Case presentation
A 10-year-old male presents with left eye edema and pain for the past 2–3 days. The child reports mild congestion for the past week but there has been no fever, vomiting, cough, vision changes, eye discharge, or trauma. He states that it is difficult for him to completely open the eye because of the swelling. When he does, he complains of generalized eye pain. He has not had fever, although during your evaluation, you note that the child has a temperature of 100.9 degrees Fahrenheit, with a heart rate of 105 beats per minute, a respiratory rate of 18 breaths per minute, and a blood pressure of 100/75 mm Hg. The physical examination is unremarkable except for obvious left upper and lower eyelid edema with erythema and warmth. There is mild induration and no palpable fluctuance. The patient is able to open his eye, and you note there is no scleral edema or erythema; there is no obvious proptosis; there is no hyphema; his pupil is briskly reactive and equal with his other pupil. He has mild photophobia. When testing his extraocular muscles, the child complains of pain looking primarily medially and laterally. He has a nonfocal neurologic examination.
Imaging considerations
Imaging is often utilized to assist in distinguishing periorbital from orbital or intracranial complications and identifying patients who would benefit from surgical intervention. There have been studies that employed clinical findings, particularly proptosis and limited or painful ocular motion, to risk stratify patients who require imaging. , Not all patients have classic findings for orbital or intracranial involvement , and the decision to obtain imaging depends upon the patient’s presenting history, examination findings, and provider experience and index of suspicion.
Plain radiography
Orbital radiography may be of some use in a trauma setting, but this modality is not useful in children with suspected orbital infection.
Computed tomography (CT)
Intravenous (IV) contrast–enhanced CT is the imaging modality of choice to evaluate orbital infections and associated complications. Patients with signs of orbital infection (fever, severe eyelid edema, proptosis, pain with movement of the eye) or for whom physical examination is unreliable or unable to be properly performed (e.g., very young or uncooperative patients) are candidates for orbital imaging. A patient with no improvement (worsening clinical condition or persistent symptoms after 24–48 hours of appropriate antibiotics) or with neurologic findings on clinical examination should also undergo imaging. An abscess will first appear as a soft tissue density, evolving into a fluid-filled ring enhancing mass. CT is useful in identifying infection extent and the presence of an abscess but may not identify an abscess in its very early stages. Sedation is rarely required to obtain this study and this modality is readily available in most institutions. Although a disadvantage is exposure to ionizing radiation, which can be limited through the application of ALARA (as low as reasonably achievable) principles, the morbidity and potential mortality of not adequately identifying and treating an orbital infection and any associated complications are high.
Magnetic resonance imaging (MRI)
This modality provides superior resolution of orbital soft tissues compared to CT and is especially useful in the identification of subperiosteal or orbital abscesses. , MRI is also useful in detecting intracranial complications of orbital cellulitis. In cases where a diagnosis is unclear, MRI may provide delineation of infectious and other inflammatory processes. Gadolinium administration is typically used, but diffusion-weighted imaging has proven useful in abscess detection and may be considered in children with renal compromise. , However, MRI is not readily available in many centers and often requires sedation to obtain an adequate study.
Ultrasound
Orbital ultrasonography does not have a role in the identification of orbital cellulitis. It can detect orbital abscesses but lacks sensitivity compared to other imaging modalities, such as CT and MRI, and cannot image the posterior one-third of the orbit and sinuses.
Imaging findings
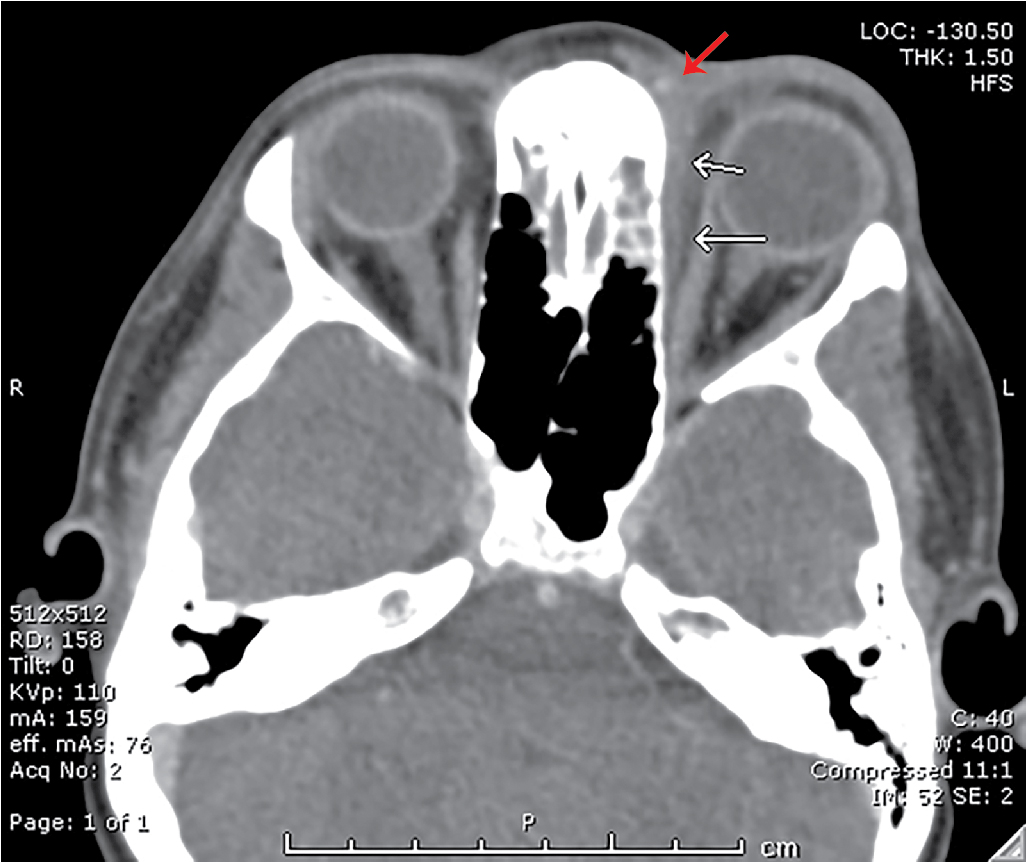
The child underwent IV contrast–enhanced orbital CT. Selected images are seen. There is a 3 mm × 18 mm × 7 mm left medial subperiosteal orbital abscess with slight lateral displacement of the medial rectus muscle. There is preseptal soft tissue edema and left ethmoid sinus opacification ( Figs. 34.1–34.3 ).