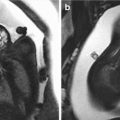
Fig. 12.1
(a, b) Sagittal 2D ultrasound views of the fetal profile show severe midfacial hypoplasia. Note the almost absent nose and severe depression of the midface. Moderate polyhydramnios was also present

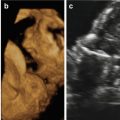
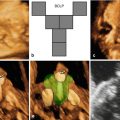
Fig. 12.2
(a, b) Three-dimensional surface-rendering ultrasound view of the fetal face show the characteristic features associated with the Binder phenotype
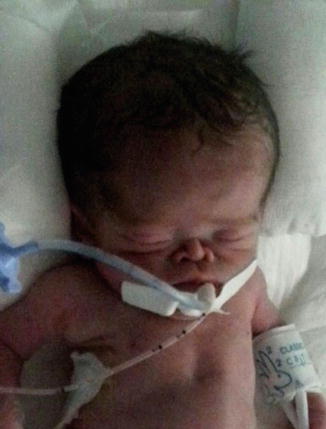
Fig. 12.3
Photograph of the neonate (with permission from the parents)
12.3 Prenatal Diagnosis
Binder syndrome has rarely been diagnosed during the prenatal period. Cook et al. [15] described a case diagnosed at 21 weeks of gestation during the routine second-trimester scan. 2D ultrasound identified nasal hypoplasia with reduced nasofrontal angle and mild hypertelorism. The karyotype was normal (46,XY). After discussion with geneticists, the leading differential diagnosis was Binder syndrome. After counseling, the parents decided to terminate the pregnancy and postmortem examination confirmed the facial dysmorphism, flat midface, mild hypertelorism, atresia of the right choanus, and stenosis of the left choanus. In this case, the suspicion of Binder syndrome was based on the flat nose as the primary abnormality, in contrast to other syndromes that usually are associated with multiple other malformations.
Cuillier et al. [16] described a case of Binder syndrome at 24 weeks of gestation. The routine second-trimester ultrasound demonstrated nasal hypoplasia with reduced naso-frontal angle. 3D ultrasound in rendering mode enhanced visualization of the abnormal facies. The karyotype was normal (46,XX). After discussion with geneticists and neonatologists, the main diagnostic hypothesis was Binder syndrome. The parents decided to continue the pregnancy and delivery occurred at 37 weeks of gestation. The neonatal exam confirmed the prenatal ultrasound findings.
In the largest case series of prenatal diagnosis of Binder syndrome, Levaillant et al. [11] described eight fetuses with Binder syndrome characteristics using both 2D and 3D ultrasound. The gestational age at diagnosis ranged from 22 to 31 weeks. All fetuses presented with verticalized nasal bones and abnormal convexity of the maxilla, consistent with the Binder profile appearance. Association with chondrodysplasia punctata was noted in five cases and one case was associated with exposure to warfarin in the first trimester of pregnancy.
As mentioned above, some authors consider Binder syndrome as a phenotype of chondrodysplasia punctata. Benaicha et al. [17] described a case of the prenatal diagnosis of chondrodysplasia punctata at 30 weeks of gestation that presented with flat nasal bridge and polyhydramnios with Binder profile. The karyotype was normal (46,XY). Furthermore, the ultrasound exam showed stippling of the vertebrae, coccyx, proximal femora, and tarsal and carpal bones with triangular hypoplastic tufts suggestive of brachytelephalangic type. The postnatal radiographic exams confirmed the prenatal diagnosis. Brachytelephalangic chondrodysplasia punctata is an X-linked inherited form and is caused by mutations in the arylsulfatase E gene and usually has a more favorable prognosis because psychomotor development is normal.
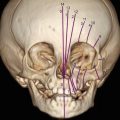
Boulet et al. [14] described another case of prenatal diagnosis of brachytelephalangic chondrodysplasia punctata performed at 23 weeks of gestation after the ultrasound exam revealed fetal midface abnormalities compatible with Binder phenotype and punctation of the upper femoral epiphyses. 3D computed tomography performed at 30 weeks of gestation confirmed the ultrasound diagnosis suspicion. Screening for Xp22 deletion and for maternal lupus was negative. Delivery occurred at 35 weeks and the postnatal radiology exam confirmed the Binder phenotype. On follow-up at 6 months, the psychomotor development was normal.
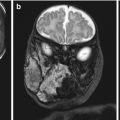
In another case of prenatally diagnosed brachytelephalangic chondrodysplasia punctata, ultrasound examination at 32 weeks of gestation showed polyhydramnios associated with Binder phenotype and low-set ears, thoracic hypoplasia, finger contracture, and cervicothoracic kyphosis. The karyotype was normal (46,XY). Magnetic resonance imaging demonstrated spinal canal stenosis with cord compression at the upper cervical level as well as a kyphotic deformity at the cervicothoracic junction. Delivery occurred at 34 weeks of gestation and the radiological exam confirmed brachytelephalangy of the hands. Computed tomography and magnetic resonance imaging confirmed the atlanto-axial subluxation with spinal cord compression [18].
12.4 Differential Diagnosis
The differential diagnosis of Binder syndrome includes other facial disorders, most of which are usually associated with genetic disorders (Table 12.1). Binder syndrome should be suspected when prenatal ultrasound identifies a low flat nasal bridge. Chondrodysplasia punctata is also associated with scoliosis and asymmetrical shortening of the limbs. Robinow syndrome is associated with short forearms, clinodactyly, and macrocephaly. Aarskog syndrome is associated with brachycephaly and clinodactyly of the 5th finger. Crouzon syndrome is associated with craniosynostosis and short occipital-frontal diameter. Apert syndrome is characterized by irregular craniosynostosis, short occipital-frontal diameter, flat occiput, ventriculomegaly, and syndactyly. Rudiger syndrome presents with short digits and talipes [19, 20]. Keutel syndrome is characterized by calcification and/or ossification of the cartilage in the external ears, nose, larynx, epiglottis, thyroid, trachea, ala nasi, and ribs; this syndrome also presents with peripheral pulmonary stenosis, sensory hearing loss, and borderline-to-mild mental retardation [21].
Table 12.1
Differential diagnosis in fetuses with sever midfacial hypoplasia
Syndrome | Facial Features | Other Features | Inheritance |
|---|---|---|---|
Binder | Flat midface Nasal hypoplasia | AR/AD | |
Robinow | Flat face Hypertelorism | Short forearms Clinodactyly Macrocephaly | AD |
Aarskog | Flat nose Hypertelorism | Brachy-/clinodactyly of the 5th finger | X-linked recessive |
Rudiger | Flat nasal bridge
Stay updated, free articles. Join our Telegram channel
Full access? Get Clinical Tree
 Get Clinical Tree app for offline access
Get Clinical Tree app for offline access

|