Abstract
There is a progressive adoption of point of care ultrasound (POCU) performed by acute care physicians in many clinical areas including the neonatal intensive care unit. There has been some resistance to POCU from consultative ultrasound specialties, much of which is due to misunderstanding the goals of POCU. Clearly there is a need for equipment, training, and accreditation structures in neonatal POCU. These structures need to be workable, relevant, and, most importantly, controlled from within the specialty of neonatology. There is a range of clinical situations in neonates where POCU can add invaluable and, at times, lifesaving diagnostic information. Understanding individual patient physiology, targeting treatment, and obtaining longitudinal feedback are important aspects of the use of neonatal POCU. Neonatal POCU is not just about the heart, but embraces the study of a range of organ systems including the brain, lungs, abdominal organs, and blood vessels for line localization.
Keywords
accreditation, cardiac ultrasound, infant newborn, point of care ultrasound, transitional circulation
- •
The use of point of care ultrasound (POCU) in the care of sick and preterm neonates is rapidly expanding.
- •
The benefits of a portable, bedside technique that is able to provide real time, longitudinal data regarding the physiology of individual patients allowing more targeted treatment is being progressively recognized as we move towards the era of personalized medicine in neonatology.
- •
POCU has an important role in managing the transitioning term or preterm infant, the septic/asphyxiated infant, the shocked or hypotensive infant and infants with suspected PPHN or congenital heart disease.
- •
POCU is usually a predominantly ‘rule in’ diagnostic modality and does not aim to ‘rule out’ all diagnoses whereas consultative ultrasound should also be a ‘rule out’ diagnostic modality.
- •
With the acceptance of the usefulness of ultrasound in the clinical setting, the need for appropriate training programs and accreditation increases.
- •
Approaches to training and accreditation vary across different countries.
It is a limitation in the intensive care of the newborn infant that we have few tools with which to monitor cardiovascular and hemodynamic function. There is usually the ability to continuously monitor invasive blood pressure and heart rate and that’s about it. Beyond that, reliance is placed on rather inaccurate measures of contemporaneous hemodynamic well-being such as skin capillary refill time and urine output and measures that do not reflect the changes in the hemodynamic status in real time, such as the acid-base status. Near-infrared spectroscopy (NIRS) is evolving as a potentially useful monitoring tool for the real-time assessment of tissue oxygenation of the organ interrogated (brain, kidney, muscle, or intestines; see Chapter 16 , Chapter 17 , Chapter 18 ). As for measuring cardiac output, there is little outcome-based validation for tools designed to measure cardiac output (see Chapter 14 , Chapter 21 ). The difficulties of small patient size and a smaller commercial market limit neonatology access to a range of tools for monitoring cardiac output which are available for the intensive care of the older subject, such as thermodilution, electrical impedance velocimetry, continuous Doppler methodologies, and derivations from blood pressure waveforms.
Doppler cardiac ultrasound provides a noninvasive, albeit noncontinuous, technique from which it is possible to derive estimates of a wide range of hemodynamic parameters as well as information on structure and function of the organ that drives the circulation, the heart. Integration of cardiac ultrasound into routine neonatal intensive care has been limited by the concentration of the necessary skills in specialist groups who work predominantly outside the neonatal intensive care unit (NICU). This results in information that is often neither timely nor particularly well focused on hemodynamics. From a research perspective, it meant that there were assumptions derived from a limited number of snapshots rather than serial studies to document natural history.
Neonatology, like many acute care specialties, has recognized the limitations of an external consultative ultrasound model and neonatologists are increasingly developing cardiac ultrasound skills themselves so they can be applied at the acute point of care. This has allowed more systematic serial studies, which in turn is facilitating the development of the research and clinical monitoring potential of these methodologies. It should be emphasized that acute point of care ultrasound (POCU) does not replace the need for consultative ultrasound. Rather it addresses different questions and complements consultative ultrasound. The best outcomes are achieved when the two models work collaboratively alongside each other.
This chapter will provide an overview on the use of cardiac ultrasound to assess the neonatal circulation (details of the individual techniques will be outlined in other chapters), as well as discussing issues of training, accreditation, and interaction with other imaging specialists.
Politics of Ultrasound
The evolution of ultrasound into the area of acute care has its political problems and this has not been confined to neonatology. On one side of the argument, acute care specialists have recognized the rapid diagnostic potential of ultrasound, a potential that is difficult to fulfill within a consultative model of ultrasound. The improvement in quality of imaging and portability of equipment has made ultrasound accessible to anyone with a good understanding of anatomy and access to training. On the other side of the argument, some consultative imaging specialists have resisted this on the basis of concerns about lack of accredited training and the risk of diagnostic error. Importantly, a recent review of medico-legal cases involving neonatal/pediatric POCU in the United States found no evidence of this risk. Like all political divides, there are merits to both arguments. Consultative ultrasound specialists have neither the ability nor often the desire to be available 24/7 for the rapid diagnostic situations facing acute care specialists. POCU, particularly in neonatology, has often evolved with a lack of good training and accreditation structures. Many of the early adopters of POCU were largely self-taught, or taught by a cardiologist with a balanced perspective of the usefulness of functional ultrasound in the NICU. While this is changing, as will be described later, there is a risk that this may lead to diagnostic error. As always, the answer lies in the middle with a system that takes advantage of the strengths of both systems and minimizes the risks. POCU is usually a predominantly “rule in” diagnostic modality and does not aim to “rule out” all diagnoses, whereas consultative ultrasound should also be a “rule out” diagnostic modality. For example, a neonatologist, when faced with a baby with possible pulmonary hypertension at 2:00 a.m., wants to assess pulmonary artery pressure, direction of shunts through the fetal channels, and estimate systemic and pulmonary blood flow. He or she would hope to recognize congenital heart disease (CHD), but would not be able to rule it out. That would be a job for the cardiologist who would come the next day. So, the baby benefits from the timely use of ultrasound to guide appropriate intensive care intervention and also benefits from the expertise of the cardiologist in being able to confirm structural normality or otherwise. Such collaborative care should not be a source of interdisciplinary conflict. Rather, it strengthens collaboration and has the potential to significantly improve patient care.
It is our experience that much of the resistance to establishing a POCU program is based on a lack of understanding of the goals. Resolution comes from reassurance about training and quality issues and education about purpose, most importantly, that the intent is to complement, not replace, the role of those consultative specialties .
What’s in a Name?
The biggest risk of cardiac ultrasound performed by non-cardiologists is that it is recorded that a baby has had an echocardiogram and so it is assumed by subsequent health care providers that CHD has been excluded. Recognizing this risk, there has been a range of terminology applied including functional echocardiography and targeted echocardiography. Our opinion on terminology has evolved from these terms, understanding that the communication risk comes, at least in part, from the use of the word echocardiography. Because this term grew up within the specialty of cardiology, if it is applied to a study, whatever the prefix, there is a risk of assumption that it has been performed by a cardiologist. Because of this risk, in this chapter, we refer to “cardiac ultrasound” with a prefix that communicates that the study was not performed by a cardiologist but by an acute care physician. This could be “point of care,” “clinician-performed,” or, more specifically, neonatologist-performed cardiac ultrasound. This also has the advantage that it does not confine the terminology to the heart, recognizing that neonatal POCU has many uses beyond the heart.
Training and Accreditation in Point of Care Ultrasound
It is the nature of the evolution of any procedure or technology that the early adopters are often self-taught. Development of training and accreditation structures follows when the need is identified and there is enough of a critical mass of early adopters to provide the necessary support. There are good examples of training structures in POCU such as that developed by the American College of Emergency Physicians; however, there is a long way to go in neonatal POCU. Internationally, there is difference of opinion in the relative weight that should be given to training provided by those outside neonatology compared with those within. In Australia and New Zealand, we have developed a training program which is based on the philosophy that training for POCU in the NICU is best undertaken in the NICU under supervision of appropriately trained and accredited neonatologists while also recognizing the need for support from the consultative imaging specialists. The program was developed in 2007 under the auspices of the Australasian Society of Ultrasound in Medicine (ASUM) who, having recognized the inevitable evolution of ultrasound into acute care areas, had developed a qualification called the Certificate in Clinician Performed Ultrasound (CCPU). There were already modules for several acute care specialties and neonatology was developed as another module. The program was developed by a steering committee consisting of mainly neonatologists from around Australia and New Zealand, which included a radiologist and a pediatric cardiologist. The qualification is based on course attendance and supervised logbooks of ultrasound scans. The trainees have to complete an on-line physics course, then the ultrasound training is in two stages, basic and advanced. Basic training is aimed at normal image acquisition of the heart and brain, while advanced training is aimed at interpretation of abnormal hemodynamic and cerebral findings, as well as learning some other aspects of neonatal POCU such as basic abdominal organ imaging and central line localization. The core part of training is undertaken within the neonatal unit under the supervision of a qualified POCU clinician who can also teach the skills of integration of the ultrasound and clinical findings. The advanced module includes training in recognition of common CHD with the understanding that the ability to exclude CHD will require further training under the supervision of pediatric cardiology. The expectation is that only a few neonatologists undertake this extra training and others will continue to consult with pediatric cardiology colleagues to exclude structural cardiac abnormalities. This program has been running since 2007, and there are more than 60 graduates with the CCPU (neonatal) and 40 trainees currently undertaking training. The Australasian CCPU was the first and, to the best of our knowledge, is still the only dedicated and functioning neonatal point of care training and accreditation program.
Consensus statements on neonatal cardiac ultrasound training have been published from North America and Europe and the United Kingdom. Both of these statements take a different focus with an emphasis on training within pediatric cardiology. Neither of these statements addresses the wider role for neonatal POCU beyond the heart. The development of national or regional administered structured training programs under these guidelines is still in progress.
It is our view that to achieve the goal of quality assurance in standards of neonatal POCU, a training program needs to be both relevant and workable. For this to happen, the practical component of the training needs to occur mainly within the NICU and the training needs to be mainly provided by neonatologists. A core component of training is understanding how to integrate imaging skills into the other clinical information available for a particular patient. Further, the training program needs to embrace the fact that POCU in any acute care specialty embraces more than one organ.
Using Physiology to Target Treatment
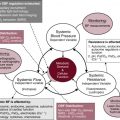
A key use of POCU in the clinical setting is to help understand the underlying physiology and subsequently to more accurately decide on what treatment is most useful for the individual patient. An illustration of the process of identifying individual physiology in a focused ultrasound, applying this information, and assessing the outcome of treatment choices is shown in Fig. 10.1 . This targeting of treatment with the ability to longitudinally monitor response is the way we most often use POCU and is best demonstrated by some case presentations.
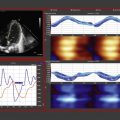
Thirty-eight-week gestation, emergency lower segment caesarean section (LSCS) for maternal pre-eclampsia. Clear amniotic fluid. Respiratory distress from birth with increasing oxygen requirement requiring CPAP at 7–8 cm H 2 O. By 6 hours of age, requiring 0.75 FiO 2 to maintain arterial O 2 saturation of >85%. At 6.5 hours, sudden deterioration with arterial O 2 saturations below 80% in FIO 2 1.0. Chest x-ray (CXR) showed some centralized opacification in both lung fields and a small right-sided pneumothorax. Options considered include mechanical ventilation, needle drainage of pneumothorax, and use of inhaled nitric oxide (iNO). As oxygen requirements were out of proportion to CXR and labile clinical state, iNO was the favored clinical option. Prior to commencement of iNO, a POCU was performed.
Findings: See Fig. 10.2 .

Outcome Case Study 1
Cardiac POCU showed no evidence of raised pulmonary pressures with normal cardiovascular function. Consequently, no iNO was administered. There was an attempted needle aspiration of pneumothorax—no air recovered. Mechanical ventilation was transitioned to high-frequency ventilation, given surfactant, a lung recruitment strategy was used and CO 2 controlled with a gradual improvement in FIO 2 requirements. Rapid recovery in 12–18 hours. Case illustrates that sometimes POCU supports a clinical decision to not introduce specific therapies such as iNO.
Twenty-five-week gestation, incomplete antenatal steroid coverage. Initial CPAP at 6 cm H 2 O. Intubated and given surfactant at 2 hours of age due to increasing oxygen requirements (0.35 FIO 2 ). Given intravenous antibiotics. Rapidly extubated back to CPAP 6 cm H 2 O in air. Now 10 hours old and increasing FIO 2 to >0.40 with borderline blood pressure (mean BP = 25 mm Hg). CPAP increased to 7 cm H 2 O with transient improvement. CXR shows well-expanded lungs. Options considered were to re-ventilate and give further surfactant, wait for further improvement, or gain more clinical information from a POCU.
Findings: See Fig. 10.3 .

Outcome Case Study 2
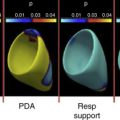
Cardiac POCU showed evidence of an unconstricted large left-to-right ductal shunt with added left-to-right shunt at the patent foramen ovale (PFO). There were also signs of increased pulmonary blood flow and impairment of systemic blood flow (SBF). Early targeted treatment with indomethacin at 0.2 mg/kg was started to attempt patent ductus arteriosus (PDA) closure. Cardiac POCU 24 hours later showed a closed PDA and return of the hemodynamic state to normal. There was concurrent improvement in ventilation requirements with decreasing FIO 2 and CPAP pressure requirements. Case illustrates that a small number of infants (particularly <26 weeks, incomplete steroid cover) still have early symptomatic PDA that has the potential to respond well to early treatment.