Acknowledgments
All figures and much of the text in this chapter have been reprinted with permission from: Sodickson A. Strategies for reducing radiation exposure in multi-detector row CT. Radiol Clin North Am . 2012;50(1):1-14; and Sodickson A. Strategies for reducing radiation exposure from multidetector computed tomography in the acute care setting. Can Assoc Radiol J . 2013;64(2):119-129.
Synopsis
Many tools and strategies exist to enable reduction of radiation exposure from computed tomography (CT). The common CT metrics of x-ray output—the volume CT dose index (CTDI vol ) and dose length product (DLP)—are explained and serve as the basis for monitoring radiation exposure from CT scans. Many strategies to dose optimize CT protocols are explored that, in combination with available hardware and software tools, allow robust, diagnostic-quality CT scans to be performed with a radiation exposure appropriate for the clinical scenario and the size of the patient. Specific emergency department (ED) example protocols are used to demonstrate these techniques.
Introduction
Radiation exposure has received much attention of late in the medical literature and lay media. It is commonly recognized that CT has tremendously advanced our diagnostic capabilities in the ED and broadly throughout medicine. These diagnostic benefits have combined with widespread availability and rapidity of scanning to produce marked increases in CT use, estimated at approximately 69 million CT scans per year in the United States. However, rapidly increasing use has heightened concerns about the collective radiation exposure to the population as a whole and about the high levels of cumulative exposure that may occur in patients undergoing recurrent imaging for chronic conditions or persistent complaints.
CT has received the greatest scrutiny because of its relatively high radiation dose per examination. Although it constitutes about 17% of all medical imaging procedures, it produces approximately half of the population’s medical radiation exposure, with nuclear medicine contributing approximately one quarter of the collective dose to the population and fluoroscopy and conventional x-ray examinations accounting for the remainder. Yet even in relatively young patients (in whom the radiation risks are thought to be larger), the risks for mortality related to the underlying disease or condition have been found in general to be far greater than the estimated risks for radiation-induced cancer mortality from CT.
There are many possible strategies for reducing radiation exposure to the population as a whole and to individual patients. Once the decision is made to perform a CT scan, many imaging strategies can reduce the radiation dose while maintaining appropriate diagnostic quality for the clinical task at hand. There have been tremendous advances in CT technology in recent years that allow high-quality examinations to be performed at progressively lower radiation dose. The common practice of porting CT protocols from older to newer scanners often fails to take maximal advantage of these new technologies. Routine optimal scan acquisition requires that radiologists invest the effort to understand their technology and to implement dose-optimized protocols, ideally in collaboration with CT manufacturers, CT technologists, and medical physicists. This is admittedly a daunting task for many radiologists, who often view their primary role as diagnosticians and interpreters of images and often have little detailed training in CT technology.
This chapter will describe several practical opportunities to reduce radiation exposure from CT, with emphasis on how CT protocols can be modified to reduce dose while maintaining diagnostic quality. Specific implementation of these strategies is highly dependent on the available technology, and there is no replacement for hands-on training at the scanner.
Reducing Radiation Exposure: Before the Scan
The most effective way to reduce radiation exposure is to avoid performing the examination. Before a scan is performed, many measures can be taken to control use, with the goal of reducing low-yield examinations that will not contribute significantly to the care of the patient. It is admittedly often challenging to prospectively determine which examinations these will be. Nonetheless, scrutiny of examination appropriateness is vital. In optimal circumstances this can rely on well-validated clinical decision rules such as those for pulmonary embolus or for head or cervical-spine imaging in trauma. These rules may be integrated into predefined imaging algorithms in the effort to standardize the imaging approach in specific clinical scenarios or patient populations. Alternatively, these algorithms or expert panel appropriateness criteria may be incorporated into decision support advice during computerized physician order entry.
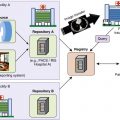
Duplicative and recurrent imaging are natural targets for radiation dose reduction. Ordering physician awareness of duplicate imaging may be achieved via review of the medical record or in automated fashion as part of decision support tools. In certain circumstances, interventions to eliminate unnecessary repeat imaging can be highly effective in reducing use. As an example, during interhospital patient transfers, importation to a picture archiving and communication system (PACS) of outside hospital imaging examinations via image transfer networks or from CD has been found to significantly reduce CT use (by 16% at our institution), primarily by eliminating unnecessary repeat scans.
Defensive medicine and self-referral of diagnostic imaging have both been implicated as significant contributors to imaging use. Effectively addressing these systemic issues will require higher-level attention in our health care delivery system.
Understanding the X-Ray Output Metrics CTDI vol and DLP
To understand and monitor radiation exposures from CT scans, a basic understanding is first needed of the radiation exposure metrics commonly used in CT. The CTDI vol and the DLP are well-calibrated and standardized measures of x-ray tube output. They are measured in cylindrical acrylic phantoms of standard diameter—either a 16-cm “head” phantom or a 32-cm “body” phantom. A 100-mm long ionization chamber connected to an electrometer is placed inside a hole in either the center or periphery of the CTDI phantom, and measurements are made (with the CT table stationary) under a particular CT exposure to yield CTDI 100 measurements. The CTDI vol is a weighted sum of these central and peripheral measurements, along with a geometric correction to account for the pitch of a helical scan:
C T D I v o l = ( 2 3 C T D I 100 , p e r i p h + 1 3 C T D I 100 , c e n t e r ) / p i t c h
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree