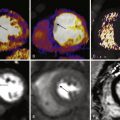
Significant advances in modern radiology and cardiology have made noninvasive cardiac imaging more effective and appealing. With the introduction of 64-slice computed tomography (CT) scanners in 2004, the improved spatial and temporal resolution allowed for accurate almost motion-free image acquisition of the coronary arterial system in a single breath hold of approximately 10 to 15 seconds. The use of cardiac CT angiography (CTA) has escalated exponentially, and cardiac CTA has become a common noninvasive imaging modality for the evaluation of cardiac diseases, especially coronary artery disease. In a multisocietal approach, experts have defined clinical situations for which cardiac CTA is considered appropriate. Cardiac CTA requires the use of ionizing radiation, however, and the potential risk of developing cancer from radiation exposure is a public health concern. Several strategies have been recommended and implemented to reduce the radiation dose associated with multislice CTA in cardiac imaging.
The desire to achieve low radiation exposure must be balanced with the likelihood of obtaining a useful diagnostic image. A nondiagnostic study may lead to additional imaging with substantially higher net radiation or to inappropriate invasive testing, delayed or lack of targeted treatment, or nontreatment.
How is Radiation Dose Estimated in Cardiovascular Computed Tomography Imaging?
The primary outcome parameters used to quantify radiation dose in cardiovascular CT imaging are the volume CT dose index (CTDI vol ) and the dose-length product (DLP). The physical details related to obtaining the CDTI vol are described by Morin et al. The CTDI vol is usually displayed on the CT console before and after CT data acquisition and allows the CT operator to compare the radiation doses that patients receive from different CT imaging protocols. The CTDI vol is unrelated to the length of the CT scan; in contrast, the DLP, which is the product of CTDI vol and the scan length, reflects the radiation exposure derived from a cardiovascular CT scan. The DLP, reported in milligray times centimeters (mGy × cm), is displayed after completion of the scan along with CTDI vol and can be used for estimating effective radiation dose and risk from a cardiovascular CT scan.
The radiation risk from cardiovascular CT imaging is typically estimated and expressed by the concept of effective dose (E), which is used in radiation protection as an estimate of the stochastic effect of a nonuniform radiation dose on a human. E, expressed in millisievert (mSv), can be estimated from sophisticated Monte Carlo simulations in which absorbed doses to various organs are adjusted by a weighting factor that accounts for organ sensitivity, patient age, and patient sex. In clinical practice, a reasonable estimate of effective dose can be obtained by multiplying the DLP provided by the scanner with a weighting factor (k), in which k depends on the exposed body regions. A k value of 0.014 mSv/mGy × cm for the chest is currently used for estimating effective dose from cardiovascular CT imaging procedures for adult patients.
How High is the Radiation Dose of Cardiac Computed Tomography Angiography?
Two large multicenter registries collected radiation dose data for coronary CTA. The Prospective Multicenter Study on Radiation Dose Estimates of Cardiac CT Angiography I (PROTECTION I), an international dose survey for cardiac CTA that included 50 study sites, collected representative radiation dose-relevant data for coronary CTA in 1960 patients. This study showed that cardiac CTA performed in 2007 was associated with a median DLP of 885 mGy × cm (value does not include radiation exposure from a localizer, coronary calcium scan, or contrast bolus timing scan). This DLP corresponded to an effective dose of approximately 12 mSv (interquartile range [IQR], 8 to 18 mSv). A second large registry included 4800 patients who underwent cardiac CTA in 2007 and 2008. Data were collected as part of a large multicenter interventional study by the Advanced Cardiovascular Imaging Consortium to investigate the effect of a formal program for lowering the radiation exposure from cardiac CTA. During a study period of 1 year, the investigators showed a 53% reduction in radiation exposure without impairment of diagnostic image quality. The median total DLP (including radiation exposure from a localizer, coronary calcium scan, or contrast bolus timing scan, when performed) was reduced from 1493 mGy × cm (21 mSv; IQR, 12 to 26 mSv) in the initial control period to 697 mGy × cm (10 mSv; IQR, 6 to 16 mSv) in the final follow-up period.
In the years following the publication of these two large cardiac CTA dose registries, progressive refinements in CT technology have resulted in decreased cardiac CTA radiation exposures. The details of these technical developments are described in more detail later.
Which Scan Techniques are Available for Cardiac Computed Tomography Angiography?
For many indications, correlation of raw CT data acquisition or reconstruction to the electrocardiogram (ECG) is required for obtaining images during a desired cardiac phase. This is accomplished using the ECG signal either to gate data acquisition retrospectively or to trigger data acquisition prospectively. These scan techniques encompass the retrospective ECG-gated helical low-pitch scan mode, as well as the prospective ECG-triggered axial and the prospective ECG-triggered helical high-pitch scan modes.
For those indications that do not require ECG synchronization, conventional helical scanning without ECG correlation is usually performed because it offers the advantage of shorter scan times compared with ECG-correlated scan modes on most CT systems. Such indications include pulmonary vein visualization before electrophysiologic ablation procedures or imaging of the descending aorta for stent planning. Non–ECG-correlated scan modes are often also associated with lower radiation exposures.
How Does the Retrospective Electrocardiogram-Gated Helical Low-Pitch Scan Mode Work in Cardiac Computed Tomography Angiography, and How is it Used to Keep Radiation Exposure Low?
The retrospective ECG-gated helical low-pitch scan mode is considered the conventional scan technique for ECG-correlated cardiovascular CT imaging because it is very robust and less prone to motion artifacts. With this scan mode, CT raw data are acquired during the entire cardiac cycle, with continuous rotation of the gantry and simultaneous table movement. By gating the simultaneously recorded ECG signal to the CT raw data and maintaining the tube current at a maximum throughout the cardiac cycle, image reconstruction can be performed at any time point during the cardiac cycle with identical image noise levels ( Fig. 27-1 ). This technique also allows for manipulation of the ECG gating process in patients with arrhythmias, such as deletion of extra systolic beats, insertion of missed beats, or shifting of R peak locations to adjust for arrhythmia. However, the resulting radiation dose associated with a retrospective ECG-gated helical low-pitch coronary CT scan often ranges between 15 and 20 mSv.

The ability to reconstruct high-resolution images with low image noise at any time point in the cardiac cycle is rarely needed in cardiovascular CT. In fact, in patients with lower heart rates, diagnostic image quality is usually achieved when images are reconstructed in mid-diastole to late diastole when coronary artery motion is at its least. Accordingly, large amounts of acquired CT data during the remaining time of the cardiac cycle are not needed for image reconstruction and thus are not needed for coronary artery assessment. When applying ECG-dependent tube current modulation (EDTCM), the tube current is modulated according to the ECG, with the maximum tube current during the relevant phases of the cardiac cycle and downregulation of tube current to a lower level (e.g., 20%) during the remaining phases. When this technique was applied to evaluation of the coronary arteries, a 40% reduction in radiation dose values was reported for retrospective ECG-gated helical low-pitch scanning with EDTCM in clinical practice ( Fig. 27-2 ).

Some CT scanners offer more “aggressive” downregulation of the tube current during the phases of cardiac cycle that are not necessary for image reconstruction. One of these algorithms, referred to as MinDose (Siemens Healthcare, Forchheim, Germany), reduces the tube current during phases not relevant for coronary diagnostic imaging down to a level of 4% ( Fig. 27-3 ). Images acquired during phases of 4% tube current are of nondiagnostic quality for assessment of the coronary arteries, but they may still be sufficient for functional cardiac diagnostic purposes. With the use of this advanced EDTCM algorithm, an additional radiation dose reduction of 30% or more can be achieved when compared with standard EDTCM algorithms.

How Does the Prospective Electrocardiogram-Triggered Axial Scan Mode Work in Cardiac Computed Tomography Angiography, and How is it Used to Keep Radiation Exposure Low?
When compared with retrospective ECG-gated helical low-pitch scanning, a considerable reduction of radiation dose can be achieved with the prospective ECG-triggered axial scan technique. In this axial mode, CT data acquisition is always prospectively triggered by the ECG signal during the desired cardiac phase while the examination table is stationary. Accordingly, radiation is applied only at a predefined time point of the cardiac cycle that is relevant for image reconstruction (i.e., the phase with greatest likelihood of minimal cardiac motion). Data acquisition is then suspended while the examination table is incremented to the next slice position, and the process is repeated until the entire scan range is covered ( Fig. 27-4 ). Because images can be reconstructed only during the prespecified phase of data acquisition, functional analysis is limited. Some additional data beyond the minimum required for image reconstruction (“padding”) can be acquired to permit minor retrospective adjustments of the reconstruction window, thus potentially reducing cardiac motion artifacts. These adjustments are associated with higher radiation exposures, however. As a consequence, the CT data acquisition window should be kept as narrow as possible.