Standard views: AP, PA with 25° caudal angulation (Ferguson) of the pelvis
Frequent types of fractures:
Isolated fractures of the pubic rami
Pelvic ring disruption
Fractures of the pelvis are usually caused by direct injury or by force transmitted longitudinally through the femur. There are two major groups of pelvic fractures: isolated fractures and pelvic ring disruption.
Any part of the pelvis may be affected by an isolated fracture. The commonest one is through the pubic ramus (superior, inferior, or both). Isolated fractures can also be seen involving the iliac wing (Duverney), sacrum, anterior inferior iliac spine (rectus femoris avulsion), anterior superior iliac spine (sartorius avulsion), and ischial tuberosity (hamstring avulsion) (Fig. 21.1).
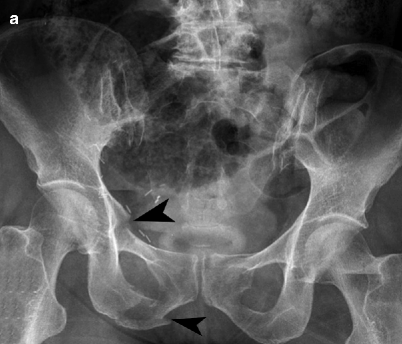
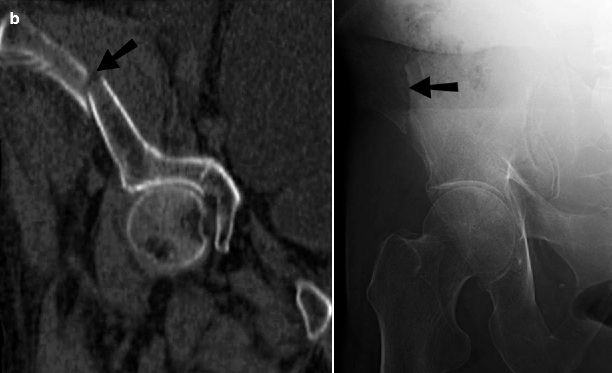


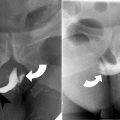
Fig. 21.1
Pelvic fracture. (a) An AP radiograph of the pelvis shows displaced vertically oriented fractures (arrowheads) of the right superior and inferior pubic rami and widening of the right sacroiliac joint, representing an anteroposterior compression (APC) type of pelvic ring disruption. (b) A focused AP radiographic view and corresponding CT image of the right iliac wing show an isolated fracture of the right iliac wing (arrows), which is considered a stable pelvic injury
Pelvic ring disruption refers to osseous or joint disruption at two points of the pelvic ring (sacrum and two innominate bones) approximately opposite to one another. The anterior injury often involves either a fracture through both pubic rami or pubic symphysis diastasis. The posterior injury is usually a subluxation of the sacroiliac joint or a fracture through the ilium or sacral ala. The most widely used classification of pelvic ring disruption is the Young-Burgess system and describes four patterns, according to the direction of forces to the pelvis [1]:
1.
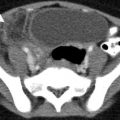
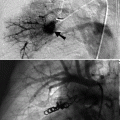
Anteroposterior compression: Vertically oriented fractures of the pubic rami, pubic symphysis diastasis, and disruption of the sacroiliac joints. They may be associated with urethral and urinary bladder rupture (Fig. 21.2).
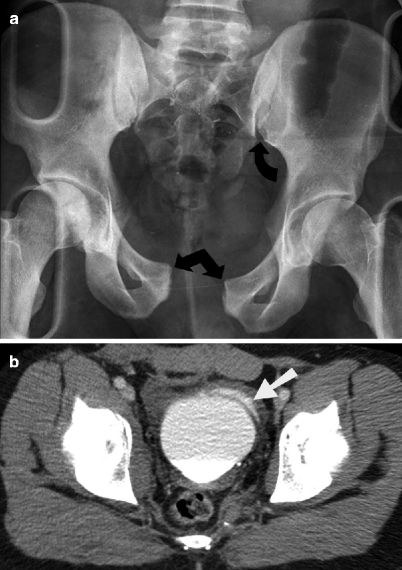

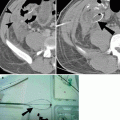
Fig. 21.2
Pelvic fracture. (a) An AP radiograph of the pelvis shows widening of the pubic symphysis (double arrow) and the left sacroiliac joint (arrow), indicative of an anteroposterior compression (APC) type of pelvic ring disruption. (b) An axial CT cystography image reveals an extraperitoneal bladder rupture (arrow)
2.
Lateral compression: It produces coronal or horizontal fractures of the pubic rami, sacral compression fracture, iliac wing fracture, and central hip dislocation.
3.
Vertical shear: It results in vertically oriented fractures of the pubic rami, sacrum, and iliac wings. There is extensive ligamentous disruption, often resulting in severe pelvic instability, sciatic nerve, and pelvic vascular injury.
4.
Combined mechanism.
In general, a single break in the pelvic ring is considered stable, while two or more breaks of the pelvic ring are unstable. Most sacral fractures are vertically oriented and are associated with fractures of the pelvis or lumbosacral dislocation.
Denis classification: It divides sacrum into three zones [2]:
Zone I fractures: They are located lateral to the sacral foramina and rarely cause neurological deficit.
Zone II fractures: These fractures are usually vertically oriented (Figs. 21.3a, b). They pass through sacral foramina and are often associated with L5 nerve root injury.
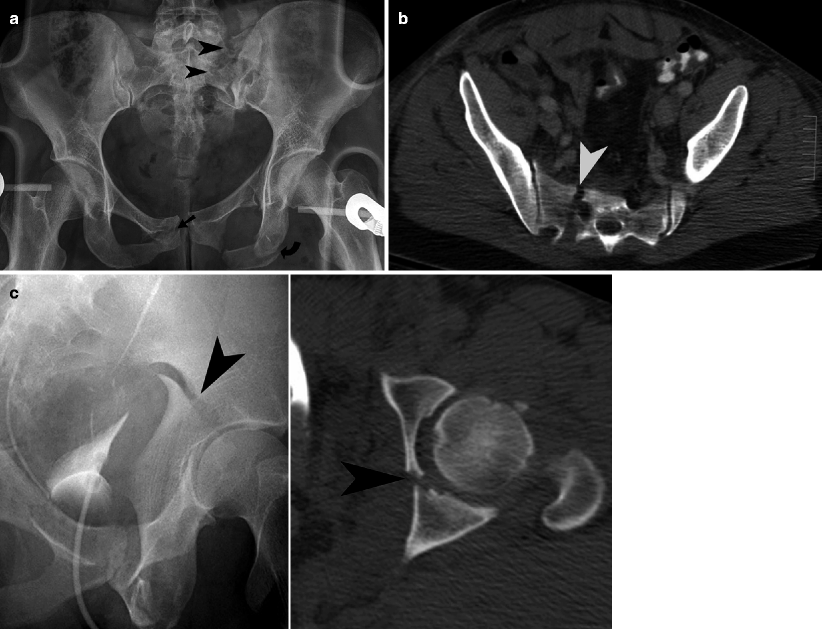
Fig. 21.3
Pelvic fractures. (a) An AP radiograph of the pelvis shows a vertical fracture through the left sacral ala (arrowheads), widening of the left sacroiliac joint, multiple bilateral pubic rami fractures (straight and curved arrow). (b) An axial CT image of another patient shows a zone II right sacral fracture (arrowhead). (c) An iliac oblique Judet view of the left hip demonstrates a disrupted ilioischial line by a displaced posterior column fracture (arrowhead). An accompanying axial CT image confirms the finding of a column fracture, which is seen as a coronally oriented fracture line (arrowhead) through the posterior half of the acetabulum
Zone III fractures: These fractures involve the central canal and have the highest frequency of neurological deficit.
Acetabulum
Standard views: AP and Judet views of the hip (two oblique views centered on the hip, tilted 45° medially or laterally from a true AP direction) |
Frequent types of fractures: |
Posterior wall |
Transverse |
Transverse plus posterior wall |
T-shaped |
Associated both column |
Imaging performed in acetabular fracture is to evaluate for wall involvement, intra-articular entrapped bone fragment and associated femoral head fracture. On the AP view of the hip, six lines relating to the acetabulum and surrounding structures have been described: iliopubic or iliopectineal line, ilioischial line, radiographic teardrop, roof of the acetabulum, anterior rim of the acetabulum, and posterior rim of the acetabulum. Disruption of any of these normal lines indicates the possible presence of abnormality [3] (Fig. 21.3c).
1.
Iliopectineal line: It extends from the sciatic notch to pubic tubercle and is discontinuous in anterior column fractures.
2.
Ilioischial line: It is drawn from the sciatic notch to internal cortex of the ischium and is discontinuous with posterior column fracture. The breaks in the anterior and posterior rim of the acetabulum indicate either a column or wall fracture. The radiographic teardrop is a composite U-shaped shadow at the anteroinferior portion of the acetabular fossa, without true structural correlate.
On lateral view, the pelvis is divided into anterior and posterior columns. The anterior column (iliopubic component) consists of pubis and ilium, whereas the posterior column (ischial component) consists of ischium, ischial spine, and ischial tuberosity. The posterior wall fractures are the most common acetabular fractures and are often associated with multiple fragments as well as posterior hip dislocation.
Hip
Standard views: AP and true lateral views of the hip |
Frequent sites of fractures: |
Femoral neck fractures |
Posterior hip dislocations |
Frequently missed injuries: |
Nondisplaced femoral neck fractures |
Fractures of the greater trochanter |
Fractures of the femoral head |
Hip Dislocations
Dislocations of the hip are infrequent injuries since strong force is required to produce such trauma. There are several types of hip dislocations, which are defined by the relationship of the femoral head relative to the acetabulum.
Posterior dislocation, which is the most common type of hip dislocation, is characterized by posterior displacement of femoral head in relation to the acetabulum (Fig. 21.4). It is classically the result of a head-on motor vehicle collision, in which the occupant’s knees strike the dashboard, while the knees are in flexed position. It commonly occurs in association with fractures of the posterior acetabular rim. On radiography, there is a lack of congruency of the femoral head and the acetabular fossa with the femoral head located superolateral to the acetabulum. In approximately half of cases, there is associated fracture of the posterior acetabular rim. Common complications of posterior hip dislocation are injury to the sciatic nerve, femoral head fracture, avascular necrosis of the femoral head, posttraumatic ossification, and osteoarthritis.
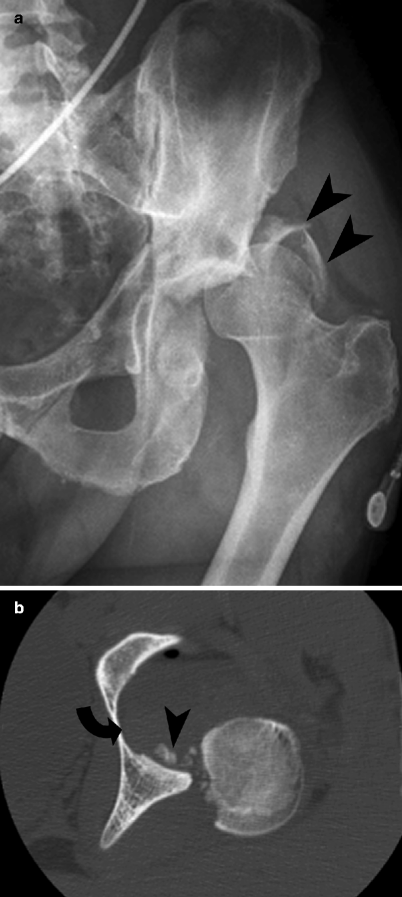

Fig. 21.4
Posterior dislocation at the hip joint. (a) An AP radiograph of the pelvis shows an apparent superolateral location of the left femoral head relative to the acetabulum, which is characteristic of posterior hip dislocation. Arrowheads point to associated acetabular fracture fragments. (b) An axial CT image shows an empty left acetabulum (arrow) with several bone fragments (arrowhead) in the hip joint from associated posterior wall acetabular fracture
Anterior hip dislocation is the second most common type of hip dislocation, accounting for 10–15 % of all hip dislocations. It is caused by forced abduction and lateral rotation of the limb, usually from motor vehicle collision. On radiography, the femoral head is often located inferomedial to the acetabulum. The dislocated femoral head appears slightly larger than on the contralateral side because of magnification (dislocated femoral head is located further away from the cassette) and the lesser trochanter is visualized in full profile. There is association with femoral head and acetabular fracture [4].
Central hip dislocation describes the medial displacement of the femoral head into the pelvis, causing comminuted fracture of the medial wall of the acetabulum. It is usually caused by a heavy lateral blow upon the femur, for example, fall from height onto the side. Retroperitoneal bleeding, subsequent retroperitoneal infection, and residual joint incongruity frequently complicate this injury.
Postreduction radiograph is required to determine the adequacy of reduction and to identify potential intra-articular fragments. Asymmetry of hip joint space or unequal widths between the radiographic teardrop and femoral head should raise suspicion of large effusion, interposed soft tissue, or intra-articular fragments. CT is the imaging method of choice to evaluate for intra-articular loose body.
Fractures of the Proximal Femur
Fractures of the femoral head are relatively infrequent in isolation given the protection of the femoral head by the acetabulum (Figs. 21.4b and 21.5a). When they occur, they are usually associated with hip dislocation and are caused by impaction or shearing by the acetabulum. Pipkin classification is the standard mean to classify femoral head fractures, with a main criterion of whether the fracture is above or below the fovea [5].
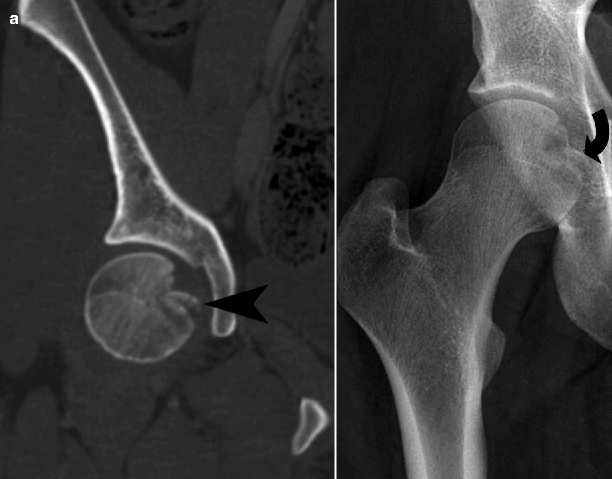
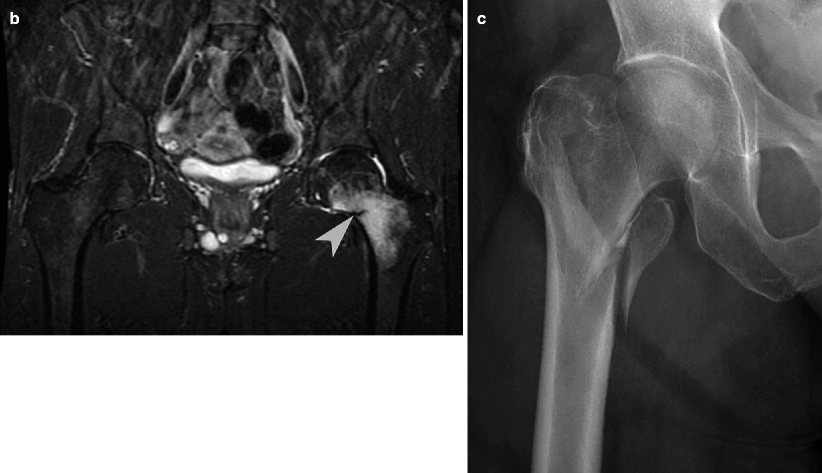


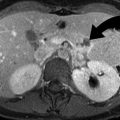
Fig. 21.5
Proximal femoral fractures. (a) An AP radiograph of the right hip reveals a depression at the femoral head (arrow), later confirmed by a corresponding CT scan as a depressed fracture (arrowhead) involving the fovea capitis. (b) A coronal STIR MR image of the pelvis in another patient demonstrates bone marrow edema of the left femoral neck with a linear hypointense line (arrowhead) in the medial aspect of the femoral neck, perpendicular to the bony cortex, representing a stress fracture. (c) An AP radiograph of the right hip of another patient shows an intertrochanteric fracture with a displaced lesser trochanter fragment
Pipkin Classification:
Type 1 is a fracture below the fovea.
Type 2 is the fracture above the fovea.
Type 3 is a femoral head fracture associated with a neck fracture.
Type 4 is a femoral head fracture associated with an acetabular fracture.
Type 3 and 4 fractures often require operative intervention, while the need for operative fixation of type 1 and 2 fractures depends on several factors including intra-articular fragment, irreducible dislocation, and involvement of the weight-bearing portion. The fractures of the femoral head are at an increased risk of avascular necrosis or nonunion because main arterial supply (medial femoral circumflex artery) may be injured.
Femoral neck fractures may result from a significant injury such as a fall but can also be seen in minor trauma among osteoporotic individuals. Garden classification is most commonly used to describe these fractures [6].
Garden I is an incomplete or impacted fracture, in which the inferior aspect of the neck trabeculae is still intact. It commonly results in a slight valgus angulation of the femoral neck.
Garden II is a complete fracture without displacement (Fig. 21.5b).
Garden III is a complete fracture with partial displacement. Shortening and external rotation of the affected limb is commonly seen.
Garden IV is a complete fracture with total displacement (no continuity between the proximal and distal fragments).
While displaced fractures are readily visualized on radiography, imaging features of nondisplaced fractures are often subtle. These features include:
1.
Disruption of a normal S or reversed S curve of the outline of the femoral head joining the concave outline of the femoral neck.
2.
Sclerotic line of impacted fracture.
3.
Abnormal angulation of the major trabeculae groups. On a lateral radiograph, one should look for posterior comminution of the fracture, since its presence indicates a higher chance of nonunion.
The blood supply to the femoral head is through three routes, including the vessels in the ligamentum teres, capsular vessels, and branches of the nutrient vessels. There is an increased risk of avascular necrosis following femoral neck fractures because of nutrient and capsular vessel disruption. The frequency of avascular necrosis in displaced and nondisplaced fractures is 30–40 and 10 %, respectively [7]. If radiography is negative but there is still a high clinical suspicion, CT with multiplanar reconstruction or MRI should be considered.
Intertrochanteric fractures occur along the line between greater and lesser trochanter (Fig. 21.5c). Since the joint capsule attaches anteriorly to the intertrochanteric line and posteriorly to the medial half of the femoral neck, trochanteric fracture is theoretically extracapsular and heals well relative to the femoral neck fractures. It is important to distinguish stable from unstable trochanteric fractures. This can be determined by assessing the medial cortex and comminution of the posterior cortex (on lateral view). Comminuted fracture line at the medial cortex, displaced lesser trochanter fracture, and lesser trochanter fragment containing calcar femorale are generally considered unstable. Presence of a fracture gap medially and posteriorly will allow fracture displacement into varus or retroversion, causing instability. Unlike fractures of the femoral neck, trochanteric fractures are almost free from serious complications.
Subtrochanteric fractures are fractures located between the lesser trochanter and 5 cm below. It is usually a result of direct trauma and may occur in isolation or with intertrochanteric fractures. The fractures are usually displaced by muscle pulls, resulting in shortening and varus deformity.
Fractures of the Femoral Shaft, Supracondyle, and Condyle
Fractures of the distal femur usually occur with high-velocity trauma in young adults and low-energy trauma in osteoporotic bone of elderly persons. Therefore, it is commonly associated with several other injuries such as fractures of the patella, hip and tibial shaft, and ligamentous disruptions of the knee. Femoral shaft fractures occur at any age and are equally common in the uppermost, middle, and lower thirds of the shaft. Their pattern may be transverse, oblique, spiral, comminuted, or greenstick. Radiographic evaluation must include the hip and knee joints since joint dislocations may coexist.
The fractures of the supracondylar and condylar regions are divided into three types: extra-articular (transverse), partial articular, and complete articular. The key components in dividing distal femoral fractures are presence of (1) a fracture line extending into the intercondylar notch (intercondylar split), (2) osteochondral fragments in the area of or between the intercondylar split, and (3) coronal-plane (Hoffa) fracture. Partial articular fractures are an intra-articular fracture that involves either the medial, lateral condyle, or in a coronal plane (best seen on a lateral radiograph). Complete articular fractures produce separate articular and metaphyseal segments, in which each can be simple or multifragmentary.
Osteochondritis dissecans (OCD) of the knee (Fig. 21.6) may present in a similar fashion to acute traumatic osteochondral fractures, although they differ. The condition is characterized by sequential degeneration or aseptic necrosis and recalcification. It can occur in persons of any age group but is most frequent between 10 and 20 years old, with male predominance. Most of the cases (85 %) involve the medial femoral condyle in the posterolateral aspect [8]. Radiography shows OCD as a well-circumscribed crescent-shaped area of radiolucency above the subchondral bone, separated from femoral condyle. MRI is helpful to help determining the vascularity of the lesion, bilaterality, occult lesions, and degree of loosening of the lesion.
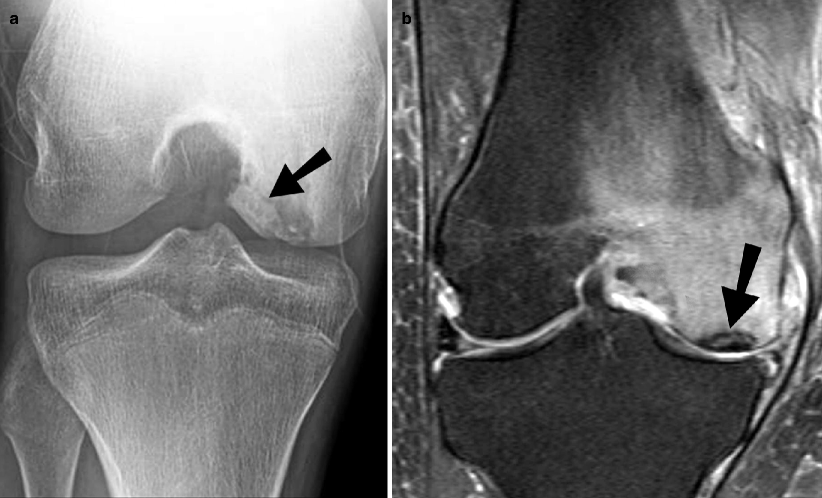

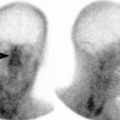
Fig. 21.6
Osteochondral injury. (a) A tunnel radiographic view of the right knee shows an osteochondral fracture (arrow) of the lateral aspect of the medial femoral condyle. (b) A coronal fat-suppressed T2W MR image of the right knee in a different patient reveals bone marrow edema of the medial femoral condyle with an osteochondral fragment in the subarticular portion (arrow). There is soft tissue edema in the medial aspect of the knee. The medial collateral ligament is intact
Knee
Standard views: AP, lateral, both obliques (optional patellar sunrise if suspicious for patellar injuries)
Stay updated, free articles. Join our Telegram channel
Full access? Get Clinical Tree
 Get Clinical Tree app for offline access
Get Clinical Tree app for offline access

|