Fig. 13.1
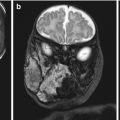
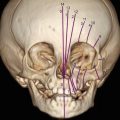
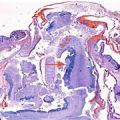
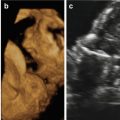
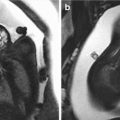
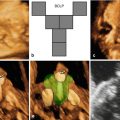
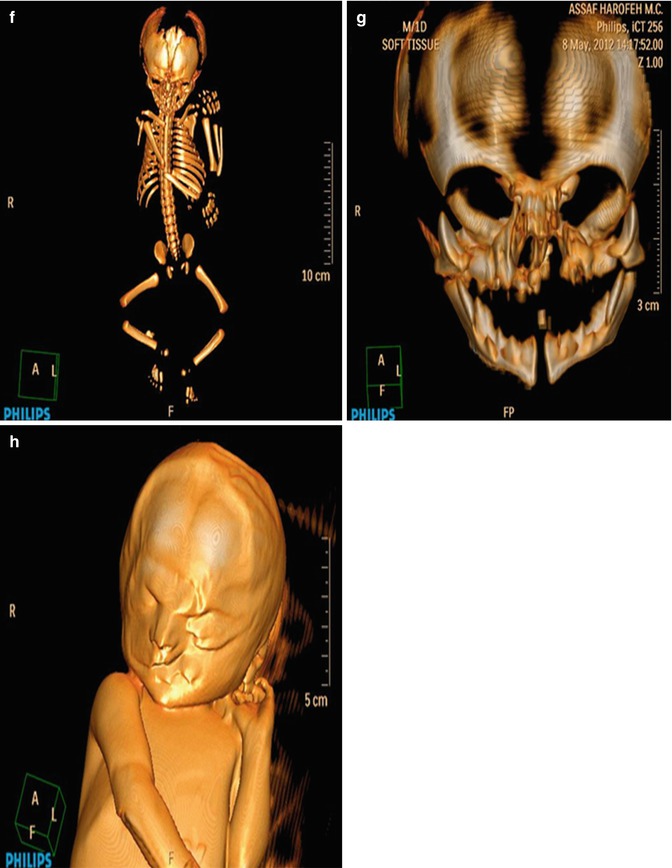
Representative images of the fetus and the postmortem findings. Prenatal 3D ultrasound in surface-rendering mode of the fetal face shows a wide, left-sided cleft lip with malformation of the ipsilateral eye (a). Same case using HDLive™ mode (b) and (c) skeletal mode. Postmortem findings show cleft lip and cleft palate (d, e). CT scan in 3D skeletal mode (f). Same modality showing cleft palate and the deformation of the maxillary bone (g). Volume reconstruction using 3D CT scan shows the bony defect of the palate (h)
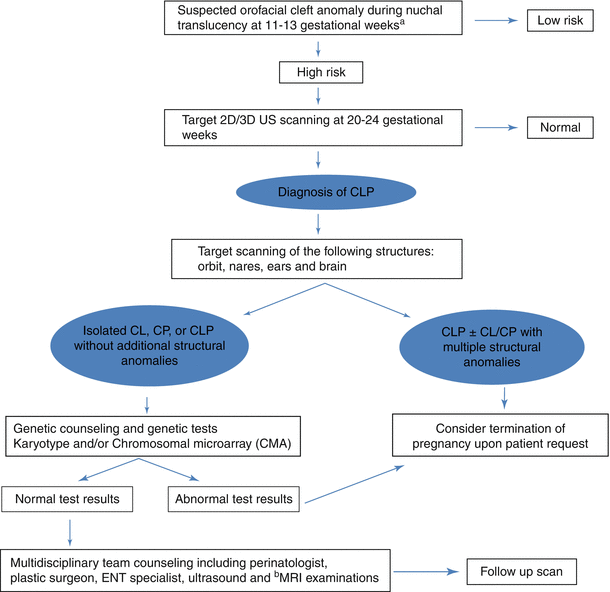
The patient requested legal termination of the pregnancy, which was approved by a special committee in accordance with our national law. Termination of pregnancy was conducted at 26 weeks of gestation and postpartum findings confirmed the prenatal diagnosis (Fig. 13.1d, e). The couple signed a consent form for postmortem pathological examination. A postmortem skeletal CT scan demonstrated a missing part of the maxillary bone on the left side causing a deformation of the left orbit base (Fig. 13.1f, g). A reconstructive computed tomography (CT REC) was also conducted, which demonstrated a left unilateral CLP extending to the level of the left orbit, but without involving it (Fig. 13.1h). This correlated well with the macroscopic evaluation of the abortus.
13.3 Discussion
The embryological pathways underlying facial clefting are well characterized. CL always begins at the lip and extends dorsally to various degrees (alveolus, hard palate, soft palate). CP is characterized as a cleft in the alveolar ridge or primary palate. CP always begins at the uvula and extends anteriorly through the midline, involving either the soft palate only or both the soft and hard palates. The lip usually fuses by 8 weeks of gestation and the palate by 12 weeks of gestation. On prenatal scan, CL is best visualized in the coronal plane and the alveolus is best viewed in the transverse plane. Sagittal views of the fetal head may show abnormalities, especially if the CLP is bilateral or midline and not unilateral.
A large Italian study [3] suggested that the best period for detecting facial defects is between 18 and 23 weeks of gestation, the same optimal period for the detection of major malformations in general as recommended by international ultrasound societies. However, early detection at 13–14 weeks of gestation by transvaginal sonography has been reported by Bronshtein et al. [14]. Recently, Tonni et al. [15] have evaluated facial clefting at 11–14 weeks of gestation using a novel 3D ultrasound technique, which reformats the retronasal triangle (RNT) [16]. Using the virtual navigation of the fetal palate with 3D ultrasound seems to be an accurate modality for diagnosis of clefting in the first trimester of pregnancy [17].
The success of ultrasound screening for CLP differs extensively among series. A Dutch study [18] found that screening for orofacial clefts in a low-risk population by transabdominal 2D ultrasound has a moderately low detection rate but low false-positive diagnosis with a substantial improvement in detection rate over time. Stoll et al. [19] showed that a systematic method improved the discovery rate of facial clefts from 5.3 % between the years 1979 and 1988 to 26.5 % between the years 1989 and 1998. Despite this, the rate of prenatal diagnosis of isolated CP is particularly low since a palatal defect will not be visualized on the standard oblique view of the face that is commonly used to assess the upper lip and alveolar ridge. Shadowing of the palate by the dense bony ridge makes the above visualization difficult [20]. A novel marker for the diagnosis of isolated cleft palate is the “equals sign” [21]. Due to the dome-shaped structure of the palate, it cannot be visualized in its entirety by 2D ultrasound. Because CP always begins at the uvula (uvula bifida as the mildest form) and continues anteriorly along the midline, the intact uvula is used as an indicator for an intact palate.
Two different techniques are described to identify the uvula. The first method is by obtaining a coronal section through the neck and the pharyngeal space, in which the uvula can be visualized cranial to the epiglottis. The normal uvula has a characteristic ultrasound appearance that highly resembles an “equals sign” (two hyperechoic lines with a hypoechoic intermediate space). Another method, which yields a higher success rate, is to take a transverse section through the head at the level of the thalamus. The transducer is moved parallel to this plane caudally until the nasopharynx is viewed centrally. By moving the transducer further in the caudal direction, the soft palate and the uvula are seen.
As a complementary tool to the conventional 2D ultrasound, 3D ultrasound has been introduced in order to perform a more accurate evaluation of orofacial malformations. The conventional 3D ultrasound display consists of the orthogonal display mode and the surface-rendering mode. The former mode permits the concurrent analysis of the three reference planes: sagittal, axial, and coronal. The primary palate is identified in the axial plane by visualizing the two front tooth buds and by rotating the volume for symmetric viewing of the anterior alveolar ridge. Surface-rendering mode allows imaging of the soft tissues of the face; this technique provides images that are very useful in counseling parents about the nature of the malformation. In addition, the maximum mode permits improved imaging of the bony structures.
Viewing the hard and soft palates involves manipulation of the orthogonal planes in the 3D volume obtained on routine surface rendering of the fetal face. A routine 3D sweep of the fetal face in the surface-rendering mode allows visualization of the skin and soft tissues of the face, including the lips. In the orthogonal planes within the multiplanar display, the lips and the anterior part of the palate may be evaluated. Further manipulation of the 3D volume to obtain oblique, axial, and sagittal planes permits evaluation of the uvula, which serves as a good landmark for guiding the examination of the soft and hard palates [22].
In 2003, an ultrasound technique called the 3D reverse face (3D RF) view was described by Campbell and Lees [23], which aimed to overcome problems of shadowing when evaluating the fetal palate. This technique proved to be simple, rapid, and quite effective at visualizing the palate and palatal defects. The fetal face is viewed by obtaining a 2D ultrasound of the profile (or near profile) and the volume box is adjusted to include the entire facial outline and cranium. The view bar is adjusted to deliver an optimized surface-rendered image of the face. After the lips are inspected, the view bar is scrolled until a view of the alveolar ridge is achieved. In order to achieve an unobstructed view of the retro-facial area, a return to the frontal view of the face and a 180-degree rotation is made to obtain a coronal plane. In this plane, the intact palate will usually be seen as a distinct line separating the nasal and oral cavity. The 3D RF technique is rapid and highly effective from 20 weeks of gestation onward. Attention should be paid to cases of tongue protrusion through the defect that can obscure the edges of the cleft. In addition, the “flipped face” technique allows for evaluation of the hard palate by obtaining a volume in the sagittal plane, visualizing the profile, and then flipping that profile on its head. After placing the marker dot in the region of the palate, the palate can be rendered with a narrow box. This yields an axial image of the primary and secondary palates [24].
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree