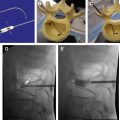
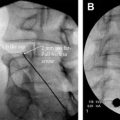
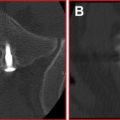
As image-guided (nonvascular) spine interventions have become progressively more common in the interventional radiologic community, there is a growing need for physician expertise regarding the materials and pharmaceuticals that are used for these procedures. This article is intended to provide information to address these needs.
Corticosteroids
Corticosteroids have a long history in the treatment of pain related to spine disease, having been used since the 1960s. They were originally injected epidurally and intrathecally for pain management. By the 1980s, there were reports of complications that included arachnoiditis, meningitis, and paraparesis/paraplegia. Controversy was sufficient in Australia that an explicit government warning was issued about the use of corticosteroids for epidural pain management. Review of the scientific literature regarding these findings revealed that many of the complications resulted from the intrathecal use of corticosteroids. It is now known that definite side effects can result from these drugs, and physicians should be aware of these side effects and include potential complications in their explanations to their patients.
Corticosteroids are believed to produce chemical stabilization of the local environment, which can produce pain relief by reducing the local amount of phospholipase A2 and arachidonic acid, as well as decreasing the cell-mediated inflammatory and immunologic responses. The usual dosages of various steroids for epidural steroid injections are given in Table 1 . Dose equivalents are given in Table 2 .
| Steroid | Dose (mg) |
|---|---|
| Depo-Medrol | 40–80 |
| Kenalog | 40–80 |
| Celestone | 6–12 |
| Dexamethasone | 6–12 |
| Drug | Equivalent Dose (mg) |
|---|---|
| Cortisone | 30 |
| Hydrocortisone | 25 |
| Prednisone | 6 |
| Prednisolone | 6 |
| Methylprednisolone | 5 |
| Triamcinolone | 5 |
| Dexamethasone | 1 |
| Betamethasone | 1 |
The most common corticosteroid used for spine injections has been a long-acting form of methylprednisolone acetate (Depo-Medrol, Pharmacia-Upjohn, Chesterfield, MO, USA). This drug is available in 40- and 80- mg/mL doses. The acetate formulation is quite insoluble in water and has a long half-life in tissues. It has a relative strength of approximately 5 times that of hydrocortisone and often contains the preservative polyethylene glycol, which is thought to be potentially neurotoxic. Indeed, this material may be the cause of arachnoiditis if given into the intrathecal space. Depo-Medrol is a particulate mixture and can create stroke if injected intra-arterially (ie, into a radicular spinal artery during an attempted cervical foraminal injection). The particulate nature is increased by adding anesthetic solutions, as the combination increases precipitation within the syringe. Mixing Depo-Medrol with anesthetic in the same syringe is contraindicated on the package insert.
Another option for an injectable corticosteroid is the combination of betamethasone sodium phosphate and betamethasone acetate (Celestone Soluspan, Schering, Kentworth, NJ, USA). This combines a short- and long-acting form of betamethasone in the same injectable solution. It contains no preservative and comes in 6mg/mL doses. Betamethasone has approximately 30 times the strength of hydrocortisone. It seems to have a lesser particulate nature and a decreased tendency to precipitate when mixed with anesthetics. All of these properties make it less apt to create arachnoiditis when injected intrathecally. Because there were periods when the availability of Depo-Medrol and Celestone was decreased, some labs used a long-acting form of triamcinolone (Kenalog, Bristol-Myers Squibb, New York, NY, USA). This material is also particulate (similar to Depo-Medrol) and contains the preservative polyethylene glycol. It is available in a 40-mg/mL dosage and has approximately 5 times the strength of hydrocortisone. It seems to be equivalent to Depo-Medrol with no discernable advantages and is recommended in the same dosage as Depo-Medrol (80 mg).
The stroke potential of each of these corticosteroids is related to their particulate nature. With Depo-Medrol and Kenalog, the particulate nature is made worse by mixing with anesthetic in the injection syringe. This seems to be a smaller problem with Celestone. However, all 3 are particulate and may produce stroke if injected intra-arterially.
Dexamethasone sodium phosphate has been substituted for the above-mentioned corticosteroids with the intent of avoiding the potential for stroke (with inadvertent intra-arterial injection). It is approved for intravenous injection but not for intra-arterial injection. Dexamethasone also contains a preservative (benzyl alcohol),which makes it particulate. Derby and colleagues found that particles of dexamethasone are approximately one-tenth the size of a red blood cell and did not aggregate when mixed with lidocaine. There is no direct proof that using dexamethasone instead of other corticosteroids prevents stroke, although it does seem to give an additional margin of safety with respect to particle size and aggregation.
Anesthetic agents
Local anesthetic agents are commonly added as part of the injectate used for numerous spinal and pain management injection procedures. Local anesthetics are sodium channel–blocking drugs that can halt electrical impulse conduction in peripheral nerves, spinal roots, and autonomic ganglia. To block nerve conduction, the local anesthetic must cover at least 3 consecutive sodium channels (nodes of Ranvier) ( Fig. 1 ). Binding to the sodium channel interrupts nerve impulse transmission. The binding is reversible (reversibility varying with the length of action of each anesthetic). Differential blocking occurs because fibers carrying different types of information (pain, sensory, motor) are of different sizes. The smallest of these are the nociceptive (pain) fibers. These fibers experience calcium channel blockade with the smallest amount of anesthetic because a physically small amount of material spreads sufficiently far enough to cover 3 small sodium channel (nociceptive) receptors, whereas that amount may not adequately cover 3 larger receptors (sensory or motor). Progressively larger fibers require a larger volume of anesthetic to produce coverage that will block enough adjacent channels to stop conduction. This means that pain fibers are the most sensitive, followed by sensory fibers and then motor fibers, allowing the potential for pain relief without obligatory motor blockade.
Local anesthetics are organic amines, with an intermediary ester or amide linkage separating the lipophilic ringed head from the hydrophilic hydrocarbon tail. The amino-ester group of anesthetics includes members such as procaine, tetracaine, and benzocaine. These anesthetics have been used for a long time and are known to have a higher allergic potential than the amide-linked group of anesthetics (lidocaine, bupivacaine, and ropivacaine) now in common usage. The amino-ester group of anesthetics is thought to have allergic potential because of the metabolite para-aminobenzoic acid (PABA). The amide group of anesthetics does not have this metabolite and is known to have a very low allergic potential and little cross-reactivity. However, the amide group may contain the preservative methylparaben. This compound is metabolized to PABA and can produce cross-reactivity for potential allergic reactions with the ester group of anesthetics. Preservative-free amide anesthetics are therefore recommended for all injection procedures.
Lidocaine represented a common first-generation member of the amide anesthetic group. It is considered to be safe except in large quantities that generally exceeded 500 mg. It has a relatively short duration of action usually lasting only several hours. Bupivacaine is a second-generation amide anesthetic that has a prolonged duration of action. It is, however, associated with cardiac and neurotoxic reactions and has a maximum recommended safe dose of 150 mg. Because of the poorer cardiac profile of bupivacaine that resulted from long-term sodium channel blockade in heart muscle, third-generation amide anesthetics were developed. Ropivacaine is a member of this group and produces local anesthesia for a longer period like bupivacaine but with a better cardiac profile. Injections of local anesthetic in percutaneous spine interventions are small enough that one should generally never approach the maximum allowable dosages.
Bupivacaine and ropivacaine come in different concentrations (0.25%, 0.5%, and 0.75% and 0.2% and 0.5%, respectively). The lower dosages are useful for pain relief in epidural and nerve blockage injections. The more-concentrated dosages produce motor blockade, which is an unwanted side effect with these procedures. The amounts of these drugs used in outpatient, percutaneous procedures are small compared with that needed to produce cardiac or neurotoxic effects.
Anesthetic agents
Local anesthetic agents are commonly added as part of the injectate used for numerous spinal and pain management injection procedures. Local anesthetics are sodium channel–blocking drugs that can halt electrical impulse conduction in peripheral nerves, spinal roots, and autonomic ganglia. To block nerve conduction, the local anesthetic must cover at least 3 consecutive sodium channels (nodes of Ranvier) ( Fig. 1 ). Binding to the sodium channel interrupts nerve impulse transmission. The binding is reversible (reversibility varying with the length of action of each anesthetic). Differential blocking occurs because fibers carrying different types of information (pain, sensory, motor) are of different sizes. The smallest of these are the nociceptive (pain) fibers. These fibers experience calcium channel blockade with the smallest amount of anesthetic because a physically small amount of material spreads sufficiently far enough to cover 3 small sodium channel (nociceptive) receptors, whereas that amount may not adequately cover 3 larger receptors (sensory or motor). Progressively larger fibers require a larger volume of anesthetic to produce coverage that will block enough adjacent channels to stop conduction. This means that pain fibers are the most sensitive, followed by sensory fibers and then motor fibers, allowing the potential for pain relief without obligatory motor blockade.
Local anesthetics are organic amines, with an intermediary ester or amide linkage separating the lipophilic ringed head from the hydrophilic hydrocarbon tail. The amino-ester group of anesthetics includes members such as procaine, tetracaine, and benzocaine. These anesthetics have been used for a long time and are known to have a higher allergic potential than the amide-linked group of anesthetics (lidocaine, bupivacaine, and ropivacaine) now in common usage. The amino-ester group of anesthetics is thought to have allergic potential because of the metabolite para-aminobenzoic acid (PABA). The amide group of anesthetics does not have this metabolite and is known to have a very low allergic potential and little cross-reactivity. However, the amide group may contain the preservative methylparaben. This compound is metabolized to PABA and can produce cross-reactivity for potential allergic reactions with the ester group of anesthetics. Preservative-free amide anesthetics are therefore recommended for all injection procedures.
Lidocaine represented a common first-generation member of the amide anesthetic group. It is considered to be safe except in large quantities that generally exceeded 500 mg. It has a relatively short duration of action usually lasting only several hours. Bupivacaine is a second-generation amide anesthetic that has a prolonged duration of action. It is, however, associated with cardiac and neurotoxic reactions and has a maximum recommended safe dose of 150 mg. Because of the poorer cardiac profile of bupivacaine that resulted from long-term sodium channel blockade in heart muscle, third-generation amide anesthetics were developed. Ropivacaine is a member of this group and produces local anesthesia for a longer period like bupivacaine but with a better cardiac profile. Injections of local anesthetic in percutaneous spine interventions are small enough that one should generally never approach the maximum allowable dosages.
Bupivacaine and ropivacaine come in different concentrations (0.25%, 0.5%, and 0.75% and 0.2% and 0.5%, respectively). The lower dosages are useful for pain relief in epidural and nerve blockage injections. The more-concentrated dosages produce motor blockade, which is an unwanted side effect with these procedures. The amounts of these drugs used in outpatient, percutaneous procedures are small compared with that needed to produce cardiac or neurotoxic effects.
Antibiotics
Antibiotics are needed only for selected procedures in spine intervention. These include discography, intradiscal electrothermal therapy, percutaneous discectomy, vertebroplasty and kyphoplasty, implantable pumps, and stimulators. Most routine injection procedures do not require antibiotics. The purpose of antibiotic coverage in most of these procedures is to decrease the chance of seeding bacteria in poorly vascularized sites, such as the disk or around foreign bodies (implantables). The antibiotics used for these procedures are generally not the more toxic or sophisticated ones, from the infectious disease standpoint. As penicillin allergy is not uncommon, a broad-spectrum antibiotic with minimal or no penicillin cross-reactivity is generally chosen. Cephalosporins have minimal penicillin cross-reactivity, and therefore a reasonable choice is _cefazolin (Ancef). Cefazolin is the most common antibiotic used for this purpose and is given in a 1-g dosage (intravenously [IV] or intramuscularly [IM]) 30 minutes before the procedure. In addition, it can be added to the contrast for discography procedures (usually 20–100 mg, with the upper range used when no IV antibiotics are given). It must be born in mind that this antibiotic will cause grand mal seizure activity if given intrathecally. No antibiotic should be included if a transdural approach is used.
In some patients, allergy or lack of access to an IV may make alternate choices better. Another commonly used antibiotic in the interventional laboratory is ciprofloxacin (Cipro). This is a fluoroquinolone with a broad spectrum of coverage and without cross-reactivity to penicillin. It is usually given orally in dosages of 500 mg twice a day. It can be given IV (400 mg) but must be given slowly over a prolonged period to avoid pain and IV site reaction. This generally limits its use in the laboratory to oral administration.
Another good alternative is levofloxacin (Levaquin), which is a fluorinated carboxyquinolone. It may be given orally or IV and has similar plasma and time profiles for both routes of administration, making it a good choice for either route (again, slow administration is required when given IV). The general dosage is 500 mg every 24 hours.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree