Localization: Desmoid fibroma is more frequent in the mandible, long bones, and pelvis. In the long bones, it is more often observed in the meta-diaphysis, but it may be diaphyseal. During adult age, it usually extends to the epiphysis.
Clinical: Symptoms are mild and late (the lesion grows slowly and is not very vascularized) and consist of moderate pain, possible pathologic fractures.
Imaging: The radiographic picture shows a large osteolysis, usually with expansion of the bone. The original cortex may be replaced by a thin shell of newly formed bone. Occasionally and focally, the tumor breaches the cortex with no clear demarcation toward the surrounding tissues. Rather typically, osteolysis has a finely trabeculated, reticulated, or bubbly appearance. Reactive chronic hyperostosis can produce a rind of sclerosis at the edges of the tumor. On angiography and CT, the tumor only moderately takes the contrast, and it appears relatively “cold” on isotope scan. MRI gives a low signal in T1 and T2 suggestive of dense collagenous tissue.
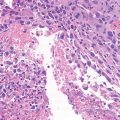
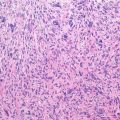
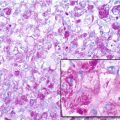
Histopathology: Hypocellular spindle cell tumor associated with large amounts of collagen. Nuclei have a bland appearance with no atypia and few mitotic figures. Areas of relative hypercellularity can be present, but are not common. β-Catenin pathway does not seem to have the same role in the tumorigenesis of desmoid tumor, as it has in the desmoid type-fibromatosis.
Course and Staging: Growth of the tumor is very slow; it may even take several years prior to causing symptoms. The stage is 2 or 3.
Treatment and Prognosis: Although historical data indicated wide en-bloc resection as the treatment of choice, recent experiences show that aggressive curettage is about equally effective providing better functional results. Desmoid fibroma does not metastasize.
Key Points
Clinical | Mild symptoms |
Radiological | Slow growing lytic lesion with possible expansion of the cortex
Stay updated, free articles. Join our Telegram channel
Full access? Get Clinical Tree
 Get Clinical Tree app for offline access
Get Clinical Tree app for offline access

|