Interventional Procedures
Aubrey J. Rybyinski
|
OBJECTIVES
Describe the benefits of sonography-guided interventional procedures.
Discuss the indications and contraindications for sonography-guided interventional procedures.
Explain the role of the sonographer during sonography-guided interventional procedures.
Discuss the difference between a fine-needle aspiration and a core biopsy and the benefits of each procedure.
List common sonography-guided interventional procedures and the potential complications involved in each.
KEY TERMS
abscess drainage
adrenal biopsy
breast biopsy
liver biopsy
lung biopsy
lymph node biopsy
musculoskeletal biopsy
pancreatic biopsy
paracentesis
prostate biopsy
pseudoaneurysm repair
renal biopsy
sonography-guided procedure
thoracentesis
thyroid biopsy
GLOSSARY
coagulopathy
a defect in the body’s mechanism for blood clotting
a defect in the body’s mechanism for blood clotting
core biopsy
a procedure that utilizes a hollow core biopsy needle to remove a sample of tissue frequently with a biopsy gun
a procedure that utilizes a hollow core biopsy needle to remove a sample of tissue frequently with a biopsy gun
fine-needle aspiration
a procedure that utilizes a small needle attached to a syringe, in which a vacuum is created and sample cells are aspirated for evaluation
a procedure that utilizes a small needle attached to a syringe, in which a vacuum is created and sample cells are aspirated for evaluation
fresh frozen plasma
a form of blood plasma that contains all of the clotting factors except platelets that is used to treat patients with a coagulopathy prior to interventional procedures
a form of blood plasma that contains all of the clotting factors except platelets that is used to treat patients with a coagulopathy prior to interventional procedures
international normalized ratio (INR)
a value used to standardize prothrombin time results between institutions because it adjusts for variations in processing; it is expressed as a number
a value used to standardize prothrombin time results between institutions because it adjusts for variations in processing; it is expressed as a number
partial thromboplastin time (PTT)
laboratory test used to evaluate for blood clotting abnormalities
laboratory test used to evaluate for blood clotting abnormalities
pneumothorax
a collection of air or gas in the pleural cavity of the chest between the lung and the chest wall that creates pressure on the lung
a collection of air or gas in the pleural cavity of the chest between the lung and the chest wall that creates pressure on the lung
prostate-specific antigen (PSA)
a laboratory examination that measures the level of PSA, a protein produced by the prostate gland, in the blood; an elevated level can indicate the presence of prostate conditions such as prostate cancer, benign prostatic hypertrophy, and prostatitis
a laboratory examination that measures the level of PSA, a protein produced by the prostate gland, in the blood; an elevated level can indicate the presence of prostate conditions such as prostate cancer, benign prostatic hypertrophy, and prostatitis
prothrombin time (PT)
laboratory test used to evaluate for blood clotting abnormalities; the time it takes the blood to clot after thromboplastin and calcium are added to the sample is recorded
laboratory test used to evaluate for blood clotting abnormalities; the time it takes the blood to clot after thromboplastin and calcium are added to the sample is recorded
pseudoaneurysm
a complication that can occur after cardiac catheterization or angioplasty in which a hematoma is formed by a leakage of blood from a small hole in the femoral artery
a complication that can occur after cardiac catheterization or angioplasty in which a hematoma is formed by a leakage of blood from a small hole in the femoral artery
The use of sonographic guidance has proven to be an invaluable asset to clinicians and patients for diagnostic and therapeutic procedures. Sonographic guidance techniques are continuing to improve with advances in transducer and equipment technology as well as increased operator experience. Sonographic guidance is frequently used for localizing organs, masses, and fluid collections in the abdomen, chest, neck, pelvis, and retroperitoneum. The most successful sonography-guided procedures have all the personnel involved work together as a team, and this includes the sonographer, physician, nurse, cytologist, and patient. This chapter focuses on those guidance procedures performed within the sonography department.
SONOGRAPHY-GUIDED BIOPSY
Percutaneous biopsy has become the widely accepted technique for confirmation of suspected malignant masses and characterization of many benign lesions in various locations throughout the body. Many of these masses are in locations that once required computed tomography (CT) guidance or open surgery, but now equipment and procedures allow for successful sonography-guided biopsy. The popularity of sonography guidance has increased steadily because it is minimally invasive, accurate, and relatively safe. Minimally invasive procedures are cost effective because patients may not require complex surgical interventions, long hospital stays, or excessive recovery times. In many cases, patients leave the same day after the procedure and quickly return to their normal activities. The ability to accurately characterize a disease lowers the number of additional examinations to confirm diagnosis, potentially decreasing the amount of radiation exposure.
Unlike other imaging modalities, sonography is readily available, inexpensive, and reproducible and can provide guidance in multiple imaging planes, allowing for multiple patient positions and approaches to be considered. The greatest advantage, however, is that it permits the real-time visualization of the needle tip because it passes through tissue planes into the target area. This allows for precise needle placement and avoidance of important structures. Studies have shown that an accurate diagnosis can be made in 95% of cases regardless of the sample size. In addition, color flow Doppler imaging can help prevent complications by identifying and helping the clinician to avoid vascular structures that may be in the needle’s path.
Traditionally, the use of sonography for guided biopsy was for large, superficial, or cystic masses. With improvements in technology and biopsy techniques, small, deeply located, and solid masses can also undergo successful and accurate biopsy. Biopsy of deep masses and masses in obese patients can be difficult with sonography because of the difficulty in lesion visualization resulting from sound attenuation in the soft tissues. Similarly, not all lesions can be visualized by sonography because they may be isoechoic to the surrounding tissues. Lesions located within or behind bone or gas-filled bowel cannot be visualized because of nearly complete reflection of sound from the bone or air interface. Frequently, biopsies of the breast, liver, kidney, prostate, thyroid, parathyroid, and cervical nodes are easily performed. However, other sites within the body can undergo biopsy if the lesion is adequately visualized. A good rule of thumb is that any mass that is well visualized on ultrasound should be amendable to a sonography-guided biopsy. A major factor in the success of sonography-guided biopsy lies in the experience and comfort level of the sonographer and radiologist.1
Indications and Contraindications
A biopsy is performed to definitively diagnose the nature of a lesion. The major indication for biopsy is the suspicion of either primary malignancy or metastatic disease. As a diagnostic tool evaluating potentially malignant conditions, biopsy is indicated for initial evaluation before both surgical and nonsurgical interventions such as the administration of chemotherapy or radiation. For example, a biopsy could be performed to differentiate a metastatic mass from a second primary malignancy in a patient with a known primary malignancy. Frequently, biopsies are performed to evaluate the nature of an indeterminate lesion, such as a solitary solid hepatic mass in a patient with no history of malignancy. Infrequently, a biopsy is performed for the confirmation of a mass that is suspected of being benign.2,3
The three contraindications to needle biopsy include uncorrectable coagulopathy, unsafe biopsy route, and an uncooperative patient. Although there are studies stating that compromised coagulopathy is not a contraindication for fluid aspiration and superficial or low-risk biopsies, it is presented to provide general knowledge.4 If the patient’s coagulopathy is unavailable within the patient’s medical record, the patient should get routine lab tests, known as a coagulation study. The three tests—prothrombin time (PT), partial thromboplastin time (PTT), and international normalized ratio (INR)—measure the time it takes for the blood to form a clot. These tests are simple, and results are usually available within 2 to 3 hours. Owing to the variability of the PT and PTT values between institutions, the World Health Organization implemented the INR. This value standardizes results between institutions because it adjusts for variations in processing and is expressed as a number.
Mild coagulopathies may occur secondary to the use of blood thinners, such as Plavix, aspirin, and warfarin, and some antibiotics.5 If a coagulopathy is present, the procedure may be delayed and the causative drug discontinued until the laboratory values return to normal. Patients who cannot wait for values to normalize can be administered fresh frozen plasma or vitamin K. An important consideration is given to patients in whom the need for biopsy outweighs any risk.
The choice of biopsy route is crucial to success, and a safe route must be chosen. A biopsy path going through major vessels or highly vascular structures increases the risk of hemorrhage. Bowel, the trachea, and other adjacent organs must also be avoided. An uncooperative patient also contraindicates needle biopsy. Patient cooperation is necessary for success because uncontrolled motion during the biopsy increases the potential for laceration and hemorrhage. It may be necessary to administer a form of sedation to a potentially uncooperative pediatric, senile demented, or mentally challenged patient.6
Types of Sonography-Guided Procedures
Sonography can be used for biopsies, core biopsies, needle placement for fluid drainage or mass localization (including fiducial marker or post-biopsy clip placement),
insertion of a nephrostomy tube in an obstructed kidney, and collecting fluid from an abscess. Most often, the biopsies are used to confirm if a lesion is benign, malignant, or infected to help determine an appropriate treatment plan. These methods are less invasive than open and closed surgical procedures because the incisions of the latter are much larger and require some level of local or general anesthesia.
insertion of a nephrostomy tube in an obstructed kidney, and collecting fluid from an abscess. Most often, the biopsies are used to confirm if a lesion is benign, malignant, or infected to help determine an appropriate treatment plan. These methods are less invasive than open and closed surgical procedures because the incisions of the latter are much larger and require some level of local or general anesthesia.
Fine-Needle Aspiration
Fine-needle aspiration (FNA) with sonographic guidance is a widely accepted technique for the confirmation of suspected malignant masses and characterization of many benign lesions in various locations. Even with a palpable, discrete lesion, ultrasound allows controlled sampling of different regions within the lesion. For this type of biopsy, a “fine” or “thin” needle, most often 20G to 27G, is utilized and attached to a syringe (Fig. 26-1). These needles allow for multiple passes and are considered low risk because of the needle’s relative thickness. As the name indicates, this technique uses aspiration to sample cells or fluid from a mass and is optimal for lesions lying superficially or at a moderate depth.2 Specimens may also be obtained using a capillary action technique involving an up-and-down motion of the needle within the mass. This technique reduces trauma to the cells, which in turn decreases the amount of background blood on cytologic evaluation. FNA is a reliable and safe method of obtaining tissue samples, allowing cellular evaluation for cytologic examination. FNA success is measured in terms of aspirating enough cells and maintaining patient comfort. The overall accuracy increases when a cytopathologist evaluates the specimens during the procedure to determine if additional tissue aspiration is required for diagnosis.7 With FNA, the cells are disorganized and no longer maintain the spatial arrangement they originally had in the lesion. In order to preserve the spatial arrangement of the cells, a core biopsy sample must be taken.8 FNA is performed predominately on thyroid nodules, parathyroids, and lymph nodes. It is important to make sure that the appropriate transducer is selected. The transducer should offer the highest frequency while maintaining visualization of the area to be sampled.
Core Biopsy
A core needle biopsy is a procedure that involves removing small samples of tissue using an automated hollow core needle commonly referred to as a “biopsy gun” (Fig. 26-2). The biopsy gun makes a loud noise when activated. It is important to make the patient aware of the noise to minimize patient alarm and patient motion during the procedure. As the name implies, the core biopsy needle facilitates the removal of a core sample of tissue and is a larger gauge than the needle used for FNA. Core biopsy needles are most often 14G to 19G, offer various throw lengths, and have a tissue-cutting tip. The device is cocked and then inserted within the mass. A button is then pushed lunging the needle forward, which takes and stores a sample within a slot on the inner needle. In a core biopsy, the larger needle allows for a “core” tissue sample for analysis. The larger sample can be recut into smaller samples, which can be used for further analysis, offering a more definitive histologic evaluation.9 The larger sample can aid in the diagnosis of parenchymal disease, involving the breast, kidney, liver, prostate gland, and transplanted organs.
Needle Selection
Each biopsy technique has its advantages and disadvantages, as does each needle type. There are a wide variety of needles commercially available, which vary in gauge, length, and tip configuration. An important consideration when choosing the appropriate needle is the amount of tissue required for accurate pathologic diagnosis.10 The bore size of the needle is inversely related to its gauge. For example, a 16G needle will offer a larger specimen than a 27G needle. The choice of needle should be made with respect to the area being sampled and the risks that may be increased due to complications associated with larger bore needle.
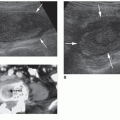
Although real-time visualization of the needle is one of the greatest strengths of sonography, it is often the most technically challenging. The sonographic appearance of a needle is either a hyperechoic line or dot depending on which imaging plane is used (Figs. 26-2 and 26-3). Larger-caliber needles with a larger reflectivity surface are more readily visualized than the smaller-gauge needles. If the needle is not visualized at first because of misalignment, usually, maneuvering the transducer should allow for visualization. The needle and transducer should be in the same plane to produce the best visualization. The ability to see the needle tip will improve the more perpendicular the needle is to the transducer. Needles that are made specifically for sonography-guided procedures are commercially available and are designed to aid in visualization, although any needle used for biopsy should be able to be visualized sonographically if aligned correctly. Experience results in improving both needle alignment and needle visualization.
PROCEDURE
Role of the Sonographer
The sonographer plays an important role in interventional procedures. It is important to be able to locate the pathology of interest and offer a recommendation for the best and safest approach. Interventional sonographers must not only possess basic sonographic knowledge but also be able to optimize images for the detection of subtle masses and utilize features such as color Doppler to find a biopsy path that does not course through a blood vessel. The sonographer must also be familiar with instrumentation technologies to include harmonics and compound imaging and consider transducer selection based on the area of interest, location, footprint size, and transmit frequency. During the procedure, the sonographer makes use of different patient positioning techniques that aid in the best approach and is aware of how breathing affects the movement of the mass. The sonographer is one of the first people the patient interacts with and can reassure the patient with a simple smile and an introduction to the procedure. Building a positive rapport from the beginning is invaluable. The sonographer can coach and support the patient during the procedure to put them at ease and to make the procedure easier for all involved.
Preprocedure
After the patient’s medical record is evaluated for appropriate history, lab values, and other imaging studies, informed consent must be obtained. Written informed consent has a detailed explanation of the major complications and should be discussed in the patient’s native language. The patient should be apprised of the indications and alternatives and be able to understand and cooperate with instructions before and during the procedure.11 After informed consent is obtained, everyone in the procedure room must pause for a time out. A time out allows the staff to verify the correct patient is present and confirm the procedure and procedure site. The sonographer may document the time out on an image (Fig. 26-4). Before, during, and after the procedure, a radiology nurse monitors vital signs by electrocardiogram (ECG) and pulse oximetry.
One of the pitfalls of biopsy involves performing the procedure on the incorrect mass. The best way to avoid this is having the images from the prior exam in the procedure room for immediate and direct comparison. A limited sonography examination must be performed to confirm the results of the prior examination and to determine the best biopsy approach. Depending on the department, the designated interventional ultrasound equipment may be the oldest piece of equipment. If you are not able to reproduce the area of interest on preprocedure imaging, try to use a newer piece of equipment as that should have improved resolution.
Possible approaches will be discussed with the performing physician and an “X” should be placed on the area where the needle will break the skin line (Fig. 26-5). Measuring the distance from the skin to the area of interest will help determine the length of the procedure needle needed (Fig. 26-6). During the procedure, it is preferable for the sonographer to stand on the opposite side of the stretcher than the physician but on the same side as the imaging equipment for ease of use. In the case requiring the sonographer to be positioned on the side opposite the sonography equipment or behind the physician, support staff can be directed to adjust instrumentation controls. It is always important to use optimal scanning ergonomics.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree