Clinical: Clinically, the tumor has an aggressive course, with an expanding soft tissue mass, soft and tender on palpation, with increased local temperature. Pathologic fracture is not uncommon.
Imaging: Imaging shows a purely osteolytic lesion with ill-defined limits. Isotope scan shows an increased uptake. CT and MRI show the multicystic pattern (high signal in both T1 and T2 because of fluid and hemosiderin content) with fluid levels.
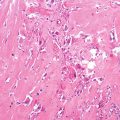
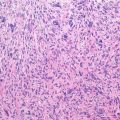
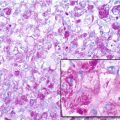
Histopathology: Grossly, the tumor is constituted by large cavities filled with blood and clots. Neoplastic tissue constitutes the septa; it is very soft and can be very scarce, overwhelmed by hemorrhage. The permeative pattern is particularly evident, and the cortex and periosteum are often extensively destroyed. Histologically under low power, the pattern is similar or identical to an ABC. Only at higher power, the sarcomatous nature of cells becomes apparent, because all telangiectatic OS are high-grade malignant. Sometimes, however, the hemorrhage and necrosis are so massive that it is difficult to find viable cells and to appreciate anaplasia. Osteogenesis is usually focal, and often it must be searched for in numerous sections and rarely may not be found at all, yet with the overall clinical, gross, and histological patterns are entirely consistent with telangiectatic OS, minus finding of osteoid or bone production by the sarcoma cells within the aneurysmal bone-cyst-like walls. Atypical mitoses are easily identified.
Course: The course is rapid, and the stage is almost regularly II-B or III.
Treatment and Prognosis: Treatment and prognosis are the same as for classic OS. Some data suggest that response to preoperative CTx is particularly good, which can be explained by the rich vascularity of the tumor, enhancing the ability of the chemotherapeutic agents to reach the malignant cells.
Key Points
Clinical
Stay updated, free articles. Join our Telegram channel
Full access? Get Clinical Tree
 Get Clinical Tree app for offline access
Get Clinical Tree app for offline access

|