Magnetic resonance imaging of the midfoot and forefoot are increasingly requested examinations for a variety of symptoms. This region has its own particular anatomic variants, which the interpreting radiologist needs to be aware of, including accessory ossicles, sesamoid variants, and tarsal coalitions. In addition, certain pulse sequences used in this region are predisposed to artifact, which may lead to false-positive findings. These topics are discussed in this content in addition to the inclusion of pointers to help avoid pitfalls in interpretation of common diseases.
For the purposes of this discussion the midfoot is defined as that region of the foot between the Chopart joint (talonavicular and calcaeocuboid articulations) and the Lisfranc (tarsometatarsal) joints. The forefoot is defined as that part of the foot distal to the Lisfranc joints. Structures usually seen in their entirety on magnetic resonance (MR) ankle studies, such as the posterior tibialis tendon, are not discussed.
Technique
It is important to tailor each MR examination for the specific clinical question and whenever possible to avoid performing a large field of view study that includes both the midfoot and forefoot, as this may result in an unwanted reduction in spatial resolution. The placement of localizing markers by technologists (eg, vitamin E markers) at the symptomatic site should be encouraged, but should be placed on the dorsal aspect of the foot to avoid unwanted artifact.
As with any MR imaging protocol it is usually prudent to perform the most important sequences first, in case the study is terminated prematurely. The most important sequence is usually a fluid sensitive sequence such as a coronal (short axis of foot) fat-saturated T2 spin echo sequence.
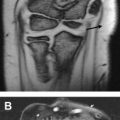
Care must be taken with interpretation of abnormalities on certain sequences. For example, on a T1 spin echo sequence, the signal within tendons may be high as a result of magic angle effect ( Fig. 1 ) and so be misinterpreted as tendinosis or tear. This pitfall may be avoided by looking at the fluid sensitive sequence performed in the same plane, which shows no increased signal. This phenomenon occurs when tendon or ligament fibers are oriented at 55° to the main magnetic field when using sequences that use a low echo time (TE) (T1 and proton density).
Midfoot
MR of the midfoot is often included in MR of the ankle. If a study is performed specifically for a lesion at the midfoot, the same imaging planes as the ankle are appropriate, including sagittal short tau inversion recovery (STIR) and T1 spin echo, axial (long axis of foot) proton density and fat-saturated T2, and a coronal (short axis of foot) fat-saturated T2. Coronal (short axis of foot) T1 spin echo may also be of value for assessment of osseous abnormalities.
Forefoot
Forefoot MR protocols should include distal tarsal level through to the distal phalanges. A suggested protocol includes sagittal STIR, T1 spin echo, short-axis T2 fat-saturated and T1 spin echo T1, and long-axis T2 fat-saturated sequences.
Coalitions
Talocalcaneal, calcaneonavicular, talonavicular, and calcaneocuboid coalitions involve at least part of the hindfoot, are readily identified on MR of the ankle, and therefore are not considered in this discussion. Isolated midfoot coalitions usually involve the cuneiforms but are uncommon.
Ossicles and multipartite bones
There are a multitude of potential accessory ossicles and sesamoids in the midfoot and forefoot. A complete analysis of each is beyond the scope of this discussion. Nevertheless, some of these ossicles and sesamoids occur frequently and have potential clinical significance.
Accessory or bipartite navicular bones and os peroneii are usually best evaluated on MR of the ankle.
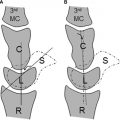
An os intermetatarseum is seen in 1% to 10% of the population. It is located dorsally between the medial cuneiform and the base of the first and second metatarsals ( Fig. 2 ). It may exist separate from the adjacent bones, articulate with these bones, or fuse with them. Its exact cause is unclear. A true os intermetatarseum can sometimes be symptomatic with associated bone marrow and soft tissue edema. A potential pitfall is confusing this entity with an avulsion fracture of the second metatarsal base, which occurs in Lisfranc fractures and dislocations.
This pitfall can be avoided by identifying the dorsally positioned os intermetatarseum and lack of injury to the Lisfranc ligaments (see section on Lisfranc injury and Fig. 3 ).
An os supranaviculare has a prevalence of approximately 1% and is located at the dorsal aspect of the talonavicular joint closer to the navicular bone than a similar appearing os supratalare (located anterosuperior to the talar head). It may cause symptoms itself but can sometimes be confused with a cortical avulsion of the talar head or navicular bone.
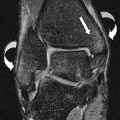
Bipartite bones are occasionally identified at the midfoot, most frequently involving the medial cuneiform ( Fig. 4 ). The incidence of this variant is quoted as between 0.3% and 2.4% in the literature. The plantar element is usually larger than the dorsal. Knowledge of this entity is important to avoid confusion with fracture of the cuneiform. A pseudoarticulation often intervenes between the 2 elements, which may be a cause for symptoms with degenerative arthropathy, allowing abnormal motion across the joint or sometimes manifesting as fracture through the synchondrosis. Features helpful in differentiating between bipartite anatomy and fracture include the bipartite medial cuneiform showing smooth, well-corticated margins and the 2 portions of the bipartite cuneiforms together appearing larger than expected for one normal bone.
Hallux sesamoids
Although sesamoid bones may be seen at other metatarsophalangeal (MTP) joints they are invariably present at the first MTP joint.
The hallux sesamoids (tibial and fibular sesamoids) are an integral part of normal biomechanics of the first MTP joint, assisting in the distribution of forces on flexion of the hallux during walking. They are therefore prone to acute and chronic trauma, leading to a variety of pathologic conditions, including stress response, fracture, degenerative arthropathy at the metatarsosesamoid (MTS) articulation and osteonecrosis. However, there is considerable variation in the size, shape, and number of bones at this site, which may act as confounders in the interpretation of suspected sesamoid abnormality.
Overall the frequency of multiple sesamoids at the first MTP joint has been quoted in the literature as ranging from 2.7% to 33.5% ; the presence of a tibial being sesamoid is more common than a fibular. The possibility of bipartite or multipartite morphology at the sesamoids with stress response and/or pseudoarthrosis may present a diagnostic challenge in the setting of suspected fracture, although some features can be used to help differentiate the 2 entities.
Sesamoid fractures usually manifest as a sharp well-demarcated line between the bone fragments, with fluid signal often intervening between. The fragments also usually have the appearance of having once fitted together like a jigsaw puzzle. Bone edema in both fragments at the fracture site and surrounding soft tissue edema are invariably present.
In contrast, bipartite sesamoids with stress response have more rounded sclerotic low T1 signal margins at the interface between the 2 bones, and the 2 bone fragments when added together are larger than the other sesamoid. With stress response, edema of the sesamoids and periosseous soft tissue are usually not helpful differentiating factors. Fluid signal (high on T2) between the 2 bone fragments may be seen in both pseudoarthrosis and fracture. Clinical history may also be of value in determining the acuteness of symptoms. If any previous imaging is available, this may also be of value in establishing a baseline for comparison.
When disease at the sesamoids is suspected a small field of view centered at this site with sequences in multiple planes is often helpful. In some circumstances a definitive diagnosis may not be possible initially and correlation with computed tomography for more definitive assessment of a discrete fracture line or follow-up imaging may be needed ( Figs. 5–7 ).