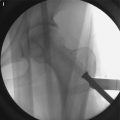
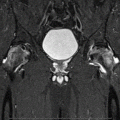
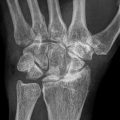
Fig. 22.1
An intraoperative photograph shows the pus-like (yellowish and turbid) joint fluid gushed from the hip joint (Reprint permission for Springer-Verlag)
22.5 Erroneous Leukocytosis of Joint Fluid by Automated Cell Counter
When an infection is suspected during operation, the joint aspirate is sent to laboratory for WBC count and neutrophil differential as well as culture. Most of the currently used automated cell counters use electrical impedance or light scattering to obtain a WBC count. The electrical impedance-based technology determines the number and size of cells by detecting and measuring the changes in electrical resistance when a cell in a conductive liquid passes through a small aperture. These cells are analyzed in an electro-optical flow cell. The cell volume is determined by the impedance. The light scattering-based technology determines the cell number and size by detecting the forward angle scatter of a laser-generated monochromatic light [4].
The size of the normal marrow fat cell is approximately 76 μm, which is much larger than that of the leukocytes ranging from 10 to 20 μm [5]. However, the fat cell membrane is ruptured in necrotic marrow and fat globules are released from the fat cells. Some shrunken fat cells and released fat globules are similar in size to leukocytes, which might be counted as leukocytes by automated cell counters [6]. Thus, most of automated cell counters, which are currently in use, may not be able to differentiate necrotic marrow fat from the leukocytes.
22.6 Distinguishing the Accumulation of Necrotic Marrow Fat from a True Septic Arthritis by Microscopic Examination
To avoid a false diagnosis of septic arthritis, microscopic examination of the smear must be performed with a hematoxylin and eosin stain. When only necrotic fat materials are observed and there is no aggregation of neutrophils in the microscopic examination of the smears (Fig. 22.2), THA can be done as scheduled regardless of automated WBC counts.
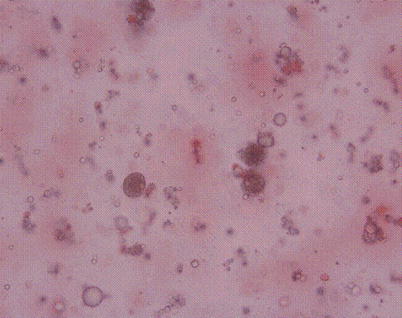

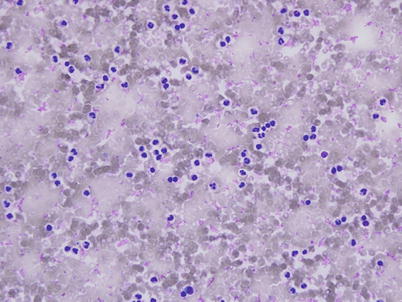
Fig. 22.2
An intraoperative smear of the liquefied fatty marrow from osteonecrotic hip shows fat globules and fat cells. No leukocytes are seen (stain, hematoxylin and eosin, original magnification, 9,400) (Reprint permission for Springer-Verlag)
Concomitant septic arthritis of the hip can occur in patients with ON of the femoral head [7], especially when the patient is immunocompromised or has sickle cell disease [7, 8]. When septic arthritis is confirmed under microscopic identification of an aggregation of neutrophils (Fig. 22.3), THA should be delayed until septic arthritis is treated. It is not known how long THA should be delayed in a patient with prior septic arthritis. The optimal timing of THA in patients with prior septic arthritis is not known. We usually delay the elective arthroplasty in patients with septic arthritis for a period of 1 year.