Localization: Tibia and femur. Less frequent in the humerus, rare in the fibula and other long bones. Usually located in the diaphysis, occasionally in the metaphysis.
Clinical: Palpable mass and moderate pain. Slower growth rate than in usual OS.
Imaging: Periosteal, fusiform, radiolucent mass, with well-defined borders. It usually contains spiculated radiodensities perpendicular to the cortex that is either intact or superficially eroded, sometimes with a Codman triangle. Typically, the medullary canal is uninvolved. This is better demonstrated by CT and MRI.
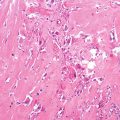
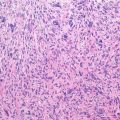
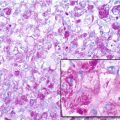
Histopathology: The cut surface of the tumor is soft to rubbery with a translucent aura. The tumor forms large lobules, separated by streaks of ossification perpendicular to the cortex. Tissue is mainly chondroblastic, being more cellular at the periphery, with spindle cells and lacelike osteoid, more chondroid at the center of the lobuli. Lacelike osteoid among malignant osteoblasts is present and defines this tumor as OS. Histological grade of malignancy is 1–3. At the bony interface, the tumor can permeate for a small thickness into the cortex.
Course and Staging: It generally grows slower than usual OS, but much less slow than parosteal OS. The stage is I-A or I-B if there is intramedullary involvement.
Treatment and Prognosis: Due to the rather typical imaging presentation, frozen section intraoperative biopsy is usually adequate. Treatment consists of en bloc resection with wide margins. Mets (lung) have been observed in about 15 % of cases. Therefore, prognosis is good, after wide surgery and without chemotherapy.
Key Points
Clinical | Young age, mild symptoms |
Radiological | Surface lesion, diaphyseal with radio opacities
Stay updated, free articles. Join our Telegram channel
Full access? Get Clinical Tree
 Get Clinical Tree app for offline access
Get Clinical Tree app for offline access

|