© Springer Japan 2015
Yasushi Nagata (ed.)Stereotactic Body Radiation Therapy10.1007/978-4-431-54883-6_11. Introduction and History of Stereotactic Body Radiation Therapy (SBRT)
(1)
Department of Radiation Oncology, Hiroshima University Hospital, Hiroshima, Japan
1.1 Introduction
Intracranial Stereotactic Radiosurgery (SRS) was a new treatment method for brain tumors introduced in the twentieth century to deliver tight spatial/temporal distribution using a high precision technique. The clinical experience from intracranial SRS, together with the technical developments in conventional RT, initiated the development of Stereotactic Body Radiation Therapy (SBRT) for extracranial tumors characterized by a very high dose per fraction, delivered in a short time. This was started at the Swedish Karolinska University hospital in 1991 with tumors in the liver and lungs by Bromgren and Lax [1–3]. In parallel this method was developed in Japan and clinically introduced in 1994 for lung tumors [4–6]. During the last 5 years of the nineties, SBRT was introduced in several centers in Europe, Japan and USA. Wulf and Herfarth in Germany reported these clinical results on lung cancer in 2001, followed by Timmerman in USA in 2003. In Japan, a Japanese study group of stereotactic body radiation therapy was formed in 1999, and it expands annually. It then transformed into the Japan 3-D conformal external beam radiotherapy group (J-CERG) in 2002. The SBRT procedure was approved by the Japanese government to be covered by the health insurance in 2004. The early reports had already shown very promising results with regard to local control and toxicity for the hypofractionation schedules which were adopted with 10–15 Gy/fraction given in 3–5 fractions during a short time. However, due to the new aspects introduced in SBRT, clinical experience was initially accumulated at a very slow rate and it was only during the last decade that outcome data from several centers was available to confirm the initial promising results. In this session, the historical development of SBRT was reviewed.
1.2 Intracranial Radiosurgery
The field of intracranial radiosurgery was mainly developed between 1950 and 1970. The treatment was named as radiosurgery by Leksell as an alternative to neurosurgery. Thereafter, the terminology of stereotactic radiosurgery meant single high dose with accurate spatial precision. The system named as the Gamma Knife is a system with a metal helmet and multiple holes attached to a capsule of 201 multiple gamma sources. The Gamma Knife system developed into from the original system up to a modern new system. The new system has an automatic helmet exchange with multi-leaf collimators. The radiosurgery technique was also possible using a conventional linear accelerator with a 3-dimensional radiosurgery systems. This system included metallic ring to be attached to a patient and fixation system attached to a couch. The 3-dimensional coordinates were essential for SRS. The accuracy of linear accelerator was essential.
1.3 Principles and Methods
To extend the intracranial radiosurgery technology to extracranial tumors, two problems should be solved. First, most extracranial tumors move with or without respiratory motion. With tumor motions, wide ITV margins prevent delivering high dose to the tumor. The other difficulty is the unknown normal tissue toxicity using single high dose. Previous experiences with clinical radiotherapy are based on daily 2 Gy radiotherapy up to 60 or 70 Gy. Therefore, 48–60 Gy in 3–5 fractions are unknown area.
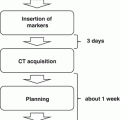
Therefore, initial SBRT was based on stereotactic coordinates using the Stereotactic Body Frame. Patients were stored within a plastic frame with three-dimensional coordinates. After the set-up with these coordinates, single high dose was irradiated with non-coplanar beams.
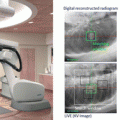
The other concern is the respiratory tumor movement. To regulate respiratory movement, various methods were used. Initially, abdominal press or breath-hold techniques were most popular methods, thereafter, developed into respiratory gating and chasing methods.
Geometric verification at each treatment is essential for SBRT, it is because single dose set-up error will consequently make local tumor recurrence. Therefore, AP and lateral portal verifications using films were essential before each treatment, which now developed into EPID technology and cone-beam CT technology.
1.4 Dose Fractionation and Normal Tissue Dose Constraints
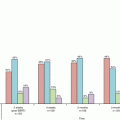
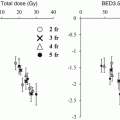
Even now, the best dose fractionation schedule for lung and liver tumors are unknown. The accurate dose constraints for normal tissue are still unknown. In Japan, Dr. Uematsu used 50 Gy in 10 fractions, followed by Arimoto 60 Gy in 8 fractions, and by Nagata 48 Gy in 4 fractions and. In USA, 60 Gy in 3 fractions was the original, currently 54 Gy in 3 or 48–50 Gy in 4 were popular. In European countries, various fractionations were used at Karolinska Hospital, followed by 45 Gy in 3 fractions and 24 Gy in single fraction. We must be careful that these doses were prescribed at different points either isocenter or margin. The normal tissue dose constraints were set by JCOG (Japan Clinical Oncology Group) mainly proposed by Dr. Shirato.
1.5 Terminology
The name of SBRT was introduced by Timmerman in 2002. He originally used Stereotactic Ablative Radiosurgery for this treatment. However, there were several opposition from radiation oncologists because this treatment is completely different from radiofrequency ablation (RFA). In 2005, Stereotactic body radiation therapy (SBRT) was used as a code of radiation therapy in USA. Extracranial stereotactic radiation therapy (ESRT) was used in Europe late 1990s and pin-pointed radiation therapy was used in Japan late 1990a. In 2010, Stereotactic ablative radiotherapy (SABR) was introduced by Loo et al. It was because the pronunciation of SBRT was difficult. Currently the terminology of SBRT and SABR are both used and are very confusing.
References
1.
2.
Lax I, Blomgren H, Larson D, et al. Extracranial stereotactic radiosurgery of localized targets. J Radiosurg. 1998;1:135–48.CrossRef
3.
4.
6.
Arimoto T, Usubuchi H, Matsuzawa T, et al. Small volume multiple non-coplanar arc radiotherapy for tumors of the lung, head & neck and the abdominopelvic region. Tokyo: Elsevier; 1998.
Bibliography
3rd Acta Oncologica symposium on stereotactic body radiotherapy. Copenhagen: Acta Oncol. 2006;45:771–994.
Bauman P, Nyman J, Hoyer M, et al. Outcome in a prospective phase II trial of medically inoperable stage I non-small cell lung cancer patients treated with stereotactic body radiotherapy. J Clin Oncol. 2009;27:3290–6.CrossRef
Blomgren H, Lax I, Göranson H, et al. Radiosurgery for tumors in the body: clinical experience using a new method. J Radiosurg. 1998;1:63–74.CrossRef
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree