Chapter 23 reviewed the technical issues and solutions for coronary artery cardiovascular magnetic resonance (CMR) imaging. This chapter reviews the clinical data comparing coronary artery CMR with invasive x-ray coronary angiography for identification of anomalous coronary artery disease (CAD), characterization of coronary artery aneurysms, detection of native vessel disease, and assessment of coronary artery bypass graft integrity. It also describes studies comparing CMR with coronary artery multidetector computed tomography (MDCT), the other principal noninvasive modality for imaging the coronary arteries. The majority of data represent single-center experience, with quantitative x-ray coronary angiography used as the reference standard for most of the larger single-center and few multicenter studies.
Identification of Anomalous Coronary Arteries
As discussed in Chapter 23 , using current whole-heart imaging with or without gadolinium contrast, the native proximal coronary arteries can be reliably visualized in nearly all subjects. Although unusual (<1% of the general population ) and most often benign, congenital coronary anomalies in which the anomalous segment courses anterior to the aorta and posterior to the pulmonary artery are well-recognized causes of myocardial ischemia and sudden cardiac death in children and young adults. These adverse events commonly occur during or immediately after intense exercise and are believed to be related to compression of the anomalous segment, vessel kinking, or coexistent eccentric ostial stenoses.
The ability of coronary artery CMR to reliably identify the major coronary arteries and their relationship to the ascending aorta and pulmonary artery immediately provides for its application for the identification and characterization of anomalous CAD. The spatial resolution requirements for identifying anomalous coronary vessels are less stringent than for defining native vessel stenoses, allowing for lower resolution and faster CMR imaging.
Projection x-ray angiography had traditionally been the imaging test of choice for the diagnosis and characterization of these anomalies. However, the presence of an anomalous vessel is sometimes suspected only after the procedure, particularly in a situation in which there was unsuccessful engagement of a coronary artery. In addition, the uncommon use of a pulmonary artery catheter has made characterization of the anterior or posterior trajectory of the anomalous vessels more difficult to appreciate on projection x-ray angiography.
Coronary artery CMR has several advantages compared with both coronary MDCT and x-ray angiography in the diagnosis of these coronary anomalies. In addition to being noninvasive and not requiring ionizing radiation or iodinated contrast agents, coronary artery CMR provides a definitive three-dimensional (3D) “road map” of the mediastinum ( Fig. 24.1 ). Early studies applied two-dimensional (2D) breath-hold segmented k -space gradient echo coronary artery CMR, although most centers now use targeted 3D or whole heart free-breathing navigator coronary artery CMR because of the superior reconstruction capabilities afforded by 3D datasets, with similar results. The ability to acquire these data using CMR without the use of ionizing radiation is likely to be of particular benefit in the generally younger population.

In addition, noncontrast coronary artery CMR is likely preferred to avoid potential long-term issues related to retention of gadolinium.
There have been at least eight published series of patients who underwent a comparison of coronary artery CMR at 1.5 T or 3 T with x-ray angiography for suspected anomalous CAD. These studies have uniformly reported excellent accuracy, including several instances in which coronary artery CMR was determined to be superior to x-ray angiography ( Table 24.1 ). Data also suggest coronary artery CMR evidence of a coronary anomaly carries important prognostic information with the identification of the anomalous segment originating from the opposite sinus of Valsalva (see Fig. 24.1 ) as conveying an adverse prognosis. As a result, CMR is considered a class I indication for suspected anomalous CAD. At experienced CMR centers, clinical coronary artery CMR is the preferred test for patients in whom anomalous disease is suspected, those with known anomalous disease that must be further clarified, and those with coronary anomalies associated with other cardiac anomalies (e.g., tetralogy of Fallot). Although MDCT has also been shown to be efficacious for this indication, coronary artery CMR is often preferred because there is no need for ionizing radiation or intravenous contrast.
| Investigator | Patients (N) | Correctly Classified Vessels |
|---|---|---|
| McConnell et al. | 15 | 14 (93%) |
| Post et al. | 19 | 19 (100%) a |
| Vliegen et al. | 12 | 11 (92%) b |
| Taylor et al. | 25 | 24 (96%) |
| Bunce et al. | 26 | 26 (100%) c |
| Razmi et al. | 12 | 12 (100%) |
| Tangcharoen et al. | 46 with congenital disease | 46 (100%) |
| Piccini | 16 | 15 (94%) |
a Including 3 patients originally misclassified by x-ray angiography.
b Including 5 patients unable to be classified by x-ray angiography.
c Including 11 patients unable to be classified by x-ray angiography.
Coronary Artery Aneurysms and Kawasaki Disease
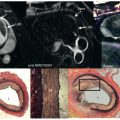
Coronary artery aneurysms are relatively uncommon, but have received increasing attention because of their common occurrence in pediatric and young adult patients with a history of mucocutaneous lymph node syndrome (Kawasaki disease), a generalized vasculitis of unknown etiology usually occurring in children age >5 years. The prevalence of Kawasaki disease is highest among children of East Asian countries, with the greatest prevalence in Japan. Infants and children with this syndrome may show evidence of myocarditis or pericarditis, with nearly 20% having coronary artery aneurysms. These aneurysms ( Fig. 24.2 ) are the source of both short-term and long-term morbidity and mortality. Fortunately, one-half of the children with coronary aneurysms during the acute phase of the disease have a normal-appearing coronary lumen on catheter-based x-ray angiography 2 years later. Transthoracic echocardiography is often adequate for diagnosing and following these proximal and mid-vessel aneurysms in very young children, but this modality is deficient after adolescence and in obese children. These young adults are therefore often referred for serial catheter-based x-ray coronary angiography, with the accumulation of significant radiation exposure over time. Coronary artery CMR data from two series of adolescents and young adults with coronary artery aneurysms have confirmed the high accuracy of coronary artery CMR for both the identification and the characterization (diameter and length [ Fig. 24.3 ]) of these aneurysms with addition of cine ventricular function and late gadolinium enhancement (LGE) for a comprehensive cardiac assessment. Although not specifically examined in long-term follow-up studies, these data suggest that coronary aneurysms can now be effectively followed with serial CMR studies, including vessel wall inflammation. Similar data have been reported for ectatic coronary vessels.


Native Vessel Coronary Artery Stenoses
Data support a broad clinical role for coronary artery CMR in the assessment of suspected anomalous CAD (and coronary artery bypass graft patency, which is addressed later), but data are not yet sufficient to support the use of clinical coronary artery CMR for routine identification of coronary artery stenoses among patients presenting with chest pain or for screening, even in high-risk patients. However, data suggest a role for coronary artery CMR among patients for the discrimination of ischemic versus nonischemic cardiomyopathy.
As discussed in earlier chapters, noncontrast gradient echo sequences show rapidly moving laminar blood flow as bright, whereas areas of stagnant flow or focal turbulence appear dark because of local saturation (stagnant flow) or dephasing (turbulence). Areas of focal stenoses appear as varying severity of “signal voids” in the coronary artery CMR, with the severity of signal loss related to the angiographic stenosis. Because of time constraints of breath-hold, 2D breath-hold coronary artery CMR has relatively limited in-plane spatial resolution, but the technique has successfully shown proximal coronary stenoses in several clinical studies ( Table 24.2 ). When reported, the distance from the vessel origin to the focal stenosis on coronary artery CMR correlates closely with x-ray angiography findings. However, there have been wide variations in the reported sensitivity and specificity of 2D coronary artery CMR, much of which may be attributable to technical and methodologic issues, including the wide variation in patient selection, presence of arrhythmias, prevalence of disease, the wide range of variation in technical implementation (CMR vendor, echo time, receiver coils, timing of acquisition, acquisition duration, and breath-hold maneuvers), and the need for 20 to 40 breath-holds to complete a study.
| Investigator | Subjects (N) | Vessels ( N, %) | Sensitivity | Specificity |
|---|---|---|---|---|
| Manning et al. | 39 | 52 (35%) | 90% (71%–100%) | 92% (78%–100%) |
| Duerinckx and Urman | 20 | 27 (34%) | 63% (0%–73%) | 56% (37%–82%) |
| Pennell et al. | 39 | 55 (35%) | 85% (75%–100%) | — |
| Post et al. | 35 | 35 (28%) | 63% (0%–100%) | 89% (73%–96%) |
Over the past decade, 2D coronary artery CMR has been supplanted by free-breathing 3D gradient echo or balanced steady-state free precession (bSSFP) coronary artery CMR with targeted 3D or whole heart approaches with or without contrast agents at 1.5 T and, increasingly, 3 T (see Chapter 23 ). The free-breathing, whole heart approach has higher patient acceptance, improved signal-to-noise ratio, and datasets that facilitate multiplanar reconstructions for improved visualization of the coronary arteries. As with noncontrast 2D gradient echo methods, a focal stenosis or turbulent flow with 3D gradient echo imaging appears as a signal void or marked narrowing of the lumen along the course of the vessel, with less dependence on blood flow characteristics (laminar vs. turbulent) with bSSFP imaging. Data from numerous single-center sites have been published using modern prospective navigator gating with real-time correction ( Table 24.3 ). Although assessment of the sensitivity of coronary artery stenosis was found to be similar for both source and projection images, our strong preference is to make diagnoses through review of the source images. We then use the projection images to convey our findings visually to the referring physician. An international, multicenter, free-breathing, noncontrast, 3D targeted coronary artery CMR study of 109 patients without previous x-ray angiography using common hardware and software showed high sensitivity (although only modest specificity) and negative predictive value of coronary artery CMR for the identification of coronary disease (>50% diameter stenosis by quantitative coronary angiography; Table 24.4 ). The sensitivity and negative predictive value were particularly high for the identification of left main or multivessel disease. Accordingly, coronary artery CMR was especially valuable for patients with dilated cardiomyopathy in the absence of clinical myocardial infarction. In our experience, coronary artery CMR is highly accurate and superior to LGE methods for determining the etiology (ischemic vs. nonischemic) of cardiomyopathy.
| Investigator | Subjects (N) | Technique | Sensitivity | Specificity |
|---|---|---|---|---|
| Prospective Navigators With Real-Time Correction Targeted Three-Dimensional Coronary Artery CMR | ||||
| Regenfus et al. | 50 | TFE | 94% | 57% |
| Bunce et al. | 34 | TFE | 88% | 72% |
| Moustapha et al. | 25 | TFE | 92% | 55% |
| 90% (proximal) | 92% (proximal) | |||
| Sommer et al. | 112 | TFE | 74% | 63% |
| 88% (good quality) | 91% (good quality) | |||
| Bogaert et al. | 19 | TFE | 85%–92% | 50%–83% |
| Plein et al. | 10 | TFE | 75% | 85% |
| Ozgun et al. | 14 | TFE | 91% | 57% |
| bSSFP | 76% | 85% | ||
| Dewey et al. | 15 a | bSSFP | 86% | 98% |
| Maintz et al. | 12 | TFE | 92% | 67% |
| bSSFP | 81% | 82% | ||
| Ozgun et al. | 20 | bSSFP | 82% | 82% |
| Jahnke et al. | 21 | bSSFP | 79% | 91% |
| Paetsch et al. | 18 | bSSFP | 83% | 77% |
| 18 | Contrast | 86% | 95% | |
| Sommer et al. | 18 | TFE | 82% | 88% |
| Prospective Navigator With Real-Time Correction Whole Heart Steady-State Free Precession Coronary Artery CMR | ||||
| Sakuma et al. | 39 | bSSFP | 82% | 91% |
| Jahnke et al. | 55 | bSSFP | 78% | 91% |
| Sakuma et al. | 113 | bSSFP | 82% | 90% |
| Nagata et al. | 62 | 32-channel SSFP | 83% | 93% |
| Klein et al. | 46 | bSSFP | 91% | 54% |
| Pouleur et al. | 77 | bSSFP | 100% | 72% |
| Greenwood et al. | 598 | bSSFP | 72% (M)/67% (F) | 90% (M)/88% (F) |
| Nagata et al. | 67 | bSSFP | 87% | 86% |
| Heer et al. | 59 | bSSFP | 86.7% | 79.3% |
| 1.5 T Self-Gated Postcontrast Whole Heart Coronary Artery CMR | ||||
| Piccini et al. | 40 | Postcontrast bSSFP | 71% | 63% |
| 3 T Whole Heart Coronary Artery CMR | ||||
| Sommer et al. | 18 | TFE | 82% | 89% |
| Yang et al. | 69 | Contrast IR-GRE | 94% | 82% |
a Based on 60% of patients with good free breathing coronary magnetic resonance images.
| Author | Field Strength | Patients (N) | Sensitivity | Specificity | PPV | NPV |
|---|---|---|---|---|---|---|
| Kim et al. | 1.5 T | 109 | 93% | 42% | 70% | 81% |
| Kato et al. | 1.5 T | 138 | 88% | 72% | 71% | 88% |
| Yang et al. | 3 T | 272 | 91% | 80% |
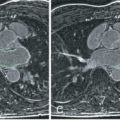
Data are increasingly available on whole heart bSSFP coronary artery CMR methods ( Fig. 24.4 ) with clinical results at least as accurate as those obtained with targeted acquisition free-breathing methods (see Table 24.3 ). A comparative study of whole heart gradient echo and whole heart bSSFP coronary artery CMR by Ozgun and colleagues suggested that gradient echo approaches had higher sensitivity, whereas bSSFP approaches had better specificity.

Increasing studies have examined the role of contrast-enhanced coronary artery CMR for the detection of disease. Paetsch and associates compared noncontrast 3D-targeted coronary artery CMR with an investigational intravascular agent using an inversion recovery prepulse. Superior specificity was found with the addition of contrast. Yang and coworkers using gadobenate dimeglumine (Gd-BOPTA, MultiHance, Bracco, Milan, Italy) with a 32-channel receiver coil at 3 T in 62 patients and found an overall patient, vessel, and segment accuracy of 92%, 94%, and 95%, respectively. In another study of 110 patients, they found a patient-based sensitivity and specificity of 96% and 87%, respectively.
A large number of the whole heart clinical studies have been led by groups led by Drs. Hajime Sakuma and Debiao Li, including multicenter trials in Japan and China, respectively (see Table 24.4 ). As expected, multicenter coronary artery CMR data are not as favorable as those reported in single centers, but multicenter coronary artery CMR and multicenter coronary MDCT data appear similar (discussed later). Available data suggest that 3D gradient echo coronary artery CMR findings at 1.5 T and 3 T are similar. A multicenter 3 T whole heart contrast-enhanced coronary artery CMR study by Yang et al. in 278 patients obtained diagnostic quality CMR images in 86% of patients with a sensitivity and specific of 91% and 80%, respectively.
A systematic review and metaanalysis of coronary artery CMR involving 24 reports and 1638 patients showed a pooled sensitivity of 89% (95% CI 63%–79%) and specificity of 72% (95% CI 63%–79%). The sensitivity of contrast-enhanced coronary artery CMR was higher (95% vs. 87% for noncontrast), and comparable with coronary MDCT. The specificity of 3 T coronary artery CMR was superior (83% vs. 68% for 1.5 T) as well as for whole heart acquisitions (78% vs. 57% for targeted acquisitions).
Comparison of Coronary Artery CMR and Other CMR Components
The multicenter Clinical Evaluation of Magnetic Resonance Imaging in Coronary Heart Disease (CE-MARC) study offered the unique opportunity to examine different components of the CMR examination (left ventricular function, myocardial perfusion, LGE, coronary artery imaging) for the detection of CAD ( Table 24.5 ) and suggests that coronary artery CMR image acquisition had the lowest technical success and offered no additional benefit for the detection of angiographic disease. A single center study by Heer et al. found that the combination of coronary artery CMR with adenosine stress perfusion improved overall accuracy from 78% to 92% for the detection of angiographically significant CAD. A 3T study by Zhang et al. involving 46 patients found the addition of contrast-enhanced coronary artery CMR resulted in higher sensitivity (100% vs. 76.5%) and accuracy (89% vs. 74%) with no change in specificity.