Case presentation
A 13-year-old male presents with acute onset of mental status changes. He was found in his room, lying facedown. Emergency medical services was called. On their arrival, the patient was conversing but appeared sleepy; he was responsive to questions but confused. He was attempting to speak but was able to manage only a few words.
Once in the Emergency Department, the patient was able to speak more easily and seemed to be more at his baseline. He reports having a left frontal headache prior to “passing out.” He denies illegal substance use. He has no history of prior episodes of “passing out” and is otherwise healthy. There is no family history of sudden cardiac death but there is a cousin with epilepsy.
He continues to complain of a left frontal headache. He does remember standing up and then “the lights went out.” His vital signs reveal no fever, a heart rate of 90 beats per minute, a respiratory rate of 18 breaths per minute, and a blood pressure of 112/63 mm Hg. He has a normal physical examination other than a large frontal hematoma with tenderness to palpation.
The patient states that he has been having left frontal headaches for the past 2 weeks, which he describes as “severe sometimes.” He has had some morning nausea and did have nonbilious/nonbloody morning emesis 2 days ago.
Imaging considerations
There are several imaging options available to the clinician when a pediatric patient presents with acute mental status changes. The initial imaging modality of choice may be dependent on the suspected diagnosis and institutional resources.
Computed tomography (CT)
Acute mental status changes in pediatric patients have a broad differential diagnosis; when an intracranial etiology is suspected, such as masses or hemorrhage, CT is an excellent first-line imaging modality. Widely available and rapid, this modality does not require sedation. In addition to hemorrhage and intracranial mass, CT can detect calcifications. If a neurovascular cause is suspected, CT angiography can provide important information about the size, location, and drainage of an arteriovenous malformation. If emergent surgical intervention is required, this modality can provide needed information for surgical planning more rapidly than other modalities.
Magnetic resonance imaging (MRI)
MRI (with and without contrast) and magnetic resonance angiography (MRA) are important imaging modalities that can be utilized when a neurovascular cause of a patient’s presenting symptoms is suspected clinically or by CT. MRI is valuable when evaluating arteriovenous malformations for several reasons: the localization of the malformation; comparison of contrast, non—contrast, and gradient echo sequences helps to rule out other hemorrhagic lesions; MRA helps delineate the vascular anatomy of the lesion; and it can be used intraoperatively to guide surgical procedures. The main obstacle to more immediate utilization of this modality is the time needed to complete the study and the common need for sedation in pediatric patients.
Cerebral angiography
Conventional cerebral angiography is the gold standard for diagnosing arteriovenous malformations, providing characteristics of the malformation, including location, size, associated vascular lesions, draining veins, and other vital information. , Conventional angiography also has the advantage of detecting small malformations that may not be seen on MRI or MRA.
There are instances of malformations being radiographically occult; usually, these are located in the region of the middle cerebral artery. Pediatric patients who present with a spontaneous intraparenchymal hemorrhage and have negative imaging studies may indeed have an arteriovenous malformation, as the resulting hematoma can compress the malformation; in this instance, delayed imaging is indicated, which can reveal the malformation as the clot resolves.
Imaging findings
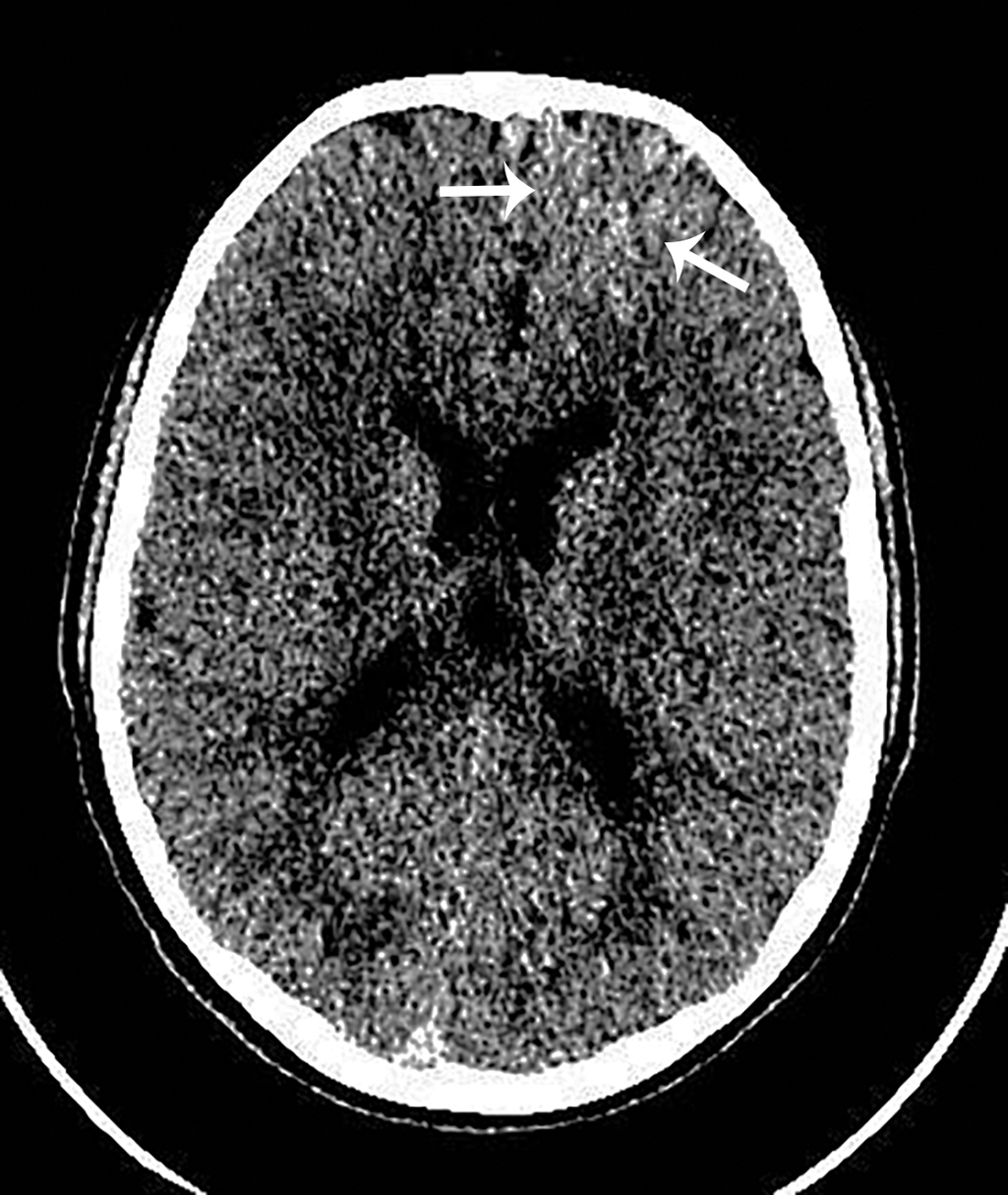
The patient was observed in the Emergency Department while blood work and an electrocardiogram were obtained. With the history of recent headaches and nausea, as well as the apparent, sudden onset of the patient’s collapse, the decision was made to obtain non—contrast CT of the brain. A selected image from that study is provided here. There is a subtle, ill-defined, increased attenuation in the anterior left frontal lobe deep white matter and evidence of prominent vascular structures around the periphery of the anterior left frontal lobe; there is no calcification or acute hemorrhage in the region and the bones are normal ( Fig. 33.1 ).
