Case presentation
An 18-month-old female presents with 1 to 2 weeks of fussiness and not wanting to ambulate. She has not had any fevers, vomiting, or diarrhea. There is no report of trauma. About 2 weeks prior, she had a cough, congestion, and low-grade fever (100.4 degrees Fahrenheit) that resolved after a few days. She has been healthy since then.
Her primary care physician evaluated the child 1 day after her symptoms began. At that time, the child was complaining of what was thought to be left leg pain (the mother stated that the child cried when attempting to ambulate and did not seem to want to bear weight on the left leg). Plain radiographs of the pelvis (including anterior-posterior [AP] and frog leg views), the left femur, and left tibia-fibula were obtained and were unremarkable. Since that time, the child has refused to ambulate and does not want to bear weight on either leg. Her primary care provider obtained a bilateral hip ultrasound (US), which was unremarkable.
Her physical examination shows a child in no distress. Her temperature is 98 degrees Fahrenheit, heart rate is 101 beats per minute, respiratory rate is 22 breaths per minute, and blood pressure is 90/60 mm Hg. She has an unremarkable examination, including her neurologic examination, which demonstrates no weakness or obvious lack of sensation. When attempting to ambulate, she refuses to do so and in fact cries when standing upright. She does not have any obvious findings on her extremities and range of motion maneuvers at her hip, knees, and ankles are normal. You note that the child prefers to lie down and, when she sits up, appears to be in discomfort.
Imaging considerations
Gait disturbances in the pediatric patient have a lengthy differential diagnosis to consider. History and physical examination should guide further laboratory and radiographic evaluation.
Plain radiography
Plain radiography is often employed as an initial imaging modality in pediatric patients who have either painful ambulation or who are refusing to ambulate. Obtaining radiographs in children with these symptoms is a reasonable first step, utilizing AP and lateral views. , Early on in the course of the illness, radiographs usually appear normal. Children who have discitis may demonstrate narrowing of the disc space with varying degrees of vertebral end plate destruction, resulting in loss of disc space height, usually 2 to 3 weeks after the onset of illness. , Radiography also has the advantage of detecting other possible causes of pain, such as fractures.
Ultrasound
The use of US in the evaluation of a patient with suspected discitis has not been established.
Computed tomography (CT)
CT has a limited role in the initial evaluation of patients with suspected discitis or other infections of the spine, although it can be used to guide biopsy procedures. This modality does have the ability to provide detailed information about anatomy (especially bone detail) but may not detect abnormalities early in the course of illness.
Bone scan (technetium-99M)
Bone scan is sensitive for the detection of inflammatory processes, such as infection, but is not specific. , , This modality has largely been replaced by magnetic resonance imaging (MRI).
Magnetic resonance imaging
MRI with and without intravenous contrast has become the imaging study of choice to evaluate for discitis or suspected infection of the spine. , , , One study showed that MRI has a sensitivity of 97% for the detection of infection and greater than 90% for discitis. This modality has largely superseded nuclear bone scanning and is both sensitive and specific for discitis. , MRI findings vary depending on when the imaging study is obtained. Early in the process, vertebral end plates, the disc, and subchondral regions show only minor changes, but as the process progresses, the end plates may become irregular and blurred, ultimately becoming dark on T1-weighted images and bright on T2-weighted images; the disc may appear collapsed; and the adjacent vertebrae may show abnormality if the infection spreads. , ,
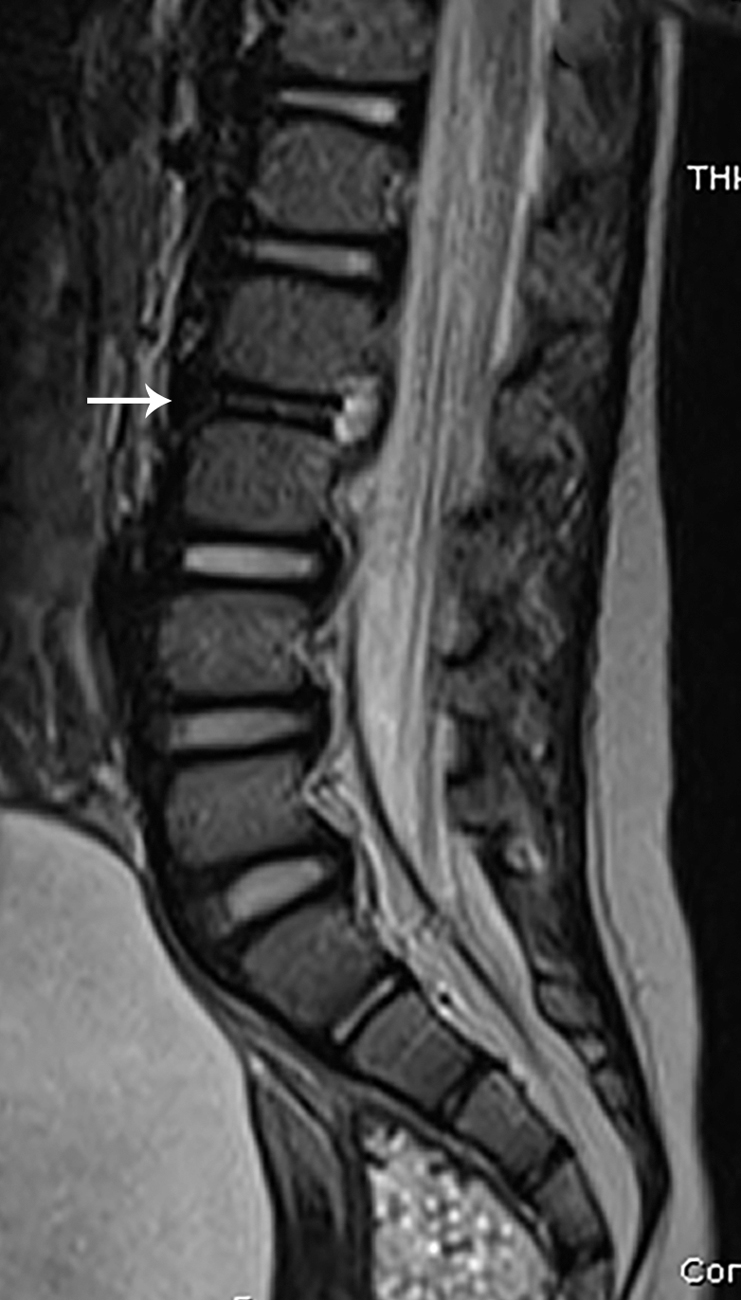
Imaging findings
The patient underwent MRI of the lumbar spine. Selected images from that study are provided here. There is abnormal marrow edema in the L2 and to a lesser extent L3 vertebral bodies. The L2/3 disc demonstrates loss of height, altered signal intensity, and enhancement ( Figs. 77.1–77.3 ).