle spasm, positive straight leg raising test
• fever (33%), wound infection (8%)
• persistently elevated / increasing ESR
MR:
√ decreased SI within disk + adjacent vertebral body marrow on T1WI
√ increased SI in disk + adjacent marrow on T2WI often with obliteration of intranuclear cleft
√ contrast-enhancement of vertebral bone marrow ± disk space
DDx: degenerative disk disease type I (no gadolinium-enhancement of disk)
Pyogenic Spondylodiskitis
= INFECTIOUS SPONDYLODISKITIS
Pathophysiology: infection of anterior vertebral body (2° to rich blood supply) → extension into disk → extension into neighboring vertebra
Predisposed: diabetes mellitus, immunocompromised, IV drug abuse
Location: lumbar > thoracic > cervical spine
• insidious back pain, fever, chills, night sweats
• elevated ESR, elevated C-reactive protein, ±leukocytosis
DDx: (1) Dialysis-associated spondyloarthropathy (intradiskal fluid + enhancement uncommon, NO epidural / paraspinal abscess)
(2) Degenerative disk disease (hypointense T1 and hyperintense T2 endplate changes flanking a degenerated disk ± enhancement, NO fluidlike disk signal intensity, disk vacuum phenomenon)
DISLOCATION OF CERVICAL SPINE
= CRANIOCERVICAL DISSOCIATION
Atlantooccipital Dislocation
= ATLANTOOCCIPITAL DISTRACTION INJURY = ATLANTO-OCCIPITAL DISSOCIATION (AOD)
= disruption of tectorial membrane + paired alar ligaments resulting in grossly unstable injury
◊ Diagnosis difficult to make and easy to overlook at whole-body CT!
Cause: rapid deceleration with either hyperextension or hyperflexion → in up to ⅓ of high-velocity injuries
Age: in adults much less common than in children ← larger size of head relative to body, increased laxity of ligaments, shallow horizontally oriented occipitoatlantoaxial joint, hypoplastic occipital condyles
May be associated with: occipital condyle fracture
• neurologic symptoms: range from respiratory arrest with quadriplegia to normal neurologic exam
• discomfort, stiffness
Direction of dislocation / subluxation: anteriorly, posteriorly, superiorly (vertical = life-threatening)
Lateral radiograph:
√ Powers ratio (assessment for anterior subluxation) = BC÷OA ratio > 1 = ratio of distance between basion + spinolaminar line of C1 and distance between posterior cortex of anterior tubercle of C1 + opisthion (74% sensitive)
√ basion-dens interval (BD) > 12 mm on X-ray / 9.5 mm on CT without traction placed on head / neck
√ basion-axial interval > 12 mm anterior / > 4 mm posterior to posterior axial line (PAL)
√ atlanto-dental interval > 3 mm (man) / > 2.5 mm (woman):
√ “V sign” = cranially divergent predental lines ← transverse ligament injury
√ atlanto-occipital interval > 4 mm
√ atlanto-axial interval > 2.6–4 mm
√ > 10 mm soft-tissue swelling anterior to C2 + pathologic convexity of soft tissues (80%)
CT (≤ 1.25 mm thick sections, superior to radiographs):
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree