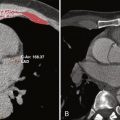
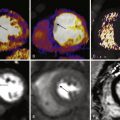
Catheter angiography refers to x-ray imaging of the blood vessels while contrast material is injected through an introducer (needle, catheter, or sheath) positioned within the vessel of interest. First developed by the Portuguese physician and neurologist Egas Moniz at the University of Lisbon in 1927, catheter angiography became popular with the introduction of a percutaneous arterial catheterization technique by Sven Ivan Seldinger in 1953. This technique, known as the Seldinger technique, eliminated the need for surgical exposure of the vessel before catheterization. Later, in 1964, Charles Dotter introduced the idea of catheter-directed therapy during the first femoral angioplasty. During the next 2 decades, catheter angiography flourished as the sole minimally invasive diagnostic tool for localization and characterization not only of vascular disease but also of other conditions such as neoplasms. With more recent developments in noninvasive vascular imaging techniques such as duplex ultrasound, computed tomography angiography (CTA), and magnetic resonance angiography (MRA), the role of catheter angiography in the diagnosis of vascular and nonvascular disease is diminishing. However, it still remains the gold standard for vascular imaging to which all other imaging modalities are compared. Despite its invasiveness, catheter angiography exceeds all other currently available noninvasive vascular imaging tests in providing the best temporal and spatial resolution for assessing the blood vessels. In addition, it is an integral part of all therapeutic vascular interventions.
The practice of angiography involves performing the procedure, as well as preprocedure patient evaluation, selection of appropriate hardware and technical parameters during the procedure, and appropriate postprocedure care. This chapter covers the basic principles and techniques of catheter angiography.
Preprocedural Clinical Assessment
Clinical assessment of patients before catheter angiography is required, to obtain the following information:
- 1.
Why does the patient require catheter angiography? Can the required information be obtained from other noninvasive vascular imaging studies? What additional information can catheter angiography provide if other noninvasive vascular imaging studies are already available? What level of selective angiography is required to answer the clinical question?
- 2.
Can the patient tolerate catheter angiography? If pharmacoangiography is planned, can the patient tolerate the pharmacologic stress?
- 3.
Is a therapeutic intervention planned? Is such therapeutic intervention better than or at least equal to the available alternatives?
- 4.
Was the patient educated and informed about the procedure, anticipated risks, and benefits?
Preprocedure assessment involves personal interaction with the patient or the family (especially if the patient is incapacitated) to obtain relevant medical history, perform physical examination, discuss the procedure, and obtain informed consent. Table 9-1 summarizes the checklist for preprocedure assessment.
| Medical History and Chart Review | History of present illness (the need for angiography) Relevant past medical history (especially about cardiac and renal function, hypertension, thromboembolic disease, bleeding diathesis, acute inflammatory disorders) Evidence of atherosclerotic disease (stroke, myocardial infarction, atheroemboli) History of bleeding disorders Allergies (especially to angiographic contrast materials) Current medications (especially metformin, which must be stopped 24 hr before and 48 hr after angiography, anticoagulants, and antiplatelet agents) Review of all available vascular imaging studies and vascular surgical procedures Previous laboratory results |
| Physical Examination | General cognition assessment to assess whether patient can provide informed consent Assessment of airway (for conscious sedation) Assessment of lungs, heart, peripheral pulses, and neurologic system (especially if supradiaphragmatic vessels or spinal arteries must be catheterized) Assessment of vascular access site |
| Laboratory Workup | Coagulation parameters: prothrombin time (PT), activated partial thromboplastin time (APTT), international normalized ratio (INR) Complete blood count: hematocrit, platelet count, white blood cell count Inflammatory markers (especially when angiography is planned in patients with inflammatory vasculitis; angiography not recommended if inflammatory markers are elevated in patients with active vasculitis) Renal function: estimated glomerular filtration rate, serum creatinine Liver function: required if hepatic arterial or portal venous interventions planned or if patient is clinically suspected to have hepatic dysfunction Electrocardiography: required in patients >70 yr old and in every patient who is undergoing pulmonary angiography Assessment of left ventricular ejection fraction: required as part of regular workup in patients with clinical signs of heart failure or any patient with significant cardiac history or pulmonary hypertension and in patients >70 yr old |
| Patient Instructions | Nothing by mouth for 6-8 hr before the procedure: required if conscious sedation planned for the angiography; otherwise, nothing by mouth for 3 hours before the procedure Clear liquids: can be consumed until 2 hr before the procedure Withholding medications: except for anticoagulants, patients receive their regular medications; insulin and antidiabetic medications may be reduced to half the regular dose if needed before angiography; warfarin (Coumadin) stopped ≥3 days before procedure to allow the INR to be at ≤1.5; low-molecular-weight heparins may be stopped 12 hr before procedure; metformin stopped 24 hr before procedure and restarted 48 hr later |
| Informed Consent | Informed consent obtained from patient or health care proxy after explaining procedure, anticipated risks, and benefits Estimated radiation dose and its effects discussed, in addition to other risks of angiography (see section on complications) |
Indications
Current indications for diagnostic catheter angiography are limited. Vascular diseases involving large and medium-size vessels can be well studied with duplex ultrasound, CTA, or MRA. The following are the current indications for catheter angiography:
- 1.
Assessment of small arteries
- a.
Detection of microaneurysms or steno-occlusive patterns in small arteries (e.g., in suspected inflammatory arteritis, noninflammatory arterial diseases such as fibromuscular dysplasia, and idiopathic or congenital microaneurysms)
- b.
Assessment of the distal arterial bed in patients with extensive peripheral arterial disease
- c.
Assessment of microvascular obstruction in patients with thromboembolic disease, thromboangiitis, frostbite, and other small vessel diseases
- d.
Assessment of smaller arterial anatomy before tissue transplantation
- a.
- 2.
Assessment of flow dynamics
- a.
Assessment of flow dynamics in patients with steal syndromes, arteriovenous fistulas or malformations, and tumoral shunting
- b.
Assessment of flow dynamics of collaterals in arterial and veno-occlusive diseases
- c.
Assessment of intravascular pressure to ascertain the hemodynamic significance of an obstructive lesion
- d.
Assessment of dynamic vascular occlusion secondary to arterial or venous compression from adjacent bony or muscular structures
- a.
- 3.
Assessment of arterial supply or venous drainage of a tissue or tumor
- a.
Accurate delineation of tumoral vascular supply, especially to assess the contribution of parasitized blood vessels
- b.
Assessment of venous drainage, which may be of paramount importance in patients with venous obstruction or when venous sampling is required in a suspected hormone-secreting tumor
- a.
- 4.
Assessment of in-stent stenosis, especially in small vessels
- 5.
Assessment of arteries and veins for vessel patency, course, and caliber when the information provided by other noninvasive modalities is inadequate
- 6.
Accurate localization of a bleeding source when the information provided by other imaging modalities is inadequate
- 7.
As part of pharmacoangiography
- 8.
As part of therapeutic interventions on blood vessels
Technique
Catheter angiography involves intravascular access, selection of the vessel of clinical interest, injection of contrast material into the vascular territory with simultaneous x-ray imaging, and safe removal of intravascular devices used for angiography. A brief review of these steps is provided in this section.
Premedication
Catheter angiography involves injection of contrast materials, which have the propensity to stimulate H 1 and H 2 histamine receptors, with subsequent development of allergic reactions. Other considerations include the risk of nephrotoxicity and cardiotoxicity associated with the contrast material. As such, premedication of patients with H 1 – and H 2 -receptor blockers (e.g., diphenhydramine and ranitidine) and adequate intravenous (IV) hydration (half-normal saline at 1 mL/kg/hour) are often recommended. Other renoprotective drugs such as N -acetylcysteine (Mucomyst, 600 mg twice a day, started at least 12 to 24 hours before the procedure) and sodium bicarbonate (150 mEq of sodium bicarbonate mixed in 850 mL of 5% dextrose in water [D5W] administered intravenously at 3 mL/kg 1 hour before the procedure and 6 hours after the procedure) may be given, although the superiority of these drugs over hydration is questioned. Adequate precautions should be taken not to overhydrate patients with poor left ventricular ejection fraction. Antibiotics are not required for diagnostic catheter angiography.
Patients with known allergy to contrast materials or who are at risk of contrast material–related allergic reactions should receive appropriate premedication (regimen 1:50 mg of oral prednisone 13 hours, 7 hours, and 1 hour before the procedure and 50 mg of oral diphenhydramine 1 hour before the procedure; or regimen 2: 125 mg IV methylprednisone, 50 mg of IV diphenhydramine, and 20 mg of IV famotidine just before angiography). Oral benzodiazepines such as midazolam are useful to alleviate anxiety in some patients. Conscious sedation may be used for diagnostic angiography.
Choice of Contrast Material
Currently, iodinated, nonionic, low-osmolar (iopamidol or iohexol) or iso-osmolar (iodixanol) contrast materials are typically used for catheter angiography. Although no maximum dose is suggested, doses in excess of 300 mL of contrast material should be avoided during angiography. Patients with renal failure or who are at risk of renal failure may benefit from alternative contrast materials such as carbon dioxide (CO 2 ). Understanding the compressibility and buoyancy of CO 2 during angiography is important. In addition, the use of CO 2 as contrast material during angiography requires digital subtraction angiography (DSA) and special image acquisition parameters. CO 2 is contraindicated for angiography of supradiaphragmatic arteries, given the risk of possible neurologic complications.
Selection of Hardware
Vascular access needles, guidewires, dilators, sheaths, and catheters are the basic tools for catheter angiography. The most commonly used vascular access needles are 18 gauge in diameter and range from 2.25 to 5 inch in length. They permit insertion of 0.038- or 0.035-inch helical spring guidewires. These needles have a central sharp stylet (the double wall puncture needles) that puncture the vessels through both the walls. The stylet is removed, and the needle is slowly withdrawn. The intravascular location of the needle tip is confirmed by visibility of blood at the needle hub ( Fig. 9-1 ). Vascular access needles without a stylet are also available, and these allow single wall puncture. A 21-gauge micropuncture needle is helpful in minimizing vessel trauma and is often preferred in patients with prolonged prothrombin time or activated partial thromboplastin time. A 21-gauge micropuncture needle permits the passage of a 0.018-inch guidewire. Then the puncture is upsized to a larger sheath.