As with other books in The Requisites series, this installment is primarily geared toward the radiology resident. It is not intended to provide an exhaustive review of pediatric imaging; rather, the hope is that it will serve as a useful and manageable resource for the topics most commonly encountered in pediatric radiology as a resident completes his or her 3-month rotation covering both the tertiary care and the community settings.
The chapters are organized by organ systems, with six devoted to body imaging and three focusing on neuroimaging. Discussions around imaging modalities and techniques are embedded in the respective chapters. In this first introductory chapter, we have chosen to present a few topics that are particularly important in pediatric imaging and may be somewhat unfamiliar to radiology residents as they begin their first experience in pediatrics. These include radiation dose optimization, the roles of child life and anesthesia/sedation in pediatric imaging, and the unique challenges of communicating effectively with patients and parents in pediatric radiology.
Radiation Dose Optimization in Pediatric Imaging
Medical imaging has a profound impact on the treatment of children and has become an integral part of pediatric patient care in both the inpatient and the outpatient settings. With the exception of magnetic resonance imaging (MRI) and ultrasound, ionizing radiation is an essential element for most common forms of diagnostic medical imaging. Although digital and computed radiographic studies represent a majority of radiologic procedures, they represent a relative minority of the collective effective dose to the pediatric patient population. A large percentage of ionizing radiation in medical imaging is related to the generalized increased use of computed tomography (CT). Despite the fact that CT generates a disproportionately higher dose than radiography and certain fluoroscopic procedures, the clinical value of CT is unquestioned, and this modality is largely regarded as a safe procedure for children provided the study is clinically justified. In general, the amount of ionizing radiation from a single pediatric CT examination is relatively small, particularly if the study is performed properly. The benefits of a clinically indicated diagnostic CT scan are well recognized and documented, and these benefits generally far outweigh the small potential risks for cancer. Even though it is the radiologist’s responsibility to perform pediatric imaging studies using the least amount of radiation necessary for a particular clinical question, it is also the responsibility of the pediatric health care professional to ensure that each CT study is indicated and have a general understanding of the relative doses and relative risks of common pediatric imaging studies.
Despite the known virtues of pediatric diagnostic imaging, public perception is often closely linked to the perceived risks of exposure to ionizing radiation. The potential hazards and perceived risks of ionizing radiation in children have been intensely studied and debated for years, and much of the fear associated with the use of ionizing radiation is unjustifiably rooted in the destructive power of nuclear weapons. Although there is no consensus on the true risks of exposure to low-level ionizing radiation, there is a general agreement that exposure to ionizing radiation at doses above a certain threshold can result in a small risk for cancer later in life. More than a decade ago, several articles were published in the February 2001 issue of the American Journal of Roentgenology describing the potential risks of ionizing radiation. This raised awareness that many children were receiving a higher dose of ionizing radiation than necessary for CT studies. Although it is challenging to directly demonstrate the potential risks for a single CT examination in an individual patient, some researchers estimate a small number of all cancers in the United States may be attributable to the radiation from CT studies. Until recently, this hypothesis was based largely on data from atomic bomb survivors. Although there is some disagreement within the medical community about the most accurate depiction of risks from ionizing radiation related to CT imaging, it is widely believed in the pediatric radiology literature that dose reduction in children and adherence to the ALARA (as low as reasonably achievable) principle are of paramount importance.
In 2008, the Image Gently campaign ( http://www.imagegently.org ) was founded and championed by the Society for Pediatric Radiology, the American Society of Radiologic Technologists, the American College of Radiology, and the American Association of Physicists in Medicine. The collaborative campaign is a dynamic alliance of individual health care professionals including the radiologist, radiology technologist, medical physicist, and pediatrician, creating a powerful force that has changed practice. The Image Gently campaign unifies more than 80 organizations, currently representing more than 800,000 international medical and dental professionals in radiology, pediatrics, physics, and radiology technology. The Image Gently website ( http://www.imagegently.org ) provides a comprehensive, peer-reviewed resource for a variety of pediatric imaging modalities including CT, digital radiography, nuclear medicine, interventional radiology, fluoroscopy, and dental imaging.
Optimizing CT protocols remains a challenge, particularly when imaging pediatric patients. Many institutions have more than one CT scanner, and many of those institutions have more than one CT vendor in their practice. This necessitates multiple different CT protocols for a similar indication or similar-sized patient. Nevertheless, any given institution’s protocols are typically vendor and scanner specific, and as a result, these protocols are not easily transferrable to other institutions. The Image Gently website is an excellent resource for pediatric CT protocols. This resource can serve as a starting point for adult-based radiology practices that image children and wish to develop pediatric specific CT protocols, or for those practices that are seeking general guidance for pediatric CT studies and would like to verify that their existing protocols meet appropriate guidelines.
When a pediatric CT scan is requested, it is important to first consider utilizing alternative imaging modalities such as ultrasound or MRI, which do not require the use of ionizing radiation. However, there should be no hesitation in performing a CT study when it is deemed to be the best imaging test for a given clinical situation. Once the decision to perform a CT is made, it is as important to optimize the CT examination parameters in an effort to minimize dose. Strauss et al provide a nice summary on optimization of CT parameters for pediatric imaging, including specific information on tube current, exposure time, kVp, pitch, and automatic exposure control. Recently the widespread use of iterative reconstruction software has provided further reductions in CT dose, but this new technology also provides another potential level of complexity to protocol generation.
Increased utilization of endoscopy, CT, and MRI has gradually resulted in decreased utilization of fluoroscopy for pediatric chest, gastrointestinal, and genitourinary imaging. However, fluoroscopy remains an important imaging modality for the evaluation of a multitude of pediatric conditions, including neonatal high or low intestinal obstruction, the acutely vomiting infant or child, dynamic large airway imaging, and the evaluation of certain patients with suspected vesicoureteral reflux including patients with a history of febrile urinary tract infection.
In addition to CT dose reduction, national efforts to reduce radiation exposure from medical imaging have included initiatives to reduce unnecessary radiation exposure from fluoroscopic examinations. Despite its virtues, fluoroscopy provides an added challenge for the diagnostic radiologist. This modality is substantially more operator dependent than CT, and doses can vary significantly from patient to patient for similar clinical indications.
When performing a pediatric fluoroscopy study, one should always make an effort to decrease patient dose by minimizing fluoroscopy time, avoiding magnification whenever possible, maximizing collimation, utilizing pulsed fluoroscopy and last image hold, and minimizing the distance between the patient and the image intensifier. These principles are highlighted in the Image Gently Pause and Pulse campaign.
Role of the Child Life Specialist and the Importance of Relationship Building in Pediatric Radiology
Certified child life specialists (CLSs) are essential to adequately meet the needs of patients and families entering the pediatric radiology department. For many children, if not most, the radiology department can be a stressful and intimidating environment. Imaging involves machines that may be perceived as loud and frightening, as well as potentially uncomfortable positioning and procedures that may cause discomfort. Radiology is often the first encounter for patients in the medical setting, but likely will not be the last. It is therefore essential to involve CLSs to help create a positive experience and assist children and families in coping with anxiety related to radiologic studies.
Certified CLSs are trained professionals who work with children and families to assist them with the challenges of hospitalization, illness, and disability. They are found throughout the pediatric health care setting. CLSs have a strong background in human growth and development. This specialized training enables them to normalize the hospital environment for children and prepare them for medical experiences, taking into account the age, developmental stage, and unique needs of each patient. As advocates of family-centered care and vital members of the multidisciplinary health care team, CLSs work in partnership with all practitioners to meet the emotional, developmental, and cultural needs of each child and family. CLSs also serve as a resource for other hospital staff members and are active in providing formal and informal education around age-appropriate practices and successful relationship-building skills.
As a clinician working in the pediatric medical setting, it is important to remember that a child’s age is not always indicative of the child’s developmental stage. Many factors such as acute pathology, chronic illness, a prolonged hospital stay, and even parenting style can affect a child’s developmental level. Despite this, there are universal approaches to interacting with children that are effective across the board. These include making eye contact, addressing fears, being present with children and their families, and clearly communicating your role as part of the health care team. When working to establish a relationship with a patient, it is important to be observant and tuned in to a child’s expression and posture. Is the child avoiding eye contact? Is the child clinging to his or her caregiver? Is the child fidgety or biting his or her nails? It is critical to take cues from the patient and tailor your approach accordingly. Information about a child’s past experience(s) in the medical setting and coping style should be elicited from a caregiver if possible. Demonstrating an honest interest in the child and individualizing care will go a long way, enhancing the child’s ability to cope and facilitating completion of the study or procedure at hand.
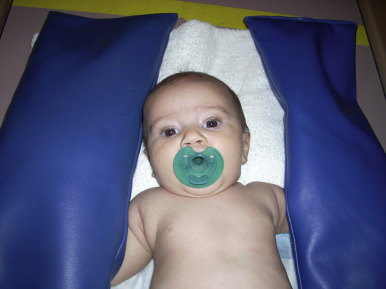
It is important to be mindful of age-appropriate techniques in facilitating cooperation with pediatric patients. Infants often respond best when a caregiver is close by and a comfort item is provided. A pacifier dipped in oral sucrose can be very soothing during procedures that may cause discomfort [ Fig. 1.1 ]. Toddlers can be particularly challenging to image, as they are constantly on the move, learning independence, and often strong-willed. Distraction techniques such as singing songs and blowing bubbles are typically very effective with this age group, affording brief windows of opportunity for study completion [ Fig. 1.2 ]. Preschool-aged children are magical thinkers and may see medical experiences as a form of punishment. For them, providing a rationale for imaging may be helpful. A statement such as “the doctor needs to take a picture to make sure everything is working okay inside your body” may facilitate patient cooperation. School-age children are logical thinkers and usually do best when they know what to expect and are given some control of their situation. In preparation for an MRI, one might say, “This test will take 30 minutes, the length of your favorite TV show. You can help us by keeping your body very still. Can you practice being still like a statue?” This type of dialogue involves the child and gives him or her a role related to imaging. For placement of an intravenous line, one might explain to the child, “First you will feel a tight squeeze around your arm, next it will feel cold and wet while we wash it, then you will feel a quick poke. Can you hold the bandage for me and put it on your arm when we are done?” In this setting, the child knows what to expect, has some control, and understands that there will be a beginning and an end to the procedure. Adolescents often see themselves as invincible, and may delay telling caregivers about medical issues they are experiencing and/or withhold important details. When taking a history before imaging, it is important to speak directly to these older patients and not only to their caregivers. Adolescents should be asked whether they prefer to be alone during imaging or have their caregiver accompany them. Privacy should be considered, particularly when performing an invasive study such as a voiding cystourethrogram (VCUG). If ample staffing is available, it is nice to offer the adolescent patient the option of a male or female practitioner, particularly for these sensitive studies. Options for distraction should be offered. These may include an iPad, a portable DVD player, or even the patient’s phone. With all patients and caregivers, medical jargon should be avoided. It is important to remember that terminology that is commonplace to practitioners in the medical setting is often unfamiliar and confusing to others.