© Springer International Publishing AG 2017
Pietro Ruggieri, Andrea Angelini, Daniel Vanel and Piero Picci (eds.)Tumors of the Sacrum10.1007/978-3-319-51202-0_1717. Ewing’s Sarcoma of the Sacrum
(1)
Department of Orthopaedics and Orthopedic Oncology, University of Padova, Via N. Giustiniani, 3, Padova, 35128, Italy
(2)
Department of Surgery, University of South Florida, H. Lee Moffitt Cancer Center, Tampa, FL 33602, USA
17.1 Introduction
Ewing’s Sarcoma (ES) is a small round cells malignant tumor that accounts for 6–8% of all primary bone tumors. Together with osteosarcoma, they are the most common primary malignant bone tumors in children, most occurring during the first two decades [1, 2]. Primary ES of the spine and sacrum presents unique anatomic limitations specific to the neurological structures, vertebral column, and pelvic involvement, that challenge our ability to offer good local control. The use of multidrug chemotherapy, together with radiation therapy (RT) and surgery for local control, has significantly improved the prognosis of ES, even if it is still considered worse in the spine compared to other site [3–5]. Owing to the rarity of sacral tumors, the observations on long-term function and survival after treatment for high-grade sarcomas are limited to case reports or small series [6–10], surgical techniques [6, 11–14], or cooperative studies reporting cohorts that include but are not limited to sacrum [11, 15–22].
17.2 Epidemiology, Presentation, and Diagnosis
Primary Ewing sarcoma rarely affects the spine, and accounts for approximately 3.5–5% of the entire skeleton, falling down to 1% if the sacrum is excluded [3, 7, 20, 23–27]. Early diagnosis of sacral tumors is usually difficult because patients with a sacral tumor usually do not see a doctor until the symptoms become severe. Night or rest pain, swelling, and low-grade fewer are the most common presenting symptoms in early stages, followed by radiculopathy and major neurological compromise, such as bowel and bladder dysfunction. When delayed diagnosis occurs, tumor may reach a large size due to the lack of anatomic barriers or tumor growth into the pelvic region [2, 12]. Serum HDL and erythrocyte sedimentation rate are frequently increased, sometimes associated to leukocytosis and anemia.
17.3 Imaging
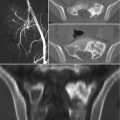
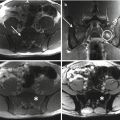
ES is a predominantly lytic lesion and may be seen on plain radiographs, better on lateral sacral view than anterior-posterior view. CT scans and MRI play a predominant role in evaluating the features, soft tissue and intramedullary/epidural extent of the lesion, and in developing a preoperative surgical plan [28]. ES may present with either a hot or cold bone scan [29]. CT-guided needle biopsy followed by immediate initiation of chemotherapy and corticosteroids for patients with stable neurologic deficits should be preferred to surgical decompression in conjunction with biopsy [17]. PET and dynamic MRI seem not to be predictive for tumor response to primary chemotherapy [30, 31].
17.4 Pathology
The histopathological diagnosis of Ewing’s sarcoma family tumors is based on the current criteria defined by the World Health Organization (WHO). Histologically, ES comprises small round blue cells originating from bone and soft tissues; the expression of neural markers distinguishes conventional ES from malignant primitive neuroectodermal tumors (PNET). The majority of cases share a cytogenetic translocation t(11;22) (q24;q12) with occasional variations and a characteristic immunohistochemical staining profile.
17.5 Treatment
The current treatment for ES includes multiagent neoadjuvant and adjuvant chemotherapy, with local control performed by surgical resection (when technically achievable) in combination with radiation therapy [5, 15, 32, 33]. Although Ewing sarcoma is highly sensitive to radiation therapy, at today surgery should be considered as treatment for local control. However, it is unclear whether and to what extent sacrectomy with wide margins provides local disease control, as well as the improvement of efficacy supported by new technologies in the field of radiation therapy [14, 17, 18, 34, 35].
17.5.1 Sacrectomy
Some authors consider that wide resection of the primary malignant sacral tumor is the only way to reduce local recurrence and cure the patient [12, 14, 26, 36], but this correlation is not clearly confirmed. As conclusion of a systematic review of the literature, en bloc resection of ES of the spine is weakly recommended as it provides improved local control, but not improved overall survival [15]. On the other hand, surgery with inadequate margins (both piecemeal excision and en bloc resection with intralesional margins) is associated with high recurrence rate and worse prognosis [16].
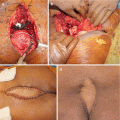
Clinical outcomes following sacral surgery parallel the level of neurologic sacrifice. Total or partial sacrectomy is a demanding procedure and may result in nerve root sacrifice, potentially causing major neurologic deficits and functional compromise, with high risk of complications (ranging from 32 to 67%, mainly infection) and a technical challenge in the reconstruction [6, 14, 21, 34, 37–40]. Patients who are able to retain one S3 nerve root and bilateral S2 nerve roots almost always regain functional bowel, bladder, and sexual capacity, while patients with higher levels of neurologic sacrifice have lesser capacity for these functions. Arkader et al. observed that despite the neurologic deficits and the associated psychological impact, survivor patients with sacrectomy are active participants in society [34].
17.5.2 Chemotherapy
Chemotherapy is critical in the treatment of ES [2, 5, 15], therefore sacrectomy without effective chemotherapy most likely would be insufficient to achieve disease-free status. Multiagent neoadjuvant chemotherapy is considered the standard in patients with ES, increasing the likelihood of local control and facilitating eventual surgical approaches [1, 2, 5, 15]. When ES is surgically treated, one of the most important prognostic predictive factors is the pathological evaluation of chemotherapy-induced tumor necrosis [5, 41]. Specific aspects on protocol of treatment are analyzed in the dedicated chapter.
17.5.3 Radiation Therapy
If en bloc resection is not feasible due to the lack of the criteria to perform wide resection or to unaccepted functional loss, the combination of radiation therapy (RT) and chemotherapy seems to be the best option rather than intralesional surgery [17, 18]. Previous experience has suggested that debulking procedures followed by RT do not improve outcomes in patients with Ewing tumor compared with RT alone [42], and intralesional dissection might result in tumor seeding [43]. With the advantages of new technologies, RT provides reasonable local control for ES of the spine with acceptable long-term toxicity in survivors, justifying its evaluation in alternative to surgical treatment [17–18].
17.6 Oncologic Outcome
The overall survival of primary high-grade malignant sacral tumors depends on the tumor type, presence of metastasis, response to chemotherapy, local control, and/or quality of surgical margins [11–15, 20–22, 34, 41]. The local recurrence rate is relatively high after surgery due to the location, the complex anatomy, and the difficulty in achieving safe margins. Bacci et al. [41] reported a series of spinal ES that includes 17 patients with sacral involvement. Authors reported their results with local recurrence rate of 29% and 5-year event-free survival rate of 0%, concluding that tumors primarily located in the sacrum have a much poorer outcome compared to those located in other bones. Guo et al. [14] reported a series on en bloc sacrectomies with only one patient affected by ES, that died of disease at 13 months of follow-up. Li et al. [13] reported a series including three cases of ES of the sacrum treated with hemisacrectomy, with two patients alive with no evidence of disease at 43 and 69 months of follow-up. Bradway and Pritchard underlined the importance of surgical resection considering that 6 out of 15 patients with sacral involvement remained alive compared to none of four patients with lumbar lesions [44]. Arkader et al. [34] reported a disease-free survival rate of 75% in children with osteosarcoma and ES of the sacrum, suggesting that sacrectomy has the potential to be curative. However, other authors reported good local control in nine cases with sacral involvement treated with radiotherapy only for local control (except one treated with surgery and radiation therapy), with 5-year EFS of 44% [17].
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree