Grade
0
1
2
3
4
Early
Symptom complex
No change
Frequency of urination or nocturia twice pretreatment habit/dysuria, urgency not requiring medication
Frequency of urination or nocturia that is less frequent than every hour. Dysuria urgency, bladder spasm requiring local anesthetic (e.g., pyridium)
Frequency with urgency and nocturia hourly or more frequently/dysuria, pelvis pain, or bladder spasm requiring regular, frequent narcotic/gross hematuria with/without clot passage
Hematuria requiring transfusion/acute bladder obstruction not secondary to clot passage, ulceration, or necrosis
Late
Symptom complex
None
Slight epithelial atrophy; minor telangeictasia (microscopic hematuria)
Moderate frequency; generalized telangiectasia; intermittent macroscopic hematuria
Severe frequency and dysuria; severe generalized telangiectasia (often with petechiae); frequent hematuria; reduction in bladder capacity (< 150 cc)
Necrosis/contracted bladder (capacity < 100 cc); severe hemorrhagic cystitis
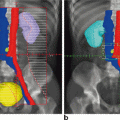
Late-onset radiation cystitis has a mean onset 35 months following completion of radiation therapy. However, it may occur after a latent period of > 20 years [22]. Therefore, radiation cystitis should be suspected in any patient with new onset hematuria who has a history of pelvic radiation regardless of time since therapy. Nonetheless, it is essential to evaluate for infection (with dipstick urinalysis and culture) or de novo bladder or upper urinary tract malignancy (with cystoscopy +/− biopsy and upper urinary tract imaging), as the risk of bladder cancer is increased following pelvic radiotherapy [23–25]. Radiation -induced hematuria can be mild or life-threatening, and it may be necessary to initially defer further diagnostic work up as the patient is stabilized.
Increased risk of late-onset radiation cystitis is related to the dose and type of radiation (e.g., combination external beam and brachytherapy) delivered. Diseases that may predispose a patient to poor healing and/or local tissue ischemia such as diabetes and vascular disease may also confer increased risk [16]. Chemotherapy , particularly cyclophosphamide, may also increase the risk of late and potentially debilitating bladder toxicity [26, 27].
Initial Management
As described, the severity of hematuria can range from mild to life-threatening. Therefore, initial management must be tailored to each individual patient depending on presentation. If necessary, aggressive fluid resuscitation and blood transfusion should be administered. A transurethral catheter designed for clot irrigation should be inserted into the bladder. If tolerated, the bladder should be manually irrigated at the bedside to remove all clots, with initiation of continuous bladder irrigation with normal saline, if necessary [19, 28]. If patient discomfort and/or organized clot prevent adequate bedside irrigation, rigid cystoscopy and clot evacuation in the operating room may be required [28]. Most patients will respond to initial conservative management (manual irrigation and continuous bladder irrigation), but refractory cases may require one or more additional interventions. It is critically important that the presence or absence of urinary tract malignancy is determined during evaluation and management.
Intravesical Agents
Aluminum Salts
Alum (aluminum ammonium sulfate or aluminum potassium sulfate) induces protein precipitation on cell surfaces and superficial interstitial spaces [28, 29]. Two case series reported cessation of bleeding in all patients treated with intravesical alum [30, 31], and another reported complete response in 10/15 (67 %) patients [32]. The authors from the latter series observed that alum tended to fail in more severe cases as the precipitant clotted, interfering with continuous irrigation [32].
Protocols for the use of alum have used 1 % alum solution (50 g of alum dissolved in 5 L sterile water or 400 g of potash of alum in 4 L hot sterile water to create a stock solution where 300 mL of stock is added to 3 L of normal saline) with irrigation at a rate of 250–300 mL/h if in sterile water or up to 30 L in 24 h if run with normal saline [28]. No anesthesia is required, and side effects associated with treatment are generally mild, consisting mainly of bladder spasms and pain. Nonetheless, severe aluminum toxicity, characterized by lethargy, confusion, seizures, metabolic acidosis, or elevated serum aluminum [33], has been reported [34], and the use of alum is cautioned in patients with renal impairment. Therapy should be stopped if symptoms of aluminum toxicity are encountered.
Formalin
Formalin is a tissue fixative that precipitates cellular proteins within the bladder mucosa [35]. Intravesical instillation results in edema, inflammation, and necrosis of all layers of the bladder [36, 37]. The concentration of formalin instilled varies in the literature, and it has been suggested that lower concentrations (1–4 % vs 10 %) can be efficacious while reducing the risks of complications [28]. When all causes of intractable hematuria are considered, success rates have been reported at 80 % or greater, even in cases of massive bleeding [35, 38–42].
Formalin must be instilled under spinal or general anesthesia. Choong et al. suggest starting with a concentration of 1–2 %, increasing concentration only if needed [28]. Cystography should be performed prior to instillation to exclude reflux, with Fogarty balloon occlusion of the ureteral orifices if reflux exists. Blood clots should be evacuated and bleeding vessels coagulated to limit systemic absorption. The skin is protected with Vaseline and the vagina packed to prevent leakage. The bladder is irrigated with the formalin solution under gravity at < 15 cm H2O, and contact time should be limited to 15 min or less.
Major toxicities associated with formalin treatment occur in about one-third of patients [43] and can include skin irritation, urinary incontinence, reflux, ureteral stricture, uretero-vesical junction obstruction, fistula, bladder rupture, permanent bladder and/or upper tract damage, sepsis, or even death [28]. Therefore, its use should be limited only to those cases in which more conservative measures have been exhausted or in patients unfit for more aggressive management. If formalin must be used, consideration should be given to modified techniques in which formalin-soaked pledgets are endoscopically placed on sites of bleeding, which has been reported to limit toxicity [44, 45].
Placental Extract
Topical placental extract has been successful in improving epithelialization of venous ulcers [46]. Based on its success in this setting, it was hypothesized that the high concentrations of growth and angiogenic factors in placental extract would promote healing of the bladder mucosa in radiation cystitis [17]. Mićić and Genbacev prospectively studied 35 women with radiation cystitis [47]. In the treatment arm, placental extract in saline was instilled in the bladder for 2 h, 3 days per week for 1 month and then weekly for 2 months. All 21 treated patients had relief of symptoms at 15 months with objective improvement in appearance of the bladder mucosa in 18/21 (86 %), which was a significant improvement in both outcomes compared to the 14 controls. Treatment-related morbidity was not reported, and there were no treatment-related deaths.
Aminocaproic Acid
Epsilon aminocaproic acid (EACA), used as an intravesical instillation, is thought to act by stabilizing the clotting process through its inhibition of fibrinolysis [48]. EACA instillation at a dose of 200 mg/L had a reported success of 93 % (13/14) in controlling bleeding in patients with intractable bleeding from radiation cystitis [49]. However, problems with Foley catheter obstruction and excessive clot formation may become problematic and require repeat trips to the operating room for clot evacuation. In general, we have not found EACA to be useful.
Hyaluronic Acid
Hyaluronic acid (HA) is a mucopolysaccharide found in connective and epithelial tissues that has been shown to inhibit immune complexes and neutrophil function while regulating fibroblast and endothelial cell proliferation [50]. Shao et al. randomized 36 patients with radiation-induced hemorrhagic cystitis to intravesical HA (40 mg for 20 min weekly for 1 month then monthly for 2 months) or HBOT (60 min, 7 days per week for at least 1 month) [51]. There were no significant differences found between the two groups in the proportion of patients with complete or partial response at 6, 12, and 18 months and no reported side effects with intravesical HA, suggesting a role for its consideration in refractory radiation-induced hematuria.
Silver Nitrate
Silver nitrate is an oxidizing agent that precipitates in water resulting in the release of free radicals [52]. The resulting tissue oxidation can serve to control bleeding. Intravesical silver nitrate irrigation has been associated with complications such as anuria [53] and reflux with extravasation and retroperitoneal inflammation [54]. Its use in the treatment radiation-induced hematuria is limited.
Prostaglandins
Prostaglandins are thought to increase cyclic adenosine monophosphate (cAMP) and sodium transport with resultant reduction in edema and inflammation [17]. Several case studies have reported success with intravesical prostaglandins either alone or in combination with hyperbaric oxygen for the treatment of radiation-induced hemorrhagic cystitis [55–57]. The durability of response is unknown, and though well tolerated, its use in cyclophosphamide-induced hematuria has been associated with a response in only 50 % of patients [58].
Liposomal Tacrolimus-Based Therapy
Tacrolimus is an immunosuppressive agent that inhibits interleukin-2-dependent T-cell activation via its inhibition of calcineurin phosphatase [59]. Systemic administration is associated with side effects such as nephrotoxicity and hypertension [60] that are not seen in topical administration [61]. Liposomes permit suspension of tacrolimus for intravesical delivery, and its use has been shown to effectively inhibit inflammatory cystitis in rats [62]. Assessment of its potential utility in humans will require further investigation.
Systemic Agents
Pentosan Polysulfate
Pentosan polysulfate is a sulfated polysaccharide that functions as a synthetic glycosaminoglycan, which is thought to reinforce the damaged mucosal lining of the bladder [63]. Success rates have been reported at 60–100 % with no reported toxicity [63–65]. Initial therapy consists of 100 mg of oral sodium pentosan polysulfate three times daily, and in many cases the dose can be reduced to once daily or stopped completely as hematuria improves [65].
Estrogens
Systemic estrogen has improved bleeding in advanced renal failure and may function to limit bleeding in radiation cystitis by decreasing capillary wall fragility [17, 19]. Liu et al. treated four patients with late hemorrhagic radiation cystitis with oral estrogen 5 mg daily (2/4 had received 1 mg/kg intravenously twice daily for 2 days prior to initiation of oral therapy) [66]. Three out of four patients had resolution of hematuria at 15 months, and no adverse effects were reported.
WF10
WF10 is a 1:10 dilution of tetrachlorodecaoxide that is delivered intravenously. It is thought to improve tissue repair through modification of macrophage activity via stimulation of phagocytosis and cellular defense systems. Down regulation of antigen presentation ultimately leads to reduced chronic inflammation and improved healing [67]. Veerasarn and colleagues conducted two studies evaluating the efficacy of intravenous WF10 in refractory radiation-induced hematuria. In the first study, 100 women were randomized to standard therapy (consisting of antibiotics, irrigations, and antispasmodics) or standard therapy plus WF10 at a dose of 0.5 mL/kg for 5 days every 2 weeks for a total of two cycles [67]. There was no significant difference in complete resolution between the treatment group and control group at 7 weeks (74 % vs 64 %, P = 0.28), however, the WF10 group had significantly lower use of antibiotics and antispasmodics. Furthermore, Kaplan–Meier analysis found that recurrence of objective hematuria occurred significantly later in the treatment arm. A second study prospectively evaluated 16 patients with grade 2–3 radiation-induced hematuria [68]. Fourteen of 16 (88 %) improved to grade 0–1 toxicity upon completion of therapy, with 4 (28 %) having recurrent grade 2 hematuria at a mean follow-up of 51 months. No serious treatment effects were attributable to the drug in either study.
Pentoxifylline
Pentoxifylline is an orally administered drug used to treat vascular occlusive disorders. Pentoxifylline increases prostacyclin release, which results in increased red cell deformity and improved flow through capillaries. Dion et al. reported complete healing of 13/15 (87 %) radiation-induced necrotic ulcers at the time of analysis in patients treated with pentoxifylline, with an average time course of healing of 9 months [69]. In one case of chronically nonhealing suburethral ulcer, pain resolved after 8 weeks of pentoxifylline 400 mg three times daily, and the ulcer healed completely at 10 weeks, suggesting a potential role for this agent in the treatment of chronic radiation-induced ulceration of the genitourinary tract. Pentoxifylline is generally well-tolerated, with the most common side effect being gastrointestinal-upset [70].
Endoscopic or Percutaneous Management
Cystoscopy and Fulguration
When intravesical and/or systemic agents fail to control bleeding from radiation cystitis, various endoscopic and/or percutaneous management strategies can be performed. Cystoscopy, clot evacuation, and fulguration of bleeding sites using electrocautery or various other energy sources is a reasonable first step when conservative measures fail. Kaushik et al. reported a novel treatment strategy for refractory radiation-induced hemorrhagic cystitis using a 980 nm diode laser [71]. The 980 nm wavelength is ideal as it is highly absorbed by both hemoglobin and water resulting in improved hemostasis [72]. The authors reported their experience using the 980 nm diode laser in four patients with refractory radiation-induced hemorrhagic cystitis who failed conservative therapy and standard cystoscopy and electrocautery fulguration. All four patients remained hematuria-free postprocedure with mean follow-up 11 months (range 3–17). Additionally, the neodymium-doped yttrium aluminum garnet (Nd:YAG) laser has been shown to be safe and effective for control of bleeding from radiation cystitis, but due to the increased depth of penetration, care must be taken to avoid bladder perforation [73]. Zhu et al. utilized the Greenlight TM potassium-titanyl-phosphate (KTP) laser in 10 patients with refractory hematuria from radiation cystitis [74]. At a mean follow-up of 17 months (range 6–36 months), 1 patient had recurrence of significant hematuria 7 months after initial laser fulguration.
Botulinum Toxin A
Botulinum toxin A is FDA approved for the treatment of neurogenic and non-neurogenic overactive bladder in adults who have failed treatment with anticholinergic medications. Chuang and colleagues injected 200 units of botulinum toxin A into the bladder of six patients with refractory radiation cystitis [75]. Patients were followed with clinic visits and 3-day voiding diaries. One patient had no subjective improvement, three had moderate improvement, and two had significant improvement at 1-week follow-up with durability of results at a 6-month follow-up visit. At 2-month follow-up, 3-day voiding diaries revealed a mean increase in bladder capacity from 105 to 250 mL and a mean decrease in urinary frequency from 14 to 11 episodes per day. No complications were reported and no patients developed urinary retention. Botulinum toxin A bladder injections appear to be a reasonable option for patients with refractory urinary storage symptoms related to radiation cystitis, although its use in this context is off-label.
Orgotein
Orgotein is a copper–zinc superoxide dismutase (SOD) that is found in the cytoplasm of all eukaryotic cells and functions to convert superoxide radicals into oxygen and hydrogen peroxide. Superoxide radicals are formed during the acute phase inflammatory process during radiation therapy and can induce tissue damage. It is hypothesized that orgotein could function at the extracellular level and inhibit the acute phase inflammatory processes mediated by free radicals thereby reducing the risk of late side effects from radiation therapy [76]. Marberger et al. initially reported a retrospective series of 30 patients with late radiation cystitis treated with orgotein injections into the bladder wall and noted clinical and cystoscopic improvement in 25 patients [77]. Other randomized prospective studies have reported a benefit of intramuscular orgotein injections administered at the time of radiation therapy to prevent early and late radiation cystitis [78, 76]. While the evidence is fairly strong for the use of orgotein to prevent early and late radiation cystitis, further studies are needed to determine the role of orgotein bladder injections in treating patients with late radiation cystitis.
Percutaneous Nephrostomy Tubes
Insertion of bilateral percutaneous nephrostomy tubes is a viable minimally invasive option in patients with refractory radiation-induced hemorrhagic cystitis who have failed other bladder-directed therapies. It is thought that diverting urine away from the bladder prevents its over-distention and limits the action of endogenous urokinase [79]. Sneiders and Pryor reported success with this strategy in two patients in whom bleeding gradually ceased during a 1-week period [79]. Both patients were alive and voiding spontaneously at 6 months follow-up. Additionally, Zagoria et al. treated six patients with refractory hemorrhagic cystitis with bilateral percutaneous nephrostomy tubes noting favorable results in five of the six patients [80]. There are no data on long-term follow-up of these patients, and while percutaneous nephrostomy tube insertion may ameliorate bleeding, questions remain regarding its long-term efficacy.
Embolization of Bladder Vessels
Embolization of the arteries to the bladder has been reported as a useful adjunct for the management of radiation-induced hemorrhagic cystitis. Potential drawbacks of embolization include the need for skilled interventional radiologists, the extensive network of collateral circulation of the bladder, and the potential for postembolization gluteal pain, claudication, and tissue necrosis. However, De Berardinis et al. reported success using super-selective embolization of the bladder arteries in a patient with refractory hemorrhagic cystitis following radiation therapy for invasive bladder cancer [81]. The super-selective embolization technique avoids embolization of the gluteal circulation and permits the utilization of adaptable embospheres, which offer better occlusion of the vessels. Despite these purported advantages, long-term durability remains questionable. Liguori et al. reported long-term results of selective embolization of the internal iliac arteries in 44 patients with intractable gross hematuria secondary to advanced pelvic malignancies [82]. Despite an initial success rate of 82 %, at a mean follow-up of 10.5 months after embolization rebleeding had occurred in all but 43 % of patients. Nonetheless, embolization of the arteries to the bladder remains a viable treatment option in patients unfit for more aggressive surgical management.
Hyperbaric Oxygen Therapy
HBOT for the management of radiation-induced hemorrhagic cystitis was first reported by Weiss and researchers in 1985 [83]. Proposed mechanisms of action of HBOT include angiogenesis and capillary regrowth stimulated by large plasma to tissue oxygen gradients, mediation of fibroblastic stromal process, and mobilization of stem cells. Patients typically undergo 30–40 treatment sessions with each session consisting of 2 h of pressurization at 1.5–2.5 absolute atmospheric pressure. During each 2-h session, 90 min are spent breathing 100 % oxygen at maximum pressure. Advantages of HBOT include its noninvasiveness and its favorable safety profile, whereas its cost and lack of widespread availability are certain drawbacks. Multiple single-centers have reported success with HBOT for the management of refractory radiation-induced hemorrhagic cystitis (Table 14.2) [51, 84–93]. Furthermore, HBOT appears safe and effective in children with hemorrhagic cystitis [94].
Table 14.2
Studies assessing hyperbaric oxygen therapy for radiation cystitis
Study | Number of patients | Number of treatments’ mean ± SD (range) | Length of treatment session (min) | Response rate (%) | Follow-up duration |
|---|---|---|---|---|---|
Hampson et al. [84] | 44 | 42 ± 9 (34–60) | 120 | 89 | No follow-up after HBOT |
Nakada et al. [85] | 38 | 62 ± 12 (39–92) | 90 | 74a | 11.6 ± 3.7 years |
Oliai et al. [86] | 19 | 29.8 (10–40) | 90–120 | 81 | 39 months (7–70) |
Shao et al. [51] | 20 | 30 | 60 | 75 | 18 months |
Yoshida et al. [87] | 8 | 19 (10–42) | 90 | 75 | 15.5 months (2–31) |
Vilar et al. [88] | 38 | 31.2 (10–48) | 90 | 89 | 56 months (4–72) |
Mohamad Al-Ali et al. [89] | 10 | 30 | 60 | 20 | 18 months (12–72) |
Chong et al. [90] | 60 | 33 (9–63) | 90 | 80 | 12 months |
Corman et al. [91] | 57 | 33 (9–68) | 90 | 86 | 10–120 months |
Del Pizzo et al. [92]
Stay updated, free articles. Join our Telegram channel
Full access? Get Clinical Tree
 Get Clinical Tree app for offline access
Get Clinical Tree app for offline access

|