and Jurgen J. Fütterer2, 3
(1)
Department of Radiological Sciences, Oncology and Pathology, Sapienza University of Rome, Rome, Italy
(2)
Department of Radiology and Nuclear Medicine, Radboudumc, Nijmegen, The Netherlands
(3)
MIRA Institute for Biomedical Technology and Technical Medicine, University of Twente, Enschede, The Netherlands
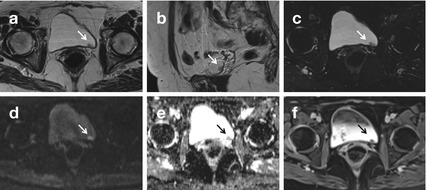
Benign Prostatic Hyperplasia
Benign prostatic hyperplasia (BPH), also called benign hypertrophy or hyperplasia, adenomatous hypertrophy, or simply adenoma, increases with age. Most benign hyperplasia occurs in the transition zone and only occasionally in the periurethral glandular zone. Sporadic BPH can be seen in the peripheral zone. Some enlarged glands contain cysts, calcifications, or even regions of hemorrhage.
Transrectal US can easily detect benign prostatic hyperplasia; it appears like a heterogeneous mass that dislocates the prostatic peripheral zone.
Due to poor parenchyma differentiation, CT is not as performed as MRI in evaluating BPH. BPH is hypointense on T1-weighted images and heterogeneous, ranging from hypo- to hyperintense, on T2-weighted images. It is difficult to discriminate between cancer and BPH, even with MR imaging.
Bladder Carcinoma
Primary bladder cancer is three times more common in men than women and more common in whites than blacks. Transitional cell carcinoma (TCC) is the most frequent cancer regarding the bladder, followed by adenocarcinoma, squamous cell carcinoma, sarcoma, and small cell carcinoma which are considerably less common and tend to occur in certain settings. Epithelial origin bladder neoplasms are uncommon in the second decade of life and rare in the first. Most bladder neoplasms at these ages are of mesodermal origin.
The most common clinical presentation is painless hematuria, ranging from gross to microscopic and often intermittent. Ureteral obstruction due to an adjacent cancer is often silent. Spontaneous perforation of a bladder carcinoma is a curiosity.
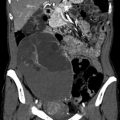
CT identifies a soft tissue tumor arising from the bladder wall. Depending on growth, these tumors range from a sessile polyp to bladder wall thickening. In general, CT misses lesions smaller than about 1–2 cm in diameter. Computed tomography also cannot distinguish adherent blood clots from a tumor. CT should be performed using oral and intravenous contrast with thin sections through the bladder with both a 70-s and a 5-min delay. The early images will serve to demonstrate hypervascular areas of the tumor, and the later images are sometimes valuable in outlining the tumor extent along the wall surface. Tumors may be polypoid or sessile and often extend to involve a large area of the bladder wall, including the ureterovesical junction (Fig. 1). Because transitional cell carcinoma is often multifocal, evaluation of the entirety of the urothelial tract should be attempted. Using multidetector CT scans with rapid reformatting, coronal images can be used to check the renal pelves and ureters for the presence of strictures and masses. All images should also be evaluated for the presence of increased number and size of pelvic and retroperitoneal lymph nodes and distant disease. In cases of advanced disease, CT is probably preferred because of its rapid acquisition and ease of interpretation.
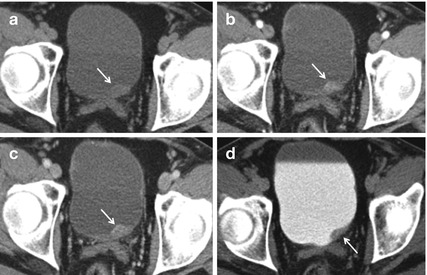
Fig. 1
In basal conditions, CT scans can barely outline a solid mass (white arrow) protruding into the bladder (a). After intravenous administration of contrast medium, the lesion is well represented both during arterial and venous phase (b, c). During the urographic phase (d), the tumor appears as an image of “minus” compared to the hyperdense bladder which is full of contrast medium
MRI: Magnetic resonance imaging offers several advantages over other imaging modalities. The multiplanar scanning capability and abundant inherent contrast between perivesical fat, soft tissue of the bladder wall, and urine in the lumen result in excellent contrast resolution. Images should be acquired in at least two orthogonal planes and with high-resolution small fields of view (FOVs). Phased-array surface coils are used to achieve the high resolution necessary for local staging. T1-weighted images are preferred for the depiction of the tumor, invasion into the adjacent fat or organs, and lymph node and bone marrow involvement. T2-weighted images are used to assess invasion into the bladder muscle, prostate, and seminal vesicles. With injection of gadolinium contrast, carcinomas involving the bladder mucosa and submucosa show early and prominent enhancement. On T2-weighted MRI, the muscular wall of the bladder is of homogeneously dark signal (Fig. 2). Extension into but not through the muscular wall is Stage II disease. Extension of high-signal mass through the wall indicates Stage III disease. Metastasis to a lymph node can be recognized if it leads to nodal enlargement. For local extension, T1-weighted, dynamic, post-Gd-DTPA enhanced images may be of help in delineating a mass from adjacent inflammatory stranding. Coronal images of the upper urinary tract, similar to those with CT or intravenous urography (IVU), can be obtained using a heavily T2-weighted coronal series, obtained either as a volume or comprising multiple slices. MRI shows that carcinomas have a T1-weighted signal intensity similar to that of muscle. T2-weighted images reveal a higher signal intensity than normal bladder wall or fibrosis. Tumor detection is superior with post-Gd-DTPA images, although one should keep in mind that both cystitis and tumors exhibit early MR contrast enhancement. The use of surface coils leads to better image quality than does the use of body coils. Endorectal coils improve visualization of the bladder base and dorsal structures but are of limited use for the rest of the bladder and should not be used. T1-weighted images provide good contrast between hyperintense perivesical fat and isointense bladder wall and detect perivesical fat invasion, spread to lymph nodes, and bone marrow metastases; the latter are identified against the hyperintense normal marrow. T2-weighted images evaluate bladder wall infiltration and prostatic and adjacent structure invasion, although differentiation between tumor and edema is difficult.