41 Osteomyelitis
Osteomyelitides can be classified according to pathogens, sites of entry, and the clinical course of the disease. Radiographic morphology only rarely indicates the pathologic organism. The clinical findings are required to identify a “moth-eaten” or permeative osteolysis as osteomyelitis. The exposure of the hand to traumatic inoculation of pathogens and the possibility of infection spreading through the tendon sheaths, fasciae, and lymphatic vessels explains the frequency of secondary osteomyelitides of the hand. In contrast, hematogenous osteomyelitis is rare. Radiographs provide the imaging basis for the detection of inflammatory lesions. MRI is the method of choice to determine the extent of inflammation in the bone marrow and the surrounding soft tissue. CT is useful to identify a sequestrum, granulation tissue, involucrum and an intraosseous abscess in chronic osteomyelitis.
Introduction
Infections of the soft tissues of the hand require a precise diagnosis and immediate therapeutic decision to prevent spread along predefined anatomic pathways. Osteomyelitis of the hand is usually the result of a soft-tissue infection or, less often, hematogenous dissemination. Confirmation of osseous infection is important for planning surgical intervention.
Diagnostic Imaging
Radiography
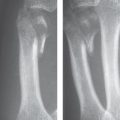
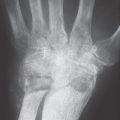
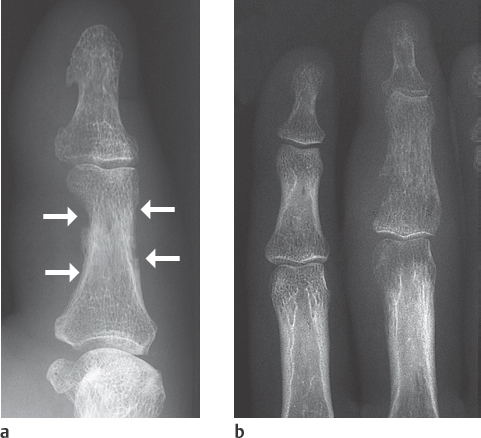
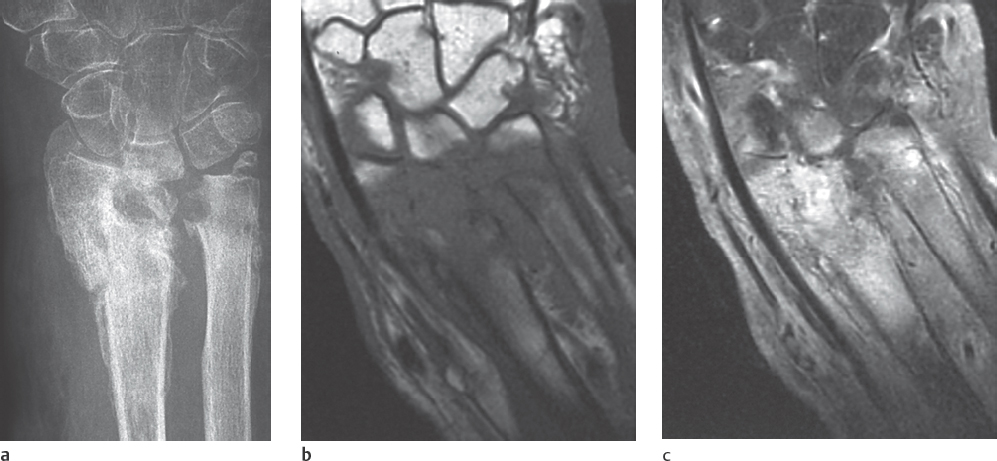
Acute courses of osteomyelitis lead to osteolytic destruction. The radiographic signs include initially focal decalcification and periosteal reaction (Fig. 41.1a). Inflammatory focal osteolyses appear later (Fig. 41.1b), and osteosclerosis appearsin chronic stages ( Table 41.1 ).
The term “early signs” should not conceal the fact that 8–10 days usually pass before osteomyelitis can be identified in radiographs. Conventional tomography offers hardly any advantages in diagnosis of inflammation of the hand in comparison to survey views (or the use of the magnification technique if necessary).
Computed Tomography
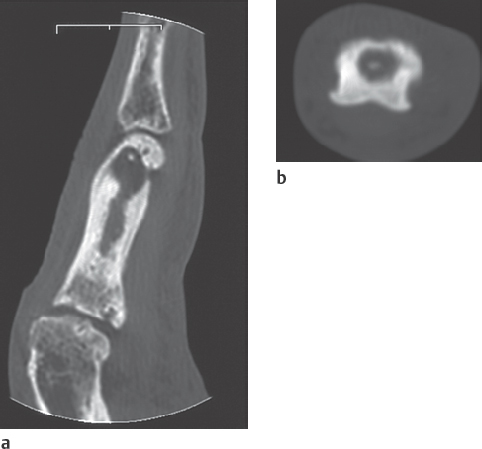
Sequester, granulation tissue, involucrum and an intraosseous abscess can be detected reliably in conventional tomography or CT ( Fig. 41.4 ).
|
Ultrasonography
Inflammatory involvement of the soft tissues and joints in osteomyelitis can reliably be confirmed with US.
Magnetic Resonance Imaging
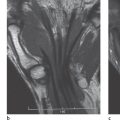
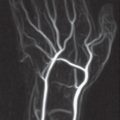
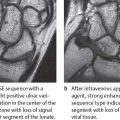
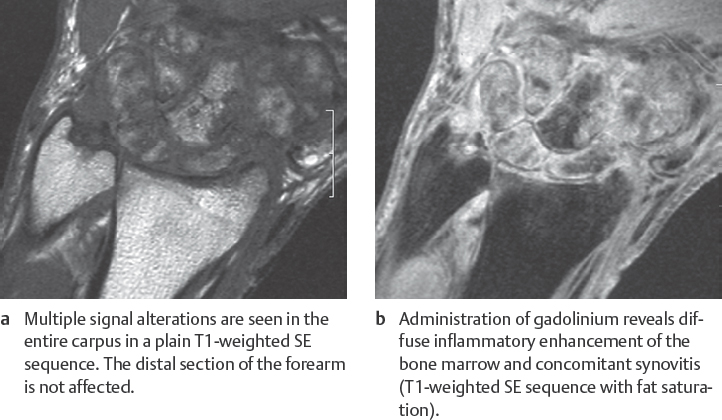
This procedure best determines the extent of bone-marrow infiltration and concomitant soft-tissue infection. Intraosseous and extraosseous inflammatory areas appear hypointense in T1-weighted sequences. After administration of gadolinium, signal intensity increases in vascularized granulation tissue( Figs. 41.2 , 41.3 ). Sequestra, however, show no enhancement. Because of their high contrast, fat-suppressed T2-weighted and STIR sequences are useful to identify bone-marrow edema. MRI is currently the method of choice to determine the complete extent of osteomyelitis.
Nuclear Medicine
If the results of three-phase skeletal scintigraphy are unremarkable, a florid inflammatory process in the hand skeleton can be largely excluded. Increased nuclide uptake in the presence of osteomyelitis is unspecific, however (Fig. 41.6a):
Differentiation between a posttraumatic process and an inflammatory process is not possible with nuclear medicine because in both inflammation and callus formation, there is an increased production of fibrous bony tissue and, thereby, an increased content of amorphous calcium phosphate with increased binding of the radiopharmaceutical substance. This is also the case for four-phase scintigraphy.
Up to six months after a trauma or surgery of the bones, leukocytic scintigraphy cannot differentiate between reparative remodeling processes and inflammatory ones. In chronic osteomyelitis, nuclide uptake of labeled granulocytes is in any case limited because of theunderlying pathophysiology.
Gallium scintigraphy, which is preferred in Anglo-American reports, has not yet reached acceptance in Europe. Labeled human immunoglobulins, which are under clinical evaluation, do not provide any more essential information than leukocyte scintigraphy. Alternatively,99m Tc-labeled nanocolloid, which leads to extravasation of the nuclide as a result of increased vascular permeability in inflammatory tissue, can be used.
Disease Entities
Hematogenous Osteomyelitis
Pathoanatomy and Clinical Symptoms
Acute hematogenous osteomyelitis is rare in the skeleton of the hand. The primary focus of infection often remains clinically unknown. The spectrum of pathogens varies according to age, and essentially all organisms can be found. Hematogenous osteomyelitis appears predominantly in the distal sections of the radius and ulna during growth when the epiphyseal plates are still open. The osseous infection usually originates in the metaphysis, where bacterial implantation is promoted by the slow blood circulation in the venous sinusoids. Edema and an accumulation of pus cause increased pressure and slowing of the blood circulation and lead to osteonecrosis. Reactive new periosteal bone formation surrounds the infected, necrotic bones.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree