Summary Key Points
- •
Diagnosis of hydrops fetalis requires two or more of the following sonographic abnormalities: scalp and body wall edema (defined as skin thickness >5 mm), ascites, pleural effusion, pericardial effusion, polyhydramnios, and placental thickening (≥4 cm in the second trimester and ≥6 cm in the third trimester).
- •
Immune hydrops refers to cases in which the underlying condition is due to fetal anemia developing from maternal red blood cell alloimmunization. Nonimmune hydrops refers to cases resulting from all other conditions.
- •
Almost 90% of cases of hydrops are secondary to a nonimmune mechanism.
- •
For women with a prior history of a fetus or child with alloimmunization, defined as requiring intrauterine transfusion or exchange transfusions after birth, the use of serial maternal titers to identify the fetus at risk is not indicated because these measures are no longer predictive in these circumstances.
- •
Measurements of the peak systolic velocity (PSV) in the middle cerebral artery (MCA) are highly predictive of fetal anemia and are the preferred method to manage pregnancies at risk for immune hydrops.
- •
If MCA PSV measurements reach a value greater than 1.5 MoM (multiples of the median), fetal blood sampling via cordocentesis should be performed.
- •
During fetal transfusions, the blood should be transfused at a rate of 5 to 10 mL/minute, and if feasible, an attempt should be made to reach a final hematocrit of 50% to 65%.
- •
The most common causes of nonimmune hydrops are cardiovascular conditions, which include arrhythmias, structural abnormalities, and diverse cardiomyopathies.
- •
A fetal echocardiogram should be part of the initial evaluation of nonimmune hydrops.
Background and Definition
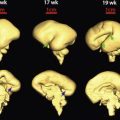
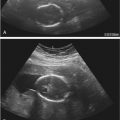
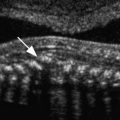
Hydrops fetalis has been defined as the pathologic accumulation of excessive fluid within two or more fetal compartments. These features can be detected sonographically and include scalp and body wall edema (defined as skin thickness greater than 5 mm), ascites, pleural effusion, pericardial effusion, presence of polyhydramnios (amniotic fluid index greater than 25 cm or maximum verticle pocket greater than 8 cm), and placental thickening (≥4 cm in the second trimester and ≥6 cm in the third trimester) ( Figs. 17-1 through 17-8 ).
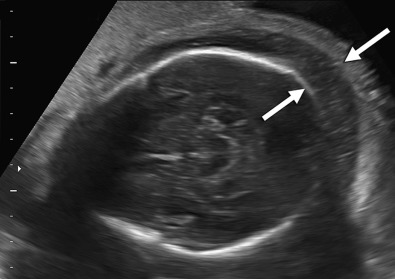
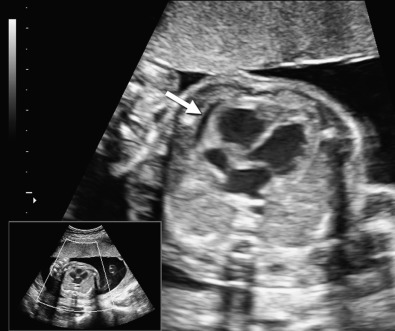



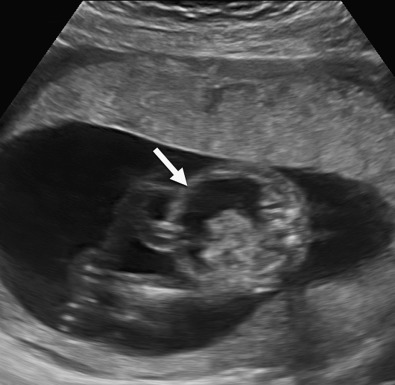


The use of this term should be limited to cases that meet the criteria outlined here because the diagnosis is associated with a poor prognosis and the workup for the cause may be extensive. The presence of one but not two of these criteria may be secondary to different causes and may also be associated with a better outcome than hydrops fetalis. In certain situations, the finding of a single abnormal fluid accumulation may be a sign of progressive and evolving hydrops fetalis and may warrant more frequent imaging and surveillance.
Based on the cause, the condition should be classified either as immune or nonimmune hydrops. Immune hydrops refers to all cases in which the underlying condition is due to fetal anemia developing from red blood cell (RBC) alloimmunization. The term nonimmune hydrops was reserved for the cases that resulted from all other conditions. Immune hydrops was probably first described in 1609 when a French midwife delivered a set of twins: the first one was hydropic and stillborn, whereas the second twin was noted to be severely jaundiced and subsequently died, most likely from kernicterus. This association was then again reported in 1932 when Diamond and colleagues described a disease characterized by anemia and jaundice that was associated with erythroblastosis and RBC hemolysis. Although the clinical features were described, the cause and pathogenesis were largely unknown. In 1938 Darrow described the concept of an antigen-antibody reaction leading to icterus gravis neonatorum. In 1940, the work by Landsteiner and Weiner led to the discovery of the rhesus (Rh) antigen that was expressed on the surface of RBCs. Later, in 1941 Levine and associates described the pathophysiology of the disease in a case series involving five patients. They observed that Rh-negative women form antibodies to Rh-positive RBCs, and transplacental passage of these antibodies to the fetus can lead to erythroblastosis fetalis.
Prevention of immune hydrops would have to wait decades. William Pollack, working in collaboration with Vincent J. Freda and John G. Gorman, developed a gamma globulin from anti-D serum. This gamma globulin was administered to RhD-negative inmates who then failed to develop anti-D antibodies when exposed to RhD-positive RBCs. At the same time, Finn and colleagues were also investigating the potential prevention of Rh hemolytic disease. They injected radioactive-labeled Rh-positive RBCs into Rh-negative men; they were able to demonstrate that administration of anti-D gamma globulin not only led to Rh-positive cells being coated by antibodies but also to a much more rapid destruction of these cells. Later, Hamilton treated RhD-negative women following their first delivery and showed that this strategy prevented formation of anti-D antibodies in the second pregnancy and led to improved perinatal outcomes. A subsequent multicenter clinical trial directed by Pollack led to the widespread use of anti-D immune globulin in clinical practice. The work by these pioneers helped the development of the current practice guidelines presently used throughout most of the world.
Incidence
The true incidence of hydrops fetalis is difficult to quantify. Many studies differ on the definition of cases included in their series as well as the study population. The reported incidence ranges from 1 : 424 to 1 : 2000 live births admitted to a neonatal intensive care unit (NICU). The widespread use of anti-D immune globulin has led to a decrease in the overall incidence of immune hydrops over the past few decades. Macafee and coworkers reported that in 1970, 82% of the hydrops cases were secondary to immune hydrops. The incidence of nonimmune hydrops has been reported to range from 1 : 1500 to 1 : 3800 births. More recent publications have reported a shift in incidence; currently almost 90% of cases of hydrops are secondary to a nonimmune mechanism.
Immune Hydrops
Mechanism
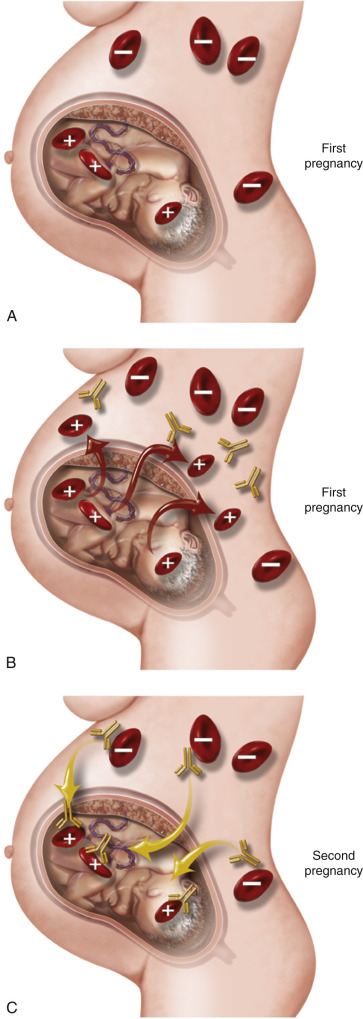
The pathophysiology of immune hydrops is exemplified by RhD isoimmunization. However, several other RBC antigens have been linked to the development of immune hydrops ( Table 17-1 ). The RhD antigen is one of the most immunogenic antigens expressed on the surface of RBCs ; other antigens differ in their ability to cause the disease. Maternal alloimmunization results from the exposure to foreign RhD-positive cells that eventually lead to an immunologic response. The most common cause of this phenomenon is a transplacental passage of fetal cells into maternal circulation, such as during a miscarriage, amniocentesis, trauma, or delivery ( Fig. 17-9 ). Using Kleihauer-Betke stain, as many as 75% of women have some evidence of the presence of fetal RBCs in maternal circulation during pregnancy or delivery.
| Antigen System | Specific Antigen | Antigen System | Specific Antigen | Antigen System | Specific Antigen |
|---|---|---|---|---|---|
| Frequently Associated With Severe Disease | |||||
| Kell | -K (K1) | ||||
| Rhesus | -D -c | ||||
| Infrequently Associated With Severe Disease | |||||
| Colton | -Co a -Co3 | MNS | -Mt a -MUT -Mur -Mv -s -s D -S -U -V w | Rhesus | -HOFM -LOCR -Riv -Rh29 -Rh32 -Rh42 -Rh46 -STEM -Tar |
| Diego | -ELO -Di a -Di b -Wr a -Wr b | ||||
| Duffy | -Fy a | ||||
| Kell | -Js a -Js b -k (K2) -Kp a -Kp b -K11 -K22 -Ku -Ul a | ||||
| Rhesus | -Be a -C -Ce -C w -C x -ce -D w -E -E w -Evans -e -G -Go a 7 -Hr -Hro -JAL | Other antigens | -HJK -JFV -JONES -Kg -MAM -REIT -Rd | ||
| Kidd | -Jk a | ||||
| MNS | -En a -Far -Hil -Hut -M -Mi a -Mit | ||||
| Associated With Mild Disease | |||||
| Dombrock | -Do a -Gy a -Hy -Jo a | Gerbich | -Ge2 -Ge3 -Ge4 -Ls a | Scianna | -Sc2 |
| Other antigens | -Vel -Lan -At a -Jr a | ||||
| Duffy | -Fy b -Fy3 | Kidd | -Jk b -Jk3 | ||
The risk of fetal-maternal hemorrhage also increases with gestational age: 0.01 mL of fetal blood may be detected in 3% of pregnancies the first trimester and 46% during the third trimester. The probability of alloimmunization is directly proportional to the amount of fetal blood that crosses the placental barrier. It has been estimated that 0.25 mL of fetal blood is the minimum amount required to lead to alloimmunization. For these reasons, delivery poses the greatest risk for Rh sensitization. The proper administration of RhD immune globulin, however, can effectively prevent the formation of maternal antibodies. Transfusion of incompatible blood can also lead to maternal sensitization; this is the most common mechanism explaining alloimmunization from other RBC antigens.
The genetics of the Rh system are complex. The Rh factor is among the largest of the blood groups and contains well over 50 different recognized antigens. Rearrangements in the Rh locus can result in hybrid proteins that can lead to additional antigen expression. Only a small number of these antigens are actually clinically relevant. During pregnancy there are three antigens that can lead to the formation of antibodies and alloimmunization, Rh (D) and Rh (CcEe). These antigens are encoded by two genes located on the short arm of chromosome 1, the RhD and RhCE genes. Each gene contains 10 exons. It has been speculated that through a mechanism involving alternative splicing these two genes could direct the synthesis of different proteins corresponding to different variations in Rh antigens. Fischer and Race have proposed a concept to explain the inheritance of the alleles in the Rh genes. In the majority of patients, three pairs of Rh antigens are inherited from each parent—Cc, Dd, and Ee. An individual can be heterozygous or homozygous for each allele. The Rh-positive or Rh-negative status of a patient is determined by the presence or absence (or possible nonexpression) of the D antigen site. The Rh (CcEe) has fewer alleles and a limited number of mutations reported. The Cc and the Ee alleles are codominant and expressed in a heterozygous fashion. It should also be noted that the symbol “d” simply indicates the absence of D antigen; there is no “d” allele.
The D antigen is a transmembrane protein located on the surface of the erythrocyte that contains several extracellular loops. More than 150 different alleles for the Rh (D) gene have been reported, most likely a byproduct of numerous mutations within the gene. The complete absence of the RhD antigen is called a negative allele. The gene frequency varies according to race and ethnicity. Rh-negative individuals are reported in approximately 1% of the Chinese and Japanese populations, whereas the Basque tribe in northern Spain has a reported incidence of approximately 30%. In the patient population of the Americas, the difference among races and various ethnic backgrounds is also noticeable. Caucasians of European descent have an Rh-negative incidence of 15%, whereas Hispanics and African Americans have an incidence closer to 8%. Among several African populations, a variant of Rh (D) gene referred to as the RhD pseudogene (Rh ψ) has also been described. This gene contains all the 10 exons normally found on the Rh (D) gene but has a difference in gene expression due to the presence of a stop codon in the intron between exons 3 and 4. Because of this change, the Rh (D) protein is not synthesized, and the patient is phenotypically Rh (D) negative. This gene is detected in more than 60% of Rh-negative black Africans.
After the first exposure to the D antigen, a weak immunologic response is mounted over 6 weeks to a year. The predominant immunoglobulin produced in this first interaction is immunoglobulin (Ig) M. This large protein does not cross the placenta, and therefore the first pregnancy is usually not affected. However, a second exposure to the antigen can cause B lymphocytes to differentiate into plasma cells and proliferate. This amnestic response in the immune system is characterized by the production of IgG almost entirely; these IgG antibodies can cross the placental barrier. Two IgG subclasses have been shown to be produced during this stage, IgG1 and IgG3. Disease severity appears to be lower in cases in which IgG1 is almost exclusively present.
Fetal erythropoiesis begins in the yolk sac by day 21. The Rh antigen can be expressed as early as day 30 of gestation. After the second exposure, there is an increase in the production of IgG antibodies leading to an increase in maternal titers. These antibodies recognize and attach to the foreign antigen on the fetal RBC surface. The IgG antibody lacks the ability to bind complement, and therefore, the antibody-coated fetal RBCs are sequestered by macrophages and are destroyed by the reticuloendothelial system extravascularly. This chain of events leads to the development of fetal anemia.
As the life span of the fetal RBC is reduced, a greater burden is placed on the hematopoietic system. It has been proposed that medullary hematopoiesis is stimulated in the early stages of mild anemia and that recruitment of extramedullary sites occurs only after anemia has progressed and become severe. This is evidenced by the fact that in severe disease, both the liver and the spleen become enlarged because of congestion and increased extramedullary hematopoiesis, causing the release of nucleated RBC precursors (erythroblasts). In a study evaluating umbilical cord samples from 127 pregnancies, Nicolaides and associates showed that significant erythroblastosis was present only when the hemoglobin deficit was greater than 7 g/dL ( Fig. 17-10 ). Severe anemia can lead to decreased oxygen delivery and hypoxia in certain end organs, causing cardiac output to increase as a compensatory mechanism. However, these mechanisms may be inadequate to maintain adequate perfusion. The loss of the buffer function of fetal RBCs also contributes to worsening acid-base disturbances. Soothill and colleagues reported an increase in the lactate concentration in the umbilical artery when hemoglobin levels were below 8 g/dL and an increase in umbilical vein concentration when this level dropped to 4 g/dL. This finding implies that disease progression leads to a shift in cellular metabolism to a predominantly anaerobic state.

The exact mechanism leading to fetal hydrops is incompletely understood. It is well known that anemia must be severe before hydrops develops and that fetal hemoglobin must fall below six standard deviations from the mean for that gestational age. Initial studies indicated that low fetal albumin levels leading to decreased colloid pressure and increased extravasation could be a contributing factor leading to hydrops. However, more recent studies have shown that hypoalbuminemia is found in only a small percentage of fetuses with hydrops and that drops in albumin levels appear to be a component of the very late stages of the disease. Other factors may also lead to increased vascular permeability facilitating the development of hydrops. Berger and coworkers demonstrated that concentration of ferritin and lipid-peroxidation products were increased, leading to the suggestion that iron overload and free radical damage may contribute to the pathogenesis. Cardiac dysfunction is also common among fetuses affected by severe anemia and could possibly play a role in the disease process. Affected fetuses develop an increase in both biventricular cardiac diameter and umbilical venous pressure. The increase in venous pressure may potentially lead to increased fluid extravasation, favoring the development of hydrops. The increase in venous pressure could also lead to an obstruction of lymphatic flow. Interestingly enough, it has also been shown that umbilical venous pressure decreases as early as 24 hours following therapeutic fetal intravascular transfusion.
Management
Severe fetal anemia that eventually leads to hydrops has direct implications for both fetal survival and long-term neonatal and infant outcomes. Cases of fetal anemia characterized by severe hydrops have a 74% survival rate compared to a 94% survival rate seen in nonhydrops cases. In a longitudinal study evaluating the long-term neurologic outcomes following intrauterine transfusion for RBC alloimmunization, over 95% of the 291 children followed were found to have normal developmental outcomes. However, a history of hydrops was found to be a significant risk factor for neurodevelopmental impairment.
Prevention is the key to management of alloimmunization. This starts at the first prenatal visit; a detailed history should be obtained from all patients. Specifics and details on past obstetric events as well as any previous transfusion of blood products are crucial to determining patients who may be at risk. Initial laboratory workup should include ABO typing with determination of RhD status as well as an antibody screen via a maternal indirect Coombs test. If a patient is found to be RhD negative, it should be determined if she is a candidate for prophylactic Rh immunoglobulin. If the antibody screen is positive, the blood bank should report the identity and the titer of the antibody. Titer levels are used to assess the likelihood of risk that the fetus may become affected. Antibodies that have been associated with hemolytic disease of the newborn are listed in Table 17-1 .
A repeat antibody screen for RhD should be done at 24 to 28 weeks. If this screen is negative, the patient is a candidate for anti-D prophylaxis via passive immunoglobulin administration. Although the exact mechanism of action is unknown, this strategy has been shown to be effective. In the United States, it is recommended that a single dose of 300 µg of anti-D immunoglobulin be administered at 28 weeks’ gestation. Immune prophylaxis probably works through the antigen clearance hypothesis. In this scenario, the administered immunoglobulin attaches to the RBCs. This interaction favors the removal of the coated cells by the mononuclear phagocytic system, particularly the macrophages, therefore not allowing these antigens to be recognized by the immune system. However, recent studies using several different animal models have shown that this hypothesis does not explain the entire mechanism of action. Other antigen-presenting cells, capable of initiating an immune response, also play a role in the clearance of D-positive RBCs.
After the administration of the immune prophylaxis at 28 weeks’ gestation, some experts recommend that a second dose of 300 µg be administered if the woman has not delivered within 12 weeks of her dose. One prophylactic dose of 300 µg of anti-D immunoglobulin is enough to prevent exposure produced by 30 mL of RhD-positive blood or 15 mL of fetal cells. Current guidelines dictate that if an RhD-negative woman delivers an RhD-positive infant, she should have a quantitative test (i.e., Kleihauer-Betke stain) done to determine the exact amount of anti-D immune globulin to be administered. The result of this test is typically multiplied by a factor of 50 to determine the total amount of fetomaternal hemorrhage. The dose should be administered within 72 hours of delivery, although this strategy has been shown to be effective up to 28 days after delivery. Also, women at risk for RhD alloimmunization should also receive a dose of prophylactic immunoglobulin after any obstetric event or procedure that puts her at risk for maternal-fetal hemorrhage.
Women who have been sensitized against RhD should have maternal antibody titer levels repeated every 4 weeks during the first and second trimesters and every 2 weeks during the third trimester in order to determine the risk of developing hemolytic disease. Maternal-fetal ABO incompatibility may be protective and decreases the risk of D alloimmunization. If a fetus is both RhD positive and ABO incompatible with the mother, this reduces the risk of alloimmunization to about 2%. Variations in the techniques used to determine the antibody level have led to the use of different thresholds to determine when a fetus is at risk for developing anemia. The titer value that is determined to be critical varies from 1 : 8 to 1 : 32. Clinicians should be familiar with the reference value used within their facilities.
Paternal testing can also be used to determine the risk of developing fetal anemia. RhD-positive fathers have a probability of being heterozygous. In the past, mathematical modeling along with ethnicity was used to determine the probability of heterozygosity. Advances in genetic testing have now allowed for the direct determination of paternal zygosity. If paternity is assured, this test can be used in the management algorithm of an RhD-negative woman. If the father is found to be heterozygous, the fetus has a 50% chance of being RhD negative. If the father is RhD negative, the fetus will likewise be RhD negative and therefore will not be at risk.
It has been estimated that 40% of RhD-negative women carry an RhD-negative fetus. For this reason, some have advocated for a more direct approach attempting to eliminate excessive testing and anxiety. Direct assessment of fetal blood type can be done via invasive prenatal testing. Amniocentesis can allow for the determination of the fetal genotype. Because genotype may not correlate with the RBC antigen expression in some rare instances, direct fetal blood sampling can also be used to determine the fetal phenotype. However, this technique is associated with a higher complication rate and a greater risk of fetal demise as compared to amniocentesis. Recently, newer noninvasive methods to determine fetal genotype have become available. As early as 1997, it was recognized that cell-free fetal DNA could be detected in the maternal circulation, with reports indicating that it was present in detectable quantities as early as 38 days’ gestation. Throughout the years, several companies developed different techniques to identify different loci on the fetal RhD gene. This test became commercially available in Europe and North America. Reports from several European centers specializing in the treatment of RhD disease started to emerge indicating the high accuracy of this test. A meta-analysis looking at over 30 articles concluded that the overall accuracy of this test was around 94% with a sensitivity of 95.4% and a specificity of 98.6%. Several European countries, with different patient populations and insurance payment plans, have started to adopt noninvasive RhD testing as part of the management protocol of women at risk for RhD alloimmunization with success. More worldwide widespread use was limited by the concerns of the lack of data regarding cost analysis. A recent cost analysis done in the United States by Hawk and associates concluded that with the current cost of RhD typing, routine antenatal anti-D immunoglobulin prophylaxis was still less costly. It is possible that with more automated techniques and increased competition driven by higher demand, the cost of testing may decrease, leading to the expansion of the acceptance of this test as part of the RhD alloimmunization management protocol. However, some have raised concern that, because cell-free DNA screening does not detect 100% of RhD-positive fetuses, routine use of cell-free DNA to target RhD immune globulin for RhD-negative women would cause increased sensitization compared with routine RhD immune globulin administration. Assays for detecting RhCc, RhE, and Kell typing via cell-free fetal DNA are also currently available.
Prediction of Anemia
Once a patient has been sensitized, there is a risk for fetal anemia. Several invasive techniques allow for the direct evaluation of fetal hemoglobin and hematocrit. Normally, fetal hemoglobin concentration increases with advancing gestation, and reference ranges for fetal hemoglobin have been established using fetal blood sampling ( Table 17-2 ). Cordocentesis can accurately detect fetal anemia; however, this technique carries with it a risk of pregnancy loss and fetal demise reported to range from 0.9% to 3.2%. Historically, another method used in the prediction of fetal anemia was through amniocentesis. Levels of bilirubin within the amniotic fluid were measured using the ΔOD 450 assay to predict hemolysis. The values obtained would be later plotted against published nomograms to determine the risk of severe fetal anemia This approach had the downside that in many cases serial amniotic fluid samplings were required to assess the severity and progression of the disease. These two procedures have been relegated to the past by the widespread use of sonographic Doppler evaluation of the middle cerebral artery (MCA).
| Gestational Age (weeks) | HEMOGLOBIN CONCENTRATION (g/dL) | |||
|---|---|---|---|---|
| 1.0 MoM (Median) | 0.55 MoM | 0.65 MoM | 0.84 MoM | |
| 18 | 10.6 | 5.8 | 6.9 | 8.9 |
| 19 | 10.9 | 6.0 | 7.1 | 9.1 |
| 20 | 11.1 | 6.1 | 7.2 | 9.3 |
| 21 | 11.4 | 6.2 | 7.4 | 9.5 |
| 22 | 11.6 | 6.4 | 7.5 | 9.7 |
| 23 | 11.8 | 6.5 | 7.6 | 9.9 |
| 24 | 12.0 | 6.6 | 7.8 | 10.0 |
| 25 | 12.1 | 6.7 | 7.9 | 10.2 |
| 26 | 12.3 | 6.8 | 8.0 | 10.3 |
| 27 | 12.4 | 6.8 | 8.1 | 10.4 |
| 28 | 12.6 | 6.9 | 8.2 | 10.6 |
| 29 | 12.7 | 7.0 | 8.3 | 10.7 |
| 30 | 12.8 | 7.1 | 8.3 | 10.8 |
| 31 | 13.0 | 7.1 | 8.4 | 10.9 |
| 32 | 13.1 | 7.2 | 8.5 | 11.0 |
| 33 | 13.2 | 7.2 | 8.6 | 11.1 |
| 34 | 13.3 | 7.3 | 8.6 | 11.1 |
| 35 | 13.4 | 7.4 | 8.7 | 11.2 |
| 36 | 13.5 | 7.4 | 8.7 | 11.3 |
| 37 | 13.5 | 7.5 | 8.8 | 11.4 |
| 38 | 13.6 | 7.5 | 8.9 | 11.4 |
| 39 | 13.7 | 7.5 | 8.9 | 11.5 |
| 40 | 13.8 | 7.6 | 9.0 | 11.6 |
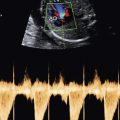
Advances in ultrasound technology have led to this technique now being the preferred method of prediction of fetal anemia. As mild to moderate anemia develops, the fetus responds with several compensatory mechanisms. The increased demand is thought to lead to increased ventricular output and stroke volume. These changes, along with a decrease in fetal blood viscosity secondary to the loss of RBCs, lead to an increase in flow velocity. Several fetal vessels were interrogated in an attempt to identify an easily accessible window for evaluation of blood flow. Measurements of the peak systolic velocity (PSV) in the MCA have been found to be highly predictive of severe fetal anemia. This vessel has the benefit of being easily identifiable with low intraobserver and interobserver variability. Because this measurement varies across gestational ages, the Collaborative Group for Doppler Assessment of the Blood Velocity in Anemic Fetuses has developed a reference in which the PSV measurement obtained is converted to multiples of the median (MoM) and used to predict the probability of fetal anemia ( Table 17-3 ). Using a hemoglobin concentration of 5 g/dL as a threshold, a cutoff of 1.5 MoM has been found to be highly predictive of severe fetal anemia requiring therapy in RBC alloimmunization affected pregnancies ( Figs. 17-10 and 17-11 ). This approach led to a false positive rate of approximately 12%. Later studies comparing the accuracy of this measurement to serial amniocentesis determined that this sonographic measurement has a better sensitivity and specificity. With the increasing experience and standardization in obtaining this measurement as well as the improvement in ultrasound technology, measurement of PSV in the MCA has become the surveillance modality of choice in alloimmunized pregnancies.
| Week of Gestation | PEAK VELOCITY (cm/s) | |||
|---|---|---|---|---|
| 1.00 MoM (Median) | 1.29 MoM | 1.50 MoM | 1.55 MoM | |
| 18 | 23.2 | 29.9 | 34.8 | 36.0 |
| 20 | 25.5 | 32.8 | 38.2 | 39.5 |
| 22 | 27.9 | 36.0 | 41.9 | 43.3 |
| 24 | 30.7 | 39.5 | 46.0 | 47.5 |
| 26 | 33.6 | 43.3 | 50.4 | 52.1 |
| 28 | 36.9 | 47.6 | 55.4 | 57.2 |
| 30 | 40.5 | 52.2 | 60.7 | 62.8 |
| 32 | 44.4 | 57.3 | 66.6 | 68.9 |
| 34 | 48.7 | 62.9 | 73.1 | 75.6 |
| 36 | 53.5 | 69.0 | 80.2 | 82.9 |
| 38 | 58.7 | 75.7 | 88.0 | 91.0 |
| 40 | 64.4 | 83.0 | 96.6 | 99.8 |

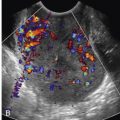
The MCA can be easily identified at the base of fetal skull. Color Doppler is utilized to identify the entire circle of Willis ( Figs. 17-12 and 17-13 ). The examiner should interrogate the MCA closest to the transducer. If this is not possible, evaluation of the MCA in the far field may provide reliable results. The 1- to 2-mm Doppler gate should then be placed just distal to the origin of the MCA from the carotid siphon. The ultrasound probe should be manipulated so a 0-degree angle of insonation is obtained. One approach to help achieve this angle is to start by obtaining the view for a biparietal diameter measurement. The probe should then be angled slightly toward the fetal skull and moved sideways in order to “tilt” the fetal head on the ultrasound screen. This will allow the MCA to be viewed in an almost completely vertical position. Angle correction can sometimes be used if the 0-degree angle insonation cannot be obtained effectively, although this approach is not preferred. Several measurements of the MCA PSV should be obtained, as these can be distorted by fetal movement or breathing. All measurements should have similar values to one another. The best measurement obtained should be used; the values obtained should not be averaged.


MCA PSV can be obtained as early as 16 to 18 weeks’ gestation. A multicenter prospective trial has shown that this measurement has a high false positive rate when measured after 35 weeks’ gestational age. Measurements should be repeated every 1 to 2 weeks depending on the clinical presentation. If MCA PSV measurements reach a value greater than 1.5 MoM, fetal blood sampling via cordocentesis should be performed. Should the fetal hematocrit be found to be below 30%, intrauterine transfusion is indicated. Many experts recommend that if the serial evaluation of MCA PSV remains below the established threshold, monitoring should be continued, with a plan for induction of labor at 37 to 38 weeks. Delivery is also warranted if there is any evidence of fetal compromise. Antenatal testing via nonstress test or biophysical profile should also be instituted starting at 32 weeks’ gestation.
Elevated MCA PSV after 35 weeks represents a therapeutic challenge. In the past, some investigators advocated performing amniocentesis to obtain both levels of bilirubin within the amniotic fluid measured using the ΔOD 450 assay as well as testing fetal lung maturity. However, the lack of familiarity with performing fetal lung maturity assays within several referral centers added to the fact that there has been a move toward abandonment of fetal lung maturity testing in well-dated pregnancies has led to the abandonment of the practice of amniocentesis beyond 35 weeks for this indication.
For women with a prior history of an affected fetus or child, defined as a fetus requiring intrauterine transfusion or exchange transfusions after birth, the use of serial maternal titers is no longer indicated because they are no longer predictive after an affected pregnancy. Fetal RhD status can be established; if the fetus is RhD positive, monitoring with serial MCA Doppler tests should commence around 16 to 18 weeks. Figure 17-14 summarize a proposed protocol for evaluation and management of affected pregnancies.


Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree