, Valery Kornienko2 and Igor Pronin2
(1)
N.N. Blockhin Russian Cancer Research Center, Moscow, Russia
(2)
N.N. Burdenko National Scientific and Practical Center for Neurosurgery, Moscow, Russia
Malignant tumors of the female genital organs occupy a special place in the clinical oncology, since they are the most common malignancies in women. Of the 12.7 million of new cases with various forms of cancer reported each year in the world, almost 1 million account for gynecologic tumors. In Russia, in 2010, the number of newly diagnosed female genital tumors was 47 700 thousand, which was 17% of all malignant tumors (Jemal et al. 2011).
Cervical cancer is one of the most common malignancies, ranking seventh among all malignant cancers and fifth in the structure of cancer incidence in women in the Russian Federation, after breast cancer and gastrointestinal cancer. In 2012 more than 15.3 thousand cervical cancer patients and 7.37 thousand deaths were reported in Russia. According to Davydov and Axel (2014), during the period from 2007 to 2012, an increase in the absolute number of cases of cervical cancer was 11.2%, defining the fourth place by the increase rate among malignant tumors. In the structure of malignant neoplasms in the female population of Russia, the proportion of cervical cancer decreased from 7.0% in 1989 to 5.3% in 2012.
In developed countries, standardized incidence rates (9.0 per 100,000) are two times lower than in developing countries (17.8 per 100,000), accounting for 78% of cases of cervical cancer, while its proportion is 15% of all malignancies in women (4.4% in developed countries). Disturbing is an increase in the incidence of cervical cancer in Russia from 12.5 per 100,000 of female population in 2007 to 13.9 per 100,000 in 2012. The maximum age-standardized incidence rates of cervical cancer were reported in the age group of 50–64 years old—31–32 per 100,000. Cervical cancer is the leading cause of death among all malignant tumors in women aged 15–40 years old, reaching 19.5%. In the age category of 40–54 years, cervical cancer moves to second place, accounting for 9.7%.
In developed countries, the incidence of uterine cancer (UC) (12.9–100,000 of female population) was 2.2 times higher than in developing countries (5.9 per 100,000). In the structure of cancer incidence among the female population in the Russian Federation (2012), UC ranked second (7.5%) after breast cancer (20.7%). During the period from 2007 to 2012, an increase in the absolute number of cases was 8.7%. The incidence of UC increased in all age groups, starting from 25 years, and reached the maximum values (91.9—100,000) for the age group of 60–64 years (Axel 2012).
The average age of patients with gynecologic cancer in Russia decreased by 6 years—from 58 years in 1989 to 52 in 2010. An important factor is insufficient mass implementation of screening programs in Russia as compared with Western European countries, allowing to diagnose precancerous conditions and early forms of cancer.
Survival rates vary: good predictions are noted in the USA, 72%; in European countries, 60%; and in developing countries, 48%. The lowest survival rate was registered in Eastern Europe.
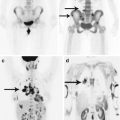
According to literature, cerebral metastases of cervical cancer , uterine cancer, and ovarian cancer are, on average, 0.5–1.2%, 0.6%, and 0.49–2.2%, respectively (Aalders et al. 1984; Ikeda and Yamada 1998; Chura et al. 2007; Ogava 2008; Setoodeh et al. 2012; Sierra et al. 2015). Spinal metastases of cervical and ovarian cancer are detected in 6% and 0.1–0.12% of cases, respectively (Matsuyama et al. 1989; Tiwari 2007).
The time interval from the detection of primary cancer to the detection of metastatic brain lesions of cervical cancer can reach up to 8 years. According to Kim et al. (2015), who analyzed a group of patients with cerebral metastases of malignant gynecologic tumors (n = 61) from 2002 to 2012, the average interval for cervical, uterine, and ovarian cancer was found to be 33.1 months, 27.8 months, and 21.6 months, respectively. The survival rates for patients with brain metastases of cervical, uterine, and ovarian cancer were 8.8 months, 23.3 months, and 14.1 months, respectively.
Although cerebral metastases are rare, according to Martinez-Manas et al. (1998), well-differentiated endometrial carcinoma with signs of vascular invasion can metastasize to the brain even before clinical manifestations of the primary tumor occur. According to Piura and Piura (2015), cerebral metastasis of endometrial carcinoma is so rare that authors found only 115 cases in the analysis of 35 studies.
In our cases, UC metastases in the brain were detected in 7% of cases, which greatly exceeds the data from literature.
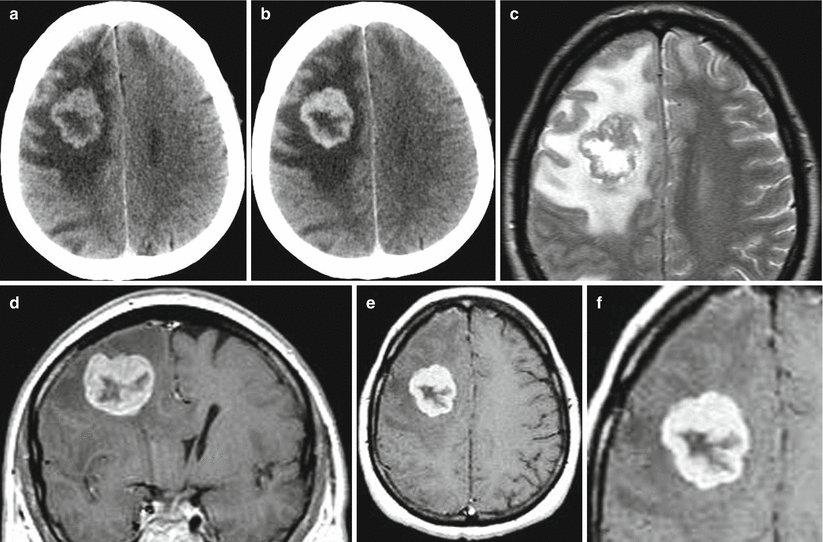
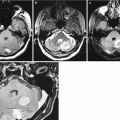
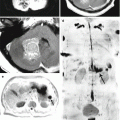
On CT and MRI, cerebral metastases of UC manifest both as single and multiple tumors. Lesions are often solid, but we often diagnosed metastases with a solid-cystic structure. Almost always an expressed area with a perifocal edema is visualized. Accumulation of the contrast agent by the solid part of the metastasis significantly increases its density on the periphery; therefore, a “target” type of accumulation is often observed.
Although the vast majority of cases of cerebral metastases have a characteristic perifocal edema, we also diagnosed large lesions without any perifocal edema in our studies. These lesions had a dense solid structure with irregular contours.
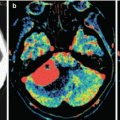
The solid part of UC metastases has almost similar low values of cerebral blood volume, CBV and CBF, such as metastatic breast cancer. UC metastases have the lowest MTT values = 5.36 ± 0.74 (s), which indicates a rapid blood flow through their parenchyma in comparison with other cerebral metastases.