Case conclusion
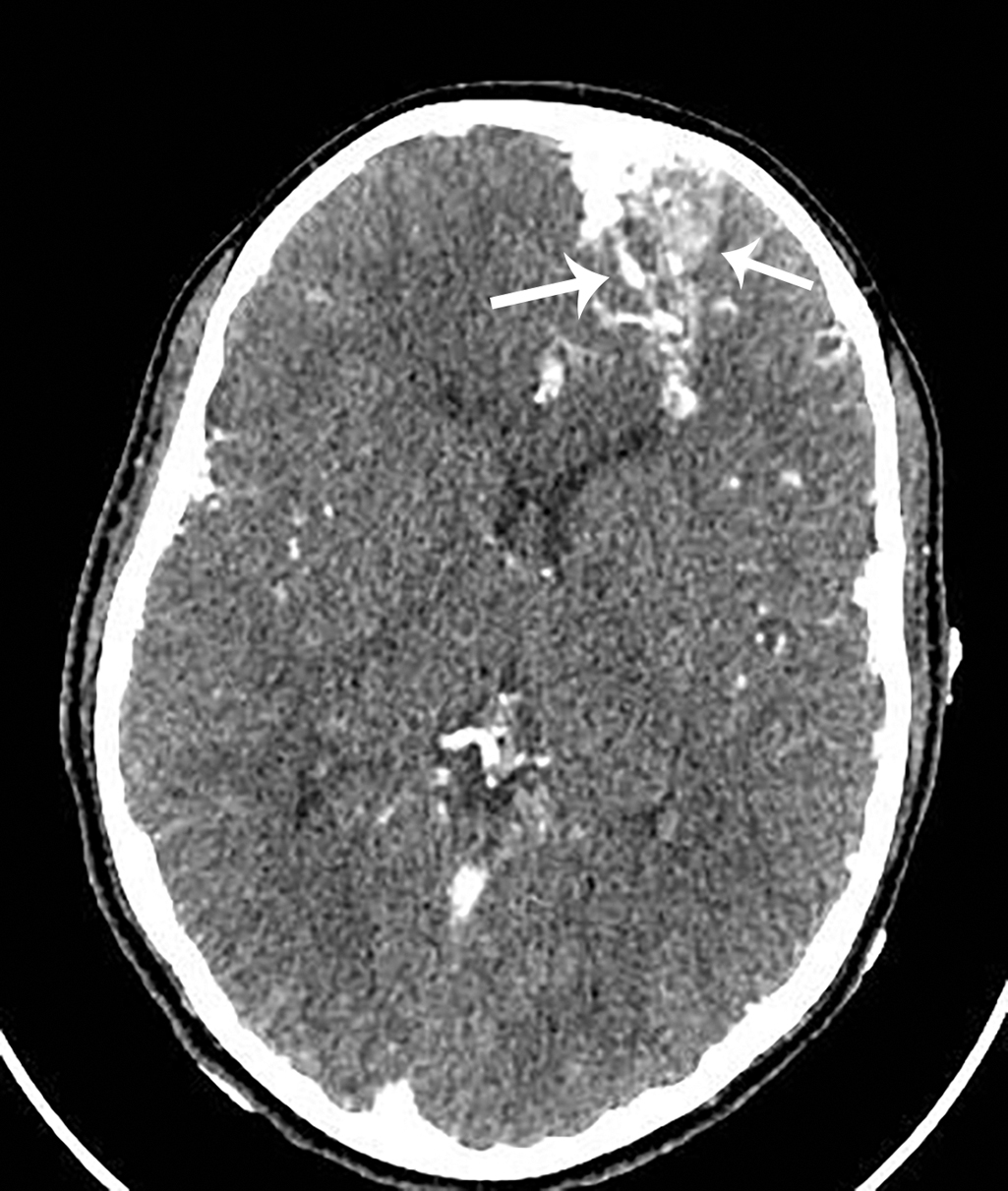
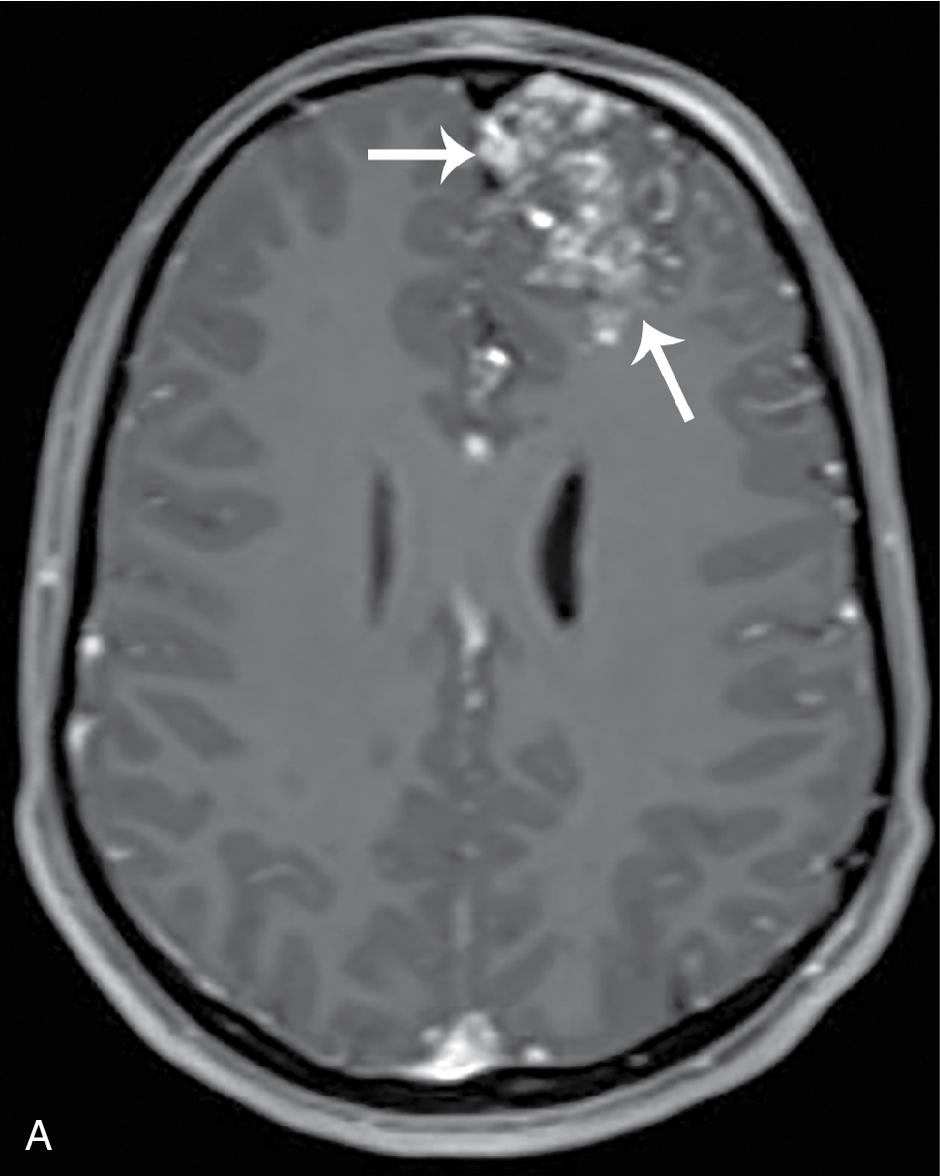
The patient was admitted with Pediatric Neurosurgical consultation. CT angiography was obtained, and a selected image from that study is provided here. This study demonstrated an ill-defined area of high attenuation in the left frontal lobe ( Fig. 33.2 ). MRI was also obtained, demonstrating multiple tightly packed vessels with surrounding enlarged feeding arteries ( Fig. 33.3 A, B) and a vascular nidus with enlarged left anterior and middle cerebral feeding arteries and multiple enlarged draining cortical veins ( Fig. 33.4 ). These findings are consistent with a vascular malformation. The patient had endovascular embolization followed by surgical resection and did well.

Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree