Lipoid Pneumonia
Helen T. Winer-Muram, MD
Key Facts
Terminology
Exogenous lipid pneumonia: Aspiration or inhalation of animal, vegetable, or mineral oils
Imaging Findings
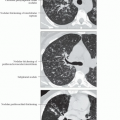
Low CT attenuation areas (-10 and -150 HU) in consolidated lung
Initial: Predominant ground-glass opacities in centrilobular (less aspiration) or panlobular distribution (more aspiration)
1 week: Aspirated segment increases in density to frank consolidation
2-4 weeks: Aspirated segment decreases in density, returns to primarily ground-glass opacities
2-4 months: As ground-glass opacities evolve, fibrosis develops, volume loss (up to 50% of affected segment) common
Fat attenuation 80% (fat not seen in all cases)
Top Differential Diagnoses
Hamartoma
Diaphragmatic Hernias
Pathology
Mineral oil most common agent, common laxative in elderly or children with chronic constipation
Clinical Issues
History important but possibility of lipoid pneumonia usually not considered until after radiographic diagnosis
Diagnostic Checklist
Consider lipoid pneumonia in masses that at 1st glance look like bronchogenic carcinoma
TERMINOLOGY
Abbreviations and Synonyms
Endogenous lipid pneumonia (“golden pneumonia”) and exogenous lipid pneumonia
Definitions
Endogenous lipid pneumonia: Accumulation of lipid containing macrophages secondary to airway obstruction
Exogenous lipid pneumonia: Aspiration or inhalation of animal, vegetable, or mineral oils
IMAGING FINDINGS
General Features
Best diagnostic clue: Low CT attenuation areas (between -10 and -150 Hounsfield units) in consolidated lung
Patient position/location: Exogenous: Gravity-dependent areas and right middle lobe (RML)
CT Findings
Endogenous: Lipid-laden macrophages show no fatty attenuation at CT
Controlled exogenous lipoid aspiration in animal models, sequence of events
Initial: Predominant ground-glass opacities in centrilobular (less aspiration) or panlobular distribution (more aspiration)
HU of attenuated material low (close to attenuation of original material, -150 HU)
1 week: Aspirated segment increases in density to frank consolidation
HU of affected segment increases (may be all water density)
2-4 weeks: Aspirated segment decreases in density, returns to primarily ground-glass opacities
“Crazy-paving” pattern evolves during this time (due to macrophage and inflammatory cell migration to interstitial lymphatics)
HU of attenuated segment again decreases
Ground-glass opacities may completely resolve, leaving smooth interlobular septal thickening
2-4 months: As ground-glass opacities evolve, fibrosis develops, volume loss (up to 50% of affected segment) common
Volume loss signs include vascular crowding, traction bronchiectasis, fissural displacement
Clinical cases will mirror this experimental sequence of events
Consolidation most common finding (90%)
Fat attenuation (80%) (fat not seen in all cases)
Ground-glass opacities (50%)
“Crazy-paving” pattern (33%)
Irregular-shaped mass (66%)
Acute vs. chronic aspiration, findings often overlap
Small effusions common in acute (50%), not seen with chronic
Masses more common in chronic (66%), not seen with acute aspiration
Signs of volume loss more common in chronic (80%) vs. acute (25%)
Fat attenuation
Seen with both acute and chronic lipoid aspiration
Acute may have larger volume of low attenuation material
Fat may shift to dependent lung with postural change
Chronic mass-like areas of aspiration often have smaller (< 10% total volume) foci of fat attenuation
15-20% will not have fat attenuation
Percentage may actually be smaller with routine use of MDCT and thin-collimation
Partial volume artifact of abnormal lung admixed with air may give false-positive fat attenuation
Distribution
Gravity dependent: Posterior segments of upper lobes and superior segments of lower lobes in supine position, basilar segments in upright position
Right middle lobe also common for unknown reason
Resolution
Acute aspiration usually improves (80%) but rarely clears completely
Chronic aspiration usually stable and indolent over time
Complications
Superinfection with atypical mycobacteria (usually M. fortuitum)
Suspect if have cavitated nodules
Occasional reports of bronchogenic carcinoma developing in chronic aspiration
Suspect if mass enlarging or cavitation
Fire-eater’s pneumonia
Unique form of lipoid pneumonia due to aspiration of paraffin hydrocarbons used to fuel fire
Aspiration results in acute lipoid pneumonia
Besides fat attenuation in lung, often develop pneumatoceles
Radiographic Findings
Radiography
Radiographic appearance nonspecific, either consolidation or interstitial opacities
Prominent mass leads to workup for presumptive diagnosis of bronchogenic carcinoma
MR Findings
May show fat: High T1 and T2 signal or demonstrate chemical shift on in-out phase T1-weighted imaging
Hemorrhage (if acute animal fat ingestion) will also be high at T1- and T2-weighted imaging
Imaging Recommendations
Best imaging tool
CT is best imaging tool to characterize lesions for presence of fatty component
Unknown whether MR more sensitive for fat
Nuclear Medicine Findings
PET: Chronic mass lesions often PET positive, mistaken as bronchogenic carcinoma if fat not specifically looked for at CT
DIFFERENTIAL DIAGNOSIS
Other Intrathoracic Lesions Containing Fat
Hamartoma
Diaphragmatic Hernias
Lipoma, Chest Wall
Mediastinal Lipomatosis
Thymolipoma
Germ Cell Tumors
Extramedullary Hematopoiesis
Liposarcoma
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree