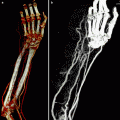
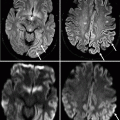
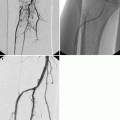
Fig. 26.1
LL projection without contrast medium. Anatomic landmarks: e epiglottis, h hyoid bone, l laryngeal vestibule, o oropharynx, r rhinopharynx, s soft palate, t (white arrows) tongue, asterisks retropharyngeal space
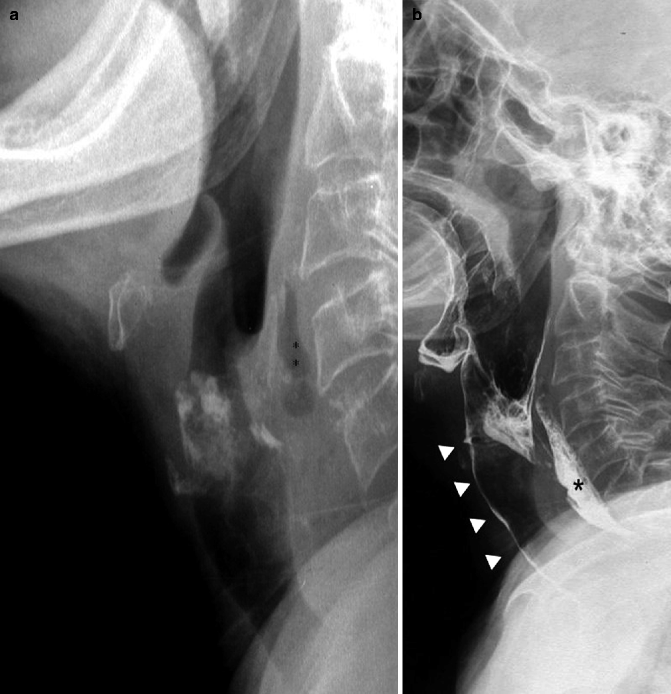
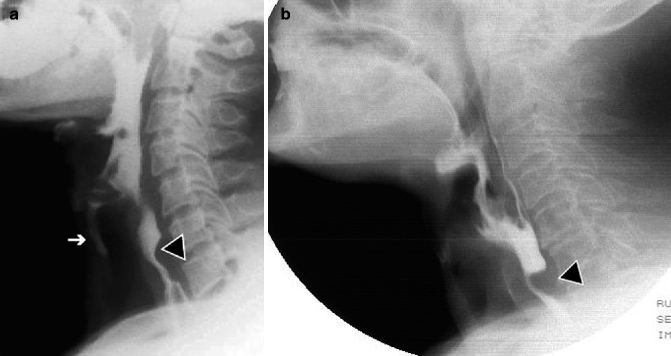
Fig. 26.2
LL projection without contrast medium (a) and with barium (b) in a patient with a retropharyngeal abscess. Small gas collection (asterisks) in the posterior retropharyngeal space (a). Abscess opacification with a small amount of barium (asterisk) after swallowing (b); barium aspiration in the airways (arrowheads)
The study in the AP projection without contrast medium is useful to assess the motility of the vocal cords and can be performed by recording videofluoroscopy during phonation, usually prompting the patient to pronounce the letter “eeee…” for a few seconds. Usually in this way it is possible to assess the symmetry of the closure of the vocal cords (Fig. 26.3a) and consequently any asymmetry or unilateral paresis (Fig. 26.3b). The VFSS continues with administration of barium contrast medium. Barium is a fairly safe substance, and the passage of a small amount in the trachea and main bronchi may be removed in a few hours by suction (Skucas 1999).
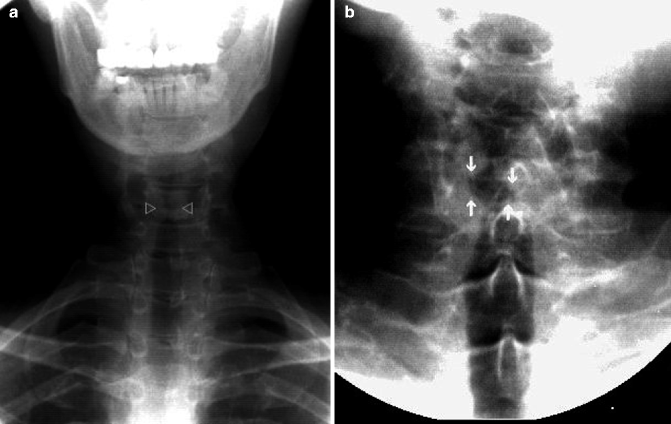

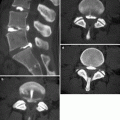
Fig. 26.3
AP projection without contrast medium acquired during phonation. Symmetric adduction and closure of the vocal cords (open arrowheads a). Right vocal cord paralysis with poor adduction and closure compared to the left side (white arrows b)
However, if a massive aspiration into the airways is suspected, especially in patients with a low level of consciousness, it may be a good precaution to use a non-ionic (iso-osmolar) iodinated contrast agent, which should not cause complications. We do not use the ionic (hyper-osmolar) iodinated contrast medium because its passage into the tracheobronchial tree can cause pulmonary edema (Jones and Donner 1991).
Generally we start with small amounts of contrast medium gradually increasing, if possible (Rubesin and Youssem 1999). In all cases it is necessary to administer boluses of different texture (Logemann 1983): liquid barium, fluid barium, high-density barium, barium mixed with rice pudding or apple smoothie and barium-coated crackers.
This allows the radiologist to:
evaluate patients who complain of dysphagia in relation to the consumption of some specific foods;
identify the food textures responsible for aspiration;
differentiate patients in which aspiration occurs with one food texture from those who have aspirations with more textures (more severe);
identify food textures that are less hazardous for the patient if oral feeding is indicated (Martin-Harris et al. 2000).
As swallowing is an extremely fast process (less than 1 s), it is necessary to have an excellent video recording system (50 frame/s) or a digital videofluoroscopy system (25–30 frame/s) for optimal evaluation of a dynamic swallowing study. The sequences are acquired in both LL and AP views.
Generally the examination starts in LL projection with the patient upright, as this is the projection that best allows documentation of the contrast medium passage in the laryngeal vestibule (penetration) and/or in the trachea (aspiration) (Fig. 26.1). If the patient cannot stand up, the examination must be done using a wheelchair.
Ideally all patients should be examined in both lateral and frontal positions. In fact an examination performed only in LL may even miss important abnormalities only detectable in the frontal position (Reginelli, Mandato, et al. 2012). The AP position is essential for detection of unilateral abnormalities such as masses (Fig. 26.4a, b), unilateral pharyngeal paresis, and unilateral vocal fold paralysis (Fig. 26.3b). In some patients, particularly if marked dorsal kyphosis is present, it may be also necessary to use oblique projections with appropriate neck rotation to obtain a better evaluation of the opening of the UES and cervical esophagus. In this way it is possible to dissociate the pharyngo-esophageal junction from the overlapping of the spine and shoulder girdle.
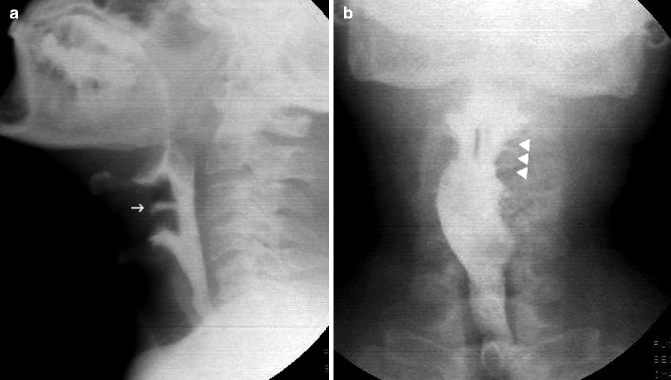

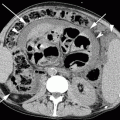
Fig. 26.4
LL (a) and AP projection (b) in patient with a left pyriform sinus mass. The lesion is well depicted in the AP view (white arrowheads) as an irregular marginal defect, but is not appreciable in the LL view. Small penetration in the laryngeal vestibule (white arrow) can be seen in the lateral projection
In some cases the change in the head posture during acquisition can reveal swallowing abnormalities that are not appreciable with the head in neutral position or in slight flexion. In the same way it could be also possible to search for compensatory maneuvers and postures (e.g. neck flexion and head rotation), ensuring safe swallowing (Solazzo et al. 2012; Palmer 2000). Finally, the appearance of alterations after repeated acts of swallowing can be a sign of myasthenia gravis (Jones and Donner 1991).
In very debilitated patients or with severe neurological deficits causing significant difficulty in swallowing, the contrast agent can be administered through a syringe connected to a tube placed in the oral cavity. This technique can also be useful to study the pharyngeal contractility without propulsive lingual activity (Jones and Donner 1991).
If an organic disease is suspected, standard radiographic pictures of the pharynx and/or esophagus should also be acquired, preferably after distension of the pharynx by Valsalva maneuver or during phonation (pronouncing “eeee…”).
The integration between morphologic images and dynamic acquisitions could be important as organic disorders often affect pharyngeal motility, while the structural aspects of movement disorders are often well demonstrated on static images. Moreover both structural damage and motility disorders may coexist (Rubesin and Youssem 1999).
Finally, in all patients with dysphagia, especially in the elderly, it is also mandatory to extend the evaluation of bolus transit up to the esophago-gastric junction to exclude organic and/or functional esophageal changes. For an optimal evaluation of esophageal peristalsis acquisitions with the patient both upright and supine are recommended. However in this case it is possible to use a smaller frame/second rate to reduce the radiation exposure.
In some rare conditions the dynamic swallow examination of the pharynx should be interrupted:
1.
total or almost total obstruction of the airways or the digestive tract for food or semi-solid;
2.
laryngospasm (except in patients with tracheostomy);
3.
bronchospasm;
4.
aspiration of gastric contents;
5.
complete absence of protective mechanisms of the airways (elevation of the larynx, closure of the glottis, epiglottis tilt, cough);
6.
other medical emergencies (cardiac or respiratory arrest).
There are also some relative contraindications to continuing the examination:
1.
barium aspiration in the airways in patients with a history of aspiration pneumonia or severe respiratory disease;
2.
barium aspiration in the airways not followed by cough (“silent” aspiration);
3.
retention of considerable amounts of solid food in the throat after swallowing;
4.
ineffectiveness of maneuvers to reduce the intake of contrast medium into the airways (Palmer 2000).
26.3 VFSS: Normal and Pathological Aspects
Swallowing is a complex physiologic event consisting of simultaneous and sequential contractions of oro-facial, pharyngeal, laryngeal, and esophageal muscles to propel ingested materials through the upper aero-digestive tract with simultaneous protection of the upper airways.
Schematically, in normal swallowing it is possible to distinguish:
1.
oral preparatory phase: the bolus is manipulated by lingual motion and masticated, if necessary, and also tasted or savored. All the actions of this phase are conscious and voluntary, the swallow reflex is absent and the airway remains open for the usual purpose of respiration (Page 2006);
2.
oral phase: the tongue starts to squeeze the bolus between the soft palate and itself. A groove or channel becomes evident in the tongue and its pressure conveys the food bolus posteriorly into the back of the mouth. As the bolus passes the posterior faucial pillars, the involuntary swallow reflex occurs (Page 2006);
3.
pharyngeal phase: four main physiologic events can be distinguished:
(a)
naso-pharyngeal seal;
(b)
elevation and anterior displacement of the larynx and hyoid bone;
(c)
laryngeal closure;
(d)
bolus compression and propulsion;
(e)
cricopharyngeal opening;
4.
esophageal phase: normal primary peristalsis as an aboral contraction wave that progressively obliterates the esophageal lumen is appreciable.
The VFSS, also known as a modified barium swallowing examination, is considered the best diagnostic method for evaluating swallow dysfunction disorders, as it allows real-time visualization of bolus flow in relation to structural movement throughout the upper aero-digestive tract. The VFSS also detects the presence and the timing of penetration/aspiration and helps to identify the causes of aspiration (often treatable). Furthermore, clinicians are able to observe the effects of various bolus volumes, bolus textures, and compensatory strategies about swallowing physiology (Martin-Harris and Jones 2008).
VFSS is the method of choice for studying the swallow physiology through the evaluation of the 15 main physiologic components of swallowing (Martin-Harris and Jones 2008):
1.
lip closure;
2.
lingual elevation;
3.
tongue-to-palatal seal;
4.
bolus preparation and mastication;
5.
bolus transport and lingual motion;
6.
initiation of pharyngeal swallow;
7.
soft palate elevation and retraction;
8.
laryngeal elevation;
9.
anterior hyoid excursion;
10.
laryngeal closure;
11.
pharyngeal contraction;
12.
pharyngo-esophageal segment opening;
13.
tongue base retraction;
14.
epiglottis inversion;
15.
esophageal clearance.
The first five physiologic components make up the oral preparatory phase and the oral phase.
In these phases it is possible to evaluate the ability to contain the bolus in the oral cavity through an anterior lip seal and latero-posterior tongue contact to palate. Bolus is kept within the mouth by a close apposition between the soft palate and posterior tongue (Fig. 26.5). Dysfunctions during this phase are frequently seen in patients with neurological diseases with consequent posterior leakage of barium into the pharynx and silent aspiration into the open unprotected airways (Fig 26.6).
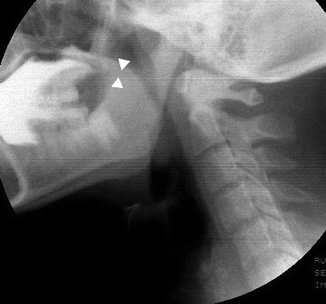
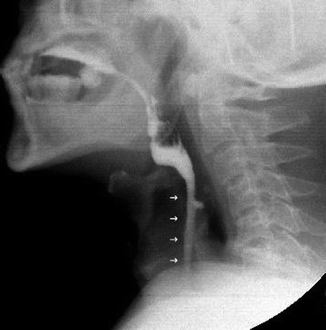

Fig. 26.5
Oral phase. Radiopaque bolus is kept within the mouth by a close apposition between the soft palate and posterior aspect of the tongue (arrowheads)

Fig. 26.6
Premature leakage of barium into the pharynx and aspiration into the open unprotected airways (small arrows) in a patient with a neuromuscular disorder
The tongue is the major mobile element of the oral swallow and plays a complementary role in bolus preparation and mastication. The bolus is held above the tongue in a central groove and is then transferred into the pharynx by a progressive upward and posterior movement of the tongue (Martin-Harris and Jones 2008). If reduced tongue control (with motor incoordination or weakness) and/or atrophy of the muscular tongue, or partial resection for cancer (Fig. 26.7), is present, it is possible to see a reduction of tongue movements with poor propulsion and compression of the bolus, stasis of the barium in the oropharynx and increased risk of subsequent aspiration into the airways.
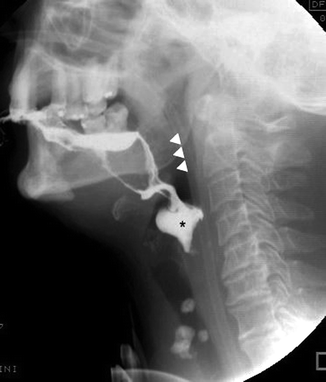

Fig. 26.7
Oral phase in patient with partial glossectomy. Premature leakage of barium into the pharynx (arrowheads) with opacification of the valleculae and pyriform sinuses (asterisk)
When the bolus reaches the oropharynx, sensory receptive fields are stimulated, initiating the pharyngeal phase of swallow. This phase is characterized by five mechanical events, which have been shown to overlap on synchronized video recordings of structural movements. These events protect the airways and contribute to clear the pharynx of ingested materials:
1.
elevation and retraction of the soft palate;
2.
elevation and anterior displacement of the larynx and hyoid bone (Fig. 26.8);
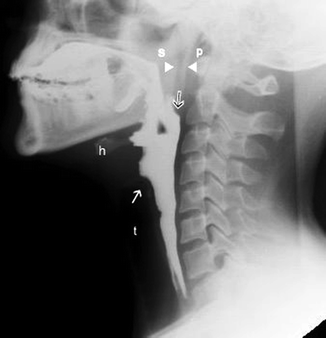

Fig. 26.8
LL view in a patient with normal pharyngeal phase: the soft palate (s) and posterior pharyngeal wall (p) remain closely in contact (arrowheads) until the bolus has cleared the oropharynx. Elevation and anterior displacement of the larynx and hyoid bone toward the mandible during swallowing (h). Note the closed larynx with the appearance of a conus (white arrow) and the tracheal air column (t). The posterior pharyngeal stripping wave (black arrow) is manifested by progressive anterior movement of the pharyngeal wall on dynamic imaging studies
4.
pharyngeal contraction;
Weakness or paralysis of the soft palate can determine closure deficiency of the palatopharyngeal seal during swallowing and will result in nasopharyngeal regurgitation (Fig. 26.9). The hyoid bone and larynx should move as a functional unit in a superior and anterior trajectory during a normal, nutritive swallow, and this movement indicates the start of swallow reflex (Martin-Harris and Jones 2008). Free up-and-down motion of the larynx and hyoid bone is an important factor in the prevention of barium laryngeal penetration. This elevation may be recognized by the upward and anterior movement of the hyoid bone toward the mandible during deglutition (Fig. 26.8). It is possible to see an abnormal initiation of the pharyngeal stage of swallow in case of trigger delay of the swallowing reflex due to sensori-motor impairment. This is easily appreciated when the bolus is conveyed into the pharynx without anterior movement of the hyoid bone and constrictor activity.
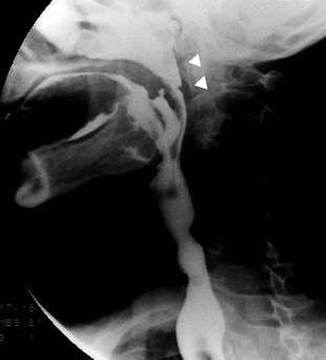

Fig. 26.9
Nasopharyngeal regurgitation during swallowing (arrowheads)
Laryngeal closure, hyoid/laryngeal elevation and epiglottis inversion are the three main mechanisms to protect the airway. Laryngeal closure has at least three levels of defense: closure of arytenoids, closure of true vocal folds, and closure of the false vocal folds. Failure of these mechanisms can lead to laryngeal penetration (entry of the bolus into the laryngeal vestibule or lower in the larynx but not through the vocal folds) (Fig. 26.10) or more serious aspiration (entry of ingested material through the level of the true vocal folds into the trachea) (Fig. 26.11). Both penetration and aspiration generally result in a reflexive cough (normal) or may not produce a cough so called silent aspiration. Aspiration can occur before swallowing: a classical cause is premature leakage from the mouth. Aspiration can also occur during or after swallowing: overflow of retained bolus (Fig. 26.12), reflux, or regurgitation (Jones 2006). There is a well-demonstrated relationship between the degree of penetration/aspiration observed during barium studies and the likelihood of developing aspiration pneumonia.
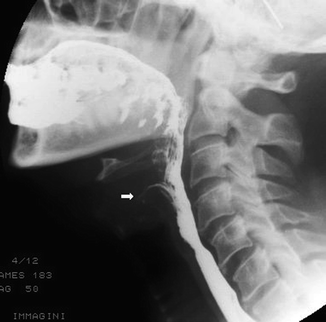
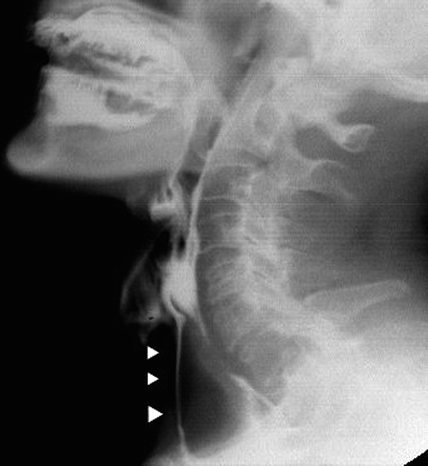

Fig. 26.10
Laryngeal penetration (arrow) during swallowing

Fig. 26.11
Silent aspiration (arrowheads) during swallowing in a patient with a previous brain ischemia
Patients with laryngeal penetration, tracheobronchial aspiration, or silent tracheobronchial aspiration were approximately 4, 10 and 13 times, respectively, more likely to develop pneumonia than those with normal swallowing (Pikus et al. 2003).
Contraction of the pharyngeal constrictors coincides with the forceful retraction of the tongue which applies strong positive pressure on the bolus tail, assisting in pharyngeal clearance and preventing pharyngeal residue. The constrictor stripping wave can be observed in the lateral position as a progressive forward movement of the posterior pharyngeal wall and in the frontal position as the movement of the lateral walls of the pharynx to the midline (Fig. 26.13a, b) (Jones 2006; Martin-Harris and Jones 2008). The absence of the posterior pharyngeal wall movement indicates paralysis. If constrictor muscles are paretic, the pharynx becomes flaccid, allowing an abnormal expansion of the chamber during swallowing and an abnormal stasis of barium in the pharynx with high risk of after-swallowing aspiration (Fig. 26.14).
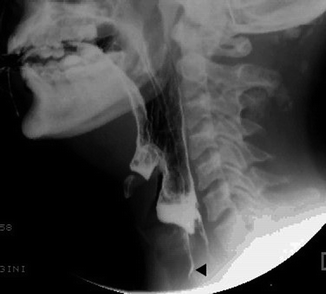
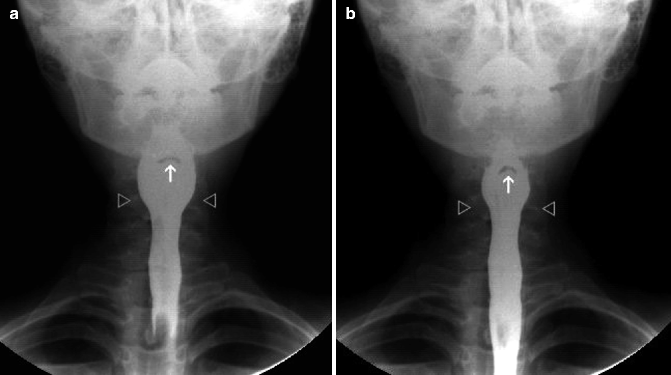
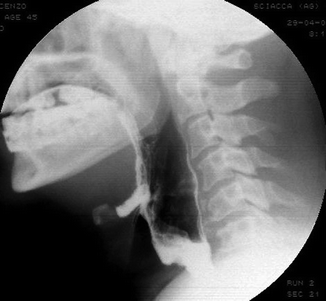

Fig. 26.12
Post-deglutitive aspiration of retained bolus in hypopharynx (black arrowhead)

Fig. 26.13
(a, b) Symmetric contraction of the constrictor muscles observed in the AP position. Note the symmetric movement of the lateral walls of the pharynx to the midline (open arrows). White arrow indicates the epiglottis

Fig. 26.14
Patient with pharyngeal paralysis related to brain-stem ischemia. Pharynx is flaccid with an abnormal expansion during swallowing and an abnormal stasis of barium in pyriform sinuses
In case of unilateral pharyngeal paralysis, the failure of the lateral pharyngeal walls coming to the midline indicates pharyngeal paresis.
The opening of the pharyngo-esophageal segment is related to the activity of the cricopharyngeal muscle (portion of the inferior constrictor muscle), which constitutes the UES together with some circular fibers of the proximal cervical esophagus. The muscle is tonically active during quiet breathing in order to prevent the entrance of inspired air into the esophagus and stomach, but during swallowing this area must relax and open completely to allow unimpeded passage of bolus from the pharynx into cervical esophagus.
On radiographic examination, the posterior indentation of the pharyngo-esophageal junction during bolus passage indicates the level of the cricopharyngeus. Functional disturbances of the cricopharyngeal muscle may make it incapable of relaxing during swallowing. The classic finding of a dynamic radiologic study is represented by the presence of a horizontal bar on the barium column at the level of the C5–C6 vertebral body; this posterior indentation persists throughout the swallow (Fig. 26.15a, b). Cricopharyngeal prominence or bar may be seen in the elderly as a secondary response to esophageal disease such as gastroesophageal reflux disease or spasm and in association with pharyngeal paresis or a frozen larynx (Jones 2006).