Anatomy, embryology, pathophysiology
Anatomy and embryology of the liver is presented in Chapter 15 . This chapter will continue with pathophysiology of cirrhosis.
- ◼
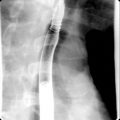
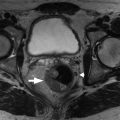
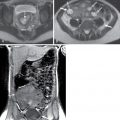
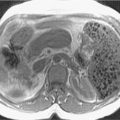
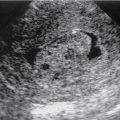
Cirrhosis is the final stage of chronic liver disease, which is characterized by diffuse parenchymal necrosis, regeneration and scarring with abnormal tissue reconstruction ( Fig. 16.1 ).

Fig. 16.1
Imaging signs of cirrhosis.
(From Roth C, Deshmukh S. Fundamentals of Body MRI , ed 2. Philadelphia: Elsevier; 2016.)
- ◼
Pathophysiology: Short-term or repetitive liver injury causes hepatocyte death. Collagen producing stellate cells are activated by cytokines, and fibrotic scarring occurs. Nodular regeneration accompanies fibrotic scarring.
Techniques
Ultrasound
- ◼
Ultrasound (US) should be the first choice imaging tool, because of its low cost, speed, use of safe acoustic waves and patient comfort. US can be used to evaluate general appearance, blood flow changes, anatomic deviations and possible cirrhosis related complications. High frequency probes may be useful to detect micronodularity along the liver surface. In cirrhotic patients, US is critically important to detect the complications of portal hypertension, like ascites and splenomegaly.
- ◼
Doppler imaging can be used to detect patency and direction of blood flow. Increased pulsatility of the portal vein tracing and loss of the normal triphasic hepatic vein tracing, may be signs of portal hypertension. Lesion vascularity can be assessed using Doppler imaging.
- ◼
US based shear wave elastography measures the transverse acoustic propagation in a localized tissue. Higher signal propagation speed (shear wave speed, in m/s) may represent more severe fibrosis formation. Shear wave speed can be converted to Young’s modulus (in kPA), which represents tissue stiffness.
- ◼
Contrast enhanced US (CEUS) uses microbubble based contrast. CEUS is useful to assess lesion vascularity in 3 phases: (1) arterial phase (15–30 seconds after administering contrast), (2) portal phase (30–60 seconds), (3) sinusoidal phase (60–240 seconds).
Magnetic resonance imaging
- ◼
On unenhanced T1-weighted magnetic resonance imaging (MRI), the cirrhotic liver has low signal intensity. Dual-phase in-phase and out-of-phase gradient images are useful to characterize T1 relaxation features and parenchymal or lesional fat content.
- ◼
On unenhanced T2-weighted MRI, the cirrhotic liver has high signal intensity. T2-weighted fast spin echo imaging is useful for bile duct, cyst and fluid collection assessment. T2-weighted imaging can also help differentiate regenerative nodules (RN) and dysplastic nodules (DN) types, but is not sensitive enough for hepatocellular carcinoma (HCC) characterization.
- ◼
In MR elastography, shear waves are generated by a 40 to 120 Hz mechanical inducer ( Fig. 16.2 ). Higher velocity and wavelength represent higher stiffness values.

Fig. 16.2
Magnetic resonance elastography. The static wave image (A) is one of a cinegraphic series of images depicting the propagation of the shear waves into the liver. The elastogram image (B) represents a tissue stiffness map that displays pixel intensity proportionally to stiffness. ROI measurements directly correspond to stiffness measurements in kilopascals (kPAs); in this case, stiffness measurements average approximately 2 kPAs, which is within the normal range.
(From Roth C, Deshmukh S. Fundamentals of Body MRI, ed 2. Philadelphia: Elsevier; 2016.)
Computed tomography
- ◼
For cirrhosis evaluation, the important phases of image acquisition are: late arterial (35–40 seconds), portal venous (60–80 seconds) and equilibrium phases (3–5 minutes).
- ◼
Early arterial phase images (20–25 seconds) can be useful to detect early enhancement of malignant lesions and to characterize lesion type.
Protocols
- ◼
Multiphasic computed tomography (CT) or MRI (≥1.5 T) based imaging can diagnose HCC. Biopsy of the lesion is not needed in most cases.
- ◼
Arterial enhancement, washout, enhancing capsule and venous invasion are critical for HCC detection in cirrhotic cases.
- ◼
Late arterial phase (35–40 s), portal venous phase (70–80 s) and delayed phase (3–5 min) should be part of a standard multiphase CT or MRI protocol.
- ◼
Precontrast and dynamic gadolinium enhanced T1-weighted gradient recalled echo, T2-weighted (with and without fat suppression), in-phase and out-phase T1-weighted sequences, and diffusion-weighed imaging should be added to the MRI protocol.
- ◼
Hepatobiliary and extracellular contrast agents are critical for cirrhosis and lesion characterization. Hepatobiliary contrast agents accumulate in hepatocytes and are excreted in bile. Extracellular contrast agents accumulate in the reticuloendothelial system, including Kupffer cells.
- ◼
Using extracellular agents, HCC can be easily diagnosed by arterial phase hyperenhancement and portal venous/delayed phase washout. Hepatobiliary agents are highly sensitive to detect small HCC lesions and premalignant lesions.
| PHASE | COMPUTED TOMOGRAPHY IMAGE QUALITY ASSESSMENT |
| Late arterial phase |
|
| Portal venous phase |
|
| Delayed phase |
|
Specific disease processes
Liver cirrhosis
It is important to remember that a normal appearance of the liver on cross-sectional imaging does not exclude cirrhosis. However, several imaging features have been proposed as characteristic findings of cirrhosis ( Fig. 16.3 ).

Ultrasound
- ◼
B-mode US has low sensitivity for fibrosis. Hyperechogenicity and poor visualization of liver vessels can appear in a cirrhotic liver on US. These findings are also common in steatosis, therefore the differential diagnosis may be challenging with B-mode images. Surface nodularity and caudate lobe hypertrophy are common findings in US imaging. Hepatomegaly and isoechoic RNs are other hepatic manifestations of cirrhosis.
- ◼
At a vascular level, dampened oscillations of the hepatic veins (resembling portal vein flow), dilation of intrahepatic hepatic artery branches, and increase in hepatic artery resistance are common US findings. On Doppler imaging, hepatofugal portal flow may be the sign of progression to end-stage liver disease, which requires shunt placement or liver transplantation. Diameters of portal vein greater than 13 mm, splenic vein greater than 11 mm, superior mesenteric vein greater than 12 mm may be signs of portal hypertension.
- ◼
Splenomegaly, ascites and dilated portal vasculature are common extrahepatic findings of cirrhosis on US.
- ◼
Stiffness values greater than 12.5 kPA may present cirrhosis on shear wave elastography. Transient elastography is another type of elastography technique, which is extensively used in gastroenterology clinics. Shear wave elastography uses real-time imaging that allows sonographers to image liver parenchyma and lesions ( Fig. 16.4 ). Transient elastography does not have a real-time imaging option ( Fig. 16.5 ).

Fig. 16.4
29-year-old man with nonalcoholic steatohepatitis related cirrhosis. Two-dimensional shear wave elastography technique provides real time imaging of the liver. Stiffness values are presented at the right side of the figure.

Fig. 16.5
33-year-old man with hemochromatosis caused liver injury and cirrhosis. Transient elastography operator collected 9 stiffness acquisitions. Stiffness values are presented in orange. Controlled attenuation parameter (used to quantify fat) values are presented in blue.
Magnetic resonance imaging
- ◼
On unenhanced MRI, extensive parenchymal heterogeneity may represent the combined appearance of fibrosis, RNs, perfusion abnormalities, and fat and/or iron deposition ( Fig. 16.6 ). Reticulations surrounding RNs may appear as intermediate-high signal intensity on unenhanced T1-weighted images and intermediate-low signal intensity on unenhanced T2-weighted images.

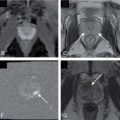
Fig. 16.6
Dynamic enhancement of fibrotic tissue in the cirrhotic liver. Dynamic contrast-enhanced (A), unenhanced portal venous phase (B) and delayed phase (C) computed tomography (CT) images show the nodular liver surface diagnostic of cirrhosis. The liver parenchyma is homogeneous, with neither fibrotic reticulations nor regenerative nodules clearly identified. Dynamic gadolinium-enhanced axial gradient recalled unenhanced (D), portal venous (E), and delayed (F) phase magnetic resonance (MR) images obtained at the same level as the CT images show progressive enhancement of the fibrotic reticulations as a result of accumulation of the low-molecular-weight gadolinium. Dynamic MR images depict the enhancement of the fibrotic septa ( arrows ) with higher clarity than CT.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree