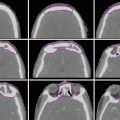
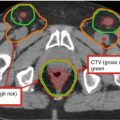
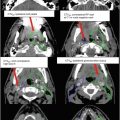
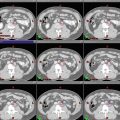
Fig. 1
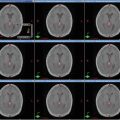
(a) Axial T1-weighted post-contrast MRI demonstrates a homogeneously enhancing meningioma in the frontal falx cerebri causing mild mass effect on the adjacent frontal gyri (arrow). (b) Axial T1-weighted post-contrast MRI demonstrates a small homogeneously enhancing dural-based lesion along the left aspect of the posterior falx cerebri adjacent to the parieto-occipital sulcus with mild extension into the patent adjacent superior sagittal sinus (arrow)
Multiple meningiomas, also known as meningiomatosis, occur in only 2.5 % of cases (Lee 2008).
1.2 Pituitary
The pituitary gland, located in the sella turcica, is typically 8 mm in males and 10 mm in females in the superior-inferior dimension. Pituitary tumors that are smaller than 10 mm are referred to as microadenomas, while tumors larger than this are referred to as macroadenomas. Pituitary adenomas are also subdivided into functioning (secreting) and nonfunctioning (non-secreting) types.
The pituitary gland and paired cavernous sinuses are located in the sellar and parasellar region of the middle cranial base. The boundaries of the sella turcica include the tuberculum sellae and anterior clinoid processes anteriorly and the dorsum sellae and posterior clinoid processes posteriorly. The sella is defined inferiorly by the portion of the sphenoid bone that also marks the superior margin of the sphenoid sinus. The superior border of the sella is covered by the diaphragma sellae. The lateral border is bounded by the cavernous sinuses which bridge the superior orbital fissure to the apex of the petrous bone (Swearingen and Biller 2008).
The cavernous sinus contains a segment of the carotid artery and is the location where multiple veins from the cerebrum and cerebellum connect with draining venous sinuses. From superior to inferior, the oculomotor (CN III), trochlear (CN IV), and ophthalmic nerves (CN V1) are located in the lateral segment of the cavernous sinus; the abducens nerve (CN VI) is located in the medial segment (Swearingen and Biller 2008; Dolenc and Rogers 2009) (Fig. 2).

Fig. 2
Coronal section through the cavernous sinus depicting the location of the cranial nerves, carotid artery, and pituitary gland
To estimate the likelihood of cavernous sinus invasion by a pituitary adenoma, it is helpful to evaluate the extent of encasement of the carotid artery. In general, if there is a plane of normal-appearing pituitary tissue between the adenoma and the cavernous sinus, there is little to no risk of cavernous sinus invasion. On the other hand, complete encasement of the carotid artery is indicative of cavernous sinus invasion. In between, if there is less than 25 % encasement of the carotid artery, there is a small chance of cavernous sinus invasion, but if there is at least 67 % encasement of the carotid artery, the probability is quite high (Swearingen and Biller 2008) (Fig. 3).

Fig. 3
Axial T1-weighted post-contrast MRI demonstrates a bulky intrasellar pituitary adenoma with suprasellar extension and extension into the bilateral cavernous sinuses, sphenoid sinus, clivus, and basisphenoid sinus. The bony sella is expanded, remodeled, extensively invaded, and demineralized. Retroclival extension is also present
1.3 Vestibular Schwannoma
Vestibular schwannomas are divided into four stages based on location and size: intracanalicular, cisternal, brainstem compressive, and hydrocephalic.
Vestibular schwannomas that are contained within the internal auditory meatus, known as intracanalicular schwannomas, are usually round or oval in shape. If the tumor contains an extrameatal component, that portion is typically spherical and tapers towards the internal auditory meatus (Sriskandan and Connor 2011).
The boundaries of the cerebellopontine angle (CPA) are the brainstem medially, the cerebellum superiorly and posteriorly, and the temporal bone laterally. The inferior extent of the CPA is bounded by the glossopharyngeal (CN IX), vagus (CN X), and spinal accessory nerves (CN XI) (Kutz et al. 2012).
The vestibular nerve root arises from the vestibular apparatus, and the cochlear nerve root arises from the auditory apparatus to form the vestibulocochlear nerve which courses through the internal auditory meatus to the cerebellopontine angle (CPA) (Schünke et al. 2007).
Vestibular schwannomas often arise from the superior or inferior branches of the vestibular nerve.
Additional important structures traversing the CPA include the anterior inferior cerebellar artery and the facial nerve (CN VII).
1.4 Arteriovenous Malformations (AVMs)
AVMs occur more commonly in the cerebral hemispheres (85 %) than in the posterior cranial fossa (15 %) (Kornienko and Pronin 2009).
The arterial blood supply to an AVM may arise either directly from the feeding artery or indirectly from supplementary arteries transmitting blood from the supply region of a single artery. Additionally, the afferent arterial vessels can form various vascular channels, aneurysms, or pseudoaneurysms. In 27–32 % of AVMs, the arterial supply arises from a combination of intracranial arteries, dural arteries, and extracranial arteries (Kornienko and Pronin 2009).
Venous drainage of an AVM may be directed through a single large or numerous small veins. The draining veins of an AVM are visualized during the arterial phase of the angiogram (Kornienko and Pronin 2009).
1.5 Trigeminal Nerve (CN V)
The trigeminal nerve contains sensory afferent fibers and visceral efferent fibers. The somatic afferent fibers are responsible for sensation from the face, nasopharyngeal mucosa, and anterior two-thirds of the tongue (Schünke et al. 2007).
The three major divisions of the trigeminal nerve are the ophthalmic division (V1) which travels through the superior orbital fissure to the orbit, the maxillary division (V2) which travels through the foramen rotundum to the pterygopalatine fossa, and the mandibular division (V3) which travels through the foramen ovale to the base of the skull (Schünke et al. 2007).
The individual divisions of the trigeminal nerves converge at the anterior aspect of the trigeminal ganglion. The trigeminal ganglion is enveloped by dura mater and located in Meckel’s cave, a depression in the petrous part of the temporal bone lateral to the cavernous sinus.
2 Diagnostic Workup Relevant for Target Volume Delineation
2.1 General Principles
A thorough history should be obtained, and an appropriate physical examination with a specific emphasis on the neurologic exam should be performed.
A patient’s performance status should be evaluated using a validated scale such as the Karnofsky performance scale (KPS), ECOG performance status, neurologic function status (NFS), or mini mental status exam (MMSE).
All patients should have an MRI of the brain performed for diagnostic and treatment planning purposes. MRI sequences should include precontrast T1-weighted, precontrast T2-weighted, and fluid-attenuated inversion recovery (FLAIR) images. Multiplanar (axial, sagittal, and coronal) post-contrast gadolinium-enhanced T1-weighted images should also be obtained. For enhancing tumors, high-resolution modes such as magnetization-prepared rapid gradient echo (MP-RAGE) are utilized for accurate delineation of the disease of interest. A constructive interference in steady state (CISS) or 3D fast imaging with steady state acquisition (3D FIESTA) may be useful for identifying the cranial nerves. Fat suppression MRI scans are also useful in determining target volumes for some tumors such as optic nerve sheath meningiomas.
2.2 Meningiomas
On diagnostic CT scans, meningiomas appear as well-circumscribed, extra-axial masses that displace adjacent parenchymal tissue. They are isodense or hyperdense when compared to the normal brain tissue and demonstrate strong homogeneous contrast enhancement. Calcifications may be visualized in 20–30 % of meningiomas, and approximately half of cranial base meningiomas are associated with adjacent bone changes such as hyperostosis and osteolysis (Pieper et al. 1999).
Typically, meningiomas are isointense or hypointense to gray matter on T1-weighted MR images and isointense, hypointense, or hyperintense on T2-weighted images. On the FLAIR sequence, meningiomas are typically hyperintense to gray matter (Tsuchiya et al. 1996).
Approximately 90 % of meningiomas demonstrate strong homogenous enhancement with gadolinium; 10 % demonstrate mild enhancement (Pamir et al. 2010) (Fig. 4a, b).

Fig. 4
(a) Axial T1-weighted post-contrast MRI demonstrates a homogeneously enhancing meningioma centered along the anterior right tentorium with extension in the right cavernous sinus. There is also posterior extension along the right aspect of the clivus and mild mass effect on the adjacent undersurface of the right cerebral peduncle and the ventral aspect of the pons. There is partial encasement of a segment of the right posterior cerebellar artery. (b) Axial T1-weighted post-contrast MRI shows an enhancing extra-axial soft tissue mass overlying the lateral aspect of the right frontal pole with heterogeneous enhancement medially and moderate compression of the underlying parenchyma consistent with a convexity meningioma (arrow)
Approximately two-thirds of meningiomas exhibit a characteristic dural thickening, classically known as a “dural tail,” which extends 0.5–3.0 cm from the meningioma mass. Imaging criteria for defining the dural tail include (Rokni-Yazdi and Sotoudeh 2006; Goldsher et al. 1990):
Presence on at least two consecutive slices in more than one imaging plane
Tapering of the tail from the meningioma mass
More enhancing than the meningioma mass
Approximately 60 % of meningiomas are accompanied by peritumoral edema, seen most frequently with meningiomas of the olfactory groove, parasagittal region, and convexity (Pamir et al. 2010).
2.3 Pituitary Adenomas
On diagnostic CT scans, pituitary microadenomas appear hypodense and exhibit less contrast enhancement than a normal pituitary gland (Swearingen and Biller 2008).
Typically, pituitary microadenomas are hypointense to the normal pituitary gland on T1-weighted MR images, but can be isointense in 25 % of cases (Bonneville et al. 2005). The isointensity of pituitary adenomas on T2-weighted images can be quite variable; for example, approximately 80 % of prolactinomas and 67 % of GH-secreting microadenomas are isointense or hypointense (Swearingen and Biller 2008; Bonneville et al. 2005).
Macroadenomas exhibit variable MRI features, but are typically hypointense on T1-weighted MR images and hyperintense to the normal pituitary gland on T2-weighted MR images (Swearingen and Biller 2008).
Pituitary adenomas that are partially cystic may be hypointense on T1-weighted MR images. If there is a significant protein or lipid concentration in the pituitary cysts or if there is intralesional hemorrhage, there may be areas of hyperintensity observed on T1-weighted MR images.
Pituitary adenomas demonstrate heterogeneous, partial, or incomplete enhancement with gadolinium (in contrast to the strong homogeneous enhancement visualized with sellar or parasellar meningiomas) (Taylor et al. 1992) (Fig. 5a, b).

Fig. 5
(a, b) Axial T1-weighted MRI demonstrates a well-circumscribed heterogeneous sellar/suprasellar mass with remodeling and expansion of the sella turcica. This mass also extends into the left cavernous sinus region, and the suprasellar portion of the mass abuts the medial aspect of the supraclinoid internal carotid arteries with uplifting of the optic chiasm and floor of the third ventricle
In pituitary adenomas with suprasellar extension, it is important to measure the extent of disease through the diaphragm sellae, including the closest distance between the tumor and the optic chiasm and optic nerves (Fig. 6a, b).

Fig. 6
(a, b) Coronal T1-weighted non-contrast and post-contrast MRIs show the heterogeneously enhancing pituitary macroadenoma in the sella that is expanding the infundibulum. The mass extends into the cavernous sinus on the left with mild displacement and elevation of the optic chiasm. The optic chiasm is outlined in red
A complete hormonal evaluation should be performed including measurement of the serum prolactin concentration, serum insulin-like growth factor (IGF)-1, serum growth hormone levels after a glucose load, 24-h urine cortisol, ACTH, LH, FSH, free T4, T3, and serum TSH.
Visual field and visual acuity testing should be performed to determine any pattern of vision loss.
2.4 Vestibular Schwannoma
On diagnostic CT scans, vestibular schwannomas appear as well-demarcated isodense masses that demonstrate enhancement with IV contrast. The absence of calcifications helps to differentiate these tumors from meningiomas radiographically.
Typically, vestibular schwannomas are isointense or hypointense to the pons on T1-weighted MR images and heterogeneously hyperintense on T2-weighted images (Fig. 7).

Fig. 7
T1-weighted post-contrast MRI demonstrates an enhancing vestibular schwannoma with internal cystic changes in the left internal auditory canal extending into the cerebellopontine angle
Vestibular schwannomas demonstrate strong homogeneous enhancement with gadolinium.
For diagnostic evaluation of vestibular schwannomas, a thin-slice T1-weighted gadolinium-enhanced MRI of the cerebellopontine angle is helpful.
A constructive interference in steady state (CISS) or 3D fast imaging with steady state acquisition (3D FIESTA) sequence can produce high-resolution images of the tumor and vestibulocochlear nerve by outlining the structures surrounded by CSF.
Ancillary testing performed at diagnosis includes pure tone and speech audiometry, brainstem-evoked response audiometry, and vestibular testing.
2.5 Arteriovenous Malformations (AVMs)
On CT scans, AVMs appear as tortuous vessels that are isodense or hyperdense. Calcifications may be present in the vessels or the surrounding brain. AVMs demonstrate strong enhancement with IV contrast. Hemorrhages may be visualized around the nidus and the adjacent brain.
On CTA, the feeding arteries and draining veins demonstrate enhancement.
Typically, AVMs appear as hypointense flow voids on both T1-weighted and T2-weighted MR images.
The nidus of the AVM demonstrates strong gadolinium enhancement, and the draining veins are also visualized on contrast-enhanced MR images (Fig. 8a, b).

Fig. 8
(a) Axial T1-weighted post-contrast MRI demonstrates a vascular malformation in the right frontoparietal lobe, right MCA territory, with draining veins without edema or hemorrhage (arrow). (b) Right frontoparietal AVM, elongated vertically, and located in the precentral-central region. Feeders originate from a large right MCA branch and a large right ACA branch (arrow)
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree