9 Venous thromboembolism (VTE) is a spectrum of disease that encompasses both deep venous thrombosis (DVT) and pulmonary embolism (PE). It is a serious and often underrecognized condition in critically ill patients that can lead to significant morbidity and mortality. PE remains one of the leading causes of unexpected death in hospitalized patients.1,2 In the intensive care unit (ICU), the Virchow triad of “stasis, endothelial injury, and hypercoagulability” is a frequent occurrence, with most critically ill patients having one or more recognizable risk factors for VTE. Immobilization, mechanical ventilation, paralysis, sedation, and central venous catheters all increase the risk for DVT.3,4 The embolic risk for DVT is related to its location in the venous system. Ninety percent of cases of acute PE are due to emboli emanating from clots in the proximal veins of the lower extremities. The significance of upper extremity deep venous thrombosis (UEDVT) was underestimated for many years. Recently, this perception has changed, and it is now recognized that proximal UEDVT accounts for 5% to 10% of cases of VTE.3–6 The use of chronic venous access catheters such as peripherally inserted central venous and various tunneled catheters has greatly increased, and these catheters have been associated with an increased incidence of UEDVT. In its latest guidelines for antithrombotic therapy and prevention of thrombosis, the American College of Chest Physicians for the first time recommended treatment of UEDVT involving the axillary or more proximal veins. Classic symptoms of DVT include swelling, pain, and erythema of the involved extremity. However, the signs and symptoms of DVT in critically ill patients are often unreliable, which makes diagnosis difficult. The true incidence and prevalence of acute DVT in critically ill patients are not known. Various studies have reported incidences ranging widely from 4% to 60% as a result of differences in the patient population, methods of detection, and use of surveillance programs.7–9 Because of rapid growth in the availability of portable ultrasound units, point-of-care ultrasonography performed at the bedside by critical care physicians is gaining increased popularity. A multicenter, retrospective review compared 128 bedside intensivist-performed compression ultrasound (IP-CUS) studies with a formal vascular study (FVS) performed by ultrasound technicians and interpreted by radiologists.10 All fellows and attending physicians performing IP-CUS had received formal training at a 3-day critical care ultrasonography course. When compared with the companion FVS study ordered immediately after completion of the IP-CUS study, IP-CUS studies had a sensitivity and specificity of 86% and 96%, respectively, for ruling in DVT. The median time between ordering the test and availability of the result of an FVS was 13.8 hours. The axillary vein is a deep vein of the arm that branches distally into the paired brachial veins. It runs through the axilla to the outer border of the first rib and is joined by the cephalic vein medially close to its termination. The confluence of the axillary vein and the cephalic vein forms the subclavian vein (SCV). The SCV runs from the outer border of the first rib to the sternal head of the clavicle, where it is joined by the internal jugular (IJ) vein, and together they form the brachiocephalic vein. The brachiocephalic vein drains into the superior vena cava. The IJ extends from the jugular foramen in the base of the skull to its confluence with the SCV (Figure 9-1).11 The two main veins of the superficial venous system are the great and small saphenous veins. The small saphenous vein runs along the lateral aspect of the calf and drains into the deep venous system at the level of the popliteal vein. The great saphenous vein (GSV) runs up from the ankle along the medial aspect of the leg and, in the proximal part of thigh, traverses the fossa ovalis and drains into the common femoral vein (CFV). The external iliac vein originates from the inferior vena cava and exits the pelvis deep to the inguinal ligament to become the CFV. The CFV is then joined on its medial aspect by the GSV. Approximately 2 cm below this point the CFV divides into the deep femoral vein (DFV) and the superficial femoral vein (SFV). The DFV can be tracked for only a short distance before it disappears into the deeper tissue away from the acoustic window. It is important to note that the SFV is part of the deep venous system and is also called the “femoral vein” to avoid confusion. The SFV travels down the anteromedial aspect of the leg to the adductor canal and then courses posteriorly into the popliteal fossa to become the popliteal vein. The popliteal vein then trifurcates into the anterior tibial, peroneal, and posterior tibial veins in the proximal part of the calf (Figure 9-2). Several ultrasound techniques can be used when assessing a vessel for the presence of a clot. This method adds color Doppler to the 2D analysis. The energy of the returning sound waves is assigned a color. By convention, flow toward the transducer probe appears as red and flow away from the probe is visualized as blue. This is superimposed on the 2D image to allow visualization of anatomy and flow simultaneously (see Chapters 1 and 8). This method adds spectral analysis to the 2D and color Doppler analysis (see Chapter 1). In this mode, flow velocities are displayed graphically, with time on the x-axis and velocity on the y-axis. Traditionally, an FVS included all of the aforementioned techniques. However, studies have shown that CUS with color and pulsed wave Doppler does not increase the accuracy of the examination over CUS alone.12
Ultrasonography for deep venous thrombosis
Background
Anatomy
Upper extremity venous sonographic anatomy
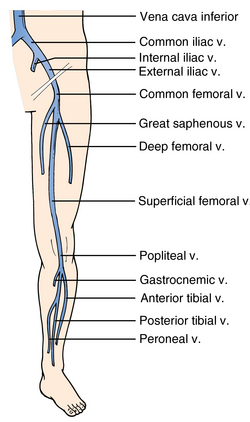
Lower extremity venous sonographic anatomy
Basic ultrasound techniques
Duplex ultrasound
Triplex ultrasound
![]()
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


Ultrasonography for deep venous thrombosis