, Valery Kornienko2 and Igor Pronin2
(1)
N.N. Blockhin Russian Cancer Research Center, Moscow, Russia
(2)
N.N. Burdenko National Scientific and Practical Center for Neurosurgery, Moscow, Russia
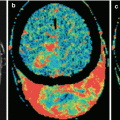
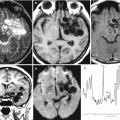
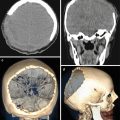
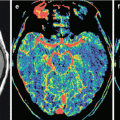
In this chapter, we sought to illustrate the possibilities of the most modern neuroimaging methods and compare their diagnostic capabilities in relation to metastases based on their primary source. Before illustrations in each nosological group, some background information is presented, while manifestations of metastases are described by their primary source. The findings allowed not only to carry out a visual assessment of the size and extent of the pathological process but also to quantify the intensity of biological processes that occur in the tumor tissues and the surrounding brain structures, as well as to evaluate changes induced by the treatment.
Before proceeding to the analysis of materials we have accumulated over 15 years, we would like to define the terminology. Metastasis is a malignant tumor or an inflammatory lesion transferred to any organ or a tissue from another affected organ or tissue. The term “metastasis of the brain” often used in practice erroneously implies a focus of an intact brain tissue in any organ. For example, the concepts of “lung cancer metastases in the brain” or “lung cancer metastases to the brain” appear to be correct.
Changes of the MR signal in different modes, degree, and character of the contrast agent accumulation by the tumor, intensity and extent of edema, hemorrhage into the tumor, and presence of its necrotic changes—all of these affect the selection of study areas and regions in MR spectroscopy, DBU, ASL, SWI (SWAN), and CT perfusion imaging. For example, the proximity of the identified tumor to the bone structures of the skull in CT perfusion forced us to change the projection (from axial to oblique) when selecting the region of interest and exclude the subsequent spectroscopic examination from the diagnostic algorithm when searching for hemorrhagic changes due to an increased “noise” caused by the presence of hemosiderin. When the sizes of MRI contrast agent accumulation areas in the regions of suspected radiation necrosis were small (up to 5 mm), we did not perform CT perfusion or PET.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree