Location: Long bones, metaepiphyseal, and eccentrical: distal femur, proximal tibia, and distal radius (65 % of the cases). Rare in the sacrum and pelvis. When occurring in long bones before closure of growth plate, the tumor is metaphyseal. Exceptionally multicentric (less than 0.5 %, rule out hyperparathyroidism).
Clinical: Pain dominates the scenario, but swelling and muscular hypotrophy is also frequently encountered; severe stiffness and pathologic fracture are less common.
Imaging: On x-ray, purely lytic with relatively well-defined margins (“puddle on the sand”) but not so sharply defined as other benign tumors and somewhat variable depending upon the tumor stage. The cortex is usually thinned, often expanded, and sometimes violated with little if any periosteal reaction. Soft tissue recurrence usually has an ossified rim. In an isotope bone scan, the uptake usually corresponds with the radiographic limits of the lesion, often it may show a cooler center with hotter rim; in aggressive forms, the uptake is beyond the radiographic limits. The CT images show a usually isodense lesion that occupies the bone with small outpockets in the borderline spongiosa. In some cases, intralesional cystic areas with fluid levels may be evident. MRI images may reveal a nonhomogenous signal, low in T1 and high in T2.
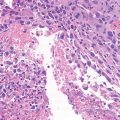
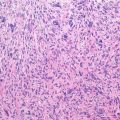
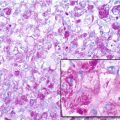
Histopathology: Gross: meaty reddish-purple tissue merged with soft yellow areas and often cystic areas (ABC-like areas). Histology: mononuclear cells and giant cells are uniformly distributed. Nuclei of mononuclear cells and giant cells are identical. There is mitotic activity but no atypical mitoses or cytological atypia. Necrotic areas and collection of foam cells are common, sometimes unusually rich of spindle cell areas. The stromal cells represent the neoplastic and proliferative component of the lesion. They secrete several chemokines which attract blood monocytes and stimulate their migration into tumor tissues. These monocytes fuse to form the osteoclast-like, multinucleated giant cells.
Course and Staging: Course unpredictable if untreated: sometimes indolent, sometimes rather aggressive. Histological grading has no value. Local recurrence rate depends upon stage and treatment. About 2–3 % is metastatic, usually to the lung. Malignant transformation: spontaneous 1 %, radiation induced 5–15 %. Presentation: about 10 % as stage 1, 60 % as stage 2, and 30 % as stage 3.
Treatment: Curettage represents the preferred surgery in stage 1, stage 2, and some stage 3 lesions. Recurrence rate ranges between 10 and 15 % with local adjuvants (cement, phenol, liquid nitrogen) and 15 and 30 % without local adjuvants. En bloc resection is recommended in stage 3 lesions with massive bone destruction, displaced pathologic fracture, and expendable bones. Radiation therapy adjuvant following intralesional surgery has been occasionally used in difficult locations (spine, pelvis, and sacrum). Recent studies indicate a possible role for medical treatment using anti-RANK-L antibodies (see Chap. 21).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree