Case presentation
A 15-year-female presents with low back pain for 2 months. She had no trauma preceding the pain but is very active and plays soccer. The pain increases with activity. She has tried ibuprofen multiple times, with some relief. Her mother took her to her primary care provider last week where a urine test was performed, which was unremarkable. She has not had fever, vomiting, abdominal pain, vaginal bleeding, vaginal discharge, numbness, or weakness.
Her physical examination reveals a well-appearing child who is afebrile. Her heart rate is 65 beats per minute, respiratory rate is 20 breaths per minute, blood pressure is 125/75 mm Hg, and pulse oximetry is 100% on room air. Her weight is 44 kg. She has an unremarkable examination except for mild midspinal lumbar tenderness without crepitus, warmth, or deformity to palpation. She ambulates with a steady gait. Her neurologic examination is benign, with equal tone and strength throughout.
Imaging considerations
Not every pediatric patient with nontraumatic back pain requires imaging. Imaging should be considered in patients with localized pain, neurologic deficits, worsening pain, or persistent pain. Feldman et al. devised an algorithm for the evaluation of nontraumatic pediatric back pain utilizing history, physical examination, complete blood count (recommended in children under 10 years of age in this study due to the association of back pain and leukemia in younger patients), and imaging (plain radiography and magnetic resonance imaging [MRI]). In this group of close to 100 patients, if radiographs were positive and correlated with historical and physical examination findings, then the patient was treated accordingly; if the radiographs were negative and concerning pain was reported (such as constant pain or night pain) or there was an abnormal neurological examination, an MRI study was obtained and positive findings on MRI were treated accordingly. Patients who had negative radiographs and intermittent pain were treated for presumed overuse syndromes or sprains with rest, physical therapy, and nonsteroidal antiinflammatory medications. Using this algorithm, 36% of the patients in the study group were diagnosed with a specific condition, 68% of these patients had a positive finding on initial radiographs, and the remaining patients in this group who had negative initial radiographs had positive findings on MRI.
A study by Ramirez et al. had similar results when examining the utility of MRI in patients after employing the Feldman et al. algorithm of history, physical examination, and plain radiography. These investigators found that 34% of patients in their study had an identifiable cause of back pain, with diagnostic yield increasing from 8.8% (based on history, physical examination, and plain radiographs) to 36% with the use of MRI. Of the 89 patients who had confirmed pathology, 26% were discovered with plain radiographs and 74% with MRI.
Bhatia et al. also employed an algorithm similar to Feldman et al. utilizing history, physical examination, laboratory investigation, and plain radiography in 73 patients; 57 (78%) of the patients in this study had no identifiable cause of back pain and none of these had abnormal radiologic or laboratory findings. Of the remaining 16 patients, 9 were diagnosed with spondylolysis (with or without spondylolisthesis), with the remaining patients having another diagnosis (osteoid osteoma and disk herniation). Thirteen patients (nearly 18%) in this study had a definitive diagnosis, and of those patients, 10 had abnormal plain radiography, 8 of whom were diagnosed with spondylolysis with or without spondylolisthesis (scoliosis was not considered an etiology of back pain).
Plain radiography
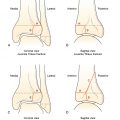
Plain radiography is an excellent first-choice imaging study due to its low cost and widespread availability, but this is not without controversy, as some authors report low diagnostic yield with plain radiographic imaging for pediatric patients with back pain. , Notably, plain radiographs appear normal in the majority of patients with non-concerning histories and physical examinations. There is also controversy regarding the optimal number of views to obtain. Posteroanterior (PA) or anteroposterior (AP) and lateral views of the spine appear to be sufficient in most cases, as an oblique view has not been shown to increase diagnostic accuracy, , , , although some authors advocate its use. There are stages in the development of spondylolysis, including early stress reaction without fracture, progression to fracture, and if healing and union do not occur, where there is nonunion and a wider osseous defect at the pars. Much of the historical plain film literature in spondylolysis has been in adults, who often have advanced, terminal spondylolysis; however, pediatric patients are more likely than adults to present with early or progressive spondylolysis that may be amenable to healing with conservative management but is more difficult to detect on plain film evaluation, including on oblique views. It is reasonable to obtain two views of the spine (PA and lateral), and, if symptoms persist or worsen, consideration can be given to obtaining oblique views or advanced imaging modalities. ,
Computed tomography (CT)
CT has been shown to be sensitive and specific for detecting spondylolysis and spondylolisthesis. , Computerized tomography can also help to characterize other pathology of the posterior elements of the spine, the vertebral end plates, and facet joints. , Single photon emission CT (SPECT/CT) combines nuclear medicine bone scan imaging with low-dose CT and detects spondylolysis and other vertebral pathology but also shows increased radionucleotide uptake of a stress reaction in the pars interarticularis prior to the development of fracture. SPECT/CT is useful if there is a strong clinical suspicion of spondylolysis and plain radiography is unremarkable. , However, this is not an imaging technique utilized in the emergency care setting and is most often ordered in outpatient follow-up, frequently by an orthopedic surgeon. There is radiation exposure with SPECT/CT imaging; most of this is the exposure of a nuclear medicine bone scan with a very small additional contribution to dose by low-dose CT.
Magnetic resonance imaging
Patients may benefit from MRI if further clarification of plain radiography findings is needed, or if there is concern for an infectious, inflammatory, or neoplastic process, as these alternative diagnoses can be readily detected with this modality. MRI is more sensitive than CT scan for the detection of stress reactions in the pars and can detect stress reactions in the pars prior to the development of an osseous defect. , T2-weighted images may demonstrate an abnormal signal that can be observed in the pars interarticularis and the adjacent pedicles, suggesting pathology. , MRI may also be useful if there are associated neurologic symptoms. There have been proposed algorithms for the utilization of MRI in patients with persistent or worsening symptoms or an abnormal neurologic examination. ,
Imaging findings
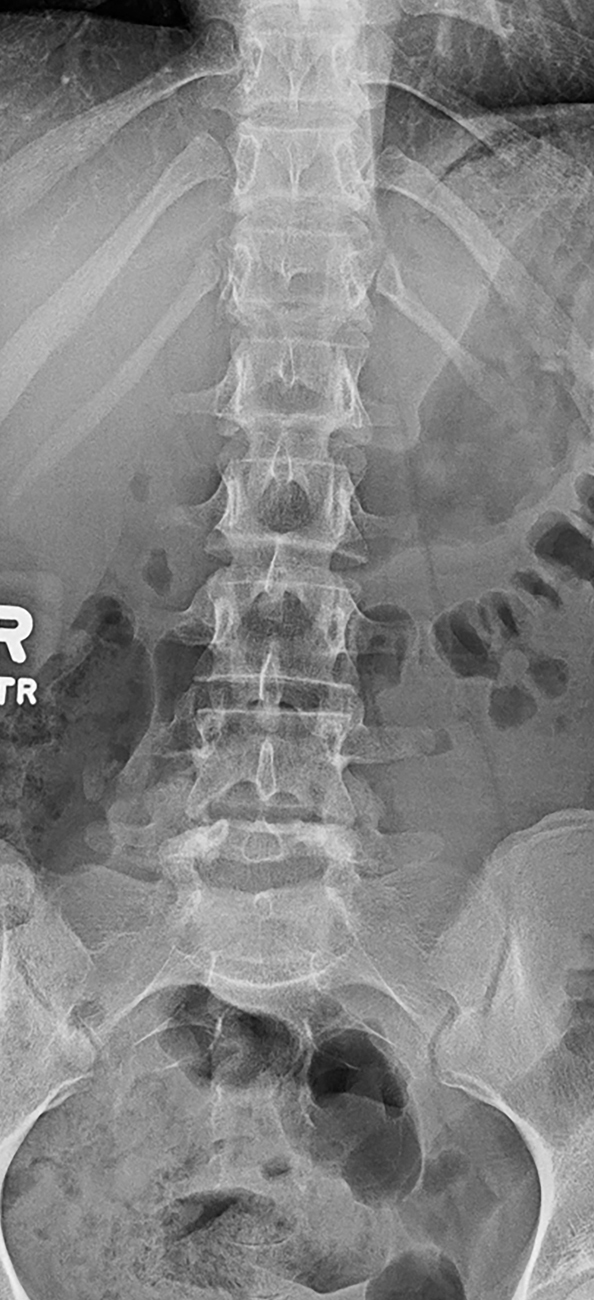
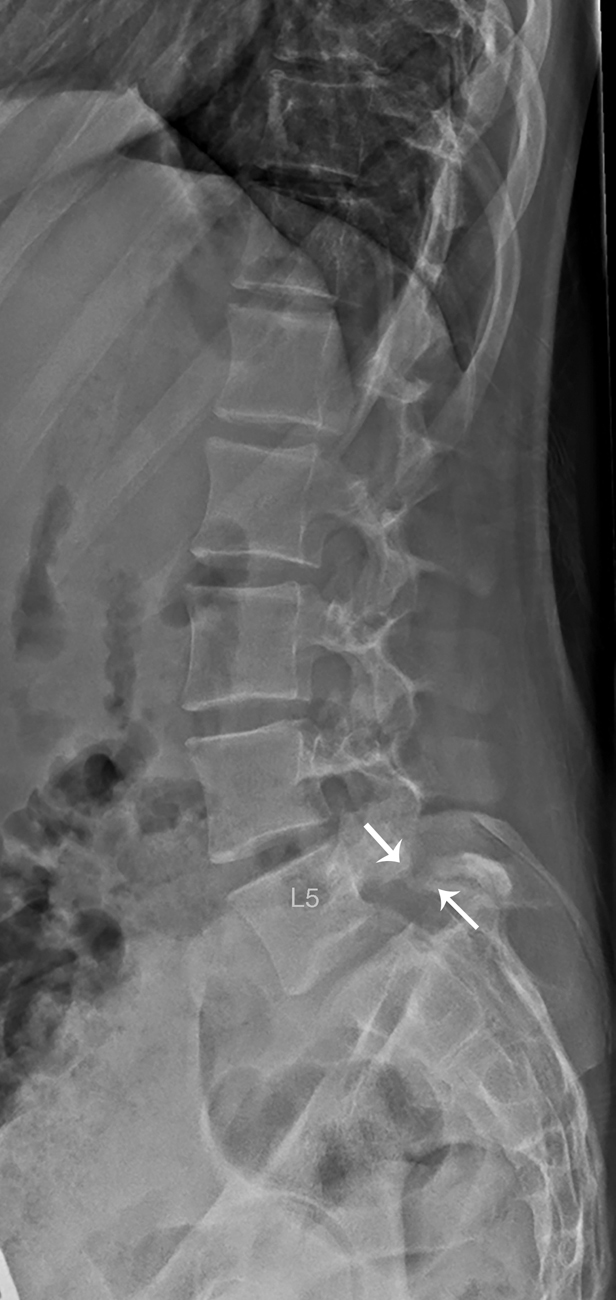
Plain radiography of the lumbar spine (AP and lateral views) was obtained. These images demonstrate a grade I spondylolisthesis of L5 on S1 associated with bilateral spondylolysis at L5. There is no other pathology of the lumbosacral spine noted ( Figs. 70.1 and 70.2 ).

Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree