Congenital
Infectious and inflammatory
Idiopathic
Bile stasis
Benign neoplasm
Malignant neoplasm
Trauma
Agenesis
Acute calculous cholecystitis
Adenomyomatosis
Gallstones
Adenoma
Gallbladder carcinoma
Gallbladder hematoma
Duplication
Acute acalculous cholecystitis
Cholesterolosis
Sludge
Gallbladder metastasis
Gallbladder laceration/rupture
Ectopic
Chronic cholecystitis
Cholesterol polyp
Milk of calcium bile
Lymphoma
Septate
Gangrenous cholecystitis
Atresia/hypoplasia
Emphysematous cholecystitis
Hemorrhagic cholecystitis
Xanthogranulomatous cholecystitis
AIDS cholecystitis
This chapter begins with a description of normal gallbladder anatomy and anatomic variants followed by gallbladder imaging techniques. Next, this chapter divides gallbladder diseases according to imaging patterns—intraluminal filling defects, diffuse gallbladder wall thickening, focal gallbladder wall thickening, abnormal gallbladder wall density, distended gallbladder, and hyperdense bile—and discusses in each section how to correctly diagnose gallbladder disease.
Normal Anatomy
The gallbladder, an embryologic derivative of the foregut, is a pear-shaped muscular membranous sac that lies on the inferior surface of the liver and serves to store and concentrate bile produced by the liver. It has a capacity of about 50 mL and measures approximately 8 cm in length by 4 cm in diameter when distended. The gallbladder normally receives its blood supply from the cystic artery, a branch off the right hepatic artery. On imaging, the normal gallbladder in a fasting patient has a thin wall (<3 mm in thickness), without intraluminal filling defects (Fig. 6.1).
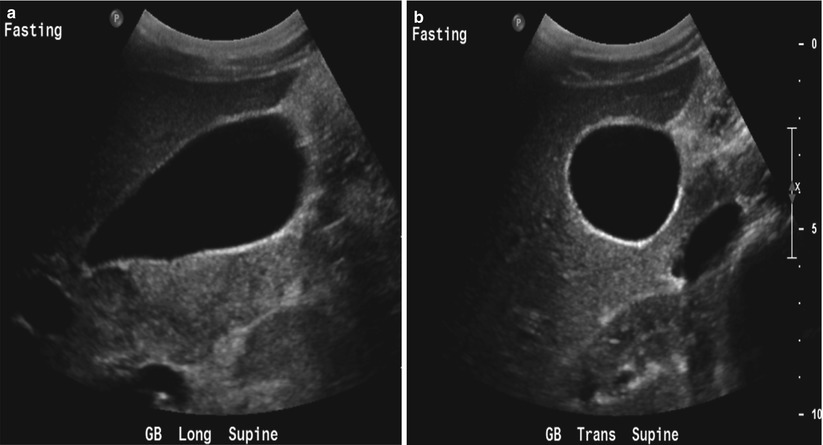

Fig. 6.1
Normal gallbladder in a fasting patient. These longitudinal (a) and transverse (b) US images show a normal distended gallbladder with thin (<3 mm) walls, with anechoic bile without filling defects
For descriptive purposes, the gallbladder is divided into the fundus; body; infundibulum; and neck, which connects to the cystic duct (Fig. 6.2). The gallbladder infundibulum is a tapered area between the gallbladder body and neck. Hartmann’s pouch is a small bulge along the inferior surface of the infundibulum close to the gallbladder neck.
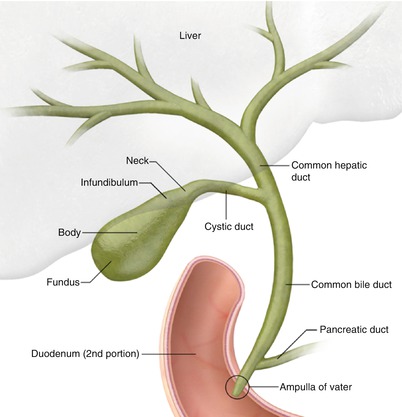

Fig. 6.2
Normal gallbladder anatomy
The cystic duct joins with the common hepatic duct to form the common bile duct. The common bile duct courses into the head of the pancreas and joins the main pancreatic duct to form the ampulla of Vater at the major duodenal papilla. The sphincter of Oddi, a circular band of smooth muscle, surrounds the distal end of the common bile duct and main pancreatic duct at the level of the ampulla of Vater.
Anatomic Variants
Gallbladder
Congenital gallbladder variations are generally of little clinical significance; however, familiarity with variants helps avoid interpreting them as pathological on imaging studies. Variant gallbladder shapes that predispose to bile stasis increase the risk of gallstone formation. See the chart below for an array of variants (Algorithm 6.1) [2, 3] (Fig. 6.3).
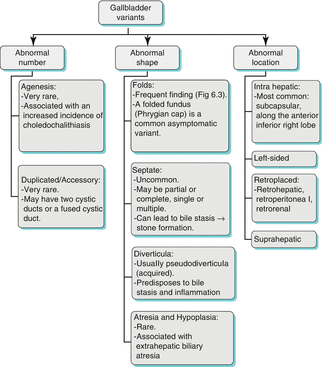

Algorithm 6.1 Chart demonstrating gallbladder variants in number, shape, and location

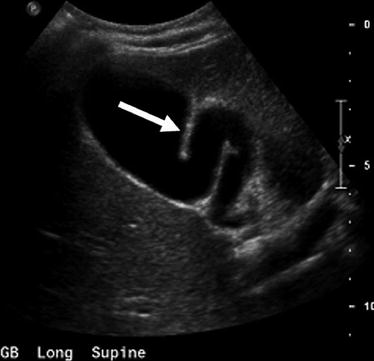
Fig. 6.3
Gallbladder fold. This longitudinal US image shows an echogenic line (arrow) in the gallbladder body consistent with a fold
Cystic Duct
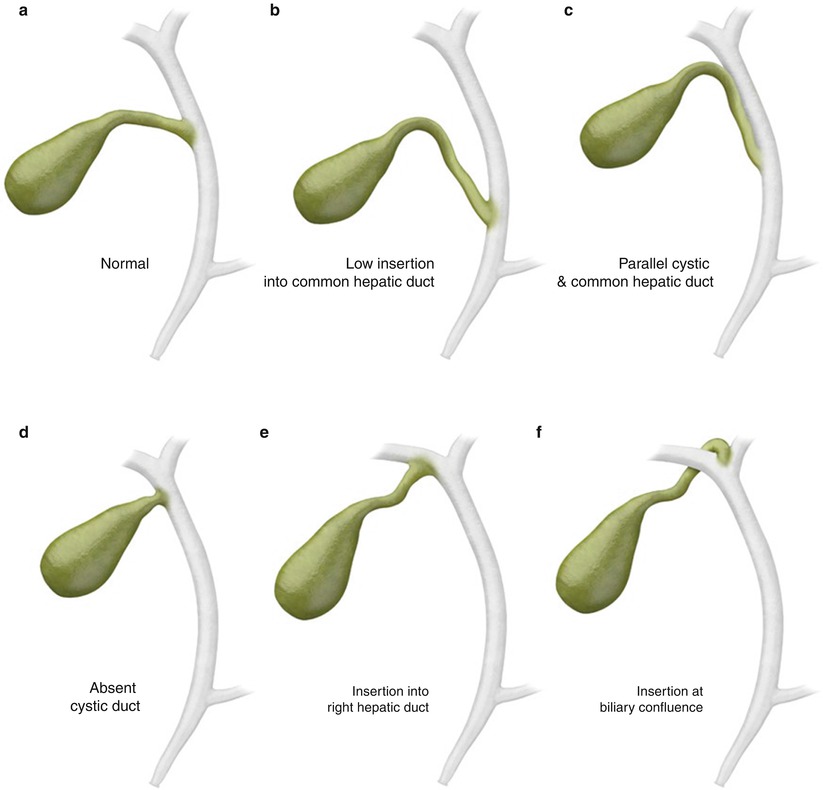
The course of the cystic duct and point of insertion into the common hepatic duct (Fig. 6.4a) varies greatly (Algorithm 6.2). The reported incidence of low insertion of the cystic duct close to the duodenal papilla (Figs. 6.4b and 6.5) ranges from 8 to 14 % [3]. When the cystic duct runs parallel to the common hepatic duct (Fig. 6.4c), there is increased risk of injuring the common hepatic duct at cholecystectomy through clamping or traction. Very rarely, the cystic duct may be absent, and the gallbladder drains directly into the common hepatic duct (Fig. 6.4d). The cystic duct may insert into the right (Fig. 6.4e) or left hepatic duct or at the biliary confluence (Fig. 6.4f). It may also loop around the common hepatic duct and insert medially [3].
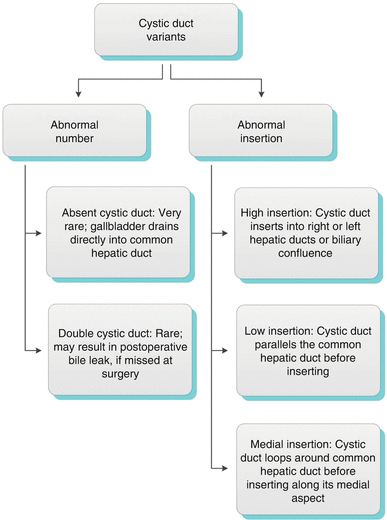

Algorithm 6.2 Chart demonstrating variants in number and location of insertion of the cystic duct

Fig. 6.4
(a–f) Cystic duct variants

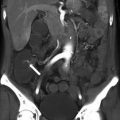
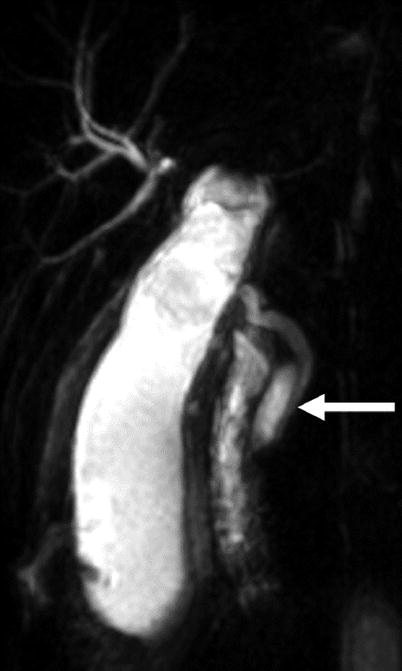
Fig. 6.5
Low medial insertion of cystic duct into common hepatic duct. This coronal maximum intensity projection (MIP) MR cholangiopancreatographic (MRCP) image demonstrates low medial insertion of the cystic duct into the distal common hepatic duct (arrow), a common cystic duct variant
Imaging Techniques
In patients with suspected gallbladder disease, several imaging techniques can help determine the best management strategy (Algorithm 6.3).
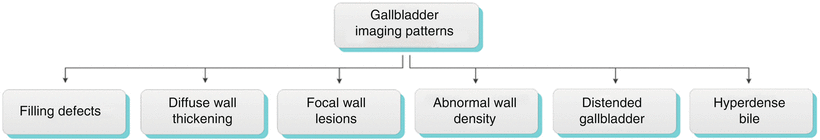

Algorithm 6.3 Chart demonstrating various imaging patterns of gallbladder diseases
Conventional radiographs are of little use in the diagnosis of gallbladder disease. Calcification outlining the gallbladder may be seen with porcelain gallbladder, but only 15–20 % of gallstones are visible on abdominal radiographs. Abnormal gas collections in the right upper quadrant may be seen in cases of emphysematous cholecystitis or when a fistula between the gallbladder and bowel is present.
Ultrasonography has a primary role in evaluating the gallbladder and biliary system since an ultrasound can usually be obtained rapidly, is cost-effective, and is excellent at assessing the presence of gallstones, gallbladder wall thickening, pericholecystic fluid, and biliary ductal dilatation. Ultrasonography also allows for the evaluation of a sonographic Murphy’s sign, which is a very specific indicator of acute cholecystitis. Ultrasonography may also detect metastatic disease in patients with a suspected malignancy.
Cholescintigraphy using Tc-99m-IDA (iminodiacetic acid) is useful to evaluate for or confirm acute cholecystitis, to assess for acalculous cholecystitis, to differentiate acute from chronic cholecystitis, and to evaluate for bile leaks.
CT is probably the best technique for evaluating complications of gallbladder disease and is useful when the diagnosis is unclear or alternative diagnoses need to be excluded. Although limited in that it may not visualize gallstones that are isodense to bile, CT depicts the gallbladder wall and pericholecystic tissues well. Intravenous iodinated contrast improves the evaluation of gallbladder disease and enables the detection of abnormal gallbladder wall enhancement, surrounding liver hyperemia, or alternate causes of right upper quadrant pathology.
MRI and MR cholangiopancreatography (MRCP) are excellent, noninvasive imaging techniques to evaluate for gallbladder and biliary disease. They can be performed without radiation or intravenous contrast and, when combined with routine contrast-enhanced MRI, can evaluate the solid parenchymal organs. MRCP is performed with heavily T2-weighted sequences, which significantly increase the signal of fluid-filled structures, such as the bile ducts and gallbladder, resulting in a very high bile-to-background contrast. Fat saturation is generally used to suppress the background signal to allow for better delineation of the gallbladder and biliary system. Thick-slab sections provide an overview of the biliary system and resemble conventional cholangiograms. Thin-slab multiplanar sequences and source images are critical in evaluating for small intraluminal filling defects or strictures, which may be obscured by volume averaging on the thick-slab images [4, 5]. High b-value diffusion-weighted MR imaging (DWI) has shown promise in differentiating benign from malignant gallbladder polypoid lesions and should be added to the routine MRI protocol for the work-up of these lesions [6].
Gallbladder Imaging Patterns
Gallbladder Intraluminal Filling Defects
This section describes a common imaging pattern in gallbladder disease, intraluminal filling defects (Algorithms 6.4 and 6.5). These filling defects include gallstones, sludge, and polypoid lesions (Fig. 6.6).
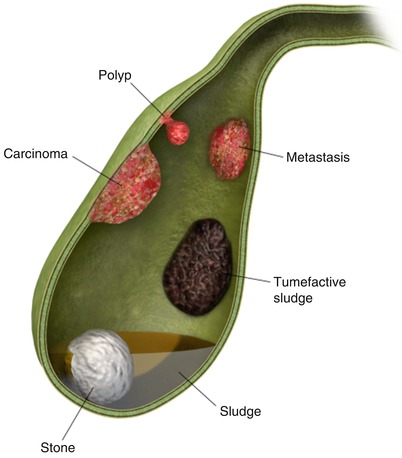
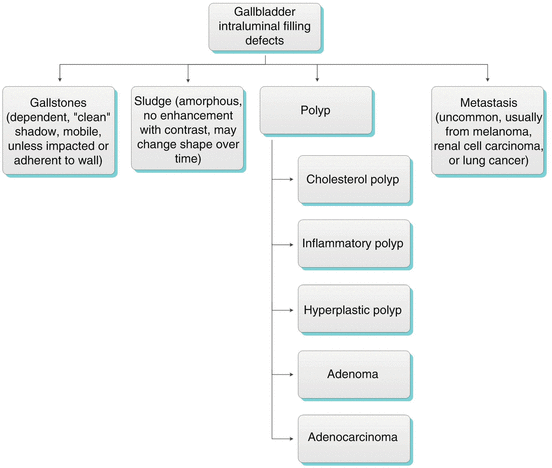
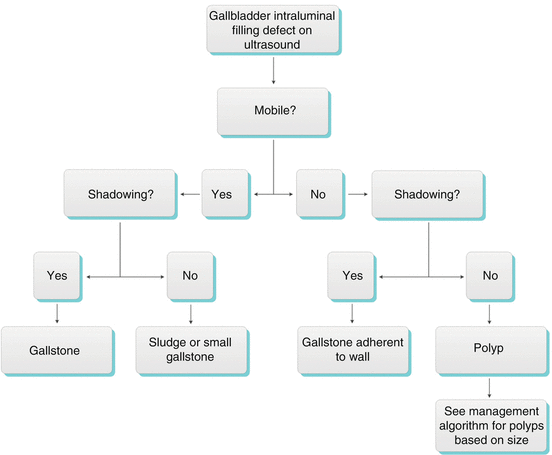

Fig. 6.6
Illustration demonstrating various etiologies and patterns of gallbladder intraluminal filling defects

Algorithm 6.4 Differential diagnosis of gallbladder intraluminal filling defects

Algorithm 6.5 Diagnostic approach to gallbladder intraluminal filling defects on ultrasound
Gallstones
Gallstones, the most common biliary pathology, are formed from insoluble bile components, including cholesterol, pigment (calcium bilirubinate), and calcium carbonate. In the United States, cholesterol stones are by far the most common type of gallstone and tend to be larger than pigment stones.
Gallstones are frequently found incidentally but may give rise to various pathologic conditions, including cholecystitis, biliary colic, biliary obstruction, and pancreatitis.
Ultrasonography is highly accurate in detecting gallstones and is the preferred imaging modality. On US, nonimpacted gallstones tend to appear as mobile, echogenic foci in a dependent position with “clean” (echo-free) posterior acoustic shadowing (Fig. 6.7). Shadowing or mobility often differentiates gallstones from polyps. Small gallstones may not shadow. To increase the detection of shadowing, the following ultrasound parameters can be adjusted: image the gallstone in the center of the beam, use a higher frequency transducer, and narrow the beam width [7].
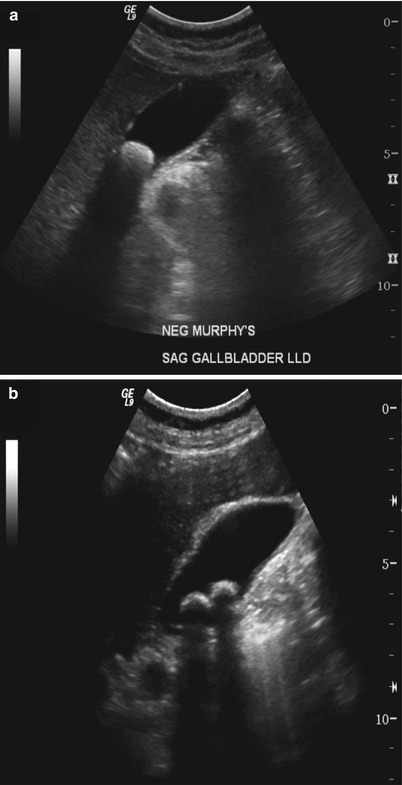

Fig. 6.7
Gallstones on US images. (a, b) Hyperechoic rounded filling defects with “clean” acoustic shadowing are shown layering in a dependent position.
In order to evaluate for gallstone mobility, the patient can be rolled into a new position, usually left lateral decubitus, and the gallbladder reimaged. A mobile gallstone will roll into the most dependent portion of the gallbladder. Gallstones that are adherent to the gallbladder wall and do not show clear shadowing may mimic polyps (Fig. 6.8).
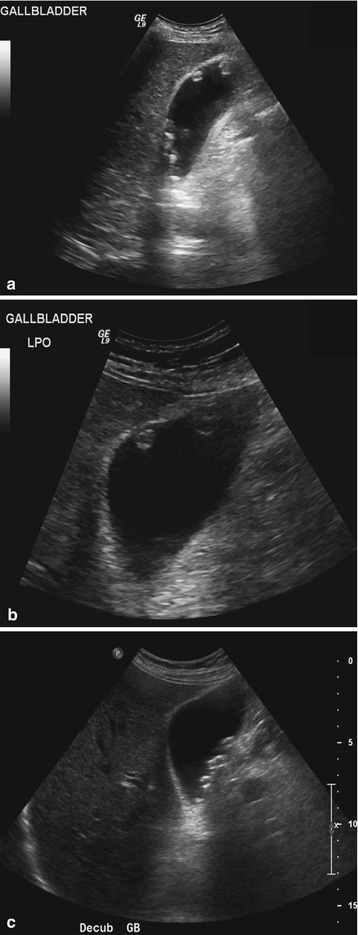

Fig. 6.8
Gallstones adherent to the gallbladder wall mimicking polyps. Longitudinal US images in supine (a) and left lateral decubitus (b) positions show rounded filling defects along the gallbladder wall, which proved immobile when the patient was repositioned. These were interpreted as possible polyps versus gallstones. (c) The patient was reimaged 2 days after the initial US study due to worsening abdominal pain, which showed the filling defects layering dependently, proving these were not polyps but rather gallstones. The patient’s abdominal pain resulted from gallstone pancreatitis (not shown)
If the gallbladder is filled with gallstones, the wall-echo-shadow sign (WES sign) may be seen (Fig. 6.9) and can make it difficult to identify and evaluate the gallbladder. The sign consists of two parallel curvilinear hyperechoic lines (line closer to transducer = gallbladder wall, line more distal = gallstones) separated by a thin hypoechoic space (thin layer of bile between gallbladder wall and gallstones), with shadowing posterior to the gallstones [8].
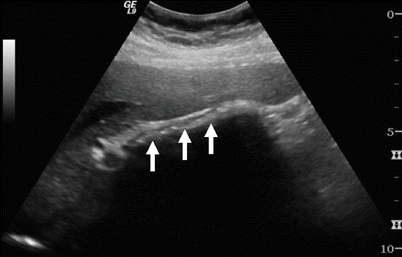

Fig. 6.9
Wall-echo-shadow sign. This longitudinal US image shows a gallbladder filled with gallstones (arrow)
CT detects approximately 75 % of gallstones. The sensitivity for CT in detecting gallstones depends on the makeup of the stones. Noncalcified stones may be isodense to bile and may not be detected (Figs. 6.10 and 6.11) or may be recognized as subtle filling defects with a density slightly higher or lower than the surrounding bile. Cholesterol stones may float when the specific gravity of the bile is higher than that of the stone. When gallstones contain calcium or gas, they can be readily identified. The patterns of gallstone calcification range from densely calcified to lamellated (Fig. 6.12) to centrally calcified. Gallstones that contain gas (nitrogen) within fissures may display a “Mercedes Benz” sign, which refers to the triradiate appearance of gas density.
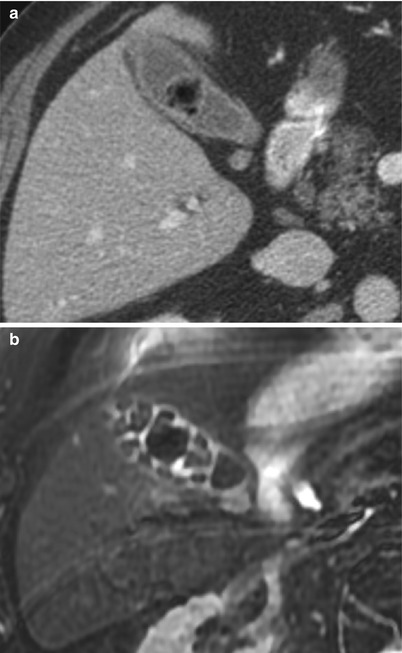
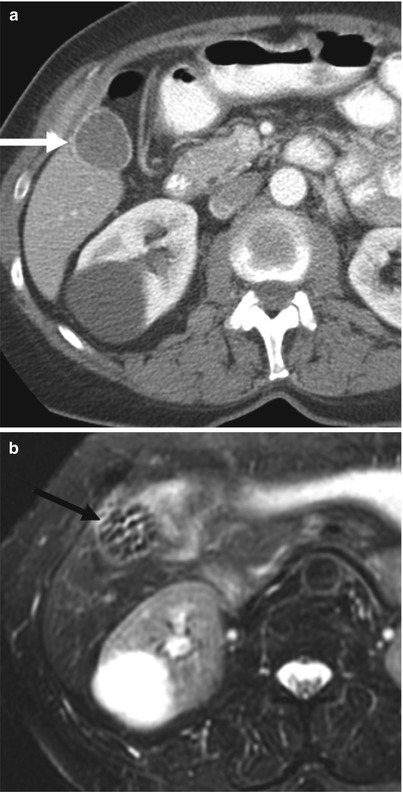
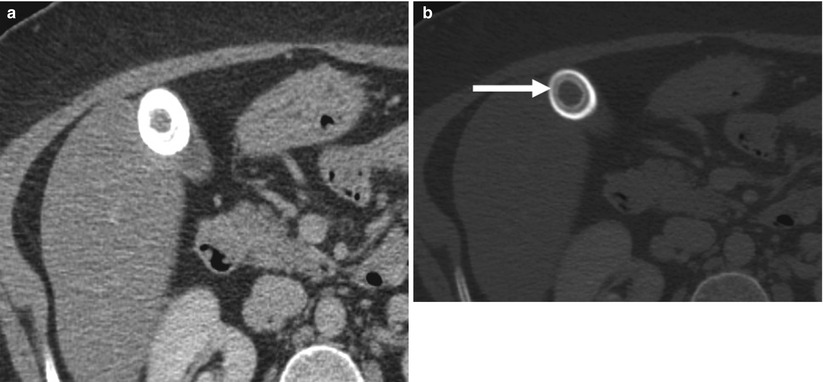

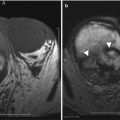
Fig. 6.10
Gallstones more visible on MRI. (a) Contrast-enhanced CT. A single hypodense filling defect in the gallbladder is consistent with a gas-filled gallstone. (b) Axial T2-weighted MRI. MRI from the same patient demonstrates multiple additional gallstones, which were isodense to the bile on the corresponding CT image, filling the gallbladder

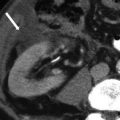
Fig. 6.11
Gallstones better seen on MRI. (a) This axial contrast-enhanced CT image demonstrates a normal-appearing gallbladder (arrow), without obvious gallstones. (b) However, this axial T2-weighted MR image, performed for further evaluation of another abnormality, demonstrates multiple small gallstones, which were undetected by CT

Fig. 6.12
Gallstone on CT. These axial CT images show a dense rounded stone on CT “soft-tissue” window (a), which shows a lamellated appearance (arrow) on CT “bone” window (b)
On MRI, gallstones are usually recognized as hypointense filling defects (Fig. 6.13) but may appear hyperintense on T1-weighted imaging.
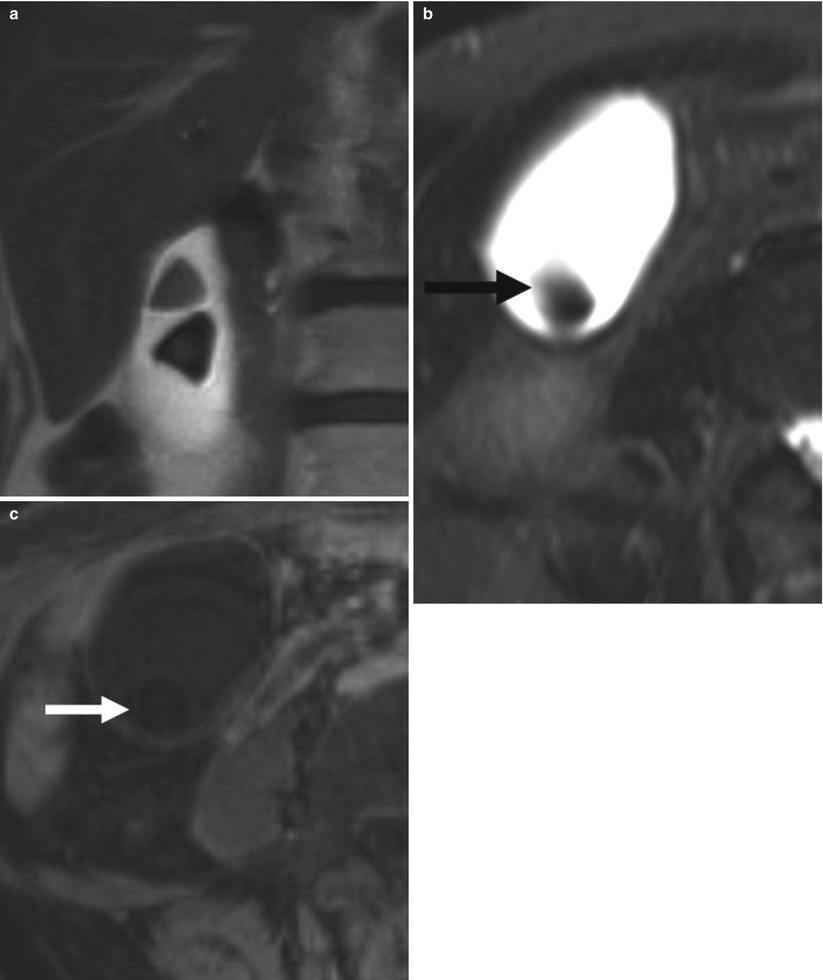

Fig. 6.13
Gallstones on MRI. (a) This coronal T2-weighted MR image shows two triangular filling defects in the gallbladder consistent with gallstones. (b) This axial T2-weighted MR image shows a gallstone (arrow) layering dependently. (c) This axial T1-weighted MR image shows the hypointense gallstone (arrow) surrounded by hypointense bile
Gallstone spillage, also known as dropped gallstones, is a well-known complication of laparoscopic cholecystectomy and may occur when the gallbladder is perforated during dissection from the liver bed or during extraction of the gallbladder through the narrow port site [9, 10]. The spilled stones may remain in the peritoneal cavity adjacent to the liver or may migrate to distant sites, such as the pelvis or pleural space (Fig. 6.14). Rarely, the spilled stones may lead to complications presenting months to years following the laparoscopic cholecystectomy, including abscess formation in 0.3 % of patients (Fig. 6.15) [10]. This is more common with bilirubinate stones which can contain viable bacteria. The diagnosis of an abscess associated with a spilled gallstone can be straightforward on CT if the stone is radiopaque, but is more challenging when the gallstones are nonopaque. Ultrasound or even MRI may be helpful to identify the gallstone.
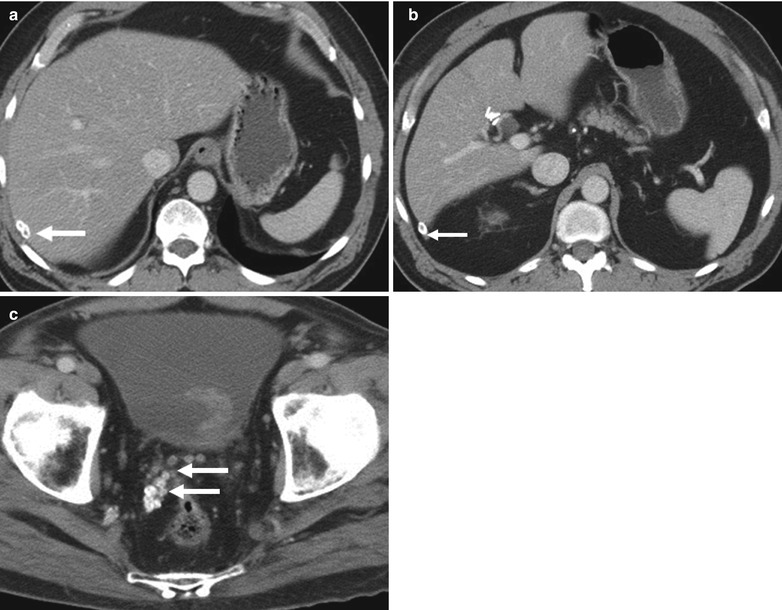
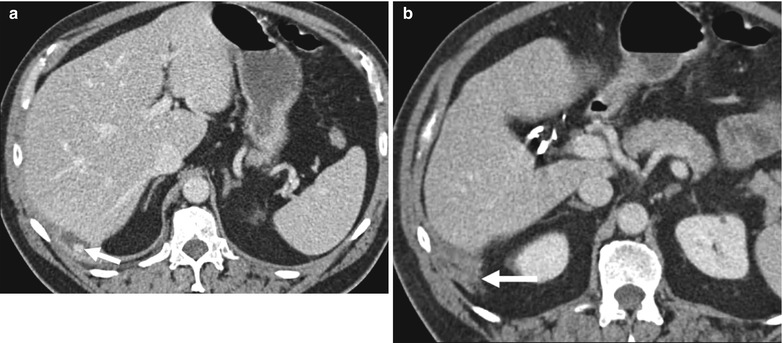

Fig. 6.14
Dropped gallstones. (a–c) Axial contrast-enhanced CT images demonstrate multiple rim-calcified gallstones (arrows) along the posterior margin of the liver and within the pelvis in this patient who underwent a laparoscopic cholecystectomy. Note the cholecystectomy surgical clips in the gallbladder fossa

Fig. 6.15
Dropped gallstone complicated by abscess formation. (a) Axial contrast-enhanced CT shows a small loculated fluid collection along the posterior liver margin of the right lobe of the liver consistent with an abscess. A spilled gallstone (arrow) is seen within the abscess. (b) Axial contrast-enhanced CT images show inflammatory changes (arrows) in the perihepatic fat posterior to the liver. Note the cholecystectomy surgical clips in the gallbladder fossa. Abscesses associated with dropped gallstones are usually treated by surgery rather than percutaneous drainage to remove all gallstones, which can act as a nidus for recurrent infections
Sludge
Gallbladder sludge is a mixture of bile and precipitated crystals/tiny gallstones and is identified on ultrasound as amorphous slightly echogenic material layering within the dependent gallbladder (Figs. 6.16 and 6.17). Sludge can be differentiated from gallstones by the lack of acoustic shadowing and its slowly shifting shape with patient repositioning. Sludge commonly results from bile stasis and is frequently noted in patients with prolonged fasting, long-term total parenteral nutrition, or critical illness [11]. It may completely resolve or progress to gallstones. Similar to gallstones, sludge is most often asymptomatic but may result in biliary colic in approximately 10 % of cases, acute cholecystitis, or acute pancreatitis [11]. Blood, pus, and necrotic debris may be indistinguishable from sludge by ultrasound but are much less common.
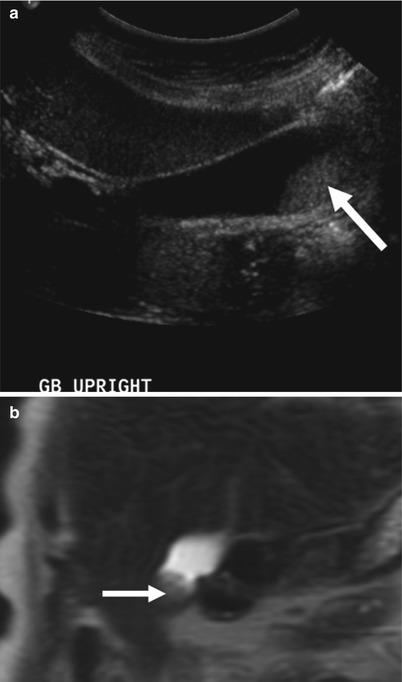
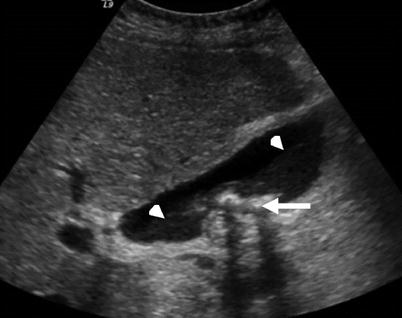

Fig. 6.16
Sludge. (a) This transverse US image in an upright patient demonstrates amorphous material (arrow) of low-level echoes within the dependent gallbladder. No posterior acoustic shadowing is seen. (b) This coronal T2-weighted MR image demonstrates a rounded filling defect of intermediate intensity within the gallbladder (arrow)

Fig. 6.17
Sludge and gallstones. This sagittal US image shows shadowing gallstones (arrow) and layering, nonshadowing sludge (arrowheads)
On CT, sludge appears as slightly hyperdense material layering within the gallbladder. When sludge forms a viscous mass, it is called tumefactive sludge and may mimic a polypoid tumor. Its mobility, changing shape over time, or lack of vascularity can differentiate sludge from a tumor.
Gallbladder Polyps
Lesions that project from the gallbladder wall into the gallbladder lumen are called gallbladder polyps and are found in 5 % of the population and are usually incidental. They include neoplasms such as adenomas or adenocarcinomas and nonneoplastic lesions such as cholesterol polyps (most common), inflammatory polyps, and hyperplastic polyps. Although usually asymptomatic, gallbladder polyps may occur when they are large or obstruct the cystic ducts. Many lesions identified as polyps on ultrasonograms prove to be small gallstones upon cholecystectomy [12]. Gallstones that are adherent to the gallbladder wall and do not show clear shadowing may mimic polyps (Fig. 6.8).
The overwhelming majority of polyps incidentally found are benign (Figs. 6.18 and 6.19); however, they rarely are malignant or premalignant neoplasms [13]. Because gallbladder cancer is usually incurable by the time it becomes symptomatic, it is imperative that potentially malignant polyps be treated by cholecystectomy.
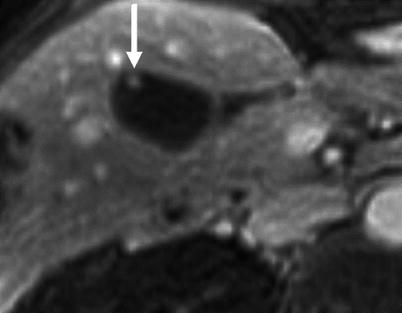
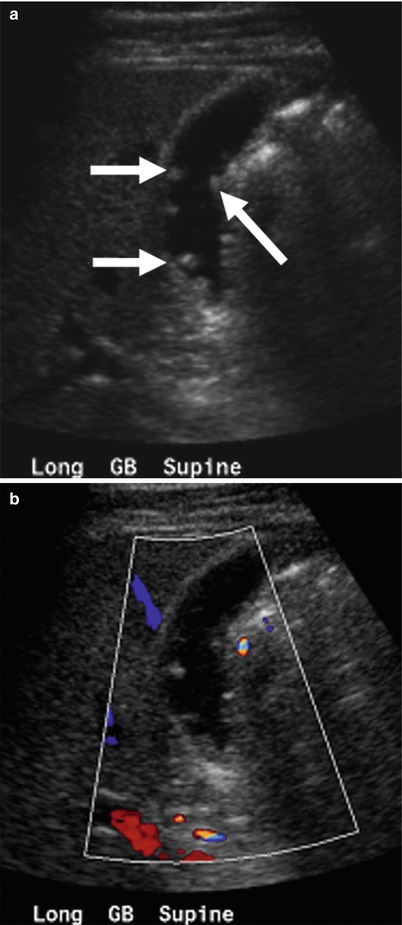

Fig. 6.18
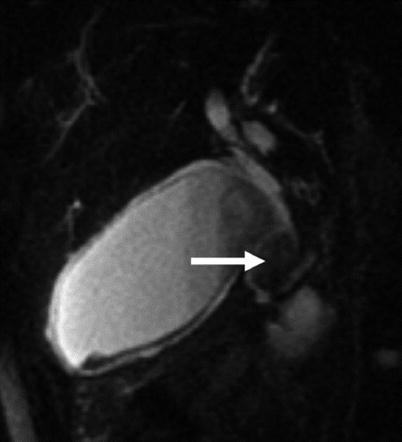
Benign gallbladder polyp. Axial postcontrast T1-weighted MR image. The polyp (arrow) measures less than 6 mm

Fig. 6.19
Multiple benign gallbladder polyps. (a) This longitudinal ultrasound image shows several small (<6 mm) intraluminal polypoid lesions (arrows) arising from the gallbladder wall. (b) This longitudinal US image with color Doppler shows lack of vascular flow within the polyps
Size greater than 10 mm is the best indicator of potential malignancy and these polyps should be treated with cholecystectomy (Fig. 6.20). In addition to size, the chance of malignancy is increased in polyps that are sessile, are single, have adjacent wall thickening, or are found in patients older than 50 [12].
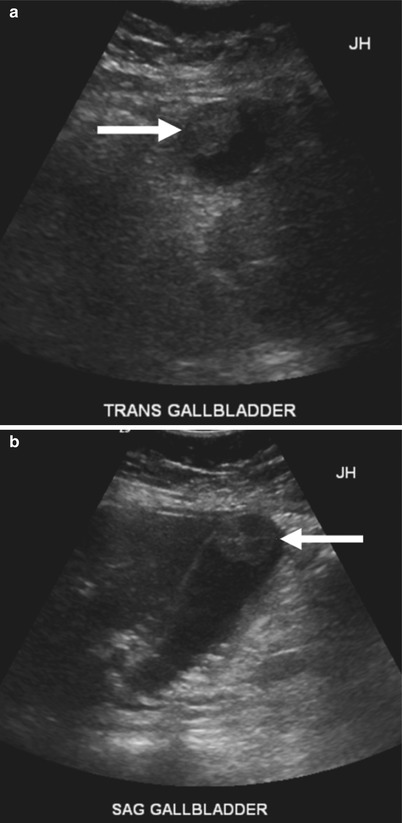

Fig. 6.20
Gallbladder adenocarcinoma. (a) Transverse and (b) longitudinal US images show a large sessile polypoid mass (arrows) at the gallbladder fundus. This was immobile on patient repositioning
Gallbladder adenomas are uncommon benign epithelial neoplasms considered to have malignant potential, similar to other gastrointestinal tumors that demonstrate an adenoma-carcinoma sequence. They are more commonly found in women and may be associated with Peutz-Jeghers or familial polyposis syndromes [14]. They are usually solitary (90 %) and may be sessile or pedunculated [15]
Cholesterolosis, an accumulation of lipid-laden macrophages in the lamina propria of the gallbladder, may result in the formation of excrescences called cholesterol polyps. Cholesterol polyps account for about half of all gallbladder polyps and arise from a defect in cholesterol metabolism. They can be single but are often multiple, are typically smaller than 10 mm, and enhance with IV contrast. They may appear to float in the gallbladder lumen on CT due to a thin stalk that may be imperceptible on CT. They have no malignant potential [15].
Inflammatory polyps are rare, arise from chronic inflammation, and are always associated with chronic cholecystitis.
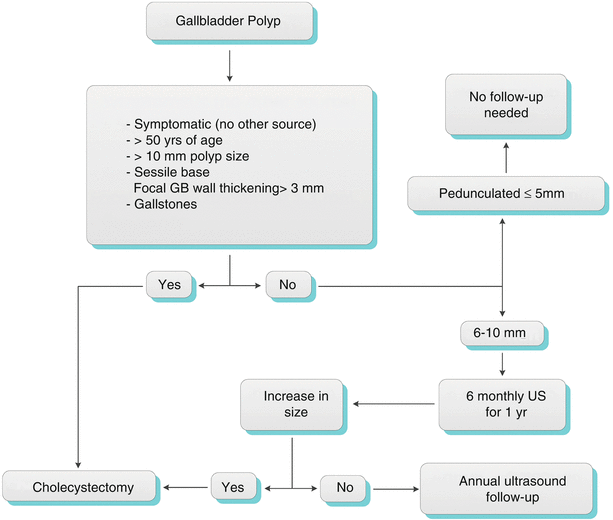
The optimal management or length of imaging follow-up for polyps smaller than 10 mm has not yet been defined; however, it is widely accepted that cholecystectomy is the treatment of choice for polyps larger than 10 mm based on the possibility of malignancy [16]. A management algorithm for gallbladder polyps is shown in Algorithm 6.6. Corwin et al. have recently proposed that no additional follow-up is necessary for incidentally detected gallbladder polyps measuring 6 mm or less, since the risk of malignancy or malignant transformation is extremely low.
On ultrasound, gallbladder polyps appear as single or multiple, immobile, nonshadowing lesions arising from the gallbladder wall. Ultrasonography is unable to reliably differentiate benign from malignant polyps [17]. However, multiplicity and polyps smaller than 10 mm are frequently cited as more suggestive of benignity. Gallbladder polyps are differentiated from gallstones by their lack of shadowing and mobility.
CT is significantly less sensitive for detecting polyps compared to ultrasound and it may not be possible to distinguish a polyp from a noncalcified gallstone on CT.
On MRI, polyps are low in signal on both T1- and T2-weighted imaging. Both benign and malignant polyps may show early enhancement; however, on 5-min delayed imaging, malignant polyps tend to demonstrate prolonged enhancement, whereas benign polyps show washout [18].
Gallbladder Polyps
Incidence: 5 %.
90 % benign, 10 % premalignant.
Most asymptomatic, discovered incidentally.
Features associated with malignancy: size >10 mm, focal adjacent wall thickening, sessile, single.
Imaging often cannot distinguish benign from malignant polyps and their management is primarily based on their size.
Gallbladder Metastases
Metastatic disease to the gallbladder is infrequent and usually occurs in the setting of widespread metastases. The most common malignancies to metastasize to the gallbladder include melanoma (Fig. 6.21), lung cancer, and renal cell carcinoma (Fig. 6.22).
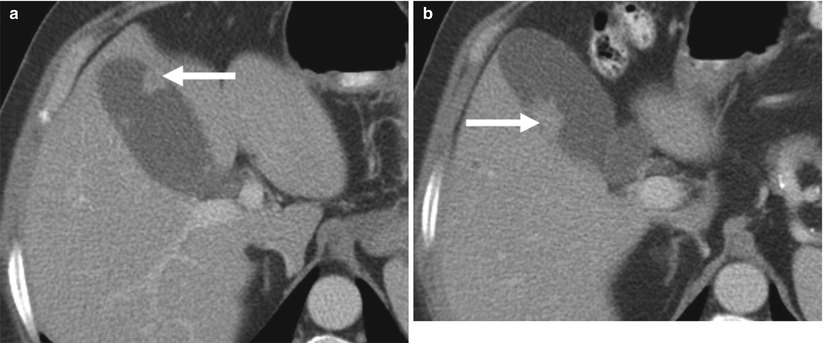
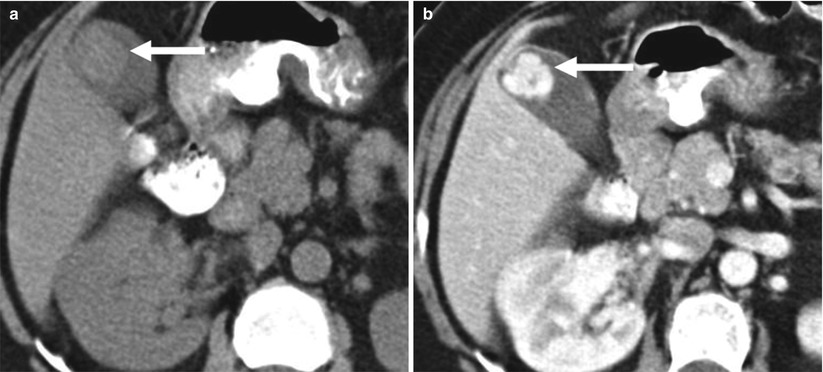

Fig. 6.21
Metastases to the gallbladder from melanoma. A 61-year-old male with metastatic melanoma. (a, b) These axial contrast-enhanced CT images show two polypoid intraluminal soft-tissues masses (arrow) arising from the gallbladder wall

Fig. 6.22
Metastasis to the gallbladder from renal cell carcinoma. (a) This axial noncontrast CT image shows an intraluminal rounded soft-tissue mass (arrow) arising from the gallbladder fundus. (b) The gallbladder mass (arrow) enhances avidly with IV contrast, similar to the patient’s primary renal tumor (not shown)
Diffuse Gallbladder Wall Thickening
The normal gallbladder wall measures 3 mm or less. Diffuse gallbladder wall thickening may be seen in many disease states. It can be caused by a wide range of processes including intrinsic gallbladder disease, either benign or malignant, and systemic disorders. It is important to narrow the differential diagnosis based on imaging and the clinical presentation to help guide management. This section will discuss the imaging characteristics that help differentiate the processes that cause diffuse gallbladder wall thickening, such as cholecystitis, adenomyomatosis, cancer, and systemic causes (Algorithm 6.7).
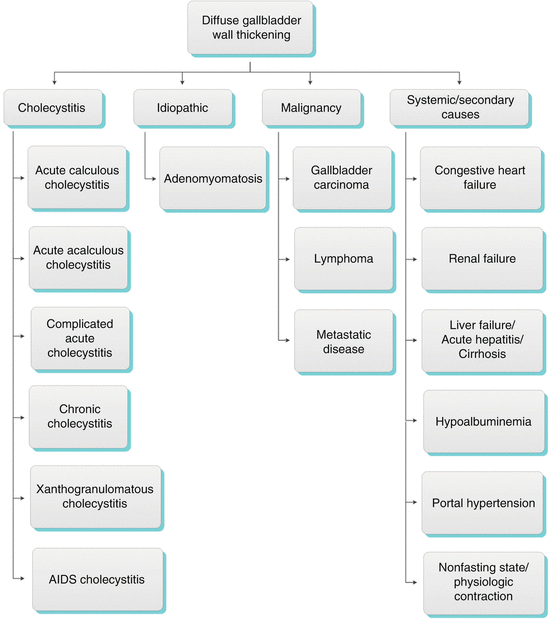

Algorithm 6.7 Chart demonstrating various etiologies for diffuse gallbladder wall thickening
Cholecystitis
Acute Calculous Cholecystitis
Acute calculous cholecystitis is the most frequent acute inflammatory condition of the gallbladder and one of the most common reasons for hospitalization for abdominal pain. Most cases (90–95 %) are caused by obstruction of the cystic duct or gallbladder neck by gallstones.
Patients with acute cholecystitis may present with persistent right upper quadrant pain, nausea, vomiting, fever, leukocytosis, and focal tenderness over the gallbladder. Physical examination often elicits a positive Murphy’s sign, defined as increased pain and inspiratory arrest on palpation of the region of the gallbladder fossa. The pain of acute cholecystitis is typically severe and constant and is often preceded by a history of a fatty meal.
If not treated, acute calculous cholecystitis may resolve over time or progress to complications, including gallbladder gangrene in up to 20 % of patients or perforation in 2 % of cases. Perforation may lead to a localized abscess or generalized peritonitis. Perforation into the small bowel may lead to a cholecystoenteric fistula, although this is more commonly due to chronic pressure from stones eroding the gallbladder wall.
When acute calculous cholecystitisis clinically suspected, ultrasonography is the preferred initial imaging modality (Algorithm 6.8), owing to its high sensitivity and specificity. Diffuse gallbladder wall thickening greater than 3 mm is often seen; however, it is not specific for cholecystitis (Figs. 6.23 and 6.24). Gallstones in a distended gallbladder with a positive sonographic Murphy’s sign (maximal tenderness over the sonographically localized gallbladder) are commonly seen. Pericholecystic fluid and wall hyperemia on Doppler imaging may be seen occasionally [19]. In patients clinically suspected of having acute cholecystitis, gallstones in conjunction with wall thickening or a positive sonographic Murphy’s sign have a high positive predictive value of 95 % and 92 %, respectively, for diagnosing acute cholecystitis [20].
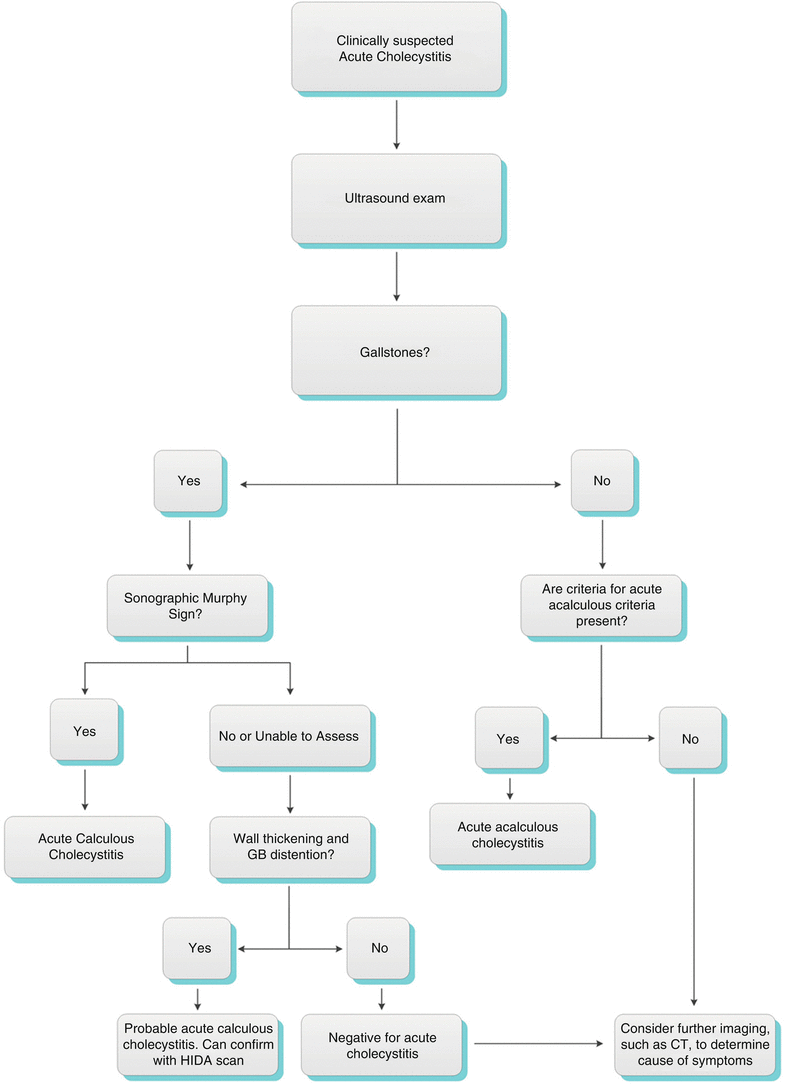

Algorithm 6.8 Algorithm for clinical management of suspected acute cholecystitis

Fig. 6.23
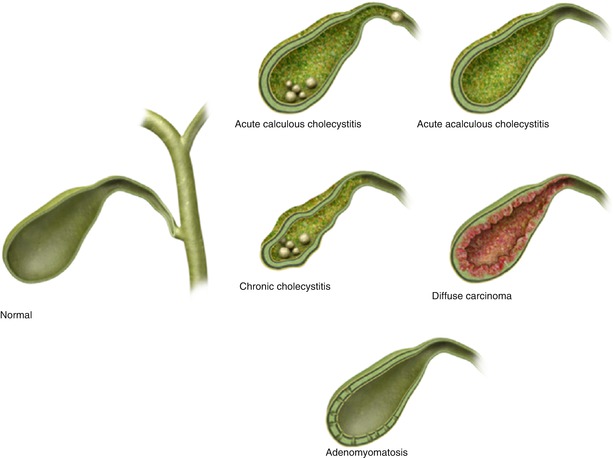
Some cause of diffuse gallbladder wall thickening

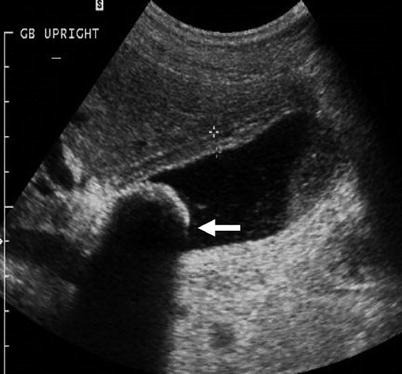
Fig. 6.24
Acute calculous cholecystitis. Longitudinal US image shows the distended gallbladder with wall thickening of 6 mm and a large impacted gallstone at the gallbladder neck (arrow). Layering gallbladder sludge is also seen
CT is less sensitive for detecting cholecystitis compared to US but may show a distended gallbladder with wall thickening (>3–5 mm), mural or mucosal hyperenhancement, pericholecystic inflammatory fat stranding or fluid, and gallstones (Figs. 6.25 and 6.26). Gallstones are frequently missed on CT when they are isodense to bile (cholesterol stones); CT is more sensitive for detecting calcified or gas-containing gallstones. The liver around the gallbladder fossa may demonstrate transient hyperenhancement on postcontrast arterial phase images owing to reactive hyperemia from acute inflammation [21]. This finding helps differentiate acute cholecystitis from chronic cholecystitis.
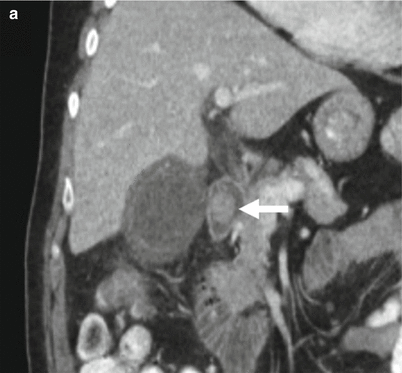
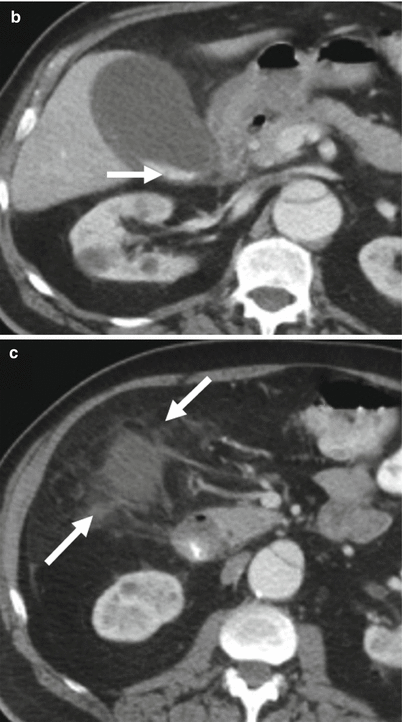
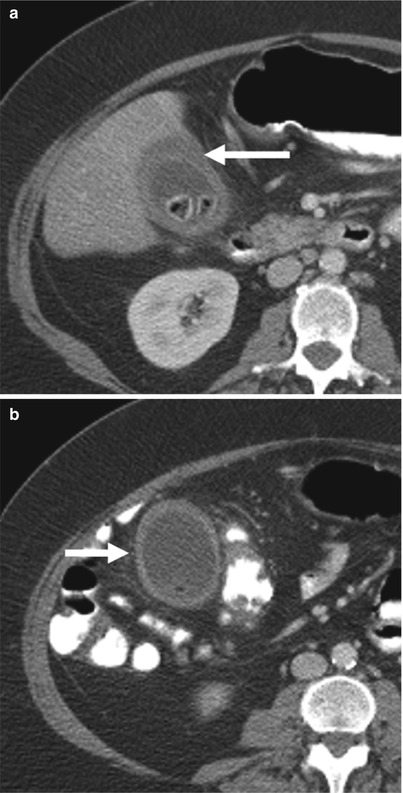


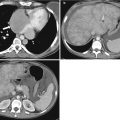
Fig. 6.25
Acute calculous cholecystitis on CT. (a) Coronal CT image. The gallbladder is distended and the gallbladder wall is thickened and there is a gallstone impacted in the gallbladder neck (arrow). (b) This axial contrast-enhanced CT image shows layering gallstones (arrow). (c) This axial contrast-enhanced CT image just below the gallbladder shows increased density in the pericholecystic fat consistent with adjacent inflammatory changes (arrows)

Fig. 6.26
Acute calculous cholecystitis. (a, b) Axial contrast-enhanced CT images demonstrate the distended gallbladder with diffuse wall thickening (arrow), gallstones, and pericholecystic inflammatory stranding (arrow)
Although acute cholecystitis is routinely diagnosed with US, in equivocal situations MRI may be helpful owing to its superior ability to identify calculi within the gallbladder neck or cystic duct compared with US [22]. In young or pregnant patients with equivocal findings of cholecystitis, MRI is preferred to CT owing to its lack of ionizing radiation [23]. On MRI, acute cholecystitis is typically characterized by a distended gallbladder with a thickened, hyperenhancing wall, gallstones, pericholecystic fluid, and pericholecystic fat signal intensity changes (Figs. 6.27 and 6.28) [23]. Less common but highly specific findings for acute cholecystitis include intraluminal membranes and wall irregularity, indicating a gangrenous or necrotic gallbladder, and pericholecystic abscess. The presence of gallbladder wall hyperenhancement and the presence of focal transient liver enhancement adjacent to the gallbladder are highly specific findings (92 % for both) with moderate sensitivity for differentiating acute cholecystitis from chronic cholecystitis on MRI [23]. On cholescintigraphy, biliary excretion of radioisotope in the absence of accumulation in the gallbladder is noted with acute cholecystitis